Abstract
Background and aims
Since introduction of total mesorectal excision (TME) the prognosis of rectal cancer patients has improved significantly. Debate exists regarding the optimal mode of multimodal treatment. The aim of this survey was to determine the preferred multimodal treatment and the significance and acceptance of short-term radiotherapy (5 × 5 Gy) in Germany.
Methods
In August 2003, a questionnaire was sent to the heads of all 1,275 surgical and 157 radiotherapy departments in Germany.
Results
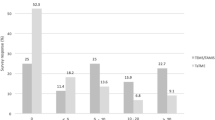
Four hundred ninety-three of 1,275 surgical (39%) and 89 of 157 radiotherapeutic questionnaires (56%) were returned. The majority of the answering surgeons and radiotherapists performed adjuvant (89 and 100%), followed by neoadjuvant (61 and 94%) and short-term radiotherapy (5 × 5 Gy) (16 and 17%). Other questions of the survey dealt with indications for each treatment modality, the initiation of treatment, and reasons for objection to short term radiotherapy.
Conclusion
Short-tem radiotherapy played a minor role in the treatment of rectal cancer patients in 2003 and was mainly initiated by surgeons (∼70%). However, 74% of the answering surgeons and 42% of the answering radiotherapists not performing short-term radiotherapy in 2003 were open minded towards the introduction of this treatment modality.







Similar content being viewed by others
References
Boyle P (1998) Some recent developments in the epidemiology of colorectal cancer. In: Bleiberg H, Rougier P, Wilke HJ (eds) Management of colorectal cancer. Martin Dunitz, London, p 19–34
Hermanek P, Wiebelt H, Staimmer D, Riedl S, German study group colorectal carcinoma (1995) Prognostic factors of rectum carcinoma-experience of the German multicentre study SGCRC. Tumori 81(3 Suppl):60–64, (May)
Rodel C, Hohenberger W, Sauer R (1998) Adjuvant and neoadjuvant therapy of rectal carcinoma. The current status. Strahlenther Onkol 174(10):497–504, (October)
Heald RJ, Husband EM, Ryall RD (1982) The mesorectum in rectal cancer surgery—the clue to pelvic recurrence? Br J Surg 69(10):613–616, (October)
Heald RJ, Ryall RD (1986) Recurrence and survival after total mesorectal excision for rectal cancer. Lancet 1(8496):1479–1482, (June 28)
Kapiteijn E, Marijnen CA, Nagtegaal ID, Putter H, Steup WH, Wiggers T, Rutten HJ, Pahlman L, Glimelius B, van Krieken JH, Leer JW, van de Velde CJ (2001) Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer. N Engl J Med 345(9):638–646, (August 30)
Marijnen CA, Kapiteijn E, van d, V, Martijn H, Steup WH, Wiggers T, Kranenbarg EK, Leer JW (2002) Acute side effects and complications after short-term preoperative radiotherapy combined with total mesorectal excision in primary rectal cancer: report of a multicenter randomized trial. J Clin Oncol 120(3):817–825, (February)
Sauer R, Becker H, Hohenberger W, Rodel C, Wittekind C, Fietkau R, Martus P, Tschmelitsch J, Hager E, Hess CF, Karstens JH, Liersch T, Schmidberger H, Raab R (2004) Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med 351(17):1731–1740, (October 21)
Stockholm rectal cancer study group (1990) Preoperative short-term radiation therapy in operable rectal carcinoma. A prospective randomized trial. Cancer 66(1):49–55, (July 1)
Pollack J, Holm T, Cedermark B, Altman D, Holmstrom B, Glimelius B, Mellgren A (2006) Late adverse effects of short-course preoperative radiotherapy in rectal cancer. Br J Surg 93(12):1519–1525, (December)
Bujko K, Nowacki MP, Nasierowska-Guttmejer A, Michalski W, Bebenek M, Kryj M (2006) Long-term results of a randomized trial comparing preoperative short-course radiotherapy with preoperative conventionally fractionated chemoradiation for rectal cancer. Br J Surg 93(10):1215–1223, (October)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ulrich, A., Schwerdt, J., Z`graggen, K. et al. Acceptance of neoadjuvant short-term radiotherapy: a survey under surgeons and radiotherapists. Langenbecks Arch Surg 392, 525–533 (2007). https://doi.org/10.1007/s00423-006-0139-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-006-0139-0