Abstract
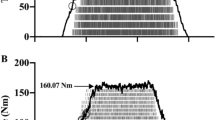
We hypothesized that the changes in muscle temperature and interstitial pressure during thermoneutral immersion may affect the reflex adaptation of the motor drive during static contraction, assessed by the decrease in median frequency (MF) of electromyogram (EMG) power spectrum. Ten subjects were totally immerged for 6 h at 35°C and repeated maximal voluntary contraction (MVC) and submaximal (60% MVC) leg extensions sustained until exhaustion. In vastus lateralis (VL) and soleus (SOL) muscles, the compound muscle potential evoked by muscle stimulation with single shocks (M-wave) was recorded at rest, and MF of surface EMG was calculated during 60% MVCs. We measured lactic acid and potassium venous blood concentrations and calculated plasma volume changes. Data were compared to those obtained in the same individuals exercising at 35°C under dry conditions where the MF decrease during 60% MVCs was modest (−4 to−5%). During immersion, the rectal temperature remained stable, but the thigh and calf surface temperatures significantly increased. Lactic acid and potassium concentrations did not vary, but plasma volume decreased from the 180th min of immersion. The M-wave did not vary in VL but was prolonged in SOL from the 30th min of immersion. From the 220th min of immersion, the maximal MF decrease was majored in both muscles (−18 to −22%). Thus, compared to the dry condition, total body thermoneutral immersion enhances fatigue-induced EMG changes in leg muscles, perhaps through the activation of warm-sensitive muscle endings and/or the changes in interstitial pressure because of vasodilatation.







Similar content being viewed by others
References
Badier M, Guillot C, Lagier F, Burnet H, Jammes Y (1993) EMG power spectrum of respiratory and skeletal muscles during static contraction in healthy man. Muscle Nerve 16:601–609
Badier M, Guillot C, Lagier-Tessonier F, Jammes Y (1994) EMG changes in respiratory and skeletal muscles during isometric contraction under normoxic, hypoxemic, or ischemic conditions. Muscle Nerve 17:500–508
Bendahan D, Badier M, Jammes Y, Confort-Gouny S, Salvan AM, Guillot C, Cozzone PJ (1998) Metabolic and myoelectrical effects of acute hypoxaemia during isometric contraction of forearm muscles in humans: a combined 31P-magnetic resonance spectroscopy-surface electromyogram (MRS-EMG) study. Clin Sci 94:279–286
Bigland-Ritchie B, Dawson NJ, Johansson RS, Lippold OCJ (1986) Reflex origin for the slowing of motoneurone firing rates in the fatigue of human voluntary contractions. J Physiol 379:451–459
Coulange M, Kipson N, Robinet C, Desruelle AV, Melin B, Galland F, Jammes Y (2006) Consequences of prolonged total body immersion in cold water on muscle performance and EMG activity. Pflugers Arch 452:91–101
Darques JL, Jammes Y (1997) Fatigue-induced changes in group IV muscle afferent activity: differences between high- and low-frequency electrically induced fatigues. Brain Res 750:147–154
Decherchi P, Darques JL, Jammes Y (1998) Modifications of afferent activities from Tibialis anterior muscle in rat by tendon vibrations, increase of interstitial potassium or lactate concentration and electrically-induced fatigue. J Periph Nerv Sys 3:267–276
Dewhurst S, Riches PE, Nimmo MA, De Vito G (2005) Temperature dependence of soleus H-reflex and M-wave in young and older women. Eur J Appl Physiol 94:491–499
Dill DB, Costill DL (1974) Calculation of percentage changes in volumes of blood, plasma and red cells in dehydration. J Appl Physiol 37:247–248
Edwards RHT, Harris RC, Hultman E, Kaijser L, Koh D, Nordesjo LO (1972) Effects of temperature on muscle energy metabolism and endurance during successive isometric contractions sustained to fatigue of the quadriceps muscle in man. J Physiol 220:335–352
Enoka RM, Stuart D (1992) Neurobiology of muscle fatigue. J Appl Physiol 72:1631–1648
Fischer M, Schafer SS (1999) Temperature effects on the discharge frequency of primary and secondary endings of isolated cat muscle spindles recorded under a ramp-and-hold stretch. Brain Res 840:1–15
Gandevia SC (2001) Spinal and supraspinal factors in human muscle fatigue. Physiol Rev 81:1725–1789
Garland SJ (1991) Role of small diameter afferents in reflex inhibition during human muscle fatigue. J Physiol 435:547–558
Gordon CJ, Fogarty AL, Greeleaf JE, Taylor NA, Stocks JM (2003) Direct and indirect methods for determining plasma volume during thermoneutral and cold-water immersion. Eur J Appl Physiol 89:471–474
Haouzi P, Chenuel B, Huszczuk (2004) Sensing vascular distension in skeletal muscle by slow conducting afferent fibers: neurophysiological basis and implication for respiratory control. J Appl Physiol 96:407–418
Holewijn M, Heus R (1992) Effects of temperature on electromyogram and muscle function. Eur J Appl Physiol 65:541–545
Jammes Y, Balzamo E (1992) Changes in afferent and efferent phrenic activities with electrically induced diaphragmatic fatigue. J Appl Physiol 73:894–902
Johansen LB, Foldager N, Stadeager C, Kristensen MS, Bie P, Warberg J, Kamegai M, Norsk P (1992) Plasma volume, fluid-shifts, and renal responses in humans during 12 h of head-out water immersion. J Appl Physiol 73:539–544
Krause KH, Magyarosy I, Gall H, Ernst E, Pongratz D, Schoeps P (2001) Effects of heat and cold application on turns and amplitude in surface EMG. Electromyogr Clin Neurophysiol 41:67–70
Lagier-Tessonnier F, Balzamo E, Jammes Y (1993) Comparative effects of ischemia and acute hypoxenia on muscle afferents from tibialis anterior in cats. Muscle Nerve 16:135–141
Mense S, Meyer H (1985) Different types of slowly conducting afferent units in cat skeletal muscle and tendon. J Physiol 363:403–417
Miki K, Hayashida Y, Shiraki K (2002) Role of cardiac-renal neural reflex in regulating sodium excretion during water immersion in conscious dogs. J Physiol 545:305–312
Nakamitsu S, Sagawa S, Miki K, Wada F, Nagaya K, Keil LC, Drummer C, Gerzer R, Greenleaf JE, Hong SK (1994) Effect of water temperature on diuresis-natriuresis: AVP, ANP, and urodilatin duting immersion in men. J Appl Physiol 77:1919–1925
Stocks JM, Patterson MJ, Hyde DE, Jenkins AB, Mittleman KD, Taylor NA (2004) Effects of immersion water temperature on whole-body fluid distribution in humans. Acta Physiol Scand 182:3–10
Woods JJ, Furbush F, Bigland-Ritchie B (1987) Evidence for a fatigue-induced reflex inhibition of motoneurone firing rates. J Neurophysiol 58:125–137
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Coulange, M., Riera, F., Melin, B. et al. Consequences of prolonged total thermoneutral immersion on muscle performance and EMG activity. Pflugers Arch - Eur J Physiol 455, 903–911 (2008). https://doi.org/10.1007/s00424-007-0335-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-007-0335-y