Abstract
Background
Percutaneous transhepatic cholangioscopic lithotripsy (PTCSL) provides an alternative method for cholelithiasis treatment. Since conventional rigid choledochoscope applied in PTCSL lacks high flexibility and high-resolution vision, we developed a new, soft fiber-optic choledochoscope (SFCS) to solve these problems.
Objective
We aim to verify the safety and efficacy of PTCSL guided by the newly developed choledochoscope, SCFS.
Methods
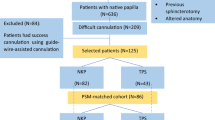
In this study, a total of 58 patients undergoing PTCSL from November, 2020 to December, 2020 in Zhuhai People’s Hospital were enrolled, including 32 patients undergoing conventional PTCSL and 26 patients undergoing SFCS-guided PTCSL. A method of propensity score matching was used in order to balance the pre-operative indexes of the two groups. As a result, a total of 21 pairs (1:1) were created. SFCS-guided PTCSL was performed on patients in the SFCS group for the treatment of cholelithiasis. The operation time, intraoperative blood loss, immediate clearance rate, final clearance rate, postoperative hospitalization time, postoperative complication rate, and recurrence rate were compared between the two groups. A 6-month follow-up was performed for the two groups.
Results
SFCS-guided PTCSL represents safe and effective treatment outcomes. The immediate clearance rate and final clearance rate in the SFCS group were significantly higher than that of the conventional group. Operation time, intraoperative blood loss, postoperative hospitalization days, and recurrence rate in the SFCS group were significantly lower than that of the conventional group.
Conclusions
SFCS applied in PTCSL appears to be a safe and effective method for the treatment of cholelithiasis.
This study has been registered in Chinese Clinical Trial Registry as required by legislation (Registration number: ChiCTR1800016864, Registration time: 2018/02/08).



Similar content being viewed by others
Data availability
All the data could be accessed via the email address of the corresponding author.
References
Park JS, Jeong S, Lee DH, Bang BW, Lee JI, Lee JW et al (2013) Risk factors for long-term outcomes after initial treatment in hepatolithiasis. J Korean Med Sci 28:1627–1631
Suzuki Y, Mori T, Yokoyama M, Yang CC, Yeh YH, Chou DA et al (2014) Hepatolithiasis: analysis of Japanese nationwide surveys over a period of 40 years. J HepatobiliaryPancreat Sci 21:617–622
Silsirivanit A, Sawanyawisuth K, Riggin GJ, Wongkham C (2014) Cancer biomarker discovery for cholangiocarcinoma: the high-throughput approaches. J Hepatobiliary Pancreat Sci 21:388
Kim HJ, Kim JS, Suh SJ, Lee BJ, Park JJ, Lee HS et al (2015) Cholangiocarcinoma risk as longterm outcome after hepatic resection in the hepatolithiasis patients. World J Surg 39:1537–1542
Zeng X, Tao H (2015) Diagnostic and prognostic serum marker of cholangiocarcinoma. Oncol Lett 9:3
Sato Y, Sasaki M, Harada K, Nakanuma Y (2014) Pathological diagnosis of flat epithelial lesions of the biliary tract with emphasis on biliary intraductalneoplasia. J Gastroenterol 49:64–72
Yang J, Huang Q, Lin XS (2014) The analysis on the methods and curative effect of iatrogenic bile duct injury reparation operation: a clinicol analysis of 102 cases. J Hepatobiliary Surg 79(3):585–590
Miura F, Takada T, Strasberg SM, Solomkin JS, Pitt HA, Gouma DJ et al (2013) TG13 flowchart for the management of acute cholangitis and cholecystitis. J Hepatobiliary Pancreat Sci 20:47–64
Wei LJ, Wei CT, Xing YX (2013) The clinical experience of endoscopic minimally invasive gallbladder-sparing cholelithotomy: with a report of 56 cases. Journal of Laparoseopic Surgery 24(8):666–669
Osipenko MF, Litvinova NV, Voloshina NB, Frolov IaA (2013) Long-term dynamics of gastrointestinal symptoms after cholecystectomy for the treatment of cholelithiasis. KlinMed(Mosk) 91(5):49–52
Ye X, Ni K, Zhou X, Xie K, Hong X (2015) Laparoscopic versus open left hemihepatectomy for hepatolithiasis. J Surg Res 199:402–406
Lee JH, Kim HW, Kang DH, Choi CW, Park SB, Kim SH et al (2013) Usefulness of percutaneous transhepaticcholangioscopic lithotomy for removal of difficult common bile duct stones. Clin Endosc 46:65–70
Koc B, Karahan S, Adas G, Cheng B, Jin X (2013) Comparison of laparoscopic common bile duct exploration an d endoscopic retrograde cholangiopancreatography plus laparoscopic cholecystectomy for choledocholithiasis: a prospective randomized study. Am J Surg 206:457–463
Narayanan SK, Chen Y, Narasimhan KL, Cohen RC (2013) Hepaticoduodenostomy versus hepaticojejunostomy after resection of choledochal cyst: a systematic review and meta-analysis. J PediatrSurg 48(11):2336–2342
Jin H, Fan J, Li W, Cui M (2019) Percutaneous transhepatic cholangioscopic lithotripsy using soft fiber-optic choledochoscope. Z Gastroenterol 57(10):1196–1199
Tian J, Li JW, Chen J, Fan YD, Bie P, Wang SG (2013) Laparoscopic hepatectomy with bile duct exploration for the treatment of hepatolithiasis: an experience of 116 cases. Dig Liver Dis 45:493
Yasuda I, Itoi T (2013) Recent advances in endoscopic management of difficult bile duct stones. Dig Endosc 25:376–385
Chen YY, Chen CC (2017) Cholelithiasis New England J Med 377(4):371
Lee JH, Kim HW, Kang DH, Choi CW, Park SB, Kim SH, Jeon UB (2013) Usefulness of percutaneous transhepatic cholangioscopic lithotomy for removal of difficult common bile duct stones. Clin Endosc 46(1):65–70
Zhuo H, Chen Z, Lin R, Yang S, Zhuang H, He C, Liu X (2020) Percutaneous Transhepatic Choledochoscopic Lithotomy (PTCSL) is effective for the treatment of intrahepatic and extrahepatic choledocholithiasis. Surg Laparosc Endosc Percutan Tech 31(3):326–330
Wang P, Tao H, Liu C, Zhou X, Sun B, Zhu C et al (2021) One-step percutaneous transhepatic cholangioscopic lithotripsy in patients with cholelithiasis. Clin Res Hepatol Gastroenterol 45(2):101477
Uchiyama K, Kawai M, Ueno M, Ozawa S, Tani M, Yamaue H (2007) Reducing residual and recurrent stones by hepatectomy for hepatolithiasis. J Gastrointest Surg 11(5):626–630
Acknowledgements
We thank Zhuhai People’s Hospital (Zhuhai hospital affiliated with Jinan University) for providing the necessary support for our study.
Funding
The study was funded by the Medical Research Program of Guangdong Provincial Health Bureau (Grant No. 2020424).
Author information
Authors and Affiliations
Contributions
Cui M proposed the study. Cui M and Jin H performed the research and wrote the first draft. Both authors contributed to the design and interpretation of the study and to further drafts. Cui M is the guarantor.
Corresponding author
Ethics declarations
Ethics approval
Our study has been approved by the Ethical Committee of Zhuhai People’s Hospital (No. 2019–6). All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional review boards of Zhuhai People’s Hospital (Zhuhai, China) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study has been registered in the Chinese Clinical Trial Registry as required by legislation (Registration number: ChiCTR1800016864).
Consent to participate
Informed consent was obtained from the individual participant included in the study.
Consent for publication
The participants gave consent for his personal and clinical details along with any identifying images to be published in this study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jin, H., Cui, M. A propensity score matching study between conventional and soft fiber-optic choledochoscope guided percutaneous transhepatic cholangioscopic lithotripsy for treatment of cholelithiasis. Langenbecks Arch Surg 407, 675–683 (2022). https://doi.org/10.1007/s00423-021-02359-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-021-02359-7