Abstract
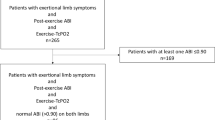
To study the concordance of exercise-oximetry and of ankle-brachial pressure index (ABI) and ankle pressure (AP) at rest, and after exercise, in patients complaining of vascular-type claudication to diagnose lower extremity artery disease (LEAD). Treadmill test in 433 patients with exercise-oximetry included constant load (3.2 km/h, 10% slope) phase for up to 15 min followed by an increment phase, if necessary. The presence (TcpO2e+) or absence (TcpO2e−) of ischemia was a decrease of limb minus chest oxygen pressure change greater than or less than − 15 mmHg. The post-exercise ABI and AP were measured after another test of a maximum of 5 min except if resting-ABI < 0.90. LEAD was diagnosed (+) based on resting-ABI < 0.90, post-exercise ABI < 0.8∙resting-ABI, or a difference of 30 mmHg between post-exercise and resting AP, or diagnosis was considered negative for all other cases (−). The discrepancies between the exercise-oximetry and pressure results were analyzed. We found 351 patients with resting-ABI+, of whom 52 were classified as TcpO2e−. Of the 82 patients with resting-ABI−, 25 had post-exercise ABI+ or AP+, of whom, 10 had TcpO2e−, while 57 had post-exercise ABI− and AP−, of whom, 28 had TcpO2e+. Discrepancies arose mainly from nonvascular limitations, isolated proximal ischemia, and detection of LEAD in the incremental phase of the exercise-oximetry. Post-exercise pressure measurements were easy and useful, but exercise-oximetry provided additional information for both resting-ABI− and resting-ABI+ patients and can help to prove the vascular origin of walking limitation of LEAD patients.




Similar content being viewed by others
Abbreviations
- ABI:
-
Ankle brachial index
- AP:
-
Ankle pressure
- DROP:
-
Decrease from rest of oxygen pressure
- LEAD:
-
Lower extremity artery disease.
- TcpO2e:
-
Exercise transcutaneous oximetry
- US:
-
Ultrasound imaging
References
Aboyans V, Criqui MH, Abraham P, Allison MA, Creager MA, Diehm C, Fowkes FG, Hiatt WR, Jonsson B, Lacroix P, Marin B, McDermott MM, Norgren L, Pande RL, Preux PM, Stoffers HE, Treat-Jacobson D, American Heart Association Council on Peripheral Vascular D, Council on E, Prevention, Council on Clinical C, Council on Cardiovascular N, Council on Cardiovascular R, Intervention, Council on Cardiovascular S, Anesthesia (2012) Measurement and interpretation of the ankle-brachial index: a scientific statement from the American Heart Association. Circulation 126:2890–2909. https://doi.org/10.1161/CIR.0b013e318276fbcb
Abraham P, Colas-Ribas C, Signolet I, Ammi M, Feuilloy M, Picquet J, Henni S (2018) Transcutaneous exercise oximetry for patients with claudication - a retrospective review of approximately 5,000 consecutive tests over 15 years. Circ J 82:1161–1167. https://doi.org/10.1253/circj.CJ-17-0948
Abraham P, Gu Y, Guo L, Kroeger K, Ouedraogo N, Wennberg P, Henni S (2018) Clinical application of transcutaneous oxygen pressure measurements during exercise. Atherosclerosis 276:117–123. https://doi.org/10.1016/j.atherosclerosis.2018.07.023
Abraham P, Picquet J, Bouye P, L'Hoste P, Enon B, Vielle B, Saumet JL (2005) Transcutaneous oxygen pressure measurements (tcpO2) at ankle during exercise in arterial claudication. Int Angiol 24:80–88
Abraham P, Picquet J, Vielle B, Sigaudo-Roussel D, Paisant-Thouveny F, Enon B, Saumet J-L (2003) Transcutaneous oxygen pressure measurements on the buttocks during exercise to detect proximal arterial ischemia: comparison with arteriography. Circulation 107:1896–1900. https://doi.org/10.1161/01.CIR.0000060500.60646.E0
Abraham P (2018) Software analysis of transcutaneous oxygen pressure measurements at exercise in patients with arterial claudication Software analysis of transcutaneous oxygen pressure measurements at exercise in patients with arterial claudication. Atherosclerosis 278:328–329. https://doi.org/10.1016/j.atherosclerosis.2018.09.014
Aday AW, Kinlay S, Gerhard-Herman MD (2018) Comparison of different exercise ankle pressure indices in the diagnosis of peripheral artery disease. Vasc Med:1358863X18781723. https://doi.org/10.1177/1358863X18781723
Audonnet M, Signolet I, Colas-Ribas C, Ammi M, Abraham P, Henni S (2017) Exercise transcutaneous oximetry of the buttocks - external validation with computed tomography angiography. Circ J 81:1123–1128. https://doi.org/10.1253/circj.CJ-16-1316
Bouye P, Picquet J, Jaquinandi V, Enon B, Leftheriotis G, Saumet JL, Abraham P (2004) Reproducibility of proximal and distal transcutaneous oxygen pressure measurements during exercise in stage 2 arterial claudication. Int Angiol 23:114–121
Carter SA (1968) Indirect systolic pressures and pulse waves in arterial occlusive diseases of the lower extremities. Circulation 37:624–637. https://doi.org/10.1161/01.cir.37.4.624
Cohoon KP, Mahe G, Liedl DA, Rooke TW, Wennberg PW (2017) Discrepancies in prevalence of peripheral arterial disease between lower extremities at rest and postexercise. Int J Angiol 26:179–185. https://doi.org/10.1055/s-0037-1598177
Gerhard-Herman MD, Gornik HL, Barrett C, Barshes NR, Corriere MA, Drachman DE, Fleisher LA, Fowkes FGR, Hamburg NM, Kinlay S, Lookstein R, Misra S, Mureebe L, Olin JW, Patel RAG, Regensteiner JG, Schanzer A, Shishehbor MH, Stewart KJ, Treat-Jacobson D, Walsh ME (2017) 2016 AHA/ACC guideline on the management of patients with lower extremity peripheral artery disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol 69:e71–e126. https://doi.org/10.1016/j.jacc.2016.11.007
Halliday A, Bax JJ (2018) The 2017 ESC guidelines on the diagnosis and treatment of peripheral arterial diseases, in collaboration with the European Society for Vascular Surgery (ESVS). Eur J Vasc Endovasc Surg 55:301–302. https://doi.org/10.1016/j.ejvs.2018.03.004
Hammad TA, Strefling JA, Zellers PR, Reed GW, Venkatachalam S, Lowry AM, Gornik HL, Bartholomew JR, Blackstone EH, Shishehbor MH (2015) The effect of post-exercise ankle-brachial index on lower extremity revascularization. JACC Cardiovasc Interv 8:1238–1244. https://doi.org/10.1016/j.jcin.2015.04.021
Laing S, Greenhalgh RM (1983) The detection and progression of asymptomatic peripheral arterial disease. Br J Surg 70:628–630
Leng GC, Fowkes FG (1992) The Edinburgh Claudication Questionnaire: an improved version of the WHO/Rose Questionnaire for use in epidemiological surveys. J Clin Epidemiol 45:1101–1109
Mahe G, Pollak AW, Liedl DA, Cohoon KP, Mc Carter C, Rooke TW, Wennberg PW (2015) Discordant diagnosis of lower extremity peripheral artery disease using American Heart Association postexercise guidelines. Medicine (Baltimore) 94:e1277. https://doi.org/10.1097/MD.0000000000001277
Morley RL, Sharma A, Horsch AD, Hinchliffe RJ (2018) Peripheral artery disease. BMJ (Clin Res ed) 360:j5842
Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, Fowkes FG, Group TIW, Bell K, Caporusso J, Durand-Zaleski I, Komori K, Lammer J, Liapis C, Novo S, Razavi M, Robbs J, Schaper N, Shigematsu H, Sapoval M, White C, White J, Clement D, Creager M, Jaff M, Mohler E 3rd, Rutherford RB, Sheehan P, Sillesen H, Rosenfield K (2007) Inter-society consensus for the management of peripheral arterial disease (TASC II). Eur J Vasc Endovasc Surg 33(Suppl 1):S1–S75. https://doi.org/10.1016/j.ejvs.2006.09.024
Ouedraogo N, Barbeau C, Legrand M, Marchand J, Leftheriotis G, Abraham P (2013) “Routine” arterial echo-Doppler is not sufficient to exclude an arterial origin of exercise-induced proximal lower limb pain. Int J Cardiol 167:1053–1054. https://doi.org/10.1016/j.ijcard.2012.10.080
Ouriel K, McDonnell AE, Metz CE, Zarins CK (1982) Critical evaluation of stress testing in the diagnosis of peripheral vascular disease. Surgery 91:686–693
Perakyla T, Tikkanen H, von Knorring J, Lepantalo M (1998) Poor reproducibility of exercise test in assessment of claudication. Clin Physiol 18:187–193. https://doi.org/10.1046/j.1365-2281.1998.00092.x
Rutherford RB, Baker JD, Ernst C, Johnston KW, Porter JM, Ahn S, Jones DN (1997) Recommended standards for reports dealing with lower extremity ischemia: revised version. J Vasc Surg 26:517–538. https://doi.org/10.1016/s0741-5214(97)70045-4
Stein R, Hriljac I, Halperin JL, Gustavson SM, Teodorescu V, Olin JW (2006) Limitation of the resting ankle-brachial index in symptomatic patients with peripheral arterial disease. Vasc Med 11:29–33. https://doi.org/10.1191/1358863x06vm663oa
Stivalet O, Paisant A, Belabbas D, Omarjee L, Le Faucheur A, Landreau P, Garlantezec R, Jaquinandi V, Liedl DA, Wennberg PW, Mahe G (2019) Exercise testing criteria to diagnose lower extremity peripheral artery disease assessed by computed-tomography angiography. PLoS One 14:e0219082. https://doi.org/10.1371/journal.pone.0219082
Acknowledgements
The authors are grateful to Stephanie Marechal, Marine Mauboussin, and Patrick Vandeputte for their technical support. We thank Laurent Landais for the image preparations. The work is presented on behalf of the SOCOS-SAM group.
Author information
Authors and Affiliations
Consortia
Contributions
PA and SH conceived and designed and analyzed the study and wrote the graft, JH, PR, JP, MF participated to data acquisition, reviewed & approved the final version of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the special issue on Exercise Physiology: future opportunities and challenges in Pflügers Archiv—European Journal of Physiology
Rights and permissions
About this article
Cite this article
Abraham, P., Hersant, J., Ramondou, P. et al. Comparison of exercise oximetry and ankle pressure measurements for patients with intermittent claudication: an observational study of 433 patients. Pflugers Arch - Eur J Physiol 472, 293–301 (2020). https://doi.org/10.1007/s00424-019-02340-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-019-02340-w