Abstract
Purpose
Klotho is a cytoprotective protein that increases during acute physiological stressors (e.g., exercise heat stress), although age-related declines in klotho may underlie cellular vulnerability to heat stress. The present study aimed to compare serum klotho in healthy older men and men with type 2 diabetes (T2D) or hypertension (HTN) during prolonged exercise in temperate or hot conditions.
Methods
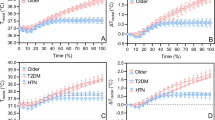
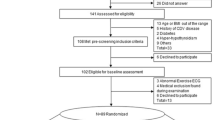
We evaluated serum klotho in 12 healthy older men (mean [SD]; 59 years [4]), 10 men with HTN (60 years [4]), and 9 men with T2D (60 years [5]) before and after 180 min of moderate-intensity (fixed metabolic rate of 200 W/m2; ~ 3.4 METs) exercise and 60 min of recovery in temperate (wet-bulb globe temperature (WBGT) 16 °C) and hot (WBGT 32 °C) environments. Core temperature (rectal), heart rate (HR), and heart rate reserve (HRR) were measured continuously while klotho was measured at the end of baseline, exercise, and recovery.
Results
Total exercise duration was reduced during the hot condition in older men with HTN and T2D than healthy older men (both p ≤ 0.049), despite similar core temperatures, HR, and HRR. Klotho was higher than rest following exercise in the heat in healthy older men (+ 191 pg/mL [189]; p < 0.001) and responses were greater (p = 0.036) than men with HTN (+ 118 pg/mL [49]; p = 0.030), although klotho did not increase in men with T2D (+ 4 pg/mL [71]; p ≥ 0.638).
Conclusion
Given klotho’s role in cytoprotection, older men with HTN and especially T2D may be at increased cellular vulnerability to prolonged exercise or physically demanding exercise in the heat.


Similar content being viewed by others
Data availability
Data are available on request from the corresponding author.
Abbreviations
- ANOVA:
-
Analysis of variance
- ELISA:
-
Enzyme-linked immunosorbent assay
- HR:
-
Heart rate
- HRR:
-
Heart rate reserve
- HTN:
-
Hypertension
- MET:
-
Metabolic equivalent of task
- ROS:
-
Reactive oxygen species
- RH:
-
Relative humidity
- SD:
-
Standard deviation
- T2D:
-
Type 2 diabetes
- WBGT:
-
Wet bulb globe temperature
References
Alkalbani M, Prabhu G, Lagbo J, Qayyum R (2022) Serum klotho and pulse pressure; insight from NHANES. Int J Cardiol 355:54–58. https://doi.org/10.1016/j.ijcard.2022.02.021
Avin KG, Coen PM, Huang W, Stolz DB, Sowa GA, Dube JJ, Goodpaster BH, O’Doherty RM, Ambrosio F (2014) Skeletal muscle as a regulator of the longevity protein, klotho. Front Physiol 5:189. https://doi.org/10.3389/fphys.2014.00189
Cheng YW, Hung CC, Fang WH, Chen WL (2022) Association between soluble alpha-klotho protein and metabolic syndrome in the adult population. Biomolecules. https://doi.org/10.3390/biom12010070
Cheuvront SN, Munoz CX, Kenefick RW (2016) The void in using urine concentration to assess population fluid intake adequacy or hydration status. Am J Clin Nutr 104(3):553–556. https://doi.org/10.3945/ajcn.115.129858
CSEP (1986) Certified fitness appraiser resource manual. determination of aerobic power. Canadian Society for Exercise Physiology, Gloucester, Ontario
Devaraj S, Syed B, Chien A, Jialal I (2012) Validation of an immunoassay for soluble klotho protein: decreased levels in diabetes and increased levels in chronic kidney disease. Am J Clin Pathol 137(3):479–485. https://doi.org/10.1309/AJCPGPMAF7SFRBO4
D’Souza AW, Notley SR, Kenny GP (2020) The relation between age and sex on whole-body heat loss during exercise-heat stress. Med Sci Sports Exerc 52(10):2242–2249. https://doi.org/10.1249/MSS.0000000000002373
Hu J, Su B, Li X, Li Y, Zhao J (2021) Klotho overexpression suppresses apoptosis by regulating the Hsp70/Akt/Bad pathway in H9c2(2–1) cells. Exp Ther Med 21(5):486. https://doi.org/10.3892/etm.2021.9917
Kanbay M, Demiray A, Afsar B, Covic A, Tapoi L, Ureche C, Ortiz A (2021) Role of klotho in the development of essential hypertension. Hypertension 77(3):740–750. https://doi.org/10.1161/HYPERTENSIONAHA.120.16635
Kenny GP, Vierula M, Mate J, Beaulieu F, Hardcastle SG, Reardon F (2012) A field evaluation of the physiological demands of miners in Canada’s deep mechanized mines. J Occup Environ Hyg 9(8):491–501. https://doi.org/10.1080/15459624.2012.693880
Kenny GP, Stapleton JM, Yardley JE, Boulay P, Sigal RJ (2013) Older adults with type 2 diabetes store more heat during exercise. Med Sci Sports Exerc 45(10):1906–1914. https://doi.org/10.1249/MSS.0b013e3182940836
Kim JH, Hwang KH, Park KS, Kong ID, Cha SK (2015) Biological role of anti-aging protein klotho. J Lifestyle Med 5(1):1–6. https://doi.org/10.15280/jlm.2015.5.1.1
King KE, McCormick JJ, Notley SR, Fujii N, Kenny GP (2022) Serum klotho concentrations in young and older men during prolonged exercise in temperate and hot conditions. Curr Aging Sci. https://doi.org/10.2174/1874609815666220304200939
Knapik JJ, Epstein Y (2019) Exertional heat stroke: pathophysiology, epidemiology, diagnosis, treatment, and prevention. J Spec Oper Med 19(2):108–116. https://doi.org/10.55460/5P2Q-1MBQ
Kuro-o M (2008) Klotho as a regulator of oxidative stress and senescence. Biol Chem 389(3):233–241. https://doi.org/10.1515/BC.2008.028
Kusaba T, Okigaki M, Matui A, Murakami M, Ishikawa K, Kimura T, Sonomura K, Adachi Y, Shibuya M, Shirayama T, Tanda S, Hatta T, Sasaki S, Mori Y, Matsubara H (2010) Klotho is associated with VEGF receptor-2 and the transient receptor potential canonical-1 Ca2+ channel to maintain endothelial integrity. Proc Natl Acad Sci U S A 107(45):19308–19313. https://doi.org/10.1073/pnas.1008544107
Lee PG, Cigolle C, Blaum C (2009) The co-occurrence of chronic diseases and geriatric syndromes: the health and retirement study. J Am Geriatr Soc 57(3):511–516. https://doi.org/10.1111/j.1532-5415.2008.02150.x
Lim SW, Jin L, Luo K, Jin J, Shin YJ, Hong SY, Yang CW (2017) Klotho enhances FoxO3-mediated manganese superoxide dismutase expression by negatively regulating PI3K/AKT pathway during tacrolimus-induced oxidative stress. Cell Death Dis 8(8):e2972. https://doi.org/10.1038/cddis.2017.365
Lin Y, Sun Z (2022) Klotho deficiency-induced arterial calcification involves osteoblastic transition of VSMCs and activation of BMP signaling. J Cell Physiol 237(1):720–729. https://doi.org/10.1002/jcp.30541
McGinn R, Poirier MP, Louie JC, Sigal RJ, Boulay P, Flouris AD, Kenny GP (2017) Increasing age is a major risk factor for susceptibility to heat stress during physical activity. Appl Physiol Nutr Metab 42(11):1232–1235. https://doi.org/10.1139/apnm-2017-0322
Meade RD, D’Souza AW, Krishen L, Kenny GP (2017) The physiological strain incurred during electrical utilities work over consecutive work shifts in hot environments: a case report. J Occup Environ Hyg 14(12):986–994. https://doi.org/10.1080/15459624.2017.1365151
NCDRF Collaboration (2016) Worldwide trends in diabetes since 1980: a pooled analysis of 751 population-based studies with 4.4 million participants. Lancet 387(10027):1513–1530. https://doi.org/10.1016/S0140-6736(16)00618-8
Notley SR, Poirier MP, Sigal RJ, D’Souza A, Flouris AD, Fujii N, Kenny GP (2019) Exercise heat stress in patients with and without type 2 diabetes. JAMA 322(14):1409–1411. https://doi.org/10.1001/jama.2019.10943
Notley SR, Akerman AP, Friesen BJ, Poirier MP, Sigal RJ, Flouris AD, Boulay P, McCourt E, Ruzicka M, Kenny GP (2021) Heat tolerance and occupational heat exposure limits in older men with and without type 2 diabetes or hypertension. Med Sci Sports Exerc 53(10):2196–2206. https://doi.org/10.1249/MSS.0000000000002698
Poulianiti KP, Havenith G, Flouris AD (2019) Metabolic energy cost of workers in agriculture, construction, manufacturing, tourism, and transportation industries. Ind Health 57(3):283–305. https://doi.org/10.2486/indhealth.2018-0075
Pouvreau C, Dayre A, Butkowski EG, de Jong B, Jelinek HF (2018) Inflammation and oxidative stress markers in diabetes and hypertension. J Inflamm Res 11:61–68. https://doi.org/10.2147/JIR.S148911
Rao Z, Zheng L, Huang H, Feng Y, Shi R (2019) alpha-Klotho expression in mouse tissues following acute exhaustive exercise. Front Physiol 10:1498. https://doi.org/10.3389/fphys.2019.01498
Saito Y, Nakamura T, Ohyama Y, Suzuki T, Iida A, Shiraki-Iida T, Kuro-o M, Nabeshima Y, Kurabayashi M, Nagai R (2000) In vivo klotho gene delivery protects against endothelial dysfunction in multiple risk factor syndrome. Biochem Biophys Res Commun 276(2):767–772. https://doi.org/10.1006/bbrc.2000.3470
Slimen IB, Najar T, Ghram A, Dabbebi H, Ben Mrad M, Abdrabbah M (2014) Reactive oxygen species, heat stress and oxidative-induced mitochondrial damage. A review. Int J Hyperthermia 30(7):513–523. https://doi.org/10.3109/02656736.2014.971446
Stapleton JM, Poirier MP, Flouris AD, Boulay P, Sigal RJ, Malcolm J, Kenny GP (2015) Aging impairs heat loss, but when does it matter? J Appl Physiol 118(3):299–309. https://doi.org/10.1152/japplphysiol.00722.2014
Su XM, Yang W (2014) Klotho protein lowered in elderly hypertension. Int J Clin Exp Med 7(8):2347–2350
Takenaka T, Kobori H, Miyazaki T, Suzuki H, Nishiyama A, Ishii N, Yamashita M, Hayashi M (2019) Klotho protein supplementation reduces blood pressure and renal hypertrophy in db/db mice, a model of type 2 diabetes. Acta Physiol (Oxf) 225(2):e13190. https://doi.org/10.1111/apha.13190
Tan SJ, Chu MM, Toussaint ND, Cai MM, Hewitson TD, Holt SG (2018) High-intensity physical exercise increases serum alpha-klotho levels in healthy volunteers. J Circ Biomark 7:1849454418794582. https://doi.org/10.1177/1849454418794582
Thurston RD, Larmonier CB, Majewski PM, Ramalingam R, Midura-Kiela M, Laubitz D, Vandewalle A, Besselsen DG, Muhlbauer M, Jobin C, Kiela PR, Ghishan FK (2010) Tumor necrosis factor and interferon-gamma down-regulate klotho in mice with colitis. Gastroenterology. https://doi.org/10.1053/j.gastro.2009.12.002
Wright HE, McLellan TM, Larose J, Hardcastle SG, Boulay P, Kenny GP (2014) Are circulating cytokine responses to exercise in the heat augmented in older men? Appl Physiol Nutr Metab 39(2):117–123. https://doi.org/10.1139/apnm-2013-0223
Yamamoto M, Clark JD, Pastor JV, Gurnani P, Nandi A, Kurosu H, Miyoshi M, Ogawa Y, Castrillon DH, Rosenblatt KP, Kuro-o M (2005) Regulation of oxidative stress by the anti-aging hormone klotho. J Biol Chem 280(45):38029–38034. https://doi.org/10.1074/jbc.M509039200
Yamazaki Y, Imura A, Urakawa I, Shimada T, Murakami J, Aono Y, Hasegawa H, Yamashita T, Nakatani K, Saito Y, Okamoto N, Kurumatani N, Namba N, Kitaoka T, Ozono K, Sakai T, Hataya H, Ichikawa S, Imel EA, Econs MJ, Nabeshima Y (2010) Establishment of sandwich ELISA for soluble alpha-klotho measurement: age-dependent change of soluble alpha-klotho levels in healthy subjects. Biochem Biophys Res Commun 398(3):513–518. https://doi.org/10.1016/j.bbrc.2010.06.110
Yeganeh-Hajahmadi M, Najafipour H, Rostamzadeh F, Naghibzadeh-Tahami A (2021) Klotho and SIRT1 changes from pre-diabetes to diabetes and pre-hypertension to hypertension. Diabetol Metab Syndr 13(1):115. https://doi.org/10.1186/s13098-021-00736-2
Zhang L, Liu T (2018) Clinical implication of alterations in serum klotho levels in patients with type 2 diabetes mellitus and its associated complications. J Diabetes Complicat 32(10):922–930. https://doi.org/10.1016/j.jdiacomp.2018.06.002
Zhou H, Pu S, Zhou H, Guo Y (2021) Klotho as potential autophagy regulator and therapeutic target. Front Pharmacol 12:755366. https://doi.org/10.3389/fphar.2021.755366
Acknowledgements
We thank all members from the Human and Environmental Physiology Research Unit for their assistance with data collection.
Funding
Project supported by the Ontario Ministry of Labour (16-R-036; funds held by G.P.K.).
Author information
Authors and Affiliations
Contributions
GPK, SRN, PB, NF, and TA conceptualized and designed the research; KEK and JJM performed data collection and blood analysis; KEK performed statistical analysis and prepared figures; KEK and JJM drafted the manuscript; All authors interpreted the results; all authors edited, revised, and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest, financial or otherwise, are declared by the author(s).
Additional information
Communicated by Narihiko kondo.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
King, K.E., McCormick, J.J., Notley, S.R. et al. Serum klotho concentrations in older men with hypertension or type 2 diabetes during prolonged exercise in temperate and hot conditions. Eur J Appl Physiol 123, 1519–1527 (2023). https://doi.org/10.1007/s00421-023-05171-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-023-05171-x