Abstract
Purpose
Few comparative studies are available on the long-term prognostic role of mesopancreas (MP) excision after pancreaticoduodenectomy (PD). We compared the long-term outcomes of patients undergoing standard PD (sPD) and PD with MP excision (PD-MPe).
Methods
Sixty sPDs were compared to 60 matched PD-MPe patients for intraoperative and postoperative data, histopathological findings, and long-term outcomes.
Results
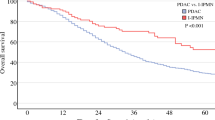
R0 rate was similar in the two groups (p = 0.17). However, PD-MPe related to a lower rate of MP resection margin positivity (16.7% vs 5%; p = 0.04) and to a higher harvested lymph nodes number (19.8 ± 7.6 vs 10.1 ± 5.1; p < 0.0001). Local tumor recurrence was more frequent in the sPD cohort (55.5% vs 26.8% in the PD-MPe group; p = 0.002), with a consequent worse disease-free survival (DFS) (14.8% vs 22.3%; p = 0.04). An inferior 5-year overall survival (OS) was noted in case of MP margin positivity compared with MP margin negativity (0% vs 29%; p < 0.0001). MP positivity resulted as an independent prognostic factor for both a worse OS and DFS at the multivariate analysis.
Conclusion
PD-MPe offers clinical advantages in terms of MP resection margin status, local recurrence, long-term mortality, and DFS. The lower MP positivity rate, achieved with PD-MPe, leads to better outcomes both in terms of OS and DFS.




Similar content being viewed by others
References
Wagner M, Redaelli C, Lietz M, Seiler C, Friess H, Büchler M (2004) Curative resection is the single most important factor determining outcome in patients with pancreatic adenocarcinoma. Br J Surg 91(5):586–594
Hartwig W, Hackert T, Hinz U, Gluth A, Bergmann F, Strobel O, Buchler MW, Werner J (2011) Pancreatic cancer surgery in the new millennium: better prediction of outcome. Ann Surg 254(2):311–319. https://doi.org/10.1097/SLA.0b013e31821fd334
Fortner JG (1973) Regional resection of cancer of the pancreas: a new surgical approach. Surgery 73(2):307–320
Nakao A, Takagi H (1993) Isolated pancreatectomy for pancreatic head carcinoma using catheter bypass of the portal vein. Hepatogastroenterology 40(5):426–429
Carrere N, Sauvanet A, Goere D, Kianmanesh R, Vullierme MP, Couvelard A, Ruszniewski P, Belghiti J (2006) Pancreaticoduodenectomy with mesentericoportal vein resection for adenocarcinoma of the pancreatic head. World J Surg 30(8):1526–1535. https://doi.org/10.1007/s00268-005-0784-4
Mollberg N, Rahbari NN, Koch M, Hartwig W, Hoeger Y, Buchler MW, Weitz J (2011) Arterial resection during pancreatectomy for pancreatic cancer: a systematic review and meta-analysis. Ann Surg 254(6):882–893. https://doi.org/10.1097/SLA.0b013e31823ac299
Zhou Y, Zhang Z, Liu Y, Li B, Xu D (2012) Pancreatectomy combined with superior mesenteric vein–portal vein resection for pancreatic cancer: a meta-analysis. World J Surg 36(4):884–891
Pedrazzoli S, DiCarlo V, Dionigi R, Mosca F, Pederzoli P, Pasquali C, Kloppel G, Dhaene K, Michelassi F, Lymphadenectomy Study Group (1998) Standard versus extended lymphadenectomy associated with pancreatoduodenectomy in the surgical treatment of adenocarcinoma of the head of the pancreas: a multicenter, prospective, randomized study. Ann Surg 228(4):508–517. https://doi.org/10.1097/00000658-199810000-00007
Yeo CJ, Cameron JL, Lillemoe KD, Sohn TA, Campbell KA, Sauter PK, Coleman J, Abrams RA, Hruban RH (2002) Pancreaticoduodenectomy with or without distal gastrectomy and extended retroperitoneal lymphadenectomy for periampullary adenocarcinoma, part 2: randomized controlled trial evaluating survival, morbidity, and mortality. Ann Surg 236(3):355–366; discussion 366-358. https://doi.org/10.1097/00000658-200209000-00012
Adham M, Singhirunnusorn J (2012) Surgical technique and results of total mesopancreas excision (TMpE) in pancreatic tumors. Eur J Surg Oncol 38(4):340–345. https://doi.org/10.1016/j.ejso.2011.12.015
Agrawal MK, Thakur DS, Somashekar U, Chandrakar SK, Sharma D (2010) Mesopancreas: myth or reality? JOP 11(3):230–233
Gockel I, Domeyer M, Wolloscheck T, Konerding MA, Junginger T (2007) Resection of the mesopancreas (RMP): a new surgical classification of a known anatomical space. World J Surg Oncol 5:44. https://doi.org/10.1186/1477-7819-5-44
Gaedcke J, Gunawan B, Grade M, Szoke R, Liersch T, Becker H, Ghadimi BM (2010) The mesopancreas is the primary site for R1 resection in pancreatic head cancer: relevance for clinical trials. Langenbeck's Arch Surg 395(4):451–458. https://doi.org/10.1007/s00423-009-0494-8
Pessaux P, Rosso E, Panaro F, Marzano E, Oussoultzoglou E, Bachellier P, Jaeck D (2009) Preliminary experience with the hanging maneuver for pancreaticoduodenectomy. Eur J Surg Oncol 35(9):1006–1010. https://doi.org/10.1016/j.ejso.2009.04.009
Pessaux P, Varma D, Arnaud JP (2006) Pancreaticoduodenectomy: superior mesenteric artery first approach. J Gastrointest Surg 10(4):607–611. https://doi.org/10.1016/j.gassur.2005.05.001
Varty PP, Yamamoto H, Farges O, Belghiti J, Sauvanet A (2005) Early retropancreatic dissection during pancreaticoduodenectomy. Am J Surg 189(4):488–491. https://doi.org/10.1016/j.amjsurg.2005.01.007
Weitz J, Rahbari N, Koch M, Buchler MW (2010) The “artery first” approach for resection of pancreatic head cancer. J Am Coll Surg 210(2):e1–e4. https://doi.org/10.1016/j.jamcollsurg.2009.10.019
Jiang X, Yu Z, Ma Z, Deng H, Ren W, Shi W, Jiao Z (2020) Superior mesenteric artery first approach can improve the clinical outcomes of pancreaticoduodenectomy: a meta-analysis. Int J Surg 73:14–24. https://doi.org/10.1016/j.ijsu.2019.11.007
Aimoto T, Mizutani S, Kawano Y, Matsushita A, Yamashita N, Suzuki H, Uchida E (2013) Left posterior approach pancreaticoduodenectomy with total mesopancreas excision and circumferential lymphadenectomy around the superior mesenteric artery for pancreatic head carcinoma. J Nippon Med Sch 80(6):438–445
Dumitrascu T, David L, Popescu I (2010) Posterior versus standard approach in pancreatoduodenectomy: a case-match study. Langenbeck's Arch Surg 395(6):677–684. https://doi.org/10.1007/s00423-009-0499-3
Kawabata Y, Nishi T, Tanaka T, Tajima Y (2014) Safety and feasibility of a pancreaticoduodenectomy with total meso-pancreatoduodenum excision: analysis in various periampullary disorders. Hepatogastroenterology 61(131):821–827
Kawabata Y, Tanaka T, Ishikawa N, Hayashi H, Tajima Y (2016) Modified total meso-pancreatoduodenum excision with pancreaticoduodenectomy as a mesopancreatic plane surgery in borderline resectable pancreatic cancer. Eur J Surg Oncol 42(5):698–705. https://doi.org/10.1016/j.ejso.2016.02.241
Kawabata Y, Tanaka T, Nishi T, Monma H, Yano S, Tajima Y (2012) Appraisal of a total meso-pancreatoduodenum excision with pancreaticoduodenectomy for pancreatic head carcinoma. Eur J Surg Oncol 38(7):574–579. https://doi.org/10.1016/j.ejso.2012.04.007
Kurosaki I, Minagawa M, Takano K, Takizawa K, Hatakeyama K (2011) Left posterior approach to the superior mesenteric vascular pedicle in pancreaticoduodenectomy for cancer of the pancreatic head. JOP 12(3):220–229
Xu J, Tian X, Chen Y, Ma Y, Liu C, Tian L, Wang J, Dong J, Cui D, Wang Y, Zhang W, Yang Y (2017) Total mesopancreas excision for the treatment of pancreatic head cancer. J Cancer 8(17):3575–3584. https://doi.org/10.7150/jca.21341
Kawabata Y, Hayashi H, Ishikawa N, Tajima Y (2016) Total meso-pancreatoduodenum excision with pancreaticoduodenectomy in lower biliary tract cancer. Langenbeck's Arch Surg 401(4):463–469. https://doi.org/10.1007/s00423-016-1435-y
Rosenthal R, Hoffmann H, Clavien PA, Bucher HC, Dell-Kuster S (2015) Definition and Classification of Intraoperative Complications (CLASSIC): Delphi study and pilot evaluation. World J Surg 39(7):1663–1671. https://doi.org/10.1007/s00268-015-3003-y
Irita K (2011) Risk and crisis management in intraoperative hemorrhage: human factors in hemorrhagic critical events. Korean J Anesthesiol 60(3):151–160. https://doi.org/10.4097/kjae.2011.60.3.151
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibanes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196. https://doi.org/10.1097/SLA.0b013e3181b13ca2
Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, Neoptolemos J, Sarr M, Traverso W, Buchler M, International Study Group on Pancreatic Fistula D (2005) Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 138(1):8–13. https://doi.org/10.1016/j.surg.2005.05.001
(2001) In: Holzheimer RG, Mannick JA (eds) Surgical treatment: evidence-based and problem-oriented. Munich
Campbell F, Foulis A, Verbeke C (2010) Dataset for the histopathological reporting of carcinomas of the pancreas, ampulla of Vater and common bile duct. R Coll Pathol
Japanese Gastric Cancer A (2017) Japanese gastric cancer treatment guidelines 2014 (ver. 4). Gastric Cancer 20(1):1–19. https://doi.org/10.1007/s10120-016-0622-4
Sener SF, Fremgen A, Menck HR, Winchester DP (1999) Pancreatic cancer: a report of treatment and survival trends for 100,313 patients diagnosed from 1985–1995, using the National Cancer Database. J Am Coll Surg 189(1):1–7
Wellner UF, Krauss T, Csanadi A, Lapshyn H, Bolm L, Timme S, Kulemann B, Hoeppner J, Kuesters S, Seifert G, Bausch D, Schilling O, Vashist YK, Bruckner T, Langer M, Makowiec F, Hopt UT, Werner M, Keck T, Bronsert P (2016) Mesopancreatic stromal clearance defines curative resection of pancreatic head cancer and can be predicted preoperatively by radiologic parameters: a retrospective study. Medicine (Baltimore) 95(3):e2529. https://doi.org/10.1097/MD.0000000000002529
Sharma D, Isaji S (2016) Mesopancreas is a misnomer: time to correct the nomenclature. J Hepatobiliary Pancreat Sci 23(12):745–749. https://doi.org/10.1002/jhbp.402
Availability of data and material
Data and material are available at claudio.fiorillo@hotmail.it.
Author information
Authors and Affiliations
Contributions
Study conception and design: GQ, SA, CF. Acquisition of data: CC, RM, FG, FS, FI. Analysis and interpretation of data: FL, FR, APT, MCG. Drafting of manuscript: GQ, CF. Critical revision of manuscript: SA, FI, APT.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Quero, G., Fiorillo, C., Menghi, R. et al. Total mesopancreas excision for periampullary malignancy: a single-center propensity score-matched comparison of long-term outcomes. Langenbecks Arch Surg 405, 303–312 (2020). https://doi.org/10.1007/s00423-020-01873-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-020-01873-4