Abstract
Background
Laparoscopic cholecystectomy is an established treatment for almost all gallbladder diseases with bile duct injury rates similar to open cholecystectomy. These laparoscopic skills must be passed on to junior surgeons without compromising patient safety.
Materials and methods
We analysed our structured training programme over 6years (May 2000 to May 2006) by following three trainee surgeons during their training and beyond. During this period, 1,000 laparoscopic cholecystectomies were carried out with five consultant surgeons supervising and three new trainees who completed their accreditation in laparoscopic cholecystectomy.
Results
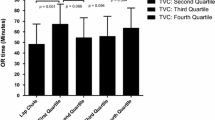
There were 694 patients operated on by consultant surgeons (Group 1), 202 by trainee surgeons (Group 2) and 104 by newly trained surgeons (Group 3). There were no differences between the groups in terms of age and gender. However, there was a significant difference in gallbladder disease among the three groups; Group 2 had more gallstone pancreatitis patients (P < 0.019). There were no differences among the three groups in conversion rates, bile duct injury rates, general complication rates or length of stay. However, the duration of operation in Group 2 was significantly longer compared to the other two groups (P < 0.0001).
Conclusion
This programme is effective in training junior surgeons and does not compromise patient safety.
Similar content being viewed by others
References
Lichten JB, Reid JJ, Zahalsky MP, Friedman RL (2001) Laparoscopic cholecystectomy in the new millennium. Surg Endosc 15:867–872
Shoemaker CP Jr (2003) Changes in the general surgical workload, 1991–1999. Arch Surg 138:417–426
EAES (1994) Guidelines: training and assessment of competence. Surg Endosc 8:721–722
SAGES (1991) Granting of privileges for laparoscopic general surgery. Am J Surg 161:324–325
SAGES (1993) Guidelines for institutions granting privileges utilizing laparoscopic and/or thorascopic techniques. Surg Endosc 7:67–68
SAGES (1994) Framework for post-residency surgical education and training. SAGES Guidel 8:1137–1147
New York State Department of Health (1992) Laparoscopic surgery. New York State Department of Health Memorandum Series 92. New York State Department of Health, Albany
Dent TL (1991) Training, credentialing and granting of clinical privileges for laparoscopic general surgery. Am J Surg 161:399–403
Lau H, Brooks DC (2002) Transitions in laparoscopic cholecystectomy: the impact of ambulatory surgery. Surg Endosc 16:323–326
Wu JS, Dunnegan DL, Luttmann DR, Soper NJ (1998) The evolution and maturation of laparoscopic cholecystectomy in an academic practice. J Am Coll Surg 186:554–560
MacFadyen BV Jr (2004) Teaching, training and clinical surgery. Surg Endosc 18:361–362
Gallagher AG, Ritter EM, Satava RM (2003) Fundamental principles of validation, and reliability: rigorous science for the assessment of surgical education and training. Surg Endosc 17:1525–1529
Adrales GL, Chu UB, Hoskins JD, Witzke DB, Park AE (2004) Development of a valid, cost-effective laparoscopic training program. Am J Surg 187:157–163
Adrales GL, Park AE, Chu UB, Witzke DB, Donnelly MB, Hoskins JD, Mastrangelo MJ Jr, Gandsas A (2003) A valid method of laparoscopic simulation training and competence assessment. J Surg Res 114:156–162
Chiasson PM, Pace DE, Schlachta CM, Mamazza J, Poulin EC (2003) Minimally invasive surgery training in Canada: a survey of general surgery. Surg Endosc 17:371–377
Rattner DW, Apelgren KN, Eubanks WS (2001) The need for training opportunities in advanced laparoscopic surgery. Surg Endosc 15:1066–1070
Liu CL, Fan ST, Lai EC, Lo CM, Chu KM (1996) Factors affecting conversion of laparoscopic cholecystectomy to open surgery. Arch Surg 131:98–101
Dagash H, Chowdhury M, Pierro A (2003) When can I be proficient in laparoscopic surgery? A systematic review of the evidence. J Pediatr Surg 38:720–724
Elliot DL, Hickam DH (1987) Evaluation of physical examination skills. Reliability of faculty observers and patient instructors. JAMA 258:3405–3408
Warf BC, Donnelly MB, Schwartz RW, Sloan DA (1999) The relative contributions of interpersonal and specific clinical skills to the perception of global clinical competence. J Surg Res 86:17–23
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ibrahim, S., Tay, K.H., Lim, S.H. et al. Analysis of a structured training programme in laparoscopic cholecystectomy. Langenbecks Arch Surg 393, 943–948 (2008). https://doi.org/10.1007/s00423-007-0269-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-007-0269-z