Abstract
Purpose
Impaired cardiorespiratory fitness (CRF) is a predictor of mortality in patients with type 2 diabetes mellitus (T2DM). It is still not known how the exercise hemodynamic response correlates with CRF. The purpose was to assess the correlation between hemodynamic changes and CRF in middle-aged patients with T2DM.
Methods
After 1:1 matching by age and sex, 139 T2DM patients and 139 non-T2DM controls who completed the exercise treadmill test were included. Maximal aerobic capacity (VO2max), exercise-induced changes in heart rate (ΔHR), systolic blood pressure (ΔSBP), diastolic blood pressure (ΔDBP), and rate-pressure product (ΔRPP) were measured. HRR1 was calculated as the maximum heart rate minus the heart rate after 1 min of rest.
Results
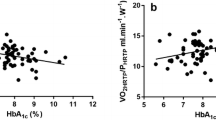
Compared to the control population, T2DM patients had decreased ΔHR (87 (77, 97) v 93 (84, 104) bpm, p < 0.05), ΔRPP (3833.64 ± 1670.34 v 4381.16 ± 1587.78 bpm∙mmHg, p < 0.05), HRR1 (21 (14, 27) v 21 (17, 27) bpm, p < 0.05), and VO2max (32.76 ± 5.63 v 34.68 ± 5.70 ml/kg/min, p < 0.05). Multiple linear regression analysis showed that ΔHR and HRR1, yielded a positive correlation with VO2max in T2DM patients (β = 0.325, P < 0.001; β = 0.173, P = 0.01).
Conclusion
The presence of impaired hemodynamic response and VO2max in middle-aged T2DM patients and the association of impaired ΔHR, HRR1, and VO2max may indicate a physiological pathway of impaired CRF, and our results support the need for cardiorespiratory screening and individualized treatment of middle-aged T2DM patients.

Similar content being viewed by others
Data availability
Due to the privacy of the participants involved in this study, the data sets used and/or analyzed in this study are not publicly available, but can be obtained from the corresponding authors upon reasonable request.
Abbreviations
- ANS:
-
Autonomic Nervous System
- ANSI:
-
Autonomic Nervous System Index
- BMI:
-
Body mass index
- CRF:
-
Cardiorespiratory fitness
- CAN:
-
Cardiac autonomic neuropathy
- DBP :
-
Diastolic blood pressure
- HR:
-
Heart rate
- HDL:
-
High density lipoprotein
- HRV:
-
Heart rate variability
- LDL:
-
Low density lipoprotein
- RPP :
-
Rate-pressure product
- SBP:
-
Systolic blood pressure
- T2DM:
-
Type 2 diabetes mellitus
- VO2max :
-
Maximal aerobic capacity
References
Abushamat LA, McClatchey PM, Scalzo RL, Schauer I, Huebschmann AG, Nadeau KJ, Liu Z, Regensteiner JG, Reusch JEB (2020) mechanistic causes of reduced cardiorespiratory fitness in type 2 diabetes. J Endocr Soc 4(7):bvaa063. https://doi.org/10.1210/jendso/bvaa063
Ansari M, Javadi H, Pourbehi M, Mogharrabi M, Rayzan M, Semnani S, Jallalat S, Amini A, Abbaszadeh M, Barekat M, Nabipour I, Assadi M (2012) The association of rate pressure product (RPP) and myocardial perfusion imaging (MPI) findings: a preliminary study. Perfusion 27(3):207–213. https://doi.org/10.1177/0267659112436631
Azam F, Shaheen A, Irshad K, Liaquat A, Naveed H, Shah SU (2020) Association of postexercise heart rate recovery with body composition in healthy male adults: findings from Pakistan. Ann Noninvasive Electrocardiol 25(3):e12711. https://doi.org/10.1111/anec.12711
Bassan MM (2005) Heart-rate profile during exercise as a predictor of sudden death. N Engl J Med 353(7):734–735. https://doi.org/10.1056/nejm200508183530717
Benichou T, Pereira B, Mermillod M, Tauveron I, Pfabigan D, Maqdasy S, Dutheil F (2018) Heart rate variability in type 2 diabetes mellitus: a systematic review and meta-analysis. PLoS ONE 13(4):e0195166. https://doi.org/10.1371/journal.pone.0195166
Bhati P, Shenoy S, Hussain ME (2018) Exercise training and cardiac autonomic function in type 2 diabetes mellitus: a systematic review. Diabetes Metab Syndr 12(1):69–78. https://doi.org/10.1016/j.dsx.2017.08.015
Brandenburg SL, Reusch JE, Bauer TA, Jeffers BW, Hiatt WR, Regensteiner JG (1999) Effects of exercise training on oxygen uptake kinetic responses in women with type 2 diabetes. Diabetes Care 22(10):1640–1646. https://doi.org/10.2337/diacare.22.10.1640
Buch AN, Coote JH, Townend JN (2002) Mortality, cardiac vagal control and physical training–what’s the link? Exp Physiol 87(4):423–435. https://doi.org/10.1111/j.1469-445x.2002.tb00055.x
Chowdhary S, Townend JN (1999) Role of nitric oxide in the regulation of cardiovascular autonomic control. Clin Sci (lond) 97(1):5–17
Chyun DA, Wackers FJ, Inzucchi SE, Jose P, Weiss C, Davey JA, Heller GV, Iskandrian AE, Young LH (2015) Autonomic dysfunction independently predicts poor cardiovascular outcomes in asymptomatic individuals with type 2 diabetes in the DIAD study. SAGE Open Med 3:2050312114568476. https://doi.org/10.1177/2050312114568476
Dimitropoulos G, Tahrani AA, Stevens MJ (2014) Cardiac autonomic neuropathy in patients with diabetes mellitus. World J Diabetes 5(1):17–39. https://doi.org/10.4239/wjd.v5.i1.17
Ebrahimi H, Emamian MH, Hashemi H, Fotouhi A (2016) High incidence of diabetes mellitus among a middle-aged population in iran: a longitudinal study. Can J Diabetes 40(6):570–575. https://doi.org/10.1016/j.jcjd.2016.05.012
Fitzgerald BT, Ballard EL, Scalia GM (2019) Estimation of the blood pressure response with exercise stress testing. Heart Lung Circ 28(5):742–751. https://doi.org/10.1016/j.hlc.2018.04.279
Foo K, Sekhri N, Knight C, Deaner A, Cooper J, Ranjadayalan K, Suliman A, Timmis AD (2004) The effect of diabetes on heart rate and other determinants of myocardial oxygen demand in acute coronary syndromes. Diabet Med 21(9):1025–1031. https://doi.org/10.1111/j.1464-5491.2004.01413.x
Freeman JV, Dewey FE, Hadley DM, Myers J, Froelicher VF (2006) Autonomic nervous system interaction with the cardiovascular system during exercise. Prog Cardiovasc Dis 48(5):342–362. https://doi.org/10.1016/j.pcad.2005.11.003
González EL, Johansson S, Wallander MA, Rodríguez LA (2009) Trends in the prevalence and incidence of diabetes in the UK: 1996–2005. J Epidemiol Community Health 63(4):332–336. https://doi.org/10.1136/jech.2008.080382
Gusso S, Hofman P, Lalande S, Cutfield W, Robinson E, Baldi JC (2008) Impaired stroke volume and aerobic capacity in female adolescents with type 1 and type 2 diabetes mellitus. Diabetologia 51(7):1317–1320. https://doi.org/10.1007/s00125-008-1012-1
Hillis GS, Hata J, Woodward M, Perkovic V, Arima H, Chow CK, Zoungas S, Patel A, Poulter NR, Mancia G, Williams B, Chalmers J (2012) Resting heart rate and the risk of microvascular complications in patients with type 2 diabetes mellitus. J Am Heart Assoc 1(5):e002832. https://doi.org/10.1161/jaha.112.002832
Hilsted J (1982) Pathophysiology in diabetic autonomic neuropathy: cardiovascular, hormonal, and metabolic studies. Diabetes 31(8 Pt 1):730–737. https://doi.org/10.2337/diab.31.8.730
Jun JE, Lee SE, Choi MS, Park SW, Hwang YC, Kim JH (2019) Clinical factors associated with the recovery of cardiovascular autonomic neuropathy in patients with type 2 diabetes mellitus. Cardiovasc Diabetol 18(1):29. https://doi.org/10.1186/s12933-019-0830-4
Khoshdel AR, Carney SL, White S (2007) Disturbed hemodynamic cardiac exercise stress test response in non-smoking, normolipidemic, normotensive, diabetic subjects. Diabetes Res Clin Pract 75(2):193–199. https://doi.org/10.1016/j.diabres.2006.06.016
Kingwell BA, Dart AM, Jennings GL, Korner PI (1992) Exercise training reduces the sympathetic component of the blood pressure-heart rate baroreflex in man. Clin Sci (lond) 82(4):357–362. https://doi.org/10.1042/cs0820357
Kiviniemi AM, Kenttä TV, Lepojärvi S, Perkiömäki JS, Piira OP, Ukkola O, Huikuri HV, Junttila MJ, Tulppo MP (2019) Recovery of rate-pressure product and cardiac mortality in coronary artery disease patients with type 2 diabetes. Diabetes Res Clin Pract 150:150–157. https://doi.org/10.1016/j.diabres.2019.03.007
Lee J, Vasan RS, Xanthakis V (2020) Association of blood pressure responses to submaximal exercise in midlife with the incidence of cardiovascular outcomes and all-cause mortality: the framingham heart study. J Am Heart Assoc 9(11):e015554. https://doi.org/10.1161/jaha.119.015554
Lind L, Andrén B (2002) Heart rate recovery after exercise is related to the insulin resistance syndrome and heart rate variability in elderly men. Am Heart J 144(4):666–672. https://doi.org/10.1067/mhj.2002.124836
Liu Y, Peng Y, Jin J, Chen Y, Chen C, Chen Z, Huang H, Xu L (2021) Insulin resistance is independently associated with cardiovascular autonomic neuropathy in type 2 diabetes. J Diabetes Investig 12(9):1651–1662. https://doi.org/10.1111/jdi.13507
Lucini D, Zuccotti GV, Scaramuzza A, Malacarne M, Gervasi F, Pagani M (2013) Exercise might improve cardiovascular autonomic regulation in adolescents with type 1 diabetes. Acta Diabetol 50(3):341–349. https://doi.org/10.1007/s00592-012-0416-z
Lucini D, Fallanca A, Malacarne M, Casasco M, Galiuto L, Pigozzi F, Galanti G, Pagani M (2020) Streamlining analysis of RR interval variability in elite soccer players: preliminary experience with a composite indicator of cardiac autonomic regulation. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph17061844
Nunan D, Sandercock GR, Brodie DA (2010) A quantitative systematic review of normal values for short-term heart rate variability in healthy adults. Pacing Clin Electrophysiol 33(11):1407–1417. https://doi.org/10.1111/j.1540-8159.2010.02841.x
O’Connor E, Kiely C, O’Shea D, Green S, Egaña M (2012) Similar level of impairment in exercise performance and oxygen uptake kinetics in middle-aged men and women with type 2 diabetes. Am J Physiol Regul Integr Comp Physiol 303(1):R70-76. https://doi.org/10.1152/ajpregu.00012.2012
Pagani M, Lombardi F, Guzzetti S, Rimoldi O, Furlan R, Pizzinelli P, Sandrone G, Malfatto G, Dell’Orto S, Piccaluga E et al (1986) Power spectral analysis of heart rate and arterial pressure variabilities as a marker of sympatho-vagal interaction in man and conscious dog. Circ Res 59(2):178–193. https://doi.org/10.1161/01.res.59.2.178
Pagkalos M, Koutlianos N, Kouidi E, Pagkalos E, Mandroukas K, Deligiannis A (2008) Heart rate variability modifications following exercise training in type 2 diabetic patients with definite cardiac autonomic neuropathy. Br J Sports Med 42(1):47–54. https://doi.org/10.1136/bjsm.2007.035303
Perregaux D, Chaudhuri A, Mohanty P, Bukhari L, Wilson MF, Sung BH, Dandona P (1999) Effect of gender differences and estrogen replacement therapy on vascular reactivity. Metabolism 48(2):227–232. https://doi.org/10.1016/s0026-0495(99)90039-2
Pinto TE, Gusso S, Hofman PL, Derraik JG, Hornung TS, Cutfield WS, Baldi JC (2014) Systolic and diastolic abnormalities reduce the cardiac response to exercise in adolescents with type 2 diabetes. Diabetes Care 37(5):1439–1446. https://doi.org/10.2337/dc13-2031
Pop-Busui R, Evans GW, Gerstein HC, Fonseca V, Fleg JL, Hoogwerf BJ, Genuth S, Grimm RH, Corson MA, Prineas R (2010) Effects of cardiac autonomic dysfunction on mortality risk in the action to control cardiovascular risk in diabetes (ACCORD) trial. Diabetes Care 33(7):1578–1584. https://doi.org/10.2337/dc10-0125
Queiroz AC, Rezk CC, Teixeira L, Tinucci T, Mion D, Forjaz CL (2013) Gender influence on post-resistance exercise hypotension and hemodynamics. Int J Sports Med 34(11):939–944. https://doi.org/10.1055/s-0033-1337948
Radice M, Rocca A, Bedon E, Musacchio N, Morabito A, Segalini G (1996) Abnormal response to exercise in middle-aged NIDDM patients with and without autonomic neuropathy. Diabet Med 13(3):259–265. https://doi.org/10.1002/(sici)1096-9136(199603)13:3%3c259::Aid-dia30%3e3.0.Co;2-e
Rajbhandari J, Fernandez CJ, Agarwal M, Yeap BXY, Pappachan JM (2021) Diabetic heart disease: a clinical update. World J Diabetes 12(4):383–406. https://doi.org/10.4239/wjd.v12.i4.383
Röhling M, Strom A, Bönhof G, Püttgen S, Bódis K, Müssig K, Szendrödi J, Markgraf D, Lehr S, Roden M, Ziegler D (2017a) Differential patterns of impaired cardiorespiratory fitness and cardiac autonomic dysfunction in recently diagnosed type 1 and type 2 diabetes. Diabetes Care 40(2):246–252. https://doi.org/10.2337/dc16-1898
Röhling M, Strom A, Bönhof GJ, Roden M, Ziegler D (2017b) Cardiorespiratory fitness and cardiac autonomic function in diabetes. Curr Diab Rep 17(12):125. https://doi.org/10.1007/s11892-017-0959-z
Sala R, Malacarne M, Solaro N, Pagani M, Lucini D (2017) A composite autonomic index as unitary metric for heart rate variability: a proof of concept. Eur J Clin Invest 47(3):241–249. https://doi.org/10.1111/eci.12730
Scott JA, Coombes JS, Prins JB, Leano RL, Marwick TH, Sharman JE (2008) Patients with type 2 diabetes have exaggerated brachial and central exercise blood pressure: relation to left ventricular relative wall thickness. Am J Hypertens 21(6):715–721. https://doi.org/10.1038/ajh.2008.166
Spallone V (2019) Update on the impact, diagnosis and management of cardiovascular autonomic neuropathy in diabetes: what is defined, what is new, and what is unmet. Diabetes Metab J 43(1):3–30. https://doi.org/10.4093/dmj.2018.0259
Standl E, Khunti K, Hansen TB, Schnell O (2019) The global epidemics of diabetes in the 21st century: current situation and perspectives. Eur J Prev Cardiol 26(2 suppl):7–14. https://doi.org/10.1177/2047487319881021
Steinberg HO, Paradisi G, Cronin J, Crowde K, Hempfling A, Hook G, Baron AD (2000) Type II diabetes abrogates sex differences in endothelial function in premenopausal women. Circulation 101(17):2040–2046. https://doi.org/10.1161/01.cir.101.17.2040
Stewart KJ, Sung J, Silber HA, Fleg JL, Kelemen MD, Turner KL, Bacher AC, Dobrosielski DA, DeRegis JR, Shapiro EP, Ouyang P (2004) Exaggerated exercise blood pressure is related to impaired endothelial vasodilator function. Am J Hypertens 17(4):314–320. https://doi.org/10.1016/s0895-7061(03)01003-3
Verma S, Moiz JA, Anwer S, Alghadir AH, Hussain ME (2018) A dose-response study of aerobic training for oxygen uptake, oxidative stress and cardiac autonomic function in type 2 diabetes mellitus: study protocol for a randomized controlled trial. Trials 19(1):289. https://doi.org/10.1186/s13063-018-2671-y
Vinik AI, Ziegler D (2007) Diabetic cardiovascular autonomic neuropathy. Circulation 115(3):387–397. https://doi.org/10.1161/circulationaha.106.634949
Voss A, Schroeder R, Heitmann A, Peters A, Perz S (2015) Short-term heart rate variability–influence of gender and age in healthy subjects. PLoS ONE 10(3):e0118308. https://doi.org/10.1371/journal.pone.0118308
Wackers FJ, Young LH, Inzucchi SE, Chyun DA, Davey JA, Barrett EJ, Taillefer R, Wittlin SD, Heller GV, Filipchuk N, Engel S, Ratner RE, Iskandrian AE (2004) Detection of silent myocardial ischemia in asymptomatic diabetic subjects: the DIAD study. Diabetes Care 27(8):1954–1961. https://doi.org/10.2337/diacare.27.8.1954
Wei M, Gibbons LW, Kampert JB, Nichaman MZ, Blair SN (2000) Low cardiorespiratory fitness and physical inactivity as predictors of mortality in men with type 2 diabetes. Ann Intern Med 132(8):605–611. https://doi.org/10.7326/0003-4819-132-8-200004180-00002
zhengzhen W (2018) ACSM’S guidelines for exercise testing and prescription tenth edition.Beijing Sports University Peking
Acknowledgements
The authors are very grateful to The Second Affiliated Hospital of Fujian University of Traditional Chinese Medicine for their support of the data and to all participants for their contributions.
Funding
This work was supported by the Key Research and Development Project funded by the Ministry of Science and Technology of the People’s Republic of China (Grant Number: 2019YFC1710301).
Author information
Authors and Affiliations
Contributions
LHY and JH contributed to study design, and data collection and analysis were performed by YX, YNC, and JWQ. The first draft of the manuscript was written by JJX. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the Ethics Committee of The Second Affiliated Hospital of Fujian University of Traditional Chinese Medicine and the procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Informed consent
All participants provided written informed consent.
Additional information
Communicated by Massimo Pagani.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Xie, J., Yin, L., Huang, J. et al. Correlation between impaired hemodynamic response and cardiopulmonary fitness in middle-aged type 2 diabetes mellitus patients: a case–control study. Eur J Appl Physiol 122, 2295–2303 (2022). https://doi.org/10.1007/s00421-022-05008-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-022-05008-z