Abstract
Background and aims
Despite advances in primary care, trauma in conjunction with shock remains the leading cause for morbidity and mortality of young adults in western countries. Herein, we report on the efficiency of small-volume resuscitation to improve compromised perfusion of traumatised skeletal muscle tissue in shock.
Methods
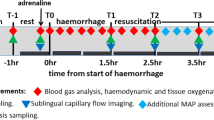
In pentobarbital anaesthetised, mechanically ventilated rats, closed soft-tissue trauma of the right hind limb was induced, followed by induction of haemorrhagic shock [mean arterial blood pressure (MAP) 40 mmHg for 1 h]. For resuscitation, animals received saline (four-times the shed blood volume/20 min), 10% hydroxyethyl starch (HES) 200/0.5 (equal to shed blood volume/5 min) or 7.2% sodium chloride/6% hydroxyethyl starch 200/0.5 (HyperHES; 10% of shed blood volume/2 min). At 2 h of resuscitation, traumatised skeletal muscle tissue was analysed by in vivo microscopy. Non-resuscitated animals served as shock controls.
Results
Despite incomplete restoration of systemic blood pressure, HyperHES was superior to saline, but not to HES, with respect to amelioration of nutritive perfusion. Inflammatory cell response within the traumatised skeletal muscle tissue escaped from the anti-adhesive properties of HyperHES when applied for resuscitation from hypovolaemic shock, and did not differ from values in HES-treated and saline-treated animals.
Conclusion
Resuscitation with HyperHES is as effective as HES in improving capillary perfusion in traumatised skeletal muscle during haemorrhagic shock. However, because values of functional capillary density in the HyperHES-treated and HES-treated animals were still markedly below those reported in traumatised skeletal muscle of normovolaemic animals, further tools are needed to enhance efficiency in treatment of local skeletal muscle tissue injury during haemorrhagic shock.


Similar content being viewed by others
References
Wang P, Ba ZF, Burkhardt J, Chaudry IH (1992) Measurement of hepatic blood flow after severe hemorrhage: lack of restoration despite adequate resuscitation. Am J Physiol 262:G92–G98
Wang P, Hauptman JG, Chaudry IH (1990) Hemorrhage produces depression in microvascular blood flow which persists despite fluid resuscitation. Circ Shock 32:307–318
Vollmar B, Lang G, Menger MD, Messmer K (1994) Hypertonic hydroxyethyl starch restores hepatic microvascular perfusion in hemorrhagic shock. Am J Physiol 266:H1927–H1934
Vollmar B, Preissler G, Menger MD (1996) Small-volume resuscitation restores hemorrhage-induced microcirculatory disorders in rat pancreas. Crit Care Med 24:445–450
Mittlmeier T, Vollmar B, Menger MD, Schewior L, Raschke M, Schaser KD (2003) Small volume hypertonic hydroxyethyl starch reduces acute microvascular dysfunction after closed soft-tissue trauma. J Bone Joint Surg Br 85:126–132
Schaser KD, Vollmar B, Menger MD, Schewior L, Kroppenstedt SN, Raschke M, Lubbe AS, Haas NP, Mittlmeier T (1999) In vivo analysis of microcirculation following closed soft-tissue injury. J Orthop Res 17:678–685
Dixon CE, Clifton GL, Lighthall JW, Yaghmai AA, Hayes RL (1991) A controlled cortical impact model of traumatic brain injury in the rat. J Neurosci Methods 39:253–262
Lighthall JW, Dixon CE, Anderson TE (1989) Experimental models of brain injury. J Neurotrauma 6:83–97
Tyml K, Budreau C (1991) A new preparation of the rat extensor digitorum longus muscle for intravital investigation of the microcirculation. Int J Microcirc Clin Exp 10:335–343
Vollmar B, Burkhardt M, Minor T, Klauke H, Menger MD (1997) High-resolution microscopic determination of hepatic NADH fluorescence for in vivo monitoring of tissue oxygenation during hemorrhagic shock and resuscitation. Microvasc Res 54:164–173
Chance B, Cohen P, Jöbsis F, Schoener B (1962) Intracellular oxidation–reduction states in vivo. The microfluorometry of pyridine nucleotide gives a continuous measurement of the oxidation state. Science 137:499–508
Ince C, Coremans JM, Bruining HA (1992) In vivo NADH fluorescence. Adv Exp Med Biol 317:277–296
Mazzoni MC, Borgstrom P, Intaglietta M, Arfors KE (1989) Lumenal narrowing and endothelial cell swelling in skeletal muscle capillaries during hemorrhagic shock. Circ Shock 29:27–39
Mazzoni MC, Borgstrom P, Intaglietta M, Arfors KE (1990) Capillary narrowing in hemorrhagic shock is rectified by hyperosmotic saline–dextran reinfusion. Circ Shock 31:407–418
Menger MD, Rücker M, Vollmar B (1997) Capillary dysfunction in striated muscle ischemia/reperfusion: on the mechanisms of capillary “no-reflow”. Shock 8:2–7
Kreimeier U, Bruckner UB, Niemczyk S, Messmer K (1990) Hyperosmotic saline dextran for resuscitation from traumatic-hemorrhagic hypotension: effect on regional blood flow. Circ Shock 32:83–99
Kreimeier U, Frey L, Messmer K (1993) Small volume resuscitation. Curr Opin Anaesth 6:400–408
Kreimeier U, Christ F, Frey L, Habler O, Thiel M, Welte M, Zwissler B, Peter K (1997) Small volume resuscitation for hypovolemic shock. Concept, experimental and clinical results. Anaesthesist 46:309–328
Kreimeier U, Peter K, Messmer K (2001) Small volume—large benefits? Anaesthesist 50:442–449
Mazzoni MC, Borgstrom P, Arfors KE, Intaglietta M (1988) Dynamic fluid redistribution in hyperosmotic resuscitation of hypovolemic hemorrhage. Am J Physiol 255: H629–H637
Menth-Chiari WA, Curl WW, Rosencrance E, Smith TL (1998) Contusion of skeletal muscle increases leukocyte–endothelial cell interactions: an intravital-microscopy study in rats. J Trauma 45:709–714
Author information
Authors and Affiliations
Corresponding author
Additional information
The paper was presented at the International Symposium on Significance of Musculo-Skeletal Soft Tissue on Pre-Operative Planning, Surgery and Healing, 13–14 February 2003, Berlin, Germany
Rights and permissions
About this article
Cite this article
Gierer, P., Vollmar, B., Schaser, KD. et al. Efficiency of small-volume resuscitation in restoration of disturbed skeletal muscle microcirculation after soft-tissue trauma and haemorrhagic shock. Langenbecks Arch Surg 389, 40–45 (2004). https://doi.org/10.1007/s00423-003-0433-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-003-0433-z