Abstract
Purpose
Ischemic preconditioning (IPC) in humans has been demonstrated to confer ergogenic benefit to aerobic exercise performance, with an improvement in the response rate when the IPC stimulus is combined with concurrent exercise. Despite potential performance improvements, the nature of the neuronal and humoral mechanisms of conferral and their respective contributions to ergogenic benefit remain unclear. We sought to examine the effects of the humoral component of ischemic preconditioning on skeletal muscle tissue using preconditioned human serum and isolated mouse soleus.
Methods
Isolated mouse soleus was electrically stimulated to contract while in human serum preconditioned with either traditional (IPC) or augmented (AUG) ischemic preconditioning compared to control (CON) and exercise (ERG) preconditioning. Force frequency (FF) curves, twitch responses, and a fatigue-recovery protocol were performed on muscles before and after the addition of serum. After preconditioning, human participants performed a 4 km cycling time trial in order to identify responders and non-responders to IPC.
Results
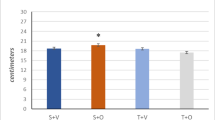
No differences in indices of contractile function, fatiguability, nor recovery were observed between conditions in mouse soleus muscles. Further, no human participants improved performance in a 4-km cycling time trial in response to traditional nor augmented ischemic preconditioning compared to control or exercise conditions (CON 407.7 ± 41.1 s, IPC 411.6 ± 41.9 s, ERG 408.8 ± 41.4 s, AUG 414.1 ± 41.9 s).
Conclusions
Our findings do not support the conferral of ergogenic benefit via a humoral component of IPC at the intracellular level. Ischemic preconditioning may not manifest prominently at submaximal exercise intensities, and augmented ischemic preconditioning may have a hormetic relationship with performance improvements.





Similar content being viewed by others
Availability of data and material
Available upon request.
Code availability
Not applicable.
Abbreviations
- ATP:
-
Adenosine triphosphate
- BFR:
-
Blood flow restriction
- CSA:
-
Cross-sectional area
- CV:
-
Coefficient of variation
- DHPR:
-
Dihydropyridine receptor
- EMS:
-
Electrical muscle stimulation
- FF:
-
Force frequency
- GET:
-
Gas exchange threshold
- IPC:
-
Ischemic preconditioning
- IR:
-
Ischemic reperfusion
- KH:
-
Krebs–Henseleit
- L0 :
-
Optimal length
- LMM:
-
Linear mixed model
- LOP:
-
Limb occlusion pressure
- MVC:
-
Maximal voluntary contraction
- PCr:
-
Phosphocreatine
- PPO:
-
Maximal aerobic power
- (RM)-ANOVA:
-
(Repeated measures) analysis of variance
- RyR:
-
Ryanodine receptor
- SBP:
-
Systolic blood pressure
- SD:
-
Standard deviation
- SERCA:
-
Sarcoplasmic reticulum calcium ATPase
- SR:
-
Sarcoplasmic reticulum
- TTE:
-
Time to exhaustion
- TTP:
-
Time to peak
- TR50:
-
Half-relaxation time
- VAS:
-
Visual analog scale
- VO2 max:
-
Maximal oxygen consumption
References
Addison PD, Neligan PC, Ashrafpour H et al (2003) Noninvasive remote ischemic preconditioning for global protection of skeletal muscle against infarction. Am J Physiol Heart Circ Physiol 285:1435–1443. https://doi.org/10.1152/ajpheart.00106.2003
Basalay M, Barsukevich V, Mastitskaya S et al (2012) Remote ischaemic pre- and delayed postconditioning—similar degree of cardioprotection but distinct mechanisms. Exp Physiol 97:908–917. https://doi.org/10.1113/expphysiol.2012.064923
Behrens M, Zschorlich V, Mittlmeier T et al (2020) Ischemic preconditioning did not affect central and peripheral factors of performance fatigability after submaximal isometric exercise. Front Physiol 11:1–14. https://doi.org/10.3389/fphys.2020.00371
Caru M, Levesque A, Lalonde F, Curnier D (2019) An overview of ischemic preconditioning in exercise performance: a systematic review. J Sport Heal Sci 8:355–369. https://doi.org/10.1016/j.jshs.2019.01.008
Christiansen D, Olsen CBL, Kehler F et al (2022) Active relative to passive ischemic preconditioning enhances intense endurance performance in well-trained men. Int J Sports Physiol Perform. https://doi.org/10.1123/ijspp.2021-0397
Clevidence MW, Mowery RE, Kushnick MR (2012) The effects of ischemic preconditioning on aerobic and anaerobic variables associated with submaximal cycling performance. Eur J Appl Physiol 112:3649–3654. https://doi.org/10.1007/s00421-012-2345-5
Cocking S, Wilson MG, Nichols D et al (2017) Is there an optimal ischaemic preconditioning dose to improve cycling performance. Int J Sports Physiol Perform 13(3):274–282
Craig NP, Norton KI (2001) Characteristics of track cycling. Sport Med 31:457–468
Crisafulli A, Tangianu F, Tocco F et al (2011) Ischemic preconditioning of the muscle improves maximal exercise performance but not maximal oxygen uptake in humans. J Appl Physiol 111:530–536. https://doi.org/10.1152/japplphysiol.00266.2011
da Mota GR, Willis SJ, Dos Santos SN et al (2019) Ischemic preconditioning maintains performance on two 5-km time trials in hypoxia. Med Sci Sports Exerc 51:2309–2317. https://doi.org/10.1249/MSS.0000000000002049
Dickson EW, Lorbar M, Porcaro WA et al (1999a) Rabbit heart can be “preconditioned” via transfer of coronary effluent. Am J Physiol Heart Circ Physiol 277:2451–2457. https://doi.org/10.1152/ajpheart.1999.277.6.h2451
Dickson EW, Reinhardt CP, Renzi FP et al (1999b) Ischemic preconditioning may be transferable via whole blood transfusion: preliminary evidence. J Thromb Thrombolysis 8:123–129. https://doi.org/10.1023/A:1008911101951
Dickson EW, Tubbs RJ, Porcaro WA et al (2002) Myocardial preconditioning factors evoke mesenteric ischemic tolerance via opioid receptors and KATP channels. Am J Physiol Heart Circ Physiol 283:22–28. https://doi.org/10.1152/ajpheart.01055.2001
Eddleston J, Christiansen SC, Zuraw BL (2006) Kinins and neuropeptides: bradykinin. Encycl Respir Med 4:502–506. https://doi.org/10.1016/B0-12-370879-6/00209-X
El Messaoudi S, Vissers A, Thijssen D et al (2013) The effect of remote ischemic preconditioning on exercise-induced plasma troponin I appearance in healthy volunteers. Int J Cardiol 168:1612–1613. https://doi.org/10.1016/j.ijcard.2013.01.029
Enko K, Nakamura K, Yunoki K et al (2011) Intermittent arm ischemia induces vasodilatation of the contralateral upper limb. J Physiol Sci 61:507–513. https://doi.org/10.1007/s12576-011-0172-9
Felippe LC, Ferreira GA, Learsi SK et al (2018) Caffeine increases both total work performed above critical power and peripheral fatigue during a 4-km cycling time trial. J Appl Physiol 124:1491–1501. https://doi.org/10.1152/japplphysiol.00930.2017
Foley KM, Kourides IA, Inturrisi CE et al (1979) β-Endorphin: analgesic and hormonal effects in humans. Proc Natl Acad Sci USA 76:5377–5381. https://doi.org/10.1073/pnas.76.10.5377
Foster GP, Westerdahl DE, Foster LA et al (2011) Ischemic preconditioning of the lower extremity attenuates the normal hypoxic increase in pulmonary artery systolic pressure. Respir Physiol Neurobiol 179:248–253. https://doi.org/10.1016/j.resp.2011.09.001
Hakim TS, Sugimori K, Camporesi EM, Andersen G (1996) Half-life of nitric oxide in aqueous solutions with and without haemoglobin. Physiol Meas 17:267–277. https://doi.org/10.1088/0967-3334/17/4/004
Hausenloy DJ, Yellon DM (2008) Remote ischaemic preconditioning: underlying mechanisms and clinical application. Cardiovasc Res 79:377–386. https://doi.org/10.1093/cvr/cvn114
Hettinga FJ, De Koning JJ, Foster C (2009) V̇O2 response in supramaximal cycling time trial exercise of 750 to 4000 m. Med Sci Sports Exerc 41:230–236. https://doi.org/10.1249/MSS.0b013e3181831f0f
Hittinger EA, Maher JL, Nash MS et al (2014) Ischemic preconditioning does not improve peak exercise capacity at sea level or simulated high altitude in trained male cyclists. Appl Physiol Nutr Metab 40:65–71. https://doi.org/10.1139/apnm-2014-0080
Horiuchi M, Endo J, Thijssen DHJ (2015) Impact of ischemic preconditioning on functional sympatholysis during handgrip exercise in humans. Physiol Rep 3:1–9. https://doi.org/10.14814/phy2.12304
Incognito AV, Burr JF, Millar PJ (2016) The effects of ischemic preconditioning on human exercise performance. Sport Med 46:531–544. https://doi.org/10.1007/s40279-015-0433-5
Jean-St-Michel E, Manlhiot C, Li J et al (2011) Remote preconditioning improves maximal performance in highly trained athletes. Med Sci Sports Exerc 43:1280–1286. https://doi.org/10.1249/MSS.0b013e318206845d
Kharbanda RK, Mortensen UM, White PA et al (2002) Transient limb ischemia induces remote ischemic preconditioning in vivo. Circulation 106:2881–2883. https://doi.org/10.1161/01.CIR.0000043806.51912.9B
Kilding AE, Sequeira GM, Wood MR (2018) Effects of ischemic preconditioning on economy, VO2 kinetics and cycling performance in endurance athletes. Eur J Appl Physiol 118:2541–2549. https://doi.org/10.1007/s00421-018-3979-8
Koch S, Della-Morte D, Dave KR et al (2014) Biomarkers for ischemic preconditioning: finding the responders. J Cereb Blood Flow Metab 34(6):933–941
Kraus AS, Pasha EP, Machin DR et al (2015) Bilateral upper limb remote ischemic preconditioning improves anaerobic power. Open Sport Med J 9:1–6. https://doi.org/10.2174/1874387001509010001
Loenneke JP, Allen KM, Mouser JG et al (2015) Blood flow restriction in the upper and lower limbs is predicted by limb circumference and systolic blood pressure. Eur J Appl Physiol 115:397–405. https://doi.org/10.1007/s00421-014-3030-7
Loukogeorgakis SP, Panagiotidou AT, Broadhead MW et al (2005) Remote ischemic preconditioning provides early and late protection against endothelial ischemia-reperfusion injury in humans: role of the autonomic nervous system. J Am Coll Cardiol 46:450–456. https://doi.org/10.1016/j.jacc.2005.04.044
Mastitskaya S, Marina N, Gourine A et al (2012) Cardioprotection evoked by remote ischaemic preconditioning is critically dependent on the activity of vagal pre-ganglionic neurones. Cardiovasc Res 95:487–494. https://doi.org/10.1093/cvr/cvs212
McIlvenna LC, Muggeridge DJ, Forrest LJ et al (2019) Lower limb ischemic preconditioning combined with dietary nitrate supplementation does not influence time-trial performance in well-trained cyclists. J Sci Med Sport 22:852–857. https://doi.org/10.1016/j.jsams.2019.01.011
Michelsen MM, Støttrup NB, Schmidt MR et al (2012) Exercise-induced cardioprotection is mediated by a bloodborne, transferable factor. Basic Res Cardiol. https://doi.org/10.1007/s00395-012-0260-x
Murrant CL, Barclay JK (1995) Endothelial cell products alter mammalian skeletal muscle function in vitro. Can J Physiol Pharmacol 73:736–741. https://doi.org/10.1139/y95-096
Murrant CL, Woodley NE, Barclay JK (1994) Effect of nitroprusside and endothelium-derived products on slow-twitch skeletal muscle function in vitro. Can J Physiol Pharmacol 72:1089–1093. https://doi.org/10.1139/y94-152
Murry CE, Jennings RB, Reimer KA (1986) Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation 74:1124–1136. https://doi.org/10.1161/01.CIR.74.5.1124
O’Brien L, Jacobs I (2021) Methodological variations contributing to heterogenous ergogenic responses to ischemic preconditioning. Front Physiol 12:1–12. https://doi.org/10.3389/fphys.2021.656980
Pang CY, Yang RZ, Zhong A et al (1995) Acute ischaemic preconditioning protects against skeletal muscle infarction in the pig. Cardiovasc Res 29:782–788. https://doi.org/10.1016/0008-6363(96)88613-5
Pantely GA, Bristow JD (1990) Adenosine. renewed interest in an old drug. Circulation 82:1854–1856. https://doi.org/10.1161/01.CIR.82.5.1854
Paradis-Deschênes P, Joanisse DR, Billaut F (2018) Ischemic preconditioning improves time trial performance at moderate altitude. Med Sci Sports Exerc 50:533–541. https://doi.org/10.1249/MSS.0000000000001473
Paradis-Deschênes P, Joanisse DR, Mauriège P, Billaut F (2020) Ischemic preconditioning enhances aerobic adaptations to sprint-interval training in athletes without altering systemic hypoxic signaling and immune function. Front Sport Act Living 2:1–16. https://doi.org/10.3389/fspor.2020.00041
Patel HH, Moore J, Hsu AK, Gross GJ (2002) Cardioprotection at a distance: mesenteric artery occlusion protects the myocardium via an opioid sensitive mechanism. J Mol Cell Cardiol 34:1317–1323. https://doi.org/10.1006/jmcc.2002.2072
Przyklenk K, Bauer B, Ovize M et al (1993) Regional ischemic “preconditioning” protects remote virgin myocardium from subsequent sustained coronary occlusion. Circulation 87:893–899. https://doi.org/10.1161/01.cir.87.3.893
Saito T, Komiyama T, Aramoto H et al (2004) Ischemic preconditioning improves oxygenation of exercising muscle in vivo. J Surg Res 120:111–118. https://doi.org/10.1016/j.jss.2003.12.021
Salvador AF, De Aguiar RA, Lisbôa FD et al (2016) Ischemic preconditioning and exercise performance: a systematic review and meta-analysis. Int J Sports Physiol Perform 11:4–14. https://doi.org/10.1123/ijspp.2015-0204
Shimizu M, Tropak M, Diaz RJ et al (2009) Transient limb ischaemia remotely preconditions through a humoral mechanism acting directly on the myocardium: evidence suggesting cross-species protection. Clin Sci 117:191–200. https://doi.org/10.1042/CS20080523
Slysz JT, Burr JF (2018) Enhanced metabolic stress augments ischemic preconditioning for exercise performance. Front Physiol. https://doi.org/10.3389/fphys.2018.01621
Slysz JT, Petrick HL, Marrow JP, Burr JF (2019) An examination of individual responses to ischemic preconditioning and the effect of repeated ischemic preconditioning on cycling performance. Eur J Sport Sci. https://doi.org/10.1080/17461391.2019.1651401
Tomschi F, Niemann D, Bloch W et al (2018) Ischemic preconditioning enhances performance and erythrocyte deformability of responders. Int J Sports Med 39:596–603. https://doi.org/10.1055/a-0631-2887
Veighey K, MacAllister RJ (2012) Clinical applications of remote ischemic preconditioning. Cardiol Res Pract. https://doi.org/10.1155/2012/620681
Wang WZ, Stepheson LL, Fang XH et al (2004) Ischemic preconditioning-induced microvascular protection at a distance. J Reconstr Microsurg 20:175–181. https://doi.org/10.1055/s-2004-820775
Warburton DER, Jamnik V, Bredin SSD, Gledhill N (2014) The 2014 physical activity readiness questionnaire for everyone (PAR-Q+) and electronic physical activity readiness medical examination (ePARmed-X+). Heal Fit J Canada 7:80–83
Funding
This work was supported by a Discovery Grant from the Natural Sciences and Engineering Research Council of Canada (grant #03974 to JFB), and the Canada Foundation for Innovation (grant #460597 to JFB).
Author information
Authors and Affiliations
Contributions
All authors contributed to research conception, design, data interpretation, and editing. WNM conducted experiments, analyzed data, and drafted the manuscript. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None.
Ethical approval
This study was carried out in accordance with the University research ethics board (REB # 19-03-011), and all subjects provided written informed consent in accordance with the Declaration of Helsinki.
Consent to participate
All participants provide written informed consent.
Consent to publication
All authors and participants provided written informed consent for publication.
Additional information
Communicated by Michalis G Nikolaidis.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Morley, W.N., Murrant, C.L. & Burr, J.F. Ergogenic effect of ischemic preconditioning is not directly conferred to isolated skeletal muscle via blood. Eur J Appl Physiol 123, 1851–1861 (2023). https://doi.org/10.1007/s00421-023-05197-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-023-05197-1