Abstract
Introduction
Whole body energy expenditure and lipid oxidation (Lox) are upregulated during and after exercise. Persons with spinal cord injury (SCI) generally have a blunted ability to utilize fat during exercise, but it is unknown if their substrate partitioning is affected during recovery from exercise.
Purpose
To determine the effect of a single session of upper body circuit resistance exercise (CRE) on energy expenditure and Lox during exercise recovery in persons with and without SCI.
Methods
Twenty four persons (3 groups; 7 male and 1 female per group) without paralysis (neurologically intact; N) or with chronic (≥ 1 yr) paraplegia (P) or tetraplegia (T) participated. Energy expenditure and substrate partitioning were assessed via indirect calorimetry before, during, and three times after (up to 120 min after) a single session of CRE, or time-matched seated control (CON).
Results
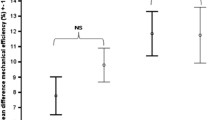
During CRE, all groups experienced a similar relative increase in oxygen consumption (49 ± 13, 55 ± 11, and 48 ± 15% VO2peak for N, P, and T, respectively). The Post0-120 energy expenditure was greater following CRE vs. CON (P < 0.01) and independent of injury characteristics (10.6, 22.6, and 14.3% higher than CON for N, P, and T; P = 0.21). The absolute increase in Lox above CON during recovery was similar for N, P, and T (5.74 ± 2.81, 6.62 ± 3.10, and 4.50 ± 3.91 g, respectively; P = 0.45).
Conclusions
Energy expenditure and lipid utilization was increased similarly following circuit exercise in persons without and with spinal cord injury in a manner independent of level of injury.


Similar content being viewed by others
Availability of data and materials
The data maintained and managed by the authors of the study. The corresponding author can be contacted with requests to access data.
References
College of Sports Medicine., Howley ET, Franklin BM, Whaley MH, Balady GJ, A (2013) ACSM’s guidelines for exercise testing and prescription, 9th edn. Lippincott williams & wilkins, Philadelphia
Astorino TA, Harness ET (2009) Substrate metabolism during exercise in the spinal cord injured. Eur J Appl Physiol 106(2):187–193. https://doi.org/10.1007/s00421-009-1005-x
Bauman WA, Spungen AM (2001) Carbohydrate and lipid metabolism in chronic spinal cord injury. J Spin Cord Med 24(4):266–277
Biering-Sorensen F, Biering-Sorensen T, Liu N, Malmqvist L, Wecht JM, Krassioukov A (2018) Alterations in cardiac autonomic control in spinal cord injury. Auton Neurosci 209:4–18. https://doi.org/10.1016/j.autneu.2017.02.004
Borsheim E, Bahr R (2003) Effect of exercise intensity, duration and mode on post-exercise oxygen consumption. Sports Med 33(14):1037–1060. https://doi.org/10.2165/00007256-200333140-00002
Braun WA, Hawthorne WE, Markofski MM (2005) Acute EPOC response in women to circuit training and treadmill exercise of matched oxygen consumption. Eur J Appl Physiol 94(5–6):500–504
Brooks GA, Fahey TD, Baldwin KM (2005) Exercise physiology: human bioenergetics and its appliaction, 4th edn. McGraw-Hill, New York
Burleson MA Jr, O’Bryant HS, Stone MH, Collins MA, Triplett-McBride T (1998) Effect of weight training exercise and treadmill exercise on post-exercise oxygen consumption. Med Sci Sports Exerc 30(4):518–522
Campbell WW, Kraus WE, Powell KE, Haskell WL, Janz KF, Jakicic JM, Troiano RP, Sprow K, Torres A, Piercy KL, Bartlett DB, Advisory PAG, C, (2019) High-intensity interval training for cardiometabolic disease prevention. Med Sci Sports Exerc 51(6):1220–1226. https://doi.org/10.1249/MSS.0000000000001934
Center NSCIS (2020) Facts and figures at a glance. university of alabama at birmingham, Birmingham
Davitt PM, Arent SM, Tuazon MA, Golem DL, Henderson GC (2013) Postprandial triglyceride and free fatty acid metabolism in obese women after either endurance or resistance exercise. J Appl Physiol 114(12):1743–1754. https://doi.org/10.1152/japplphysiol.00095.2013
de Groot S, Adriaansen JJ, Tepper M, Snoek GJ, van der Woude LH, Post MW (2016) Metabolic syndrome in people with a long-standing spinal cord injury: associations with physical activity and capacity. Appl Physiol Nutr Metab 41(11):1190–1196. https://doi.org/10.1139/apnm-2016-0269
Durstine JL, Grandjean PW, Davis PG, Ferguson MA, Alderson NL, DuBose KD (2001) Blood lipid and lipoprotein adaptations to exercise: a quantitative analysis. Sports Med 31(15):1033–1062
Emmons RR, Cirnigliaro CM, Kirshblum SC, Bauman WA (2014) The relationship between the postprandial lipemic response and lipid composition in persons with spinal cord injury. J Spinal Cord Med 37(6):765–773. https://doi.org/10.1179/2045772314y.0000000231
Frayn KN (1983) Calculation of substrate oxidation rates in vivo from gaseous exchange. J Appl Physiol: Respir, Environ Exerc Physiol 55(2):628–634
Haugen HA, Melanson EL, Tran ZV, Kearney JT, Hill JO (2003) Variability of measured resting metabolic rate. Am J Clinic Nutr 78(6):1141–1145
Henderson GC, Alderman BL (2014) Determinants of resting lipid oxidation in response to a prior bout of endurance exercise. J Appl Physiol 116(1):95–103. https://doi.org/10.1152/japplphysiol.00956.2013
Henderson GC, Fattor JA, Horning MA, Faghihnia N, Luke-Zeitoun M, Brooks GA (2007) Retention of intravenously infused [13C]bicarbonate is transiently increased during recovery from hard exercise. J Appl Physiol 103(5):1604–1612. https://doi.org/10.1152/japplphysiol.00309.2007
Hojman P, Brolin C, Norgaard-Christensen N, Dethlefsen C, Lauenborg B, Olsen CK, Abom MM, Krag T, Gehl J, Pedersen BK (2019) IL-6 release from muscles during exercise is stimulated by lactate-dependent protease activity. Am J Physiol Endocrinol Metab 316(5):E940–E947
Jacobs BP, Kressler J, Nash M (2013) Heavy reliance on carbohydrate across a wide range of exercise intensities during voluntary arm ergometry in persons with paraplegia. J Spinal Cord Med 36(5):427–435. https://doi.org/10.1179/2045772313Y.0000000123
Jacobs KA, Mahoney ET, Nash MS, Green BA (2002) Circuit resistance training in persons with complete paraplegia. J Rehabil Res Dev 39(1):21–28
Jacobs PL, Nash MS, Rusinowski JW (2001) Circuit training provides cardiorespiratory and strength benefits in persons with paraplegia. Med Sci Sports Exerc 33(5):711–717
Jeukendrup AE, Wallis GA (2005) Measurement of substrate oxidation during exercise by means of gas exchange measurements. Int J Sports Med 26(Suppl 1):S28-37. https://doi.org/10.1055/s-2004-830512
Kang J, Hoffman JR, Wendell M, Walker H, Hebert M (2004) Effect of contraction frequency on energy expenditure and substrate utilisation during upper and lower body exercise. Br J Sports Med 38(1):31–35
Karlsson AK, Elam M, Friberg P, Biering-Sörensen F, Sullivan L, Lönnroth P (1997) Regulation of lipolysis by the sympathetic nervous system: a microdialysis study in normal and spinal cord injured subjects. Metabolism 46(4):388–394
Kjaer M, Dela F, Sorensen FB, Secher NH, Bangsbo J, Mohr T, Galbo H (2001) Fatty acid kinetics and carbohydrate metabolism during electrical exercise in spinal cord-injured humans. Am J Physiol Regul Integr Comp Physiol 281(5):R1492-1498
Kodama S, Tanaka S, Saito K, Shu M, Sone Y, Onitake F, Suzuki E, Shimano H, Yamamoto S, Kondo K, Ohashi Y, Yamada N, Sone H (2007) Effect of aerobic exercise training on serum levels of high-density lipoprotein cholesterol: a meta-analysis. Arch Intern Med 167(10):999–1008. https://doi.org/10.1001/archinte.167.10.999
Kressler J, Burns PA, Betancourt L, Nash MS (2014) Circuit training and protein supplementation in persons with chronic tetraplegia. Med Sci Sports Exerc 46(7):1277–1284. https://doi.org/10.1249/MSS.0000000000000250
Kuo CC, Fattor JA, Henderson GC, Brooks GA (2005) Lipid oxidation in fit young adults during postexercise recovery. J Appl Physiol 99(1):349–356. https://doi.org/10.1152/japplphysiol.00997.2004
La Fountaine MF, Cirnigliaro CM, Kirshblum SC, McKenna C, Bauman WA (2017) Effect of functional sympathetic nervous system impairment of the liver and abdominal visceral adipose tissue on circulating triglyceride-rich lipoproteins. PLoS ONE 12(3):e0173934. https://doi.org/10.1371/journal.pone.0173934
Libin A, Tinsley EA, Nash MS, Mendez AJ, Burns P, Elrod M, Hamm LF, Groah SL (2013) Cardiometabolic risk clustering in spinal cord injury: results of exploratory factor analysis. Top Spinal Cord Inj Rehabil 19(3):183–194. https://doi.org/10.1310/sci1903-183
Martin Ginis KA, van der Scheer JW, Latimer-Cheung AE, Barrow A, Bourne C, Carruthers P, Bernardi M, Ditor DS, Gaudet S, de Groot S, Hayes KC, Hicks AL, Leicht CA, Lexell J, Macaluso S, Manns PJ, McBride CB, Noonan VK, Pomerleau P, Rimmer JH, Shaw RB, Smith B, Smith KM, Steeves JD, Tussler D, West CR, Wolfe DL, Goosey-Tolfrey VL (2018) Evidence-based scientific exercise guidelines for adults with spinal cord injury: an update and a new guideline. Spinal Cord 56(4):308–321. https://doi.org/10.1038/s41393-017-0017-3
Mayhew JL, Ball TE, Bowen JC (1992) Relative muscular endurance performance as a predictor of bench press strength in college men and women. Sports Med Train Rehabil 3:195–201
McCully KK, Mulcahy TK, Ryan TE, Zhao Q (2011) Skeletal muscle metabolism in individuals with spinal cord injury. J Appl Physiol 111(1):143–148. https://doi.org/10.1152/japplphysiol.00094.2011
Nash MS, DeGroot J, Martinez-Arizala A, Mendez AJ (2005) Evidence for an exaggerated postprandial lipemia in chronic paraplegia. J Spinal Cord Med 28(4):320–325
Nash MS, Groah SL, Gater DR, Dyson-Hudson TA, Lieberman JA, Myers J, Sabharwal S, Taylor AJ (2019) Identification and management of cardiometabolic risk after spinal cord injury. J Spinal Cord Med 42(5):643–677
Nash MS, Jacobs PL, Mendez AJ, Goldberg RB (2001) Circuit resistance training improves the atherogenic lipid profiles of persons with chronic paraplegia. J Spinal Cord Med 24(1):2–9
Nash MS, Jacobs PL, Woods JM, Clark JE, Pray TA, Pumarejo AE (2002) A comparison of 2 circuit exercise training techniques for eliciting matched metabolic responses in persons with paraplegia. Arch Phys Med Rehabil 83(1):201–209
Nash MS, van de Ven I, van Elk N, Johnson BM (2007) Effects of circuit resistance training on fitness attributes and upper-extremity pain in middle-aged men with paraplegia. Arch Phys Med Rehabil 88(1):70–75. https://doi.org/10.1016/j.apmr.2006.10.003
Nightingale TE, Metcalfe RS, Vollaard NB, Bilzon JL (2017) Exercise guidelines to promote cardiometabolic health in spinal cord injured humans: time to raise the intensity? Arch Phys Med Rehabil 98(8):1693–1704. https://doi.org/10.1016/j.apmr.2016.12.008
Paoli A, Moro T, Marcolin G, Neri M, Bianco A, Palma A, Grimaldi K (2012) High-Intensity Interval Resistance Training (HIRT) influences resting energy expenditure and respiratory ratio in non-dieting individuals. J Transl Med 10:237. https://doi.org/10.1186/1479-5876-10-237
Schmid A, Huonker M, Barturen JM, Stahl F, Schmidt-Trucksass A, Konig D, Grathwohl D, Lehmann M, Keul J (1998) Catecholamines, heart rate, and oxygen uptake during exercise in persons with spinal cord injury. J Appl Physiol 85(2):635–641
Schuenke MD, Mikat RP, McBride JM (2002) Effect of an acute period of resistance exercise on excess post-exercise oxygen consumption: implications for body mass management. Eur J Appl Physiol 86(5):411–417. https://doi.org/10.1007/s00421-001-0568-y
Scott CB, Leighton BH, Ahearn KJ, McManus JJ (2011) Aerobic, anaerobic, and excess postexercise oxygen consumption energy expenditure of muscular endurance and strength: 1-set of bench press to muscular fatigue. J Strength Cond Res 25(4):903–908. https://doi.org/10.1519/JSC.0b013e3181c6a128
Sedlock DA, Schneider DA, Gass E, Gass G (2004) Excess post-exercise oxygen consumption in spinal cord-injured men. Eur J Appl Physiol 93(1–2):231–236. https://doi.org/10.1007/s00421-004-1205-3
Simmons OL, Kressler J, Nash MS (2014) Reference fitness values in the untrained spinal cord injury population. Arch Phys Med Rehabil 95(12):2272–2278. https://doi.org/10.1016/j.apmr.2014.06.015
Weir JB (1949) New methods for calculating metabolic rate with special reference to protein metabolism. J Physiol 109(1–2):1–9
Whitham M, Parker BL, Friedrichsen M, Hingst JR, Hjorth M, Hughes WE, Egan CL, Cron L, Watt KI, Kuchel RP, Jayasooriah N (2018) Extracellular vesicles provide a means for tissue crosstalk during exercise. Cell Metab 27(1):237–251
Acknowledgements
The authors thank Dr. Gregory Bigford and Dr. Gregory Henderson for their insightful contributions to the manuscript. We also thank Mr. Doyle Freeman and Ms. Amariah Lem for their contributions to data collection and data analysis.
Author information
Authors and Affiliations
Contributions
DWM: contributed to study design, data collection, data analysis/interpretation, and manuscript original draft preparation; JK: contributed to study design, data collection, data analysis/interpretation, and manuscript review/editing; KAJ: contributed to data interpretation and manuscript review/editing; MSN: was the project supervisor and contributed to data interpretation and manuscript review/editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts to report.
Ethical approval
This study was approved by the University of Miami School of Medicine institutional review board (IRB ID: 20140178).
Additional information
Communicated by Philip D. Chilibeck.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
McMillan, D.W., Kressler, J., Jacobs, K.A. et al. Substrate metabolism during recovery from circuit resistance exercise in persons with spinal cord injury. Eur J Appl Physiol 121, 1631–1640 (2021). https://doi.org/10.1007/s00421-021-04629-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-021-04629-0