Abstract
Purpose
This study aimed to evaluate the short- and long-term outcomes in obese patients with gastric cancer undergoing totally laparoscopic total gastrectomy (TLTG) to clarify its feasibility in this population.
Methods
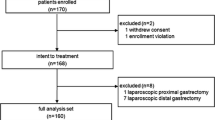
We examined 136 consecutive patients who underwent TLTG for gastric cancer (GC) between 2013 and 2018. A total of 45 patients with a body mass index (BMI) ≥ 25 kg/m2 were defined as the obese group (obese and overweight patients by the WHO classification), and 91 patients with a BMI < 25 kg/m2 were defined as the non-obese group. Short- and long-term outcomes were compared, and the correlation between obesity and postoperative complications was examined in patients who underwent TLTG.
Results
Although the operation time (min) was significantly longer in the obese group than in the non-obese group (329 vs 307, p = 0.002), there were no significant differences in the total volume of blood loss (mL) (118 vs 60, p = 0.059) or the rate of conversion to laparotomy between the two groups (2 vs 2, p = 0.466). Moreover, there was no significant difference in the incidence of postoperative complications between the two groups (16% vs 19%, p = 0.653). In the multivariate analysis, obesity was not identified as a risk factor for postoperative complications among patients who underwent TLTG. The rate of overall survival was not significantly different between the groups (p = 0.512).
Conclusion
TLTG is feasible for obese Japanese patients with GC. To validate the results of the present study, it is necessary to conduct a prospective study of a large population of patients with GC.

Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article (and its supplementary information files).
Code availability
Not applicable.
References
https://gco.iarc.fr/today/data/factsheets/populations/900-world-fact-sheets.pdf. Accessed 5 Sep 2021
Chen HK, Zhu GW, Huang YJ, Zheng W, Yang SG, Ye JX (2018) Impact of body mass index on short-term outcomes of laparoscopic gastrectomy in Asian patients: a meta-analysis. World J Clin Cases 6(15):985–94. https://doi.org/10.12998/wjcc.v6.i15.985
Zhao B, Zhang J, Mei D, Luo R, Lu H, Xu H et al (2018) Does high body mass index negatively affect the surgical outcome and long-term survival of gastric cancer patients who underwent gastrectomy: a systematic review and meta-analysis. Eur J Surg Oncol 44(12):1971–1981. https://doi.org/10.1016/j.ejso.2018.09.007
Sun L, Zhao B, Huang Y, Lu H, Luo R, Huang B (2020) Feasibility of laparoscopy gastrectomy for gastric cancer in the patients with high body mass index: a systematic review and meta-analysis. Asian J Surg 43(1):69–77. https://doi.org/10.1016/j.asjsur.2019.03.017
Li HZ, Chen JX, Zheng Y, Zhu XN (2016) Laparoscopic-assisted versus open radical gastrectomy for resectable gastric cancer: systematic review, meta-analysis, and trial sequential analysis of randomized controlled trials. J Surg Oncol 113(7):756–767. https://doi.org/10.1002/jso.24243
Chen K, Pan Y, Yu WH, Zheng XY, Zhu LH, Wang XF (2018) Application of laparoscopic gastrectomy in obese patients (BMI≥30 kg/m2) with gastric cancer: a comparison with open gastrectomy regarding short-term outcomes. Surg Laparosc Endosc Percutan Tech 28(1):e18–e23. https://doi.org/10.1097/sle.0000000000000497
Yamada H, Kojima K, Inokuchi M, Kawano T, Sugihara K (2008) Effect of obesity on technical feasibility and postoperative outcomes of laparoscopy-assisted distal gastrectomy–comparison with open distal gastrectomy. J Gastrointest Surg 12(6):997–1004. https://doi.org/10.1007/s11605-007-0374-x
Zhang GT, Liang D, Zhang XD (2013) Comparison of hand-assisted laparoscopic and open radical distal gastrectomy for obese patients. Am Surg 79(12):1273–1278
Katai H, Mizusawa J, Katayama H, Morita S, Yamada T, Bando E et al (2020) Survival outcomes after laparoscopy-assisted distal gastrectomy versus open distal gastrectomy with nodal dissection for clinical stage IA or IB gastric cancer (JCOG0912): a multicentre, non-inferiority, phase 3 randomised controlled trial. Lancet Gastroenterol Hepatol 5(2):142–151. https://doi.org/10.1016/s2468-1253(19)30332-2
Aiolfi A, Lombardo F, Matsushima K, Sozzi A, Cavalli M, Panizzo V et al (2021) Systematic review and updated network meta-analysis of randomized controlled trials comparing open, laparoscopic-assisted, and robotic distal gastrectomy for early and locally advanced gastric cancer. Surgery 170(3):942–951. https://doi.org/10.1016/j.surg.2021.04.014
van der Wielen N, Straatman J, Daams F, Rosati R, Parise P, Weitz J et al (2021) Open versus minimally invasive total gastrectomy after neoadjuvant chemotherapy: results of a European randomized trial. Gastric Cancer 24(1):258–271. https://doi.org/10.1007/s10120-020-01109-w
Katai H, Mizusawa J, Katayama H, Kunisaki C, Sakuramoto S, Inaki N et al (2019) Single-arm confirmatory trial of laparoscopy-assisted total or proximal gastrectomy with nodal dissection for clinical stage I gastric cancer: Japan Clinical Oncology Group study JCOG1401. Gastric Cancer 22(5):999–1008. https://doi.org/10.1007/s10120-019-00929-9
Tan J, Zhu S (2017) Laparoscopic gastrectomy in obese patients with gastric cancer. J BUON 22(2):410–416
Wu XS, Wu WG, Li ML, Yang JH, Ding QC, Zhang L et al (2013) Impact of being overweight on the surgical outcomes of patients with gastric cancer: a meta-analysis. World J Gastroenterol 19(28):4596–4606. https://doi.org/10.3748/wjg.v19.i27.4596
Japanese gastric cancer treatment guidelines 2010 (ver. 3) (2011) Gastric Cancer 14(2):113–23. https://doi.org/10.1007/s10120-011-0042-4
. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight. Accessed 5 Sep 2021
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383. https://doi.org/10.1016/0021-9681(87)90171-8
McMillan DC, Crozier JE, Canna K, Angerson WJ, McArdle CS (2007) Evaluation of an inflammation-based prognostic score (GPS) in patients undergoing resection for colon and rectal cancer. Int J Colorectal Dis 22(8):881–886. https://doi.org/10.1007/s00384-006-0259-6
Onodera T, Goseki N, Kosaki G (1984) Prognostic nutritional index in gastrointestinal surgery of malnourished cancer patients. Nihon Geka Gakkai Zasshi 85(9):1001–1005
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Kunisaki C, Makino H, Kimura J, Takagawa R, Ota M, Kosaka T et al (2015) Application of reduced-port laparoscopic total gastrectomy in gastric cancer preserving the pancreas and spleen. Gastric Cancer 18(4):868–875. https://doi.org/10.1007/s10120-014-0441-4
Chen H, Sui W (2017) Influence of obesity on short- and long-term outcomes after laparoscopic distal gastrectomy for gastric cancer. J BUON 22(2):417–423
Chen K, Pan Y, Zhai ST, Cai JQ, Chen QL, Chen DW et al (2017) Laparoscopic gastrectomy in obese gastric cancer patients: a comparative study with non-obese patients and evaluation of difference in laparoscopic methods. BMC Gastroenterol 17(1):78. https://doi.org/10.1186/s12876-017-0638-1
Flegal KM, Kit BK, Orpana H, Graubard BI (2013) Association of all-cause mortality with overweight and obesity using standard body mass index categories: a systematic review and meta-analysis. JAMA 309(1):71–82. https://doi.org/10.1001/jama.2012.113905
Jung JH, Ryu SY, Jung MR, Park YK, Jeong O (2014) Laparoscopic distal gastrectomy for gastric cancer in morbidly obese patients in South Korea. J Gastric Cancer 14(3):187–195. https://doi.org/10.5230/jgc.2014.14.3.187
Liu M, Xing J, Arslan A, Tan F, Fan Y, Xu K et al (2019) Safety and efficacy of laparoscopic gastrectomy in obese patients with gastric cancer. Medicine (Baltimore) 98(47):e17991. https://doi.org/10.1097/md.0000000000017991
Noshiro H, Shimizu S, Nagai E, Ohuchida K, Tanaka M (2003) Laparoscopy-assisted distal gastrectomy for early gastric cancer: is it beneficial for patients of heavier weight? Ann Surg 238(5):680–685. https://doi.org/10.1097/01.sla.0000094302.51616.2a
Shimada S, Sawada N, Ishiyama Y, Nakahara K, Maeda C, Mukai S et al (2018) Impact of obesity on short- and long-term outcomes of laparoscopy assisted distal gastrectomy for gastric cancer. Surg Endosc 32(1):358–366. https://doi.org/10.1007/s00464-017-5684-9
Sugimoto M, Kinoshita T, Shibasaki H, Kato Y, Gotohda N, Takahashi S et al (2013) Short-term outcome of total laparoscopic distal gastrectomy for overweight and obese patients with gastric cancer. Surg Endosc 27(11):4291–4296. https://doi.org/10.1007/s00464-013-3045-x
Tsujiura M, Hiki N, Ohashi M, Nunobe S, Kumagai K, Ida S et al (2019) Should pylorus-preserving gastrectomy be performed for overweight/obese patients with gastric cancer? Gastric Cancer 22(6):1247–1255. https://doi.org/10.1007/s10120-019-00951-x
Kim HS, Kim BS, Lee S, Lee IS, Yook JH, Kim BS (2013) Reconstruction of esophagojejunostomies using endoscopic linear staplers in totally laparoscopic total gastrectomy: report of 139 cases in a large-volume center. Surg Laparosc Endosc Percutan Tech 23(6):e209–e216. https://doi.org/10.1097/SLE.0b013e31828e3b79
Bracale U, Marzano E, Nastro P, Barone M, Cuccurullo D, Cutini G et al (2010) Side-to-side esophagojejunostomy during totally laparoscopic total gastrectomy for malignant disease: a multicenter study. Surg Endosc 24(10):2475–2479. https://doi.org/10.1007/s00464-010-0988-z
Tsunoda S, Okabe H, Obama K, Tanaka E, Hisamori S, Kinjo Y et al (2014) Short-term outcomes of totally laparoscopic total gastrectomy: experience with the first consecutive 112 cases. World J Surg 38(10):2662–2667. https://doi.org/10.1007/s00268-014-2611-2
Kunisaki C, Makino H, Takagawa R, Sato K, Kawamata M, Kanazawa A et al (2009) Predictive factors for surgical complications of laparoscopy-assisted distal gastrectomy for gastric cancer. Surg Endosc 23(9):2085–2093. https://doi.org/10.1007/s00464-008-0247-8
World Health Organization (2000) The Asia-Pacific Perspective: Redefining Obesity and Its Treatment. https://apps.who.int/iris/bitstream/handle/10665/206936/0957708211_eng.pdf. Accessed 5 Sep 2021.
Author information
Authors and Affiliations
Contributions
Study conception and design: All authors contributed to the conception and design of this study. Acquisition: Data collection was performed by H.S., C.K., H.M., K.S., S.S., Y.T., and T.K. Analysis and interpretation of data: The data was analyzed by H.S., C.K., H.M., K.S., S.S., Y.T., AND T.K. and interpreted by H.S., C.K., N.Y., Y.R., I.E., and M.M. Drafting of manuscript: H.S. and C.K. were responsible for manuscript preparation. Critical revision of manuscript: This paper has been revised and approved by all authors.
Corresponding author
Ethics declarations
Ethics approval
This study was conducted in compliance with the principles of the Declaration of Helsinki. The study protocol was approved by the Yokohama City University Institutional Review Board (B200800017).
Consent to participate
Informed consent was obtained from all the patients.
Consent for publication
The participant has consented to the submission of the case report to the journal.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Suematsu, H., Kunisaki, C., Miyamato, H. et al. Feasibility of totally laparoscopic total gastrectomy in obese patients with gastric cancer. Langenbecks Arch Surg 407, 999–1008 (2022). https://doi.org/10.1007/s00423-021-02369-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-021-02369-5