Abstract
Purpose
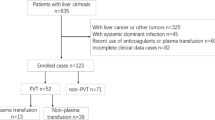
Portal vein thrombosis (PVT) following hepatectomy is potentially life-threatening. We aimed to evaluate the incidence of PVT after hepatectomy for hepatocellular carcinoma and identify coagulation and fibrinolytic factors that could predict early-stage postoperative PVT.
Methods
A retrospective analysis was conducted on 65 hepatocellular carcinoma patients who underwent radical hepatectomy. The risk factors for postoperative PVT were identified based on univariate and multivariate analyses, and the levels of coagulation and fibrinolytic factors were measured during the perioperative period.
Results
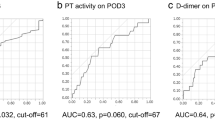
The incidence of PVT after hepatectomy was 20.0%. The patients were divided into two groups: those with PVT (n=13; PVT group) and those without PVT (n=52; no-PVT group). The frequency of the use of the Pringle maneuver during surgery was higher in the PVT group than in the no-PVT group, and the postoperative/preoperative ratios of thrombin-antithrombin III complex (TAT) and of D-dimer were significantly higher in the PVT group.
Conclusion
A high incidence of PVT was found in hepatocellular carcinoma patients after hepatectomy. The frequency of the Pringle maneuver is a potential risk factor for postoperative PVT, and the postoperative/preoperative TAT and D-dimer ratios may be used as early predictors of PVT after hepatectomy for hepatocellular carcinoma.


Similar content being viewed by others
Data Availability
Data is available on request from the corresponding author.
References
Valla DC, Condat B (2000) Portal vein thrombosis in adults: pathophysiology, pathogenesis and management. J Hepatol 32(5):865–871. https://doi.org/10.1016/s0168-8278(00)80259-7
Tsochatzis EA, Senzolo M, Germani G, Gatt A, Burroughs AK (2010) Systematic review: portal vein thrombosis in cirrhosis. Aliment Pharmacol Ther 31(3):366–374. https://doi.org/10.1111/j.1365-2036.2009.04182.x
Lisman T, Kamphuisen PW, Northup PG, Porte RJ (2013) Established and new-generation antithrombotic drugs in patients with cirrhosis - possibilities and caveats. J Hepatol 59(2):358–366. https://doi.org/10.1016/j.jhep.2013.03.027
Yoshida H, Taniai N, Yoshioka M, Hirakata A, Kawano Y, Shimizu T, Ueda J, Takata H, Nakamura Y, Mamada Y (2019) Current status of laparoscopic hepatectomy. J Nippon Med Sch 86(4):201–206. https://doi.org/10.1272/jnms.JNMS.2019_86-411
Yoshiya S, Shirabe K, Nakagawara H, Soejima Y, Yoshizumi T, Ikegami T, Yamashita Y, Harimoto N, Nishie A, Yamanaka T, Maehara Y (2014) Portal vein thrombosis after hepatectomy. World J Surg 38(6):1491–1497. https://doi.org/10.1007/s00268-013-2440-8
Kuboki S, Shimizu H, Ohtsuka M, Kato A, Yoshitomi H, Furukawa K, Takayashiki T, Takano S, Okamura D, Suzuki D, Sakai N, Kagawa S, Miyazaki M (2015) Incidence, risk factors, and management options for portal vein thrombosis after hepatectomy: a 14-year, single-center experience. Am J Surg 210(5):878–885.e872. https://doi.org/10.1016/j.amjsurg.2014.11.021
Han JH, Kim DS, Yu YD, Jung SW, Yoon YI, Jo HS (2019) Analysis of risk factors for portal vein thrombosis after liver resection. Ann Surg Treat Res 96(5):230–236. https://doi.org/10.4174/astr.2019.96.5.230
Onda S, Furukawa K, Shirai Y, Hamura R, Horiuchi T, Yasuda J, Shiozaki H, Gocho T, Shiba H, Ikegami T New classification-oriented treatment strategy for portal vein thrombosis after hepatectomy. Annals of Gastroenterological Surgery n/a (n/a). https://doi.org/10.1002/ags3.12383
Chawla YK, Bodh V (2015) Portal vein thrombosis. J Clin Exp Hepatol 5(1):22–40. https://doi.org/10.1016/j.jceh.2014.12.008
Bach AM, Hann LE, Brown KT, Getrajdman GI, Herman SK, Fong Y, Blumgart LH (1996) Portal vein evaluation with US: comparison to angiography combined with CT arterial portography. Radiology 201(1):149–154. https://doi.org/10.1148/radiology.201.1.8816536
Fei Y, Zong GQ, Chen J, Liu RM (2015) Evaluation the value of markers for prediction of portal vein thrombosis after devascularization. Ann Hepatol 14(6):856–861. https://doi.org/10.5604/16652681.1171772
Zhang D, Hao J, Yang N (2010) Protein C and D-dimer are related to portal vein thrombosis in patients with liver cirrhosis. J Gastroenterol Hepatol 25(1):116–121. https://doi.org/10.1111/j.1440-1746.2009.05921.x
Strasberg SM (2005) Nomenclature of hepatic anatomy and resections: a review of the Brisbane 2000 system. J Hepatobiliary Pancreat Surg 12(5):351–355. https://doi.org/10.1007/s00534-005-0999-7
Reddy SK, Barbas AS, Turley RS, Steel JL, Tsung A, Marsh JW, Geller DA, Clary BM (2011) A standard definition of major hepatectomy: resection of four or more liver segments. HPB (Oxford) 13(7):494–502. https://doi.org/10.1111/j.1477-2574.2011.00330.x
Seyama Y, Kokudo N (2009) Assessment of liver function for safe hepatic resection. Hepatology Research 39(2):107–116. https://doi.org/10.1111/j.1872-034X.2008.00441.x
Ueda J, Mamada Y, Taniai N, Yoshioka M, Hirakata A, Kawano Y, Shimizu T, Kanda T, Takata H, Kondo R, Kaneya Y, Aoki Y, Yoshida H (2020) Massage of the hepatoduodenal ligament recovers portal vein flow immediately after the Pringle maneuver in hepatectomy. World J Surg. https://doi.org/10.1007/s00268-020-05570-7
Nonami T, Yokoyama I, Iwatsuki S, Starzl TE (1992) The incidence of portal vein thrombosis at liver transplantation. Hepatology 16(5):1195–1198
Bianchini M, De Pietri L, Villa E (2014) Coagulopathy in liver diseases: complication or therapy? Dig Dis 32(5):609–614. https://doi.org/10.1159/000360514
Kalambokis GN, Oikonomou A, Baltayiannis G, Christou L, Kolaitis NI, Tsianos EV (2016) Thrombin generation measured as thrombin-antithrombin complexes predicts clinical outcomes in patients with cirrhosis. Hepatol Res 46(3):E36–E44. https://doi.org/10.1111/hepr.12520
Tomiya T, Fujiwara K (1991) Plasma thrombin-antithrombin III complexes in the diagnosis of primary hepatocellular carcinoma complicating liver cirrhosis. Cancer 67(2):481–485. https://doi.org/10.1002/1097-0142(19910115)67:2<481::aid-cncr2820670227>3.0.co;2-j
Cohen J, Edelman RR, Chopra S (1992) Portal vein thrombosis: a review. Am J Med 92(2):173–182. https://doi.org/10.1016/0002-9343(92)90109-o
Zhang ZY, Dong KS, Zhang EL, Huang ZY, Chen XP, Dong HH (2018) Acute portal vein thrombosis after hepatectomy in a patient with hepatolithiasis: a case report and review of the literature. Medicine (Baltimore) 97(25):e11174. https://doi.org/10.1097/md.0000000000011174
Thomas RM, Ahmad SA (2010) Management of acute post-operative portal venous thrombosis. J Gastrointest Surg 14(3):570–577. https://doi.org/10.1007/s11605-009-0967-7
Hoek JA, Sturk A, ten Cate JW, Lamping RJ, Berends F, Borm JJ (1988) Laboratory and clinical evaluation of an assay of thrombin-antithrombin III complexes in plasma. Clin Chem 34(10):2058–2062
Nakagawa K, Watanabe J, Suwa Y, Suzuki S, Ishibe A, Ota M, Kunisaki C, Endo I (2019) Clinical analysis of preoperative deep vein thrombosis risk factors in patients with colorectal cancer: retrospective observational study. Ann Gastroenterol Surg 3(4):451–458. https://doi.org/10.1002/ags3.12256
Malaguarnera M, Latteri S, Bertino G, Madeddu R, Catania VE, Curro G, Borzi AM, Drago F, Malaguarnera G (2018) D-dimer plasmatic levels as a marker for diagnosis and prognosis of hepatocellular carcinoma patients with portal vein thrombosis. Clin Exp Gastroenterol 11:373–380. https://doi.org/10.2147/ceg.S172663
Takeda S, Katoh H, Takaki A, Okamoto K, Ohsato K (1990) Increased fibrin/fibrinogen degradation products without increase of plasmin-alpha 2-plasmin inhibitor complex after hepatectomy for hepatocellular carcinoma. Thromb Res 57(2):289–300. https://doi.org/10.1016/0049-3848(90)90328-a
Acknowledgements
We would like to thank Editage (http://www.editage.jp) for English language editing.
Code availability
Not applicable.
Author information
Authors and Affiliations
Contributions
Study conception and design: Hideyuki Takata, Atsushi Hirakata, Junji Ueda, and Hiroshi Yoshida. Acquisition of data: Hideyuki Takata, Atsushi Hirakata, Junji Ueda, Tadashi Yokoyama, Hiroshi Maruyama, Nobuhiko Taniai, Ryotaro Takano, and Takahiro Haruna. Analysis and interpretation of data: Hideyuki Takata, Atsushi Hirakata, Junji Ueda, and Hiroshi Makino. Drafting of manuscript: Hideyuki Takata. Critical revision of manuscript: Hiroshi Yoshida.
Corresponding author
Ethics declarations
Ethics approval
This study was carried out under the principles embodied in the Declaration of Helsinki, 2013, and was approved by the institutional review board of the Nippon Medical School Tama Nagayama Hospital (Approval number: 627).
Consent to participate
Informed consent was obtained from all individual patients included in the study.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Fig. 1
Time-course changes of the ratio of the postoperative to the preoperative values of coagulation and fibrinolytic factors. (a) PIC. (b) Total PAI-1. (c) platelet count. (d) PT activity. (e) APTT. (f) AT-III activity. (PNG 977 kb)
Rights and permissions
About this article
Cite this article
Takata, H., Hirakata, A., Ueda, J. et al. Prediction of portal vein thrombosis after hepatectomy for hepatocellular carcinoma. Langenbecks Arch Surg 406, 781–789 (2021). https://doi.org/10.1007/s00423-021-02125-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-021-02125-9