Abstract
Background
Clostridium difficile is an increasingly common source of in-patient morbidity and mortality. We aim to assess the effects of diverting loop ileostomy (DLI) versus total abdominal colectomy (TAC) for Clostridium difficile colitis (CDC), in terms of mortality and morbidity.
Methods
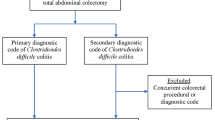
Systematic literature search was performed using PubMed, Embase, Cochrane, and Web of Science databases for randomized and non-randomized studies comparing DLI and TAC for fulminant CDC. Meta-analysis was carried out for mortality and postoperative complications.
Results
Five non-randomized studies qualified for inclusion in the quantitative synthesis. In total, 3683 patients were allocated to DLI (n = 733) or TAC (n = 2950). The overall mortality was equivalent (OR 0.73; 95% CI 0.45–1.20; P = 0.22). Regarding secondary outcomes, the pooled analysis revealed the following equivalent rates of postoperative events: thromboembolism (OR 0.45; 95% CI 0.14–1.43; P = 0.18), acute renal failure (OR 1.71; 95% CI 0.91–3.23; P = 0.10), surgical site infection (OR 0.95; 95% CI 0.11–8.59; P = 0.97), pneumonia (OR 0.98; 95% CI 0.36–2.66; P = 0.97), urinary tract infection (OR 0.81; 95% CI 0.26–2.52; P = 0.72), and reoperation (OR 0.95; 95% CI 0.50–1.82; P = 0.78). The ostomy reversal rate was significantly higher in DLI (OR 12.55; 95% CI 3.31–47.55; P = 0.0002).
Conclusions
The overall morbidity and mortality rates between DLI and TAC for the treatment of CDC seemed to be equivalent. Evidence from a randomized controlled trial is needed to clarify the timing and understand the impact of DLI for CDC.




Similar content being viewed by others
References
Balsells E, Shi T, Leese C et al (2019) Global burden of Clostridium difficile infections: a systematic review and meta-analysis. J Glob Health 9:010407
Kwon JH, Olsen MA, Dubberke ER (2015) The morbidity, mortality, and costs associated with Clostridium difficile infection. Infect Dis Clin N Am 29:123–134
McDonald LC, Gerding DN, Johnson S et al (2018) Clinical practice guidelines for Clostridium difficile infection in adults and children: 2017 update by the Infectious Diseases Society of America (IDSA) and Society for Healthcare Epidemiology of America (SHEA). Clin Infect Dis 66:987–994
Steele SR, McCormick J, Melton GB, Paquette I, Rivadeneira DE, Stewart D, Buie WD, Rafferty J (2015) Practice parameters for the management of Clostridium difficile infection. Dis Colon Rectum 58:10–24
Halabi WJ, Nguyen VQ, Carmichael JC, Pigazzi A, Stamos MJ, Mills S (2013) Clostridium difficile colitis in the United States: a decade of trends, outcomes, risk factors for colectomy, and mortality after colectomy. J Am Coll Surg 217:802–812
Neal MD, Alverdy JC, Hall DE, Simmons RL, Zuckerbraun BS (2011) Diverting loop ileostomy and colonic lavage: an alternative to total abdominal colectomy for the treatment of severe, complicated Clostridium difficile associated disease. Ann Surg 254:423–427
Juo YY, Sanaiha Y, Jabaji Z et al (2019) Trends in diverting loop ileostomy vs total abdominal colectomy as surgical Management for Clostridium difficile colitis. JAMA Surg 2019
Moher D, Liberati A, Tetzlaff J, Altman DG, for the PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283:2008–2012
Bhangu A, Nepogodiev D, Gupta A, Torrance A, Singh P, on behalf of the West Midlands Research Collaborative (2012) Systematic review and meta-analysis of outcomes following emergency surgery for Clostridium difficile colitis. Br J Surg 99:1501–1513
Goossen K, Tenckhoff S, Probst P, Grummich K, Mihaljevic AL, Büchler MW, Diener MK (2018) Optimal literature search for systematic reviews in surgery. Langenbeck's Arch Surg 403:119–129
Higgins JP, Altman DG, Gøtzsche PC et al (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928
Sterne JA, Hernan MA, Reeves BC et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Balshem H, Helfand M, Schunemann HJ et al (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol 64:401–406
Hall BR, Leinicke JA, Armijo PR, Smith LM, Langenfeld SJ, Oleynikov D (2019) No survival advantage exists for patients undergoing loop ileostomy for clostridium difficile colitis. Am J Surg 217:34–39
Fashandi AZ, Martin AN, Wang PT, Hedrick TL, Friel CM, Smith PW, Hays RA, Hallowell PT (2017) An institutional comparison of total abdominal colectomy and diverting loop ileostomy and colonic lavage in the treatment of severe, complicated Clostridium difficile infections. Am J Surg 213:507–511
Ferrada P, Callcut R, Zielinski MD, Bruns B, Yeh DD, Zakrison TL, Meizoso JP, Sarani B, Catalano RD, Kim P, Plant V, Pasley A, Dultz LA, Choudhry AJ, Haut ER, EAST Multi-Institutional Trials Committee (2017) Loop ileostomy versus total colectomy as surgical treatment for Clostridium difficile-associated disease: an Eastern Association for the Surgery of Trauma multicenter trial. J Trauma Acute Care Surg 83:36–40
Massachusetts General Hospital (2019) Optimal surgical treatment of fulminant Clostridium difficile colitis. In: ClinicalTrials.gov. National Library of Medicine (US), Bethesda. Updated May 01, 2015; Available at: http://clinicaltrials.gov/ show/NCT01441271 NLM Identifier: NCT0144127. Accessed August 10, 2019
Jewish General Hospital (2019) Loop ileostomy with colonic lavage for fulminant Clostridium difficile colitis. In: ClinicalTrials.gov. National Library of Medicine (US), Bethesda. Updated February 27, 2019; Available at: https://clinicaltrials.gov/ct2/show/NCT02347280. NLM Identifier: NCT02347280. Accessed August 10, 2019
Adams SD, Mercer DW (2007) Fulminant Clostridium difficile colitis. Curr Opin Crit Care 13:450–455
Kautza B, Zuckerbraun BS (2016) The surgical management of complicated Clostridium difficile infection: alternatives to colectomy. Surg Infect 17:337–342
Napolitano LM, Edmiston CE Jr (2017) Clostridium difficile disease: diagnosis, pathogenesis, and treatment update. Surgery 162:325–348
Peprah D, Chiu AS, Jean RA, Pei KY (2019) Comparison of outcomes between total abdominal and partial colectomy for the management of severe, complicated Clostridium difficile infection. J Am Coll Surg 228:925–930
Ali SO, Welch JP, Dring RJ (2008) Early surgical intervention for fulminant pseudomembranous colitis. Am Surg 74:20–26
Al-Abed YA, Gray EA, Rothnie ND (2010) Outcomes of emergency colectomy for fulminant Clostridium difficile colitis. Surgeon 8:330–333
Stewart DB, Hollenbeak CS, Wilson MZ (2013) Is colectomy for fulminant Clostridium difficile colitis life saving? A systematic review. Color Dis 15:798–804
Fashandi AZ, Ellis SR, Smith PW et al (2016) Overwhelming recurrent Clostridium difficile infection after reversal of diverting loop ileostomy created for prior fulminant C. difficile colitis. Am Surg 82:194–195
Fashandi AZ, Wang PT, Hedrick TL et al (2017) Recurrent Clostridium difficile infection after diverting loop ileostomy and colonic lavage: an unreported complication of the novel surgical therapy. Am Surg 83:335–338
Hecker A, Reichert M, Reuß CJ, Schmoch T, Riedel JG, Schneck E, Padberg W, Weigand MA, Hecker M (2019) Intra-abdominal sepsis: new definitions and current clinical standards. Langenbeck's Arch Surg 404:257–271
Ferrada P, Velopulos CG, Sultan S, Haut ER, Johnson E, Praba-Egge A, Enniss T, Dorion H, Martin ND, Bosarge P, Rushing A, Duane TM (2014) Timing and type of surgical treatment of Clostridium difficile-associated disease: a practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 76:1484–1493
Beinortas T, Burr NE, Wilcox MH, Subramanian V (2018) Comparative efficacy of treatments for Clostridium difficile infection: a systematic review and network meta-analysis. Lancet Infect Dis 18:1035–1044
Dallas KB, Condren A, Divino CM (2014) Life after colectomy for fulminant Clostridium difficile colitis: a 7-year follow up study. Am J Surg 207:533–539
Lee DY, Chung EL, Guend H, Whelan RL, Wedderburn RV, Rose KM (2014) Predictors of mortality after emergency colectomy for Clostridium difficile colitis: an analysis of ACS-NSQIP. Ann Surg 259:148–156
Jaber MR, Ruan JH, Fung WL, Reeves ME (2009) Are vasopressor use and mechanical ventilation the only predictors of worse outcome for fulminant Clostridium difficile infection? Am J Surg 198:581–582
Pepin J, Vo TT, Boutros M et al (2009) Risk factors for mortality following emergency colectomy for fulminant Clostridium difficile infection. Dis Colon Rectum 52:400–405
Sailhamer EA, Carson K, Chang Y, Zacharias N, Spaniolas K, Tabbara M, Alam HB, DeMoya M, Velmahos GC (2009) Fulminant Clostridium difficile colitis: patterns of care and predictors of mortality. Arch Surg 144:433–439
Kulaylat AS, Kassam Z, Hollenbeak CS, Stewart DB Sr (2017) A surgical Clostridium-associated risk of death score predicts mortality after colectomy for Clostridium difficile. Dis Colon Rectum 60:1285–1290
Quezada F, Castillo R, Villalon C et al (2015) Treatment of a severe Clostridium difficile infection with colonic lavages. Report of one case. Rev Med Chil 143:668–672
Rosso F, Hormaza MP, Cedano JA, Mora BL, García AF (2018) Ileostomía y lavado colónico anterógrado con Vancomicina en el manejo de infección por Clostridium difficile. Infectio 23:52–54
Dela’O CM, Quyyum A, Dumire RD et al (2014) Community hospital experience of refractory Clostridium difficile colitis: treatment and efficacy of diverting loop ileostomy and colonic lavage. Am Surg 80:E247–E249
Author information
Authors and Affiliations
Contributions
MTA: designed this work, collected and interpreted the data, drafted the manuscript, contributed to study concept, critically revised the manuscript, performed overall supervision, and contributed to the final approval of the manuscript. OVF, OS, DSV, JCSH, PMV and NSN: collected and interpreted the data, drafted the manuscript, critically revised the manuscript, and contributed to the final approval of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This systematic review and meta-analysis of outcomes does not contain any studies with human participants performed by any of the authors.
Informed consent
Considering the nature of this study, informed consent was not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Trejo-Avila, M., Vergara-Fernandez, O., Solórzano-Vicuña, D. et al. A systematic review and meta-analysis of diverting loop ileostomy versus total abdominal colectomy for the treatment of Clostridium difficile colitis. Langenbecks Arch Surg 405, 715–723 (2020). https://doi.org/10.1007/s00423-020-01910-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-020-01910-2