Abstract
Purpose
Exercise prescription based on a population-specific physiological response can help ensure safe and effective physical interventions. However, as a facile approach for exercise prescription in hemodialysis population that is based on their exercise capacity has not yet been established, the aim of our study was to develop a unique prediction formula for peak heart rate (HR) that can be used in this population.
Methods
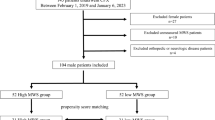
This cross-sectional study measured physical function and HR at peak exercise and anaerobic threshold (AT) during cardiopulmonary exercise tests in 126 individuals. Participants were randomly assigned to the development group (n = 78), whose data were used to calculate the prediction equation, or the validation group (n = 48).
Results
The HR reserve in this population was significantly lower (0.44 ± 0.20%) and there was a large discrepancy between conventional age-predicted maximal HR and measured peak-HR values (R = 0.36). The average of the ratio between HR at AT point and peak HR was 85% (95% CI, 83.5%–86.4%). The peak-HR prediction equation was based on resting HR, presence of diabetes, physical dysfunction (gait speed < 1.0 m/s), and hypoalbuminemia (< 3.5 g/dL). It showed high prediction accuracy (R2 [95%CI] = 0.71 [0.70–0.71]) with similar correlation coefficients between the development and validation groups (R = 0.82).
Conclusion
Aerobic exercise based on estimated peak HR < 85% obtained from the equation in this study may enable safe and effective physical intervention in this population.





Similar content being viewed by others
Abbreviations
- AT:
-
Anaerobic threshold
- HR:
-
Heart rate
- CPET:
-
Cardiopulmonary exercise test
References
American College of Sports Medicine (2016) ACSM’s Guidelines for Exercise Testing and Prescription. 10th ed. Wolters Kluwer Health
Arai Y, Saul JP, Albrecht P, Hartley LH, Lilly LS, Cohen RJ, Colucci WS (1989) Modulation of cardiac autonomic activity during and immediately after exercise. Am J Physiol 256(1 Pt 2):H132-141. https://doi.org/10.1152/ajpheart.1989.256.1.H132
Azarbal B, Hayes SW, Lewin HC, Hachamovitch R, Cohen I, Berman DS (2004) The incremental prognostic value of percentage of heart rate reserve achieved over myocardial perfusion single-photon emission computed tomography in the prediction of cardiac death and all-cause mortality: superiority over 85% of maximal age-predicted heart rate. J Am Coll Cardiol 44(2):423–430. https://doi.org/10.1016/j.jacc.2004.02.060
Balady GJ, Arena R, Sietsema K, Myers J, Coke L, Fletcher GF, Forman D, Franklin B, Guazzi M, Gulati M, Keteyian SJ, Lavie CJ, Macko R, Mancini D, Milani RV (2010) Clinician’s guide to cardiopulmonary exercise testing in adults: a scientific statement from the american heart association. Circulation 122(2):191–225. https://doi.org/10.1161/CIR.0b013e3181e52e69
Bonaz B, Sinniger V, Pellissier S (2017) The vagus nerve in the neuro-immune axis: implications in the pathology of the gastrointestinal tract. Front Immunol 8:1452. https://doi.org/10.3389/fimmu.2017.01452
Brubaker PH, Kitzman DW (2011) Chronotropic incompetence: causes, consequences, and management. Circulation 123(9):1010–1020. https://doi.org/10.1161/circulationaha.110.940577
Chan CT, Levin NW, Chertow GM, Larive B, Schulman G, Kotanko P (2010) Determinants of cardiac autonomic dysfunction in ESRD. Clin J Am Soc Nephrol 5(10):1821–1827. https://doi.org/10.2215/cjn.03080410
Duan H, Cai X, Luan Y, Yang S, Yang J, Dong H, Zeng H, Shao L (2021) Regulation of the autonomic nervous system on intestine. Front Physiol 12:700129. https://doi.org/10.3389/fphys.2021.700129
Fletcher GF, Balady GJ, Amsterdam EA, Chaitman B, Eckel R, Fleg J, Froelicher VF, Leon AS, Piña IL, Rodney R, Simons-Morton DA, Williams MA, Bazzarre T (2001) Exercise standards for testing and training: a statement for healthcare professionals from the American heart association. Circulation 104(14):1694–1740. https://doi.org/10.1161/hc3901.095960
Foley RN, Parfrey PS, Sarnak MJ (1998) Epidemiology of cardiovascular disease in chronic renal disease. J Am Soc Nephrol 9(12 Suppl):S16-23
Fouque D, Kalantar-Zadeh K, Kopple J, Cano N, Chauveau P, Cuppari L, Franch H, Guarnieri G, Ikizler TA, Kaysen G, Lindholm B, Massy Z, Mitch W, Pineda E, Stenvinkel P, Treviño-Becerra A, Wanner C (2008) A proposed nomenclature and diagnostic criteria for protein-energy wasting in acute and chronic kidney disease. Kidney Int U S. https://doi.org/10.1038/sj.ki.5002585
Gronwald T, Törpel A, Herold F, Budde H (2020) Perspective of dose and response for individualized physical exercise and training prescription. J Funct Morphol Kinesiol. https://doi.org/10.3390/jfmk5030048
Gulati M, Shaw LJ, Thisted RA, Black HR, Bairey Merz CN, Arnsdorf MF (2010) Heart rate response to exercise stress testing in asymptomatic women: the st. James Women Take Heart Project Circulation 122(2):130–137. https://doi.org/10.1161/circulationaha.110.939249
Hilderman M, Bruchfeld A (2020) The cholinergic anti-inflammatory pathway in chronic kidney disease-review and vagus nerve stimulation clinical pilot study. Nephrol Dial Transplant 35(11):1840–1852. https://doi.org/10.1093/ndt/gfaa200
Hiraki K, Yasuda T, Hotta C, Izawa KP, Morio Y, Watanabe S, Sakurada T, Shibagaki Y, Kimura K (2013) Decreased physical function in pre-dialysis patients with chronic kidney disease. Clin Exp Nephrol 17(2):225–231. https://doi.org/10.1007/s10157-012-0681-8
Ikizler TA, Cano NJ, Franch H, Fouque D, Himmelfarb J, Kalantar-Zadeh K, Kuhlmann MK, Stenvinkel P, TerWee P, Teta D, Wang AY, Wanner C (2013) Prevention and treatment of protein energy wasting in chronic kidney disease patients: a consensus statement by the international society of renal nutrition and metabolism. Kidney Int 84(6):1096–1107. https://doi.org/10.1038/ki.2013.147
Imai K, Sato H, Hori M, Kusuoka H, Ozaki H, Yokoyama H, Takeda H, Inoue M, Kamada T (1994) Vagally mediated heart rate recovery after exercise is accelerated in athletes but blunted in patients with chronic heart failure. J Am Coll Cardiol 24(6):1529–1535. https://doi.org/10.1016/0735-1097(94)90150-3
Kanda E, Kato A, Masakane I, Kanno Y (2019) A new nutritional risk index for predicting mortality in hemodialysis patients: Nationwide cohort study. PLoS ONE 14(3):e0214524. https://doi.org/10.1371/journal.pone.0214524
Klein DA, Katz DH, Beussink-Nelson L, Sanchez CL, Strzelczyk TA, Shah SJ (2015) Association of chronic kidney disease with chronotropic incompetence in heart failure with preserved ejection fraction. Am J Cardiol 116(7):1093–1100. https://doi.org/10.1016/j.amjcard.2015.06.038
Mann T, Lamberts RP, Lambert MI (2013) Methods of prescribing relative exercise intensity: physiological and practical considerations. Sports Med 43(7):613–625. https://doi.org/10.1007/s40279-013-0045-x
McAdams-DeMarco MA, Law A, Salter ML, Boyarsky B, Gimenez L, Jaar BG, Walston JD, Segev DL (2013) Frailty as a novel predictor of mortality and hospitalization in individuals of all ages undergoing hemodialysis. J Am Geriatr Soc 61(6):896–901. https://doi.org/10.1111/jgs.12266
Meyer T, Gabriel HH, Kindermann W (1999) Is determination of exercise intensities as percentages of VO2max or HRmax adequate? Med Sci Sports Exerc 31(9):1342–1345. https://doi.org/10.1097/00005768-199909000-00017
Pu J, Jiang Z, Wu W, Li L, Zhang L, Li Y, Liu Q, Ou S (2019) Efficacy and safety of intradialytic exercise in haemodialysis patients: a systematic review and meta-analysis. BMJ Open 9(1):e020633. https://doi.org/10.1136/bmjopen-2017-020633
Salhab N, Karavetian M, Kooman J, Fiaccadori E, El Khoury CF (2019) Effects of intradialytic aerobic exercise on hemodialysis patients: a systematic review and meta-analysis. J Nephrol 32(4):549–566. https://doi.org/10.1007/s40620-018-00565-z
Satake S, Arai H (2020) The revised Japanese version of the Cardiovascular Health Study criteria (revised J-CHS criteria). Geriatr Gerontol Int 20(10):992–993. https://doi.org/10.1111/ggi.14005
Scharhag-Rosenberger F, Meyer T, Gässler N, Faude O, Kindermann W (2010) Exercise at given percentages of VO2max: heterogeneous metabolic responses between individuals. J Sci Med Sport 13(1):74–79. https://doi.org/10.1016/j.jsams.2008.12.626
Siamopoulos KC, Tsianos EV, Dardamanis M, Berecos C (1990) Esophageal dysfunction in chronic hemodialysis patients. Nephron 55(4):389–393. https://doi.org/10.1159/000186006
Tanaka H, Monahan KD, Seals DR (2001) Age-predicted maximal heart rate revisited. J Am Coll Cardiol 37(1):153–156. https://doi.org/10.1016/s0735-1097(00)01054-8
The Japanese Society of Renal Rehabilitation (2018) Guideline for renal rehabilitation. Nankodo, Tokyo
Usui N, Yokoyama M, Nakata J, Suzuki Y, Tsubaki A, Kojima S, Inatsu A, Hisadome H, Uehata A (2021) Association between social frailty as well as early physical dysfunction and exercise intolerance among older patients receiving hemodialysis. Geriatr Gerontol Int 21(8):664–669. https://doi.org/10.1111/ggi.14223
Vinik AI, Erbas T, Casellini CM (2013) Diabetic cardiac autonomic neuropathy, inflammation and cardiovascular disease. J Diabetes Investig 4(1):4–18. https://doi.org/10.1111/jdi.12042
Wasserman K (1986) The anaerobic threshold: definition, physiological significance and identification. Adv Cardiol 35:1–23
Wasserman K, Stringer WW, Casaburi R, Koike A, Cooper CB (1994) Determination of the anaerobic threshold by gas exchange: biochemical considerations, methodology and physiological effects. Z Kardiol 83(Suppl 3):1–12
Whipp BJ, Davis JA, Torres F, Wasserman K (1981) A test to determine parameters of aerobic function during exercise. J Appl Physiol Respir Environ Exerc Physiol 50(1):217–221. https://doi.org/10.1152/jappl.1981.50.1.217
Williams DP, Koenig J, Carnevali L, Sgoifo A, Jarczok MN, Sternberg EM, Thayer JF (2019) Heart rate variability and inflammation: a meta-analysis of human studies. Brain Behav Immun 80:219–226. https://doi.org/10.1016/j.bbi.2019.03.009
Young HML, March DS, Graham-Brown MPM, Jones AW, Curtis F, Grantham CS, Churchward DR, Highton P, Smith AC, Singh SJ, Bridle C, Burton JO (2018) Effects of intradialytic cycling exercise on exercise capacity, quality of life, physical function and cardiovascular measures in adult haemodialysis patients: a systematic review and meta-analysis. Nephrol Dial Transplant 33(8):1436–1445. https://doi.org/10.1093/ndt/gfy045
Acknowledgements
This work was supported by the Kisen Hospital. The authors wish to express heartfelt appreciation to the personnel and patients at the institutions participating in this survey.
Author information
Authors and Affiliations
Contributions
HO, NU, AT, and AU. contributed to the study conception and design. AU, AI, HH, SK., and NU. collected data. SA, MS, SO, and N.U. analyzed and interpreted data. OH. and NU. drafted the manuscript. All authors contributed to critically reviewed the manuscript and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interests
No conflicts of interest, financial or otherwise, are declared by the authors.
Ethical approval
This study was approved by the Ethics Review Board at Kisen Hospital. (Approval number: 2021–11–001).
Additional information
Communicated by Massimo Pagani.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Oyanagi, H., Usui, N., Tsubaki, A. et al. An equation to predict peak heart rate for prescribing exercise intensity in middle-aged to older patients requiring hemodialysis. Eur J Appl Physiol 122, 2233–2241 (2022). https://doi.org/10.1007/s00421-022-05002-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-022-05002-5