Abstract
Purpose
Surgical strategies for perforated diverticulitis (Hinchey stages III and IV) remain controversial. This systematic review aimed to compare the outcome of primary anastomosis, Hartmann procedure and laparoscopic lavage.
Methods
A systematic literature search was conducted through Medline, Embase, Cochrane Central Register and Health Technology Assessment Database to identify randomized and non-randomized controlled trials involving patients with perforated left-sided colonic diverticulitis comparing different surgical strategies. The methodological quality of the included studies was assessed systematically (Grading of Recommendations, Assessment, Development and Evaluation) and a meta-analysis was performed.
Results
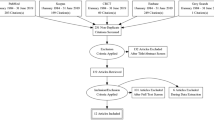
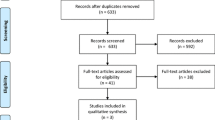
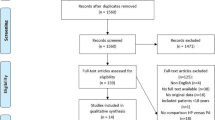
After screening 4090 titles and abstracts published between 1958 and January 2018, 148 were selected for full text assessment. Sixteen trials (7 RCTs, 9 non-RCTs) with 1223 patients were included. Mortality rates were not significantly different between Hartmann procedure and primary anastomosis for Hinchey III and IV, neither in the meta-analysis of three RCTs (RR 2.03 (95% CI 0.79 to 5.25); p = 0.14, moderate quality of evidence) nor in the meta-analysis of six observational studies (RR 1.53 (95% CI 0.89 to 2.65); p = 0.13, very low quality of evidence). However, stoma reversal rates were significantly higher in the primary anastomosis group (RR 0.73 (95% CI 0.58 to 0.98); p = 0.008, moderate quality of evidence). Meta-analysis of four RCTs showed no significant difference between laparoscopic lavage for Hinchey III compared to sigmoid resection neither for mortality (RR 1.07 (95% CI 0.65 to 1.76); p = 0.79, moderate quality of evidence) nor for major complications (RR 0.86 (95% CI 0.69 to 1.08); p = 0.20, moderate quality of evidence).
Conclusions
This systematic review suggests similar rates of complications but higher rates of colonic restoration after primary anastomosis compared to Hartmann procedure in perforated diverticulitis with generalized peritonitis (Hinchey III and IV). Results in laparoscopic lavage for Hinchey III are not superior to primary resection. However, further studies with a careful interpretation of the meaning of re-interventions are required.




Similar content being viewed by others
Abbreviations
- ASA:
-
American Society of Anaesthesiologists
- GRADE:
-
Grading of Recommendations, Assessment, Development and Evaluation
- HP:
-
Hartmann procedure
- LL:
-
Laparoscopic lavage
- LOS:
-
Length of hospital stay
- PA:
-
Primary anastomosis
- RCT:
-
Randomized controlled trial
References
Parra-Blanco A (2006) Colonic diverticular disease: pathophysiology and clinical picture. Digestion 73(Suppl 1):47–57
Wong WD, Wexner SD, Lowry A et al (2000) Practice parameters for the treatment of sigmoid diverticulitis—supporting documentation. The Standards Task Force. The American Society of Colon and Rectal Surgeons. Dis Colon Rectum 43:290–297
Krukowski ZH, Matheson NA (1984) Emergency surgery for diverticular disease complicated by generalized and faecal peritonitis: a review. Br J Surg 71:921–927
Stollman N, Raskin JB (2004) Diverticular disease of the colon. Lancet 363:631–639
Zorcolo L, Covotta L, Carlomagno N, Bartolo DCC (2003) Safety of primary anastomosis in emergency colo-rectal surgery. Color Dis 5:262–269
Hinchey EJ, Schaal PG, Richards GK (1978) Treatment of perforated diverticular disease of the colon. Adv Surg 12:85–109
Constantinides VA, Heriot A, Remzi F, Darzi A, Senapati A, Fazio VW, Tekkis PP (2007) Operative strategies for diverticular peritonitis: a decision analysis between primary resection and anastomosis versus Hartmann’s procedures. Ann Surg 245:94–103
Leitfeld L, Germer CT, Böhm S, et al. (2013) S2k Leitlinie Divertikelkrankheit/Divertikulitis. Arbeitsgemeinschaft der Wissenschaftlichen Medizinischen Fachgesellschaften e.V. http://www.awmf.org/uploads/tx_szleitlinien/021-020l_S3_Divertikelkrankheit_Divertikulus_2014-05.pdf. 05 April 2018
Trenti L, Biondo S, Golda T, Monica M, Kreisler E, Fraccalvieri D, Frago R, Jaurrieta E (2011) Generalized peritonitis due to perforated diverticulitis: Hartmann’s procedure or primary anastomosis? Int J Color Dis 26:377–384
Zeitoun G, Laurent A, Rouffet F, Hay JM, Fingerhut A, Paquet JC, Peillon C, Research FAS (2000) Multicentre, randomized clinical trial of primary versus secondary sigmoid resection in generalized peritonitis complicating sigmoid diverticulitis. Br J Surg 87:1366–1374
Myers E, Hurley M, O’Sullivan GC, Kavanagh D, Wilson I, Winter DC (2008) Laparoscopic peritoneal lavage for generalized peritonitis due to perforated diverticulitis. Br J Surg 95:97–101
O’Sullivan GC, Murphy D, O’Brien MG, Ireland A (1996) Laparoscopic management of generalized peritonitis due to perforated colonic diverticula. Am J Surg 171:432–434
Taylor CJ, Layani L, Ghusn MA, White SI (2006) Perforated diverticulitis managed by laparoscopic lavage. ANZ J Surg 76:962–965
Abbas S (2007) Resection and primary anastomosis in acute complicated diverticulitis, a systematic review of the literature. Int J Color Dis 22:351–357
Constantinides VA, Tekkis PP, Athanasiou T, Aziz O, Purkayastha S, Remzi FH, Fazio VW, Aydin N, Darzi A, Senapati A (2006) Primary resection with anastomosis vs. Hartmann’s procedure in nonelective surgery for acute colonic diverticulitis: a systematic review. Dis Colon Rectum 49:966–981
Salem L, Flum DR (2004) Primary anastomosis or Hartmann’s procedure for patients with diverticular peritonitis? A systematic review. Dis Colon Rectum 47:1953–1964
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Goossen K, Tenckhoff S, Probst P, Grummich K, Mihaljevic AL, Büchler MW, Diener MK (2018) Optimal literature search for systematic reviews in surgery. Langenbeck’s Arch Surg 403:119–129
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P, Schünemann HJ, GRADE Working Group (2008) GRADE: an emerging consensus on rating quality of evidence and strength of recommendations. BMJ 336:924–926
Binda GA, Karas JR, Serventi A, Sokmen S, Amato A, Hydo L, Bergamaschi R, for the Study Group on Diverticulitis (2012) Primary anastomosis vs nonrestorative resection for perforated diverticulitis with peritonitis: a prematurely terminated randomized controlled trial. Color Dis 14:1403–1410
Bridoux V, Regimbeau JM, Ouaissi M, Mathonnet M, Mauvais F, Houivet E, Schwarz L, Mege D, Sielezneff I, Sabbagh C, Tuech JJ (2017) Hartmann’s procedure or primary anastomosis for generalized peritonitis due to perforated diverticulitis: a prospective multicenter randomized trial (DIVERTI). J Am Coll Surg 225:798–805
Gooszen AW, Gooszen HG, Veerman W, van Dongen V, Hermans J, Klien Kranenbarg E, Tollenaar RA (2001) Operative treatment of acute complications of diverticular disease: primary or secondary anastomosis after sigmoid resection. Eur J Surg 167:35–39
Hold M, Denck H, Bull P (1990) Surgical management of perforating diverticular disease in Austria. Int J Color Dis 5:195–199
Magenta A, Carraro PS, Segala M et al (1997) The choice of surgery in perforated diverticular disease. Chirurgia 10:34–39
Oberkofler CE, Rickenbacher A, Raptis DA, Lehmann K, Villiger P, Buchli C, Grieder F, Gelpke H, Decurtins M, Tempia-Caliera AA, Demartines N, Hahnloser D, Clavien PA, Breitenstein S (2012) A multicenter randomized clinical trial of primary anastomosis or Hartmann’s procedure for perforated left colonic diverticulitis with purulent or fecal peritonitis. Ann Surg 256:819–826; discussion 826–817, 827
Regenet N, Pessaux P, Hennekinne S, Lermite E, Tuech JJ, Brehant O, Arnaud JP (2003) Primary anastomosis after intraoperative colonic lavage vs. Hartmann’s procedure in generalized peritonitis complicating diverticular disease of the colon. Int J Color Dis 18:503–507
Schilling MK, Maurer CA, Kollmar O, Büchler MW (2001) Primary vs. secondary anastomosis after sigmoid colon resection for perforated diverticulitis (Hinchey Stage III and IV): a prospective outcome and cost analysis. Dis Colon Rectum 44:699–703; discussion 703–695
Thaler K, Neumann F, Gero A, Kreuzer W (2000) Utility of appropriate peritonitis grading in the surgical management of perforated sigmoid diverticulitis. Color Dis 2:359–363
Angenete E, Thornell A, Burcharth J, Pommergaard HC, Skullman S, Bisgaard T, Jess P, Läckberg Z, Matthiessen P, Heath J, Rosenberg J, Haglind E (2016) Laparoscopic lavage is feasible and safe for the treatment of perforated diverticulitis with purulent peritonitis: the first results from the randomized controlled trial DILALA. Ann Surg 263:117–122
Catry J, Brouquet A, Peschaud F, Vychnevskaia K, Abdalla S, Malafosse R, Lambert B, Costaglioli B, Benoist S, Penna C (2016) Sigmoid resection with primary anastomosis and ileostomy versus laparoscopic lavage in purulent peritonitis from perforated diverticulitis: outcome analysis in a prospective cohort of 40 consecutive patients. Int J Color Dis 31:1693–1699
Karoui M, Champault A, Pautrat K, Valleur P, Cherqui D, Champault G (2009) Laparoscopic peritoneal lavage or primary anastomosis with defunctioning stoma for Hinchey 3 complicated diverticulitis: results of a comparative study. Dis Colon Rectum 52:609–615
Liang S, Russek K, Franklin ME, Jr. (2012) Damage control strategy for the management of perforated diverticulitis with generalized peritonitis: laparoscopic lavage and drainage vs. laparoscopic Hartmann’s procedure. Surg Endosc 26:2835–2842
Schultz JK, Yaqub S, Wallon C, Blecic L, Forsmo HM, Folkesson J, Buchwald P, Körner H, Dahl FA, Øresland T, SCANDIV Study Group (2015) Laparoscopic lavage vs primary resection for acute perforated diverticulitis: the SCANDIV randomized clinical trial. JAMA 314:1364–1375
Thornell A, Angenete E, Bisgaard T, Bock D, Burcharth J, Heath J, Pommergaard HC, Rosenberg J, Stilling N, Skullman S, Haglind E (2016) Laparoscopic lavage for perforated diverticulitis with purulent peritonitis: a randomized trial. Ann Intern Med 164:137–145
Vennix S, Musters GD, Mulder IM, Swank HA, Consten EC, Belgers EH, van Geloven AA, Gerhards MF, Govaert MJ, van Grevenstein WM, Hoofwijk AG, Kruyt PM, Nienhuijs SW, Boermeester MA, Vermeulen J, van Dieren S, Lange JF, Bemelman WA (2015) Laparoscopic peritoneal lavage or sigmoidectomy for perforated diverticulitis with purulent peritonitis: a multicentre, parallel-group, randomised, open-label trial. Lancet 386:1269–1277
Howe HJ, Casali RE, Westbrook KC, Thompson BW, Read RC (1979) Acute perforations of the sigmoid colon secondary to diverticulitis. Am J Surg 137:184–187
Feingold D, Steele SR, Lee S, Kaiser A, Boushey R, Buie WD, Rafferty JF (2014) Practice parameters for the treatment of sigmoid diverticulitis. Dis Colon rectum 57:284–294
Haiden G, Schima E (1980) Procedure in perforated diverticulitis of the sigmoid colon (author’s transl). Zentralbl Chir 105:652–655
Killingback M (1983) Management of perforative diverticulitis. Surg Clin North Am 63:97–115
Parks TG (1975) Natural history of diverticular disease of the colon. Clin Gastroenterol 4:53–69
Acknowledgements
We would like to thank Angela Munson and Christa Bosshard or her assistance and proofreading of the manuscript.
Author information
Authors and Affiliations
Contributions
Dr. med. Sina Schmidt, Dr. med. Tarek Ismail, Dr. med. Christopher Soll, and Prof. Dr. med. Stefan Breitenstein: study conception and design, acquisition of data, analysis and interpretation of data, drafting of manuscript, and critical revision of manuscript. Prof. Dr. med. Milo A. Puhan: study conception and design, analysis and interpretation of data, drafting of manuscript, and critical revision of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This manuscript is a meta-analysis; it does not contain any procedures involving human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all participants involved in this study.
Additional information
Sina Schmidt and Tarek Ismail shared first authorship.
Electronic supplementary material
Suppl. Fig. 1
Analysis of 6 observational studies comparing Hartmann Procedure with primary anastomosis (PDF 13 kb)
Suppl. Fig. 2
Analysis of overall morbidity of three observational studies comparing laparoscopic lavage with resection (res.) (PDF 10 kb)
Suppl. Fig. 3
Search Strategy (PDF 51 kb)
Suppl. Table 1
Description of included studies (PDF 200 kb)
Suppl. Table 2
Outcome results of included studies (PDF 13 kb)
Suppl. Table 3b
a: Quality Assessment of included studies comparing Hartmann Procedure with primary anastomosis (randomized controlled trials and observational studies). b: Quality Assessment of included studies comparing colonic resection (Hartmann Procedure or primary anastomosis) with laparoscopic lavage (randomized controlled trials and observational studies) (PDF 51 kb)
Rights and permissions
About this article
Cite this article
Schmidt, S., Ismail, T., Puhan, M.A. et al. Meta-analysis of surgical strategies in perforated left colonic diverticulitis with generalized peritonitis. Langenbecks Arch Surg 403, 425–433 (2018). https://doi.org/10.1007/s00423-018-1686-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-018-1686-x