Abstract
Purpose
Laparoscopic surgery (LS) is gaining popularity worldwide because of benefits like faster recovery, earlier hospital discharge, and better cosmetic results. In hemophiliacs, surgery in general harbors an increased risk for severe complications. Whether LS or conventional surgery (CS) should be recommended in these patients is controversial and therefore the issue of our present study.
Methods
We performed a retrospective matched-pair analysis including laparoscopically operated non-hemophiliacs (LONH), laparoscopically operated hemophiliacs (LOH), and conventionally operated hemophiliacs (COH) concerning duration of surgery, drainages, hospital stay, complications, factor use (VIII, IX, and X), and blood values. Mann-Whitney U test was used (significance level P = 0.05).
Results
No significant differences were found in duration of surgery and drains in laparoscopically or conventionally operated hemophiliacs versus matched pairs. Complication rate did not differ among the different groups.
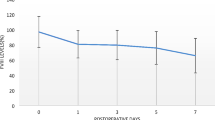
Concerning the total duration of hospital stay (t-DHOS) and the postoperative duration of hospital stay (p-DHOS), there was no statistical difference between LOH versus matched LONH. However, in COH versus matched LOH, a longer time was required for preparation and recovery (t-DHOS, P = 0.04; p-DHOS, P < 0.001).
Also, the median factor supply perioperatively including the day of surgery did not differ between laparoscopically versus conventionally operated hemophiliacs.
Conclusions
Our study underscores the safety and benefits of laparoscopic procedures in hemophiliacs by showing a significantly shorter hospital stay for these patients resulting in reduced therapeutic costs and a faster mobilization. Still, the surgical and perioperative management of hemophiliacs continues to be a challenge requiring an experienced interdisciplinary team.






Similar content being viewed by others
References
Sauerland S, Jaschinski T, Neugebauer EA (2010) Laparoscopic versus open surgery for suspected appendicitis. Cochrane Database Syst Rev 10, CD001546. doi:10.1002/14651858.CD001546.pub3
Pedersen AG, Petersen OB, Wara P, Ronning H, Qvist N, Laurberg S (2001) Randomized clinical trial of laparoscopic versus open appendicectomy. Br J Surg 88(2):200–205. doi:10.1046/j.1365-2168.2001.01652.x
Lee WJ, Chan CP, Wang BY (2013) Recent advances in laparoscopic surgery. Asian J Endosc Surg 6(1):1–8. doi:10.1111/ases.12001
Keus F, de Jong JA, Gooszen HG, van Laarhoven CJ (2006) Laparoscopic versus open cholecystectomy for patients with symptomatic cholecystolithiasis. Cochrane Database Syst Rev 4, CD006231. doi:10.1002/14651858.CD006231
Nilsson IM, Hedner U, Ahlberg A, Larsson SA, Bergentz SE (1977) Surgery of hemophiliacs—20 years’ experience. World J Surg 1(1):55–66
Bolton-Maggs PH (2006) Optimal haemophilia care versus the reality. Br J Haematol 132(6):671–682. doi:10.1111/j.1365-2141.2005.05952.x
Goldmann G, Holoborodska Y, Oldenburg J, Schaefer N, Hoeller T, Standop J, Kalff JC, Hirner A, Overhaus M (2010) Perioperative management and outcome of general and abdominal surgery in hemophiliacs. Am J Surg 199(5):702–707. doi:10.1016/j.amjsurg.2009.02.018
Matzsch T, Almqvist P, Berntorp E, Lethagen S, Montgomery A (1992) Laparoscopic cholecystectomy in a patient with hemophilia B. Surg Laparosc Endosc 2(4):339–340
Mallen JK, Paulson RL (1993) Elective laparoscopic cholecystectomy in a patient with hemophilia. J Clin Gastroenterol 16(3):260–261
Walsh JD, Landercasper J, Bottner WA, Boyd WC (2004) Cholecystectomy and acquired factor VIII inhibitor coagulopathy. Am Surg 70(9):815–817
Slaoui M, Lambert T, Stieltjes N, Claeyssens S, Borel-Derlon A (2004) Intestinal surgery with activated recombinant factor VII prophylaxis in patients with haemophilia A and high responding inhibitors: a report of five cases. Blood Coagul Fibrinolysis : Int J Haemost Thromb 15(8):687–691
Acknowledgments
We kindly thank all the colleagues working in our different departments helping us to gain such promising results for our patients.
Funding
There was no specific funding used for this paper.
Conflicts of interest
All authors have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lingohr, P., Bensoukehal, S., Matthaei, H. et al. Value and risk of laparoscopic surgery in hemophiliacs—experiences from a tertiary referral center for hemorrhagic diatheses. Langenbecks Arch Surg 399, 609–618 (2014). https://doi.org/10.1007/s00423-014-1185-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-014-1185-7