Abstract
Aims
To evaluate comparative outcomes of emergency laparotomy closure with and without prophylactic mesh.
Methods
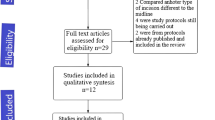
A systematic review was performed via literature databases: PubMed, Cochrane Library, Science Direct, and Google Scholar. Studies were examined for eligibility and included if they compared prophylactic mesh closure to the conventional laparotomy closure following emergency abdominal surgery. Both acute wound failure and incisional hernia (IH) occurence were our primary outcomes. Secondary outcomes included surgical site infection (SSI), seroma/hematoma formation, Clavien-Dindo complications (score ≥ 3), total operative time, and length of hospital stay (LOS).
Results
Two randomised controlled trials (RCTs) and four comparative studies with a total of 817 patients met the inclusion criteria. Overall acute wound failure and incisional hernia rate was significantly lower in the mesh group compared to non-mesh group (odd ratio (OR) 0.23, p = 0.002) and (OR 0.21, p = 0.00001), respectively. There was no significant difference between the two groups regarding the following outcomes: total operative time (mean difference (MD) 21.44, p = 0.15), SSI (OR 1.47, p = 0.06), seroma/haematoma formation (OR 2.74, p = 0.07), grade ≥ 3 Clavien-Dindo complications (OR 2.39, p = 0.28), and LOS (MD 0.26, p = 0.84).
Conclusion
The current evidence for the use of prophylactic mesh in emergency laparotomy is diverse and obscure. Although the data trends towards a reduction in the incidence of IH, a reliable conclusion requires further high-quality RCTs to fully assess the efficacy and safety of mesh use in an emergency setting.



Similar content being viewed by others
References
Tolstrup M-B, Watt SK, Gögenur I (2017) Morbidity and mortality rates after emergency abdominal surgery: an analysis of 4346 patients scheduled for emergency laparotomy or laparoscopy. Langenbecks Arch Surg 402(4):615–623
Murtaza B, Saeed S, Sharif MA (2010) Postoperative complications in emergency versus elective laparotomies at a peripheral hospital. J Ayub Med Coll Abbottabad 22(3):42–47
Webster C, Neumayer L, Smout R, Horn S, Daley J, Henderson W et al (2003) Prognostic models of abdominal wound dehiscence after laparotomy. J Surg Res 109(2):130–137
Halasz NA (1968) Dehiscence of laparotomy wounds. Am J Surg 116(2):210–214
Díaz CJG, Cladera PR, Soto SN, Rosas JMH, Aufroy AL, Vioque SM et al (2014) Validation of abdominal wound dehiscence’s risk model. Cirugía Española (English Edition) 92(2):114–119
Meena K, Ali S, Chawla AS, Aggarwal L, Suhani S, Kumar S et al (2013) A prospective study of factors influencing wound dehiscence after midline laparotomy. Surg Sci 4(8):354–358
van Ramshorst GH, Nieuwenhuizen J, Hop WC, Arends P, Boom J, Jeekel J et al (2010) Abdominal wound dehiscence in adults: development and validation of a risk model. World J Surg 34(1):20–27
Fleischer G, Rennert A, Rühmer M (2000) Infected abdominal wall and burst abdomen. Der Chirurg; Zeitschrift fur Alle Gebiete der Operativen Medizen 71(7):754–62
Carlson MA (1997) Acute wound failure. Surg Clin North Am 77(3):607–636
Fischer JP, Basta MN, Mirzabeigi MN, Bauder AR, Fox JP, Drebin JA et al (2016) A risk model and cost analysis of incisional hernia after elective, abdominal surgery based upon 12,373 cases: the case for targeted prophylactic intervention. Ann Surg 263(5):1010–1017
van Ramshorst GH, Eker HH, Hop WC, Jeekel J, Lange JF (2012) Impact of incisional hernia on health-related quality of life and body image: a prospective cohort study. Am J Surg 204(2):144–150
Sørensen LT, Hemmingsen U, Kallehave F, Wille-Jørgensen P, Kjærgaard J, Møller LN et al (2005) Risk factors for tissue and wound complications in gastrointestinal surgery. Ann Surg 241(4):654
Sanders DL, Kingsnorth AN (2012) The modern management of incisional hernias. BMJ 344:e2843
Moussavian MR, Schuld J, Dauer D, Justinger C, Kollmar O, Schilling MK et al (2010) Long term follow up for incisional hernia after severe secondary peritonitis—incidence and risk factors. Am J Surg 200(2):229–234
Mingoli A, Puggioni A, Sgarzini G, Luciani G, Corzani F, Ciccarone F et al (1999) Incidence of incisional hernia following emergency abdominal surgery. Ital J Gastroenterol Hepatol 31(6):449–453
Itatsu K, Yokoyama Y, Sugawara G, Kubota H, Tojima Y, Kurumiya Y et al (2014) Incidence of and risk factors for incisional hernia after abdominal surgery. Br J Surg 101(11):1439–1447
Aksamija G, Mulabdic A, Rasic I, Aksamija L (2016) Evaluation of risk factors of surgical wound dehiscence in adults after laparotomy. Med Arch 70(5):369
Deerenberg EB, Harlaar JJ, Steyerberg EW, Lont HE, van Doorn HC, Heisterkamp J et al (2015) Small bites versus large bites for closure of abdominal midline incisions (STITCH): a double-blind, multicentre, randomised controlled trial. Lancet 386(10000):1254–1260
Rink AD, Goldschmidt D, Dietrich J, Nagelschmidt M, Vestweber K-H (2000) Negative side-effects of retention sutures for abdominal wound closure. A prospective randomised study. Eur J Surg 166(12):932–7
Khorgami Z, Shoar S, Laghaie B, Aminian A, Araghi NH, Soroush A (2013) Prophylactic retention sutures in midline laparotomy in high-risk patients for wound dehiscence: a randomized controlled trial. J Surg Res 180(2):238–243
Borab ZM, Shakir S, Lanni MA, Tecce MG, MacDonald J, Hope WW et al (2017) Does prophylactic mesh placement in elective, midline laparotomy reduce the incidence of incisional hernia? A systematic review and meta-analysis. Surgery 161(4):1149–1163
Bhangu A, Fitzgerald J, Singh P, Battersby N, Marriott P, Pinkney T (2013) Systematic review and meta-analysis of prophylactic mesh placement for prevention of incisional hernia following midline laparotomy. Hernia 17(4):445–455
Bhangu A, Nepogodiev D, Ives N, Magill L, Glasbey J, Forde C et al (2020) Prophylactic biological mesh reinforcement versus standard closure of stoma site (ROCSS): a multicentre, randomised controlled trial. Lancet 395(10222):417–426
Rios-Diaz AJ, Fischer JP (2020) Stoma closure reinforcement with biological mesh and incisional hernia. The Lancet 395(10222):393–395
Mohamedahmed AYY, Stonelake S, Zaman S, Hajibandeh S (2020) Closure of stoma site with or without prophylactic mesh reinforcement: a systematic review and meta-analysis. Int J Colorectal Dis: 1–12
Bravo-Salva A, Argudo-Aguirre N, González-Castillo A, Membrilla-Fernandez E, Sancho-Insenser J, Grande-Posa L et al (2021) Long-term follow-up of prophylactic mesh reinforcement after emergency laparotomy. A retrospective controlled study. BMC Surg 21(1):1–8
Kurmann A, Barnetta C, Candinas D, Beldi G (2013) Implantation of prophylactic nonabsorbable intraperitoneal mesh in patients with peritonitis is safe and feasible. World J Surg 37(7):1656–1660
Argudo N, Pereira JA, Sancho JJ, Membrilla E, Pons MJ, Grande L (2014) Prophylactic synthetic mesh can be safely used to close emergency laparotomies, even in peritonitis. Surgery 156(5):1238–1244
Lima HV, Rasslan R, Novo FC, Lima TM, Damous SH, Bernini CO et al (2020) Prevention of fascial dehiscence with onlay prophylactic mesh in emergency laparotomy: a randomized clinical trial. J Am Coll Surg 230(1):76–87
Jakob MO, Haltmeier T, Candinas D, Beldi G (2020) Biologic mesh implantation is associated with serious abdominal wall complications in patients undergoing emergency abdominal surgery: a randomized-controlled clinical trial. J Trauma Acute Care Surg 89(6):1149–1155
Tiwari G, Dadoriya A, Thakur DS, Somashekar U, Kothari R, Agarwal P, Sharma D (2020) Prophylactic mesh placement for emergency midline laparotomy in peptic perforation peritonitis: a prospective observational study of short term results. Asian J Surg 43(2):456–457. https://doi.org/10.1016/j.asjsur.2019.11.017
Choi JJ, Palaniappa NC, Dallas KB, Rudich TB, Colon MJ, Divino CM (2012) Use of mesh during ventral hernia repair in clean-contaminated and contaminated cases: outcomes of 33,832 cases. Ann Surg 255(1):176–180
Haskins IN, Amdur RL, Lin PP, Vaziri K (2016) The use of mesh in emergent ventral hernia repair: effects on early patient morbidity and mortality. J Gastrointest Surg 20(11):1899–1903
Higgins JP, Green S, Collaboration C (2011) Cochrane handbook for systematic reviews of interventions. 2011
Moher D, Liberati A, Tetzlaff J, Altman DG (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8(5):336–341
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M et al (2000) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Oxford
Higgins JP, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD et al (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5(1):1–10
Lau J, Ioannidis JP, Schmid CH (1997) Quantitative synthesis in systematic reviews. Ann Intern Med 127(9):820–826
Nela.org.uk. NELAN. National Emergency Laparotomy Audit (NELA). Nela.org.uk.
Bansal A, Mallick MR, Jena S (2019) A study of post-operative complications of all emergency laparotomy in a tertiary care hospital within 90 days. Arch Clin Gastroenterol 5(2):015–018
Pearse RM, Moreno RP, Bauer P, Pelosi P, Metnitz P, Spies C et al (2012) Mortality after surgery in Europe: a 7 day cohort study. Lancet 380(9847):1059–1065
Peponis T, Bohnen JD, Muse S, Fuentes E, Van Der Wilden GM, Mejaddam A et al (2018) Interrupted versus continuous fascial closure in patients undergoing emergent laparotomy: a randomized controlled trial. J Trauma Acute Care Surg 85(3):459–465
Kaneko T, Funahashi K, Ushigome M, Kagami S, Goto M, Koda T et al (2019) Incidence of and risk factors for incisional hernia after closure of temporary ileostomy for colorectal malignancy. Hernia 23(4):743–748
Basta MN, Kozak GM, Broach RB, Messa CA IV, Rhemtulla I, DeMatteo RP et al (2019) Can we predict incisional hernia?: Development of a surgery-specific decision–support interface. Ann Surg 270(3):544–553
Inamdar MF, Singh AR, Inamdar N (2017) Incisional hernia: risk factors, clinical presentations, and pre-peritoneal polypropylene mesh repair. Int Surg J 4(4):1189–1194
Nho RLH, Mege D, Ouaïssi M, Sielezneff I, Sastre B (2012) Incidence and prevention of ventral incisional hernia. J Visc Surg 149(5):e3–e14
Jairam AP, Timmermans L, Eker HH, Pierik RE, van Klaveren D, Steyerberg EW et al (2017) Prevention of incisional hernia with prophylactic onlay and sublay mesh reinforcement versus primary suture only in midline laparotomies (PRIMA): 2-year follow-up of a multicentre, double-blind, randomised controlled trial. Lancet 390(10094):567–576
Strzelczyk J, Szymański D, Nowicki M, Wilczyński W, Gaszynski T, Czupryniak L (2006) Randomized clinical trial of postoperative hernia prophylaxis in open bariatric surgery. Br J Surg 93(11):1347–1350
Bevis P, Windhaber R, Lear P, Poskitt K, Earnshaw J, Mitchell D (2010) Randomized clinical trial of mesh versus sutured wound closure after open abdominal aortic aneurysm surgery. Br J Surg 97(10):1497–1502
Curro G, Centorrino T, Low V, Sarra G, Navarra G (2012) Long-term outcome with the prophylactic use of polypropylene mesh in morbidly obese patients undergoing biliopancreatic diversion. Obes Surg 22(2):279–282
Burns FA, Heywood E, Challand C, Lee MJ (2020) Is there a role for prophylactic mesh in abdominal wall closure after emergency laparotomy? A systematic review and meta-analysis. Hernia 24(3):441–447
Bondre IL, Holihan JL, Askenasy EP, Greenberg JA, Keith JN, Martindale RG, Roth JS, Liang MK, Ventral Hernia Outcomes Collaborative (2016) Suture, synthetic, or biologic in contaminated ventral hernia repair. J Surg Res. 200(2):488–494
Rosen MJ, Bauer JJ, Harmaty M et al (2017) Multicenter, prospective, longitudinal study of the recurrence, surgical site infection, and quality of life after contaminated ventral hernia repair using biosynthetic absorbable mesh: the COBRA study. Ann Surg 265(1):205–211
Atema JJ, de Vries FE, Boermeester MA (2016) Systematic review and meta-analysis of the repair of potentially contaminated and contaminated abdominal wall defects. Am J Surg 212(5):982-95e1
Kockerling F, Alam NN, Antoniou SA et al (2018) What is the evidence for the use of biologic or biosynthetic meshes in abdominal wall reconstruction? Hernia 22(2):249–269
Deerenberg EB, Harlaar JJ, Steyerberg EW, Lont HE, van Doorn HC et al (2015) Small bites versus large bites for closure of abdominal midline incisions (STITCH): a double-blind, multicentre, randomised controlled trial. Lancet 386(10000):1254–1260. https://doi.org/10.1016/S0140-6736(15)60459-7
Henriksen NA, Deerenberg EB, Venclauskas L, Fortelny RH, Miserez M, Muysoms FE (2018) Meta-analysis on materials and techniques for laparotomy closure: the MATCH review. World J Surg 42(6):1666–1678. https://doi.org/10.1007/s00268-017-4393-9
Lesch C, Kallinowski F, Uhr K, Vollmer M, Gerhard CP, Gutjahr D, Krimmel L, Ludwig Y-M (2021) Reduction of failure rates after incisional hernia repair by adding a prophylactic mesh. Brit J Surg 108(Supplement_8):znab395.050. https://doi.org/10.1093/bjs/znab395.050
Author information
Authors and Affiliations
Contributions
Conception and design: MA, AYYM, SZ. Literature search and study selection: MA, AYYM. Data collection, analysis, and interpretation: MA, AYYM, SZ. Writing the article and critical revision: all authors. Final approval of the article: all authors. Statistical analysis: AYYM, MA.
Corresponding author
Ethics declarations
Ethical approval
Considering the nature of this study, ethical approval was not required.
Human and animal rights
This study is a systematic review with meta-analysis of outcomes which does not include research directly involving human or animal participation.
Informed consent
Considering the nature of this study, informed consent was not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Mohamed Albendary and Ali Yasen Y Mohamedahmed had equal contribution in this study proposing joint first authorship.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Albendary, M., Mohamedahmed, A.Y.Y., Alamin, A. et al. Efficacy and safety of mesh closure in preventing wound failure following emergency laparotomy: a systematic review and meta-analysis. Langenbecks Arch Surg 407, 1333–1344 (2022). https://doi.org/10.1007/s00423-021-02421-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-021-02421-4