Abstract
Purpose
Pseudoaneurysm (PA) after pancreaticoduodenectomy (PD) is a harmful complication due to postoperative pancreatic fistula. However, the preventive method for PA is unclear. This study aimed to assess the risk factors for PA after PD and to evaluate the clinical features of patients with PA.
Methods
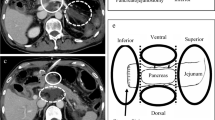
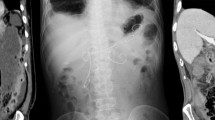
Medical records of 54 patients who underwent PD and developed clinically relevant postoperative pancreatic fistula (POPF) were retrospectively reviewed. We evaluated postoperative computed tomography (CT) findings, including the perianastomotic fluid collection (PFC) location on postoperative day 4. Perioperative findings and postoperative CT findings were compared between patients with and without PA after PD.
Results
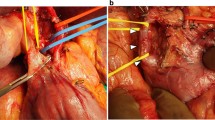
The PA group included nine patients (17%). The median postoperative day of diagnosis of PA was 17 (range, 7–33). The PA locations were the gastroduodenal artery stump (n = 3), dorsal pancreatic artery (DPA) stump from the common hepatic artery (n = 4), DPA stump from the replaced right hepatic artery (n = 1), and inferior pancreaticoduodenal artery stump (n = 1). The prevalence of falciform ligament wrap to the hepatic artery was lower (33% vs. 78%, p = 0.014) and superior PFC prevalence was higher (100% vs. 58%, p = 0.019) in the PA group than in the non-PA group. Superior PFC reached the dorsal part of the caudate lobe of the liver in all patients with PA. Furthermore, all PAs occurred at the arteries that could not be wrapped by the falciform ligament.
Conclusion
Prevention of superior PFC and falciform ligament wrapping may reduce PA occurrence after PD with clinically relevant POPF.


Similar content being viewed by others
References
Buchler MW, Friess H, Wagner M, Kulli C, Wagener V, Z’Graggen K (2000) Pancreatic fistula after pancreatic head resection. Br J Surg 87:883–889. https://doi.org/10.1046/j.1365-2168.2000.01465.x
Munoz-Bongrand N, Sauvanet A, Denys A, Sibert A, Vilgrain V, Belghiti J (2004) Conservative management of pancreatic fistula after pancreaticoduodenectomy with pancreaticogastrostomy. J Am Coll Surg 199:198–203. https://doi.org/10.1016/j.jamcollsurg.2004.03.015
DeOliveira ML, Winter JM, Schafer M et al (2006) Assessment of complications after pancreatic surgery: a novel grading system applied to 633 patients undergoing pancreaticoduodenectomy. Ann Surg 244:931–937. https://doi.org/10.1097/01.sla.0000246856.03918.9a
Hashimoto Y, Traverso LW (2010) Incidence of pancreatic anastomotic failure and delayed gastric emptying after pancreaticoduodenectomy in 507 consecutive patients: use of a web-based calculator to improve homogeneity of definition. Surgery 147:503–515. https://doi.org/10.1016/j.surg.2009.10.034
Kawai M, Kondo S, Yamaue H, Wada K, Sano K, Motoi F, Unno M, Satoi S, Kwon AH, Hatori T, Yamamoto M, Matsumoto J, Murakami Y, Doi R, Ito M, Miyakawa S, Shinchi H, Natsugoe S, Nakagawara H, Ohta T, Takada T (2011) Predictive risk factors for clinically relevant pancreatic fistula analyzed in 1,239 patients with pancreaticoduodenectomy: multicenter data collection as a project study of pancreatic surgery by the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J Hepatobiliary Pancreat Sci 18:601–608. https://doi.org/10.1007/s00534-011-0373-x
Choi SH, Moon HJ, Heo JS, Joh JW, Kim YI (2004) Delayed hemorrhage after pancreaticoduodenectomy. J Am Coll Surg 199:186–191. https://doi.org/10.1016/j.jamcollsurg.2004.04.005
Welsch T, Eisele H, Zschäbitz S, Hinz U, Büchler MW, Wente MN (2011) Critical appraisal of the International Study of Pancreatic Surgery (ISGPS) consensus definition of postoperative hemorrhage after pancreaticoduodenectomy. Langenbeck’s Arch Surg 396:783–791. https://doi.org/10.1007/s00423-011-0811-x
Roulin D, Cerantola Y, Demartines N, Schäfer M (2011) Systematic review of delayed postoperative hemorrhage after pancreatic resection. J Gastrointest Surg 15:1055–1062. https://doi.org/10.1007/s11605-011-1427-8
Hasegawa H, Takahashi A, Kakeji Y, Ueno H, Eguchi S, Endo I, Sasaki A, Takiguchi S, Takeuchi H, Hashimoto M, Horiguchi A, Masaki T, Marubashi S, Yoshida K, Konno H, Gotoh M, Miyata H, Seto Y (2019) Surgical outcomes of gastroenterological surgery in Japan: report of the National Clinical Database 2011–2017. Ann Gastroenterol Surg 3:426–450. https://doi.org/10.1002/ags3.12258
Rumstadt B, Schwab M, Korth P, Samman M, Trede M (1998) Hemorrhage after pancreatoduodenectomy. Ann Surg 227:236–241. https://doi.org/10.1097/00000658-199802000-00013
Lee HG, Heo JS, Choi SH, Choi DW (2010) Management of bleeding from pseudoaneurysms following pancreaticoduodenectomy. World J Gastroenterol 16:1239–1244. https://doi.org/10.3748/wjg.v16.i10.1239
de Castro SM, Kuhlmann KF, Busch OR et al (2005) Delayed massive hemorrhage after pancreatic and biliary surgery: embolization or surgery? Ann Surg 241:85–91. https://doi.org/10.1097/01.sla.0000150169.22834.13
Darnis B, Lebeau R, Chopin-Laly X, Adham M (2013) Postpancreatectomy hemorrhage (PPH): predictors and management from a prospective database. Langenbeck’s Arch Surg 398:441–448. https://doi.org/10.1007/s00423-013-1047-8
Ray S, Sanyal S, Ghatak S, Sonar PK, Das S, Khamrui S, Chattopadhyay G (2016) Falciform ligament flap for the protection of the gastroduodenal artery stump after pancreaticoduodenectomy: a single center experience. J Visc Surg 153:9–13. https://doi.org/10.1016/j.jviscsurg.2015.10.007
Xu C, Yang X, Luo X et al (2014) “Wrapping the gastroduodenal artery stump” during pancreatoduodenectomy reduced the stump hemorrhage incidence after operation. Chin J Cancer Res 26:299–308. https://doi.org/10.3978/j.issn.1000-9604.2014.06.08
Andreasi V, Partelli S, Crippa S, Balzano G, Tamburrino D, Muffatti F, Belfiori G, Cirocchi R, Falconi M (2020) A systematic review and meta-analysis on the role of omental or falciform ligament wrapping during pancreaticoduodenectomy. HPB 22:1227–1239. https://doi.org/10.1016/j.hpb.2020.05.003
Tani M, Kawai M, Hirono S et al (2012) Use of omentum or falciform ligament does not decrease complications after pancreaticoduodenectomy: nationwide survey of the Japanese Society of Pancreatic Surgery. Surgery 151:183–191. https://doi.org/10.1016/j.surg.2011.07.023
Müssle B, Wierick A, Distler M, Weitz J, Welsch T (2017) Falciform ligament wrap for prevention of gastroduodenal artery bleed after pancreatoduodenectomy. J Surg Res 207:215–222. https://doi.org/10.1016/j.jss.2016.08.087
Bassi C, Marchegiani G, Dervenis C, Sarr M, Abu Hilal M, Adham M, Allen P, Andersson R, Asbun HJ, Besselink MG, Conlon K, del Chiaro M, Falconi M, Fernandez-Cruz L, Fernandez-del Castillo C, Fingerhut A, Friess H, Gouma DJ, Hackert T, Izbicki J, Lillemoe KD, Neoptolemos JP, Olah A, Schulick R, Shrikhande SV, Takada T, Takaori K, Traverso W, Vollmer CR, Wolfgang CL, Yeo CJ, Salvia R, Buchler M (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery 161:584–591. https://doi.org/10.1016/j.surg.2016.11.014
Koch M, Garden OJ, Padbury R et al (2011) Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the International Study Group of Liver Surgery. Surgery 149:680–688. https://doi.org/10.1016/j.surg.2010.12.002
Maehira H, Iida H, Matsunaga T, Yasukawa D, Mori H, Miyake T, Tani M (2020) The location of perianastomotic fluid collection predicts postoperative complications after pancreaticoduodenectomy. Langenbeck’s Arch Surg 405:325–336. https://doi.org/10.1007/s00423-020-01880-5
Kanda Y (2013) Investigation of the freely available easy-to use software ‘EZR’ for medical statistics. Bone Marrow Transplant 48:452–458. https://doi.org/10.1038/bmt.2012.244
Hashimoto M, Koga M, Ishiyama K, Watarai J, Shibata S, Sato T, Yamamoto Y (2007) CT features of pancreatic fistula after pancreaticoduodenectomy. Am J Roentgenol 188:W323–W327. https://doi.org/10.2214/AJR.05.1174
Bruno O, Brancatelli G, Sauvanet A, Vullierme MP, Barrau V, Vilgrain V (2009) Utility of CT in the diagnosis of pancreatic fistula after pancreaticoduodenectomy in patients with soft pancreas. Am J Roentgenol 193:W175–W180. https://doi.org/10.2214/AJR.08.1800
Hirono S, Kawai M, Okada K et al (2019) Modified blumgart mattress suture versus conventional interrupted suture in pancreaticojejunostomy during pancreaticoduodenectomy. Ann Surg 269:243–251. https://doi.org/10.1097/SLA.0000000000002802
Hirashita T, Iwashita Y, Fujinaga A, Nakanuma H, Tada K, Masuda T, Endo Y, Ohta M, Inomata M (2020) Short internal pancreatic stent reduces pancreatic fistula in pancreatoduodenectomy. Langenbeck’s Arch Surg. https://doi.org/10.1007/s00423-020-02036-1
Kawai M, Yamaue H, Jang JY, Uesaka K, Unno M, Nakamura M, Fujii T, Satoi S, Choi SH, Sho M, Fukumoto T, Kim SC, Hong TH, Izumo W, Yoon DS, Amano R, Park SJ, Choi SB, Yu HC, Kim JS, Ahn YJ, Kim H, Ashida R, Hirono S, Heo JS, Song KB, Park JS, Yamamoto M, Shimokawa T, Kim SW (2020) Propensity score-matched analysis of internal stent vs external stent for pancreatojejunostomy during pancreaticoduodenectomy: Japanese-Korean cooperative project. Pancreatology 20:984–991. https://doi.org/10.1016/j.pan.2020.06.014
Hirono S, Shimokawa Y, Nagakawa Y et al (2020) Risk factors for pancreatic fistula grade C after pancreatoduodenectomy: a large prospective, multicenter Japan-Taiwan collaboration study. J Hepatobiliary Pancreat Sci 27:622–631. https://doi.org/10.1002/jhbp.799
Senda Y, Shimizu Y, Natsume, et al. (2018) Randomized clinical trial of duct-to-mucosa versus invagination pancreaticojejunostomy after pancreatoduodenectomy. Br J Surg 105:48–57. https://doi.org/10.1002/bjs.10727
Jang JY, Chang YR, Kim SW, Choi SH, Park SJ, Lee SE, Lim CS, Kang MJ, Lee H, Heo JS (2016) Randomized multicentre trial comparing external and internal pancreatic stenting during pancreaticoduodenectomy. Br J Surg 103:668–675. https://doi.org/10.1002/bjs.10160
Figueras J, Sabater L, Planellas P, Muñoz-Forner E, Lopez-Ben S, Falgueras L, Sala-Palau C, Albiol M, Ortega-Serrano J, Castro-Gutierrez E (2013) Randomized clinical trial of pancreaticogastrostomy versus pancreaticojejunostomy on the rate and severity of pancreatic fistula after pancreaticoduodenectomy. Br J Surg 100:1597–1605. https://doi.org/10.1002/bjs.9252
Lee JH, Hwang DW, Lee SY, Hwang JW, Song DK, Gwon DI, Shin JH, Ko GY, Park KM, Lee YJ (2012) Clinical features and management of pseudoaneurysmal bleeding after pancreatoduodenectomy. Am Surg 78:309–317
Author information
Authors and Affiliations
Contributions
Study conception and design: H. Maehira described and designed the manuscript. Acquisition of data: H. Maehira and H. Mori reviewed the computed tomography findings. H. Maehira performed the data analysis and interpretation. D. Yasukawa, T. Maekawa, K. Muramoto, K. Takebayashi, S. Kaida, and T. Miyake performed the surgery and postoperative management. Analysis and interpretation of data: H. Maehira. Drafting of manuscript: H. Maehira. Critical revision of manuscript: M. Tani and H. Iida revised the manuscript. All the authors have approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (ethics committee of Shiga University of Medical Science (registration number 29-170)) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maehira, H., Iida, H., Mori, H. et al. Superior perianastomotic fluid collection in the early postoperative period affects pseudoaneurysm occurrence after pancreaticoduodenectomy. Langenbecks Arch Surg 406, 1461–1468 (2021). https://doi.org/10.1007/s00423-020-02072-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-020-02072-x