Abstract
Background
Elective pancreatic surgery can be carried out with mortality rates below 5 % in specialized centers today. Only few data exist on pancreatic resections in emergency situations. The aim of the study was to characterize indications, procedures, and outcome of emergency pancreatic surgery in a tertiary center.
Methods
Prospectively collected data of all patients undergoing pancreatic operations at the authors’ institution between October 2001 and December 2012 were analyzed regarding primary emergency operations in terms of indications, procedures, perioperative complications, and outcome. Emergency operations after preceding resections were excluded from the analysis.
Results
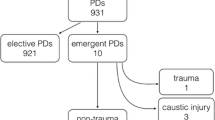
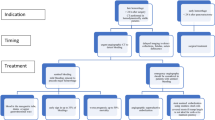
Twenty-three emergency operations were performed during the observation period. Indications were duodenal perforation (n = 8), upper GI bleeding (n = 6), complicated pseudocysts (n = 3), bile duct perforation (n = 2), pancreatic bleeding after blunt abdominal trauma (n = 1), pancreatic stent perforation (n = 1), necrotizing cholecystitis (n = 1), and ileus (n = 1). Procedures included partial and total duodeno-pancreatectomy (n = 15), cystojejunostomy (n = 2), distal pancreatectomy (n = 4), reconstruction of the ampulla Vateri (n = 1), and duodenectomy (n = 1). Median intraoperative blood loss was 750 (200–2500) ml and OP time 4.25 (1.75–9.25) h. Mean ICU stay was 21.3 (1–80) days with an overall surgical morbidity of 52.2 %. Overall in-hospital mortality was 34.8 % (8/23 pat.).
Conclusions
Emergency pancreatic operations are infrequent and mainly performed due to duodenal perforation or bleeding; blunt abdominal trauma is rarely leading to emergency pancreas resections. They are associated with an increased morbidity and mortality and require a high level of surgical as well as interdisciplinary experience. Perioperative anesthesiological care and interventional radiological complication management are essential to improve outcome in this selective patient collective.
Similar content being viewed by others
References
de Wilde RF, Besselink MG, van der Tweel I, de Hingh IH, van Eijck CH, Dejong CH et al (2012) Impact of nationwide centralization of pancreaticoduodenectomy on hospital mortality. Br J Surg 99:404–410
Büchler MW, Wagner M, Schmied BM, Uhl W, Friess H, Z’graggen K (2003) Changes in morbidity after pancreatic resection: toward the end of completion pancreatectomy. Arch Surg 138:1310–1314
Lavu H, Nowcid LJ, Klinge MJ, Mahendraraj K, Grenda DR, Sauter PK et al (2011) Reoperative completion pancreatectomy for suspected malignant disease of the pancreas. J Surg Res 170:89–95
Crippa S, Tamburrino D, Partelli S, Salvia R, Germenia S, Bassi C et al (2011) Total pancreatectomy: indications, different timing, and perioperative and long-term outcomes. Surgery 149:79–86
van Berge Henegouwen MI, De Wit LT, Van Gulik TM, Obertop H, Gouma DJ (1997) Incidence, risk factors, and treatment of pancreatic leakage after pancreaticoduodenectomy: drainage versus resection of the pancreatic remnant. J Am Coll Surg 185:18–24
Lin BC, Chen RJ, Fang JF, Hsu YP, Kao YC, Kao JL (2004) Management of blunt major pancreatic injury. J Trauma 56:774–778
Heuer M, Hussmann B, Lefering R, Taeger G, Kaiser GM, Paul A et al (2011) Pancreatic injury in 284 patients with severe abdominal trauma: outcome, course, and treatment algorithm. Langenbeck’s Arch Surg 396:1067–1076
Wolf A, Bernhardt J, Patrzyk M, Heidecke CD (2005) The value of endoscopic diagnosis and the treatment of pancreas injuries following blunt abdominal trauma. Surg Endosc 19:665–669
Asensio JA, Petrone P, Roldán G, Kuncir E, Demetriades D (2003) Pancreaticoduodenectomy: a rare procedure for the management of complex pancreaticoduodenal injuries. J Am Coll Surg 197:937–942
Standop J, Glowka T, Schmitz V, Schaefer N, Hirner A, Kalff JC (2010) Emergency Kausch-Whipple procedure: indications and experiences. Pancreas 39:156–159
Z’Graggen K, Strobel O, Schmied BM, Zimmermann A, Buchler MW (2002) Emergency pancreatoduodenectomy in nontrauma patients. Pancreas 24:258–263
Vladov NN, Takorov IR, Mutafchiiski VM, Kjossev KT, Kazarov K, Mladenov N et al (2007) Successful emergency pancreatoduodenectomy in a non-trauma patient. Hepatogastroenterology 54:1844–1846
Stratigos P, Kouskos E, Kouroglou M, Chrisafis I, Fois L, Mavrogiorgis A et al (2007) Emergency pancreatoduodenectomy (Whipple procedure) for massive upper gastrointestinal bleeding caused by a diffuse B-cell lymphoma of the duodenum: report of a case. Surg Today 37:680–684
Lefrancois M, Gaujoux S, Resche-Rigon M, Chirica M, Munoz-Bongrand N, Sarfati E et al (2011) Oesophagogastrectomy and pancreatoduodenectomy for caustic injury. Br J Surg 98:983–990
Wente MN, Bassi C, Dervenis C, Fingerhut A, Gouma DJ, Izbicki JR et al (2007) Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 142:761–768
Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J et al (2005) Postoperative pancreatic fistula: an International Study Group (ISGPF) definition. Surgery 138:8–13
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Cho HS, Han DS, Ahn SB, Byun TJ, Kim TY, Eun CS, Jeon YC et al (2009) Comparison of the effectiveness of interventional endoscopy in bleeding peptic ulcer disease according to the timing of endoscopy. Gut Liver 3:266–270
Holster IL, Kuipers EJ (2011) Update on the endoscopic management of peptic ulcer bleeding. Curr Gastroenterol Rep 13:525–531
Machado NO (2012) Management of duodenal perforation post-endoscopic retrograde cholangiopancreatography. When and whom to operate and what factors determine the outcome? A review article. JOP 13:18–25
Lin BC, Liu NJ, Fang JF, Kao YC (2006) Long-term results of endoscopic stent in the management of blunt major pancreatic duct injury. Surg Endosc 20:1551–1555
Sohn TA, Yeo CJ, Cameron JL, Geschwind JF, Mitchell SE, Venbrux AC et al (2003) Pancreaticoduodenectomy: role of interventional radiologists in managing patients and complications. J Gastrointest Surg 7:209–219
Stampfl U, Hackert T, Sommer CM, Klauss M, Bellemann N, Siebert S et al (2012) Superselective embolization for the management of postpancreatectomy hemorrhage: a single-center experience in 25 patients. J Vasc Interv Radiol 23:504–510
Kalva SP, Yeddula K, Wicky S, Fernandez del Castillo C, Warshaw AL (2011) Angiographic intervention in patients with a suspected visceral artery pseudoaneurysm complicating pancreatitis and pancreatic surgery. Arch Surg 146:647–652
Yekebas EF, Wolfram L, Cataldegirmen G, Habermann CR, Bogoevski D, Koenig AM et al (2007) Postpancreatectomy hemorrhage: diagnosis and treatment: an analysis in 1669 consecutive pancreatic resections. Ann Surg 246:269–280
Stampfl U, Hackert T, Radeleff B, Sommer CM, Stampfl S, Werner J et al (2011) Percutaneous management of postoperative bile leaks after upper gastrointestinal surgery. Cardiovasc Intervent Radiol 34:808–815
Choi SH, Moon HJ, Heo JS, Joh JW, Kim YI (2004) Delayed hemorrhage after pancreaticoduodenectomy. J Am Coll Surg 199:186–191
Hackert T, Kienle P, Weitz J, Werner J, Szabo G, Hagl S et al (2003) Accuracy of diagnostic laparoscopy for early diagnosis of abdominal complications after cardiac surgery. Surg Endosc 17:1671–1674
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Strobel, O., Schneider, L., Philipp, S. et al. Emergency pancreatic surgery—demanding and dangerous. Langenbecks Arch Surg 400, 837–841 (2015). https://doi.org/10.1007/s00423-015-1321-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-015-1321-z