Abstract
Purpose
This study aimed to investigate the risk factors for re-drainage in patients with early drain removal after pancreaticoduodenectomy (PD).
Methods
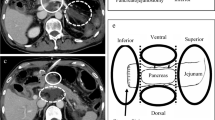
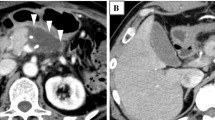
This study retrospectively analyzed 114 patients who underwent PD and prophylactic drain removal on postoperative day (POD) 4 between January 2012 and March 2021. We analyzed the risk factors for re-drainage according to various factors. Peri-pancreaticojejunostomic fluid collection (PFC) index and pancreatic cross-sectional area (CSA) were evaluated using computed tomography on POD 4. The PFC index was calculated by multiplying the length, width, and height at the maximum aspect.
Results
Among the 114 patients, 15 (13%) underwent re-drainage due to postoperative pancreatic fistula. Multivariate analysis identified a PFC index ≥ 8.16 cm3 on POD 4 (odds ratio [OR], 20.40, 95%CI 2.38–174.00; p = 0.006) and pancreatic CSA on POD 4 ≥ 3.65 cm2 (OR, 16.40, 95%CI 1.57–171.00; p = 0.020) as independent risk factors for re-drainage.
Conclusion
A careful decision might be necessary for early drain removal in patients with a PFC index ≥ 8.16 cm3 and pancreatic CSA ≥ 3.65 cm2.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, HM, upon reasonable request.
References
Fernandez-del Castillo C, Morales-Oyarvide V, McGrath D et al (2012) Evolution of the Whipple procedure at the Massachusetts General Hospital. Surgery 152:S56–S63
Vollmer CM Jr, Lewis RS, Hall BL et al (2015) Establishing a quantitative benchmark for morbidity in pancreatoduodenectomy using ACS-NSQIP, the Accordion Severity Grading System, and the Postoperative Morbidity Index. Ann Surg 261:527–536
McMillan MT, Vollmer CM Jr, Asbun HJ et al (2016) The characterization and prediction of ISGPF grade C fistulas gollowing pancreatoduodenectomy. J Gastrointest Surg 20:262–276
Mackay TM, Smits FJ, Roos D et al (2020) The risk of not receiving adjuvant chemotherapy after resection of pancreatic ductal adenocarcinoma: a nationwide analysis. HPB (Oxford) 22:233–240
Bonaroti JW, Zenati MS, Al-Abbas AI et al (2021) Impact of postoperative pancreatic fistula on long-term oncologic outcomes after pancreatic resection. HPB (Oxford) 23:1269–1276
Mungroop TH, Klompmaker S, Wellner UF et al (2021) Updated alternative fistula risk score (ua-FRS) to include minimally invasive pancreatoduodenectomy: pan-European validation. Ann Surg 273:334–340
Hirono S, Shimokawa T, Nagakawa Y et al (2020) Risk factors for pancreatic fistula grade C after pancreatoduodenectomy: a large prospective, multicenter Japan-Taiwan collaboration study. J Hepatobiliary Pancreat Sci 27:622–631
Van Buren G 2nd, Bloomston M, Hughes SJ et al (2014) A randomized prospective multicenter trial of pancreaticoduodenectomy with and without routine intraperitoneal drainage. Ann Surg 259:605–612
Kawai M, Tani M, Terasawa H et al (2006) Early removal of prophylactic drains reduces the risk of intra-abdominal infections in patients with pancreatic head resection: prospective study for 104 consecutive patients. Ann Surg 244:1–7
Bassi C, Molinari E, Malleo G et al (2010) Early versus late drain removal after standard pancreatic resections: results of a prospective randomized trial. Ann Surg 252:207–214
Beane JD, House MG, Ceppa EP et al (2019) Variation in drain management after pancreatoduodenectomy: early versus delayed removal. Ann Surg 269:718–724
Ohgi K, Yamamoto Y, Sugiura T et al (2020) The clinical impact and risk factors of latent pancreatic fistula after pancreatoduodenectomy. J Hepatobiliary Pancreat Sci 27:1002–1010
Maehira H, Iida H, Matsunaga T et al (2020) The location of perianastomotic fluid collection predicts postoperative complications after pancreaticoduodenectomy. Langenbecks Arch Surg 405:325–336
Maehira H, Iida H, Mori H et al (2019) Computed tomography enhancement pattern of the pancreatic parenchyma predicts postoperative pancreatic fistula after pancreaticoduodenectomy. Pancreas 48:209–215
Kanda Y (2013) Investigation of the freely available easy-to-use software 'EZR' for medical statistics. Bone Marrow Transplant 48:452–458
Zink SI, Soloff EV, White RR et al (2009) Pancreaticoduodenectomy: frequency and outcome of post-operative imaging-guided percutaneous drainage. Abdom Imaging 34:767–771
Caillol F, Godat S, Turrini O et al (2019) Fluid collection after partial pancreatectomy: EUS drainage and long-term follow-up. Endosc Ultrasound 8:91–98
Giglio MC, Spalding DR, Giakoustidis A et al (2016) Meta-analysis of drain amylase content on postoperative day 1 as a predictor of pancreatic fistula following pancreatic resection. Br J Surg 103:328–336
Lee CW, Pitt HA, Riall TS et al (2014) Low drain fluid amylase predicts absence of pancreatic fistula following pancreatectomy. J Gastrointest Surg 18:1902–1910
Xourafas D, Ejaz A, Tsung A et al (2019) Validation of early drain removal after pancreatoduodenectomy based on modified fistula risk score stratification: a population-based assessment. HPB (Oxford) 21:1303–1311
Marchegiani G, Ramera M, Viviani E et al (2019) Dislocation of intra-abdominal drains after pancreatic surgery: results of a prospective observational study. Langenbecks Arch Surg 404:213–222
Maehira H, Iida H, Mori H et al (2021) Superior perianastomotic fluid collection in the early postoperative period affects pseudoaneurysm occurrence after pancreaticoduodenectomy. Langenbecks Arch Surg 406:1461–1468
Roberts KJ, Hodson J, Mehrzad H et al (2014) A preoperative predictive score of pancreatic fistula following pancreatoduodenectomy. HPB (Oxford) 16:620–628
Sugimoto M, Takahashi S, Gotohda N et al (2013) Schematic pancreatic configuration: a risk assessment for postoperative pancreatic fistula after pancreaticoduodenectomy. J Gastrointest Surg 17:1744–1751
Fang CH, Chen QS, Yang J et al (2016) Body mass index and stump morphology predict an increased incidence of pancreatic fistula after pancreaticoduodenectomy. World J Surg 40:1467–1476
Shi Y, Liu Y, Gao F et al (2018) Pancreatic stiffness quantified with MR elastography: relationship to postoperative pancreatic fistula after pancreaticoenteric anastomosis. Radiology 288:476–484
Iida H, Tani M, Maehira H et al (2019) Postoperative pancreatic swelling predicts pancreatic fistula after pancreaticoduodenectomy. Am Surg 85:321–326
Lin C, Gao J, Zheng H et al (2020) Three-dimensional visualization technology used in pancreatic surgery: a valuable tool for surgical trainees. J Gastrointest Surg 24:866–873
Fang C, An J, Bruno A et al (2020) Consensus recommendations of three-dimensional visualization for diagnosis and management of liver diseases. Hepatol Int 4:437–453
Mohan BP, Shakhatreh M, Dugyala S et al (2019) EUS versus percutaneous management of postoperative pancreatic fluid collection: a systematic review and meta-analysis. Endosc Ultrasound 8(5):298–309
Author information
Authors and Affiliations
Contributions
Study conception and design were performed by Nobuhito Nitta and Hiromitsu Maehira. The first draft of the manuscript was written by Nobuhito Nitta. Masaji Tani and Hiromitsu Maehira commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nitta, N., Maehira, H., Ishikawa, H. et al. Postoperative computed tomography findings predict re-drainage cases after early drain removal in pancreaticoduodenectomy. Langenbecks Arch Surg 408, 427 (2023). https://doi.org/10.1007/s00423-023-03165-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-023-03165-z