Abstract
Background and aims
Insufficient perfusion of distal flap areas, which may lead to partial necrosis, still represents a challenge in reconstructive surgery. In the process of microvascular and endothelial dysfunction, endothelins (ETs) and their receptors may play an important role. Therefore, the aim of the study was to investigate in a chronic in vivo model the effect of various ET-receptor antagonists in critically perfused flap tissue.
Materials and methods
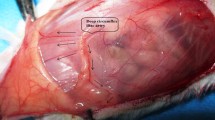
A random pattern musculocutaneous flap was elevated in the back of 25 C57BL/6 mice and fixed into a dorsal skinfold chamber. Repetitive intravital fluorescence microscopy was performed over a 10-day observation period, assessing arteriolar diameter, arteriolar blood flow (aBF), functional capillary density (FCD), the area of tissue necrosis, and the development of newly formed blood vessels. ET-receptor blockers were administrated intraperitoneally 30 min before induction of ischemia, as well as daily during the subsequent 4-day period, including (1) BQ-123, a specific ET-A-receptor antagonist (ET-A = 1 mg/kg), (2) BQ-788, a selective ET-B-receptor antagonist (ET-B = 1 mg/kg), and (3) PD-142893, a nonselective ET-AB-receptor antagonist (ET-AB = 0.5 mg/kg). Animals receiving saline only served as controls (n = 7).
Results
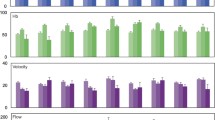
Despite an increase in aBF during the 10-day observation period (day 1 = 1.92 ± 0.29 nl/s; day 10 = 4.70 ± 1.64 nl/s), the flaps of saline-treated controls showed a distinct decrease in FCD (94 ± 12 cm/cm2). This perfusion failure resulted in flap necrosis of 52 ± 3%. Selective blockade of the ET-B receptor caused a further increase in aBF already at day 1 (2.97 ± 0.42 nl/s), which persisted during the following 10-day observation period (day 10 = 5.74 ± 0.69 nl/s). Accordingly, adequate FCD could be maintained (day 10 = 215 ± 8 cm/cm2; p < 0.05 vs control), resulting in a significant reduction in flap necrosis (day 10 = 25 ± 4%; p < 0,05). In contrast, neither selective blockade of the ET-A receptor nor nonselective ET-A- and ET-B-receptor blockade were able to significantly affect aBF when compared to controls (day 1 = ET-A = 1.39 ± 0.10 nl/s; ET-AB = 1.53 ± 0.80 nl/s; n.s.). Accordingly, flap necrosis after ET-A- and ET-AB-receptor inhibition did not differ from that of controls (day 10 = ET-A: 46 ± 10%; ET-AB = 51 ± 7%).
Conclusion
Our data show that only selective ET-B-receptor inhibition is capable of maintaining nutritive perfusion and, hence, reducing necrosis in critically perfused flap tissue. Accordingly, administration of ET-B-receptor antagonists may be considered in the treatment of critically perfused flaps.




Similar content being viewed by others
References
Erni D, Wessendorf R, Wettstein R, Schilling MK, Banic A (2001) Endothelin receptor blockade improves oxygenation in contralateral TRAM flap tissue in pigs. Br J Plast Surg 54:412–418
Jokuszies A, Jansen V, Lahoda LU, Steinau HU, Vogt PM (2005) Plasma concentration of endothelin-1 after myocutaneous latissimus dorsi-transplantation—role in reperfusion injury. Handchir Mikrochir Plast Chir 37:193–201
Lantieri LA, Carayon A, Maistre O, Evrin J, Hemery F, Torossian JM, Collins ED, Raulo Y (2003) Tissue and plasma levels of endothelin in free flaps. Plast Reconstr Surg 111:85–91
Matsuzaki K (1993) Effect of skin flap ischemia on plasma endothelin-1 levels. Ann Plast Surg 31:499–503
Tane N, Inoue H, Aihara M, Ishida H (1995) The effects of endothelin-1 on flap necrosis. Ann Plast Surg 35:389–395
Pang CY, Yang RZ, Neligan P, Xu N, Chiu C, Zhong A, Forrest CR (1995) Vascular effects and mechanism of action of endothelin-1 in isolated perfused pig skin. J Appl Physiol 79:2106–2113
Zhang J, Lipa JE, Black CE, Huang N, Neligan PC, Ling FT, Levine RH, Semple JL, Pang CY (2000) Pharmacological characterization of vasomotor activity of human musculocutaneous perforator artery and vein. J Appl Physiol 89:2268–2275
Marsault R, Vigne P, Breittmayer JP, Frelin C (1991) Kinetics of vasoconstrictor action of endothelins. Am J Physiol 261:C987–C993
Mickley EJ, Gray GA, Webb DJ (1997) Activation of endothelin ETA receptors masks the constrictor role of endothelin ETB receptors in rat isolated small mesenteric arteries. Br J Pharmacol 120:1376–1382
Seo B, Oemar BS, Siebenmann R, von Segesser L, Lüscher TF (1994) Both ETA and ETB receptors mediate contraction to endothelin-1 in human blood vessels. Circulation 89:1203–1208
de Nucci G, Thomas R, D’Orleans-Juste P, Antunes E, Walder C, Warner TD, Vane JR (1998) Pressor effects of circulating endothelin are limited by its removal in the pulmonary circulation and by the release of prostacyclin and endothelium-derived relaxing factor. Proc Natl Acad Sci USA 85:9797–9800
Dohi Y, Lüscher TF (1991) Endothelin in hypertensive resistance arteries. Intraluminal and extraluminal dysfunction. Hypertension 18:543–549
Strachan FE, Spratt JC, Wilkinson IB, Johnston NR, Gray GA, Webb DJ (1999) Systemic blockade of the endothelin-B receptor increases peripheral vascular resistance in healthy men. Hypertension 33:581–585
Hjortdal VE, Hauge EM, Hansen ES, Sörensen SS (1994) Differential release of endothelin in myocutaneous island flaps in response to gradually insetting venous stasis or arterial ischemia. Metabolism 43:1201–1206
Inoue H, Aihara M, Tomioka M, Ishida H (1998) Changes in endothelin-1, 6-keto-PG-F1 alpha, and TX-B2 in random pattern flaps. J Cardiovasc Pharmacol 31(Suppl 1):S477–S479
Mobley SR, Glassberg MK, Luebke A, Perlyn CA, Davis RE (2003) Expression of endothelin 1 in rat random-pattern skin flaps treated with topical nifedipine. Arch Facial Plast Surg 5:78–82
Tuominen HP, Svartling NE, Tikkanen IT, Saijonmaa O, Asko-Seljavaara S (1995) Perioperative plasma endothelin-1 concentrations and vasoconstriction during prolonged plastic surgical procedures. Br J Anaesth 74:661–666
Harder Y, Amon M, Erni D, Menger MD (2004) Evolution of ischemic tissue injury in a random pattern flap: a new mouse model using intravital microscopy. J Surg Res 121:197–205
Lehr HA, Leunig M, Menger MD, Nolte D, Messmer K (1993) Dorsal skinfold chamber technique for intravital microscopy in nude mice. Am J Pathol 143:1055–1062
Klyscz T, Junger M, Jung F, Zeintl H (1997) Cap image—a new kind of computer-assisted video image analysis system for dynamic capillary microscopy. Biomed Tech 42:168–175
Gross JF, Aroesty J (1972) Mathematical models of capillary flow: a critical review. Biorheology 9:225–264
Harder Y, Amon M, Georgi M, Banic A, Erni D, Menger MD (2005) Evolution of a “falx lunatica” in demarcation of critically ischemic myocutaneous tissue. Am J Physiol Heart Circ Physiol 288:H1224–H1232
Angel MF, Mellow CG, Knight KR, O’Brien BM (1990) Secondary ischemia time in rodents: contrasting complete pedicle interruption with venous obstruction. Plast Reconstr Surg 85:789–793, discussion 794–785
Cocks TM, Faulkner NL, Sudhir K, Angus J (1989) Reactivity of endothelin-1 on human and canine large veins compared with large arteries in vitro. Eur J Pharmacol 171:17–24
Sasser JM, Sullivan JC, Hobbs JL, Yamamoto T, Pollock DM, Carmines PK, Pollock JS (2007) Endothelin a receptor blockade reduces diabetic renal injury via an anti-inflammatory mechanism. J Am Soc Nephrol 18:143–154
Clozel M, Gray GA (1995) Are there different ETB receptors mediating constriction and relaxation? J Cardiovasc Pharmacol 26(Suppl 3):S262–S264
Haefliger IO, Flammer J, Lüscher TF (1992) Nitric oxide and endothelin-1 are important regulators of human ophthalmic artery. Invest Ophthalmol Vis Sci 33:2340–2343
Boldrini L, Pistolesi S, Gisfredi S, Ursino S, Ali G, Pieracci N, Basolo F, Parenti G, Fontanini G (2006) Expression of endothelin 1 and its angiogenic role in meningiomas. Virchows Arch 449:546–553
Acknowledgments
Y. H. is a recipient of a fellowship of the Swiss National Science Foundation (SNF-no. PBBSB-102601), the “Freiwillige Akademische Gesellschaft” (FAG) and the “Margarete und Walter Lichtenstein Stiftung, Medical Department” in Basel, Switzerland.
Author information
Authors and Affiliations
Corresponding author
Additional information
Best abstracts - Surgical Forum 2007
Rights and permissions
About this article
Cite this article
Wettstein, R., Mörsdorf, P., Bächle, A. et al. Selective blockade of endothelin-B receptor improves survival of critically perfused musculocutaneous flaps. Langenbecks Arch Surg 392, 331–338 (2007). https://doi.org/10.1007/s00423-007-0163-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-007-0163-8