Abstract
Purpose
Exertional-heat stress adversely disrupts gastrointestinal (GI) barrier integrity, whereby subsequent microbial translocation (MT) can result in potentially serious health consequences. To date, the influence of aerobic fitness on GI barrier integrity and MT following exertional-heat stress is poorly characterised.
Method
Ten untrained (UT; VO2max = 45 ± 3 ml·kg−1·min−1) and ten highly trained (HT; VO2max = 64 ± 4 ml·kg−1·min−1) males completed an ecologically valid (military) 80-min fixed-intensity exertional-heat stress test (EHST). Venous blood was drawn immediately pre- and post-EHST. GI barrier integrity was assessed using the serum dual-sugar absorption test (DSAT) and plasma Intestinal Fatty-Acid Binding Protein (I-FABP). MT was assessed using plasma Bacteroides/total 16S DNA.
Results
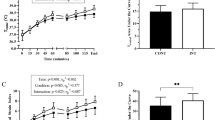
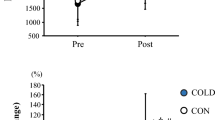
UT experienced greater thermoregulatory, cardiovascular and perceptual strain (p < 0.05) than HT during the EHST. Serum DSAT responses were similar between the two groups (p = 0.59), although Δ I-FABP was greater (p = 0.04) in the UT (1.14 ± 1.36 ng·ml−1) versus HT (0.20 ± 0.29 ng·ml−1) group. Bacteroides/Total 16S DNA ratio was unchanged (Δ; -0.04 ± 0.18) following the EHST in the HT group, but increased (Δ; 0.19 ± 0.25) in the UT group (p = 0.05). Weekly aerobic training hours had a weak, negative correlation with Δ I-FABP and Bacteroides/total 16S DNA responses.
Conclusion
When exercising at the same absolute workload, UT individuals are more susceptible to small intestinal epithelial injury and MT than HT individuals. These responses appear partially attributable to greater thermoregulatory, cardiovascular, and perceptual strain.




Similar content being viewed by others
Abbreviations
- ANOVA:
-
Analysis of variance
- CV:
-
Coefficient of variation
- DSAT:
-
Dual sugar absorption test
- EDTA:
-
Ethylenediaminetetraacetic acid
- EHS:
-
Exertional heat stroke
- EHST:
-
Exertional heat stress test
- ELISA:
-
Enzyme linked immunosorbent assay
- GI:
-
Gastrointestinal
- HPLC:
-
High performance liquid chromatography
- HR:
-
Heart rate
- HT:
-
Highly trained
- I-FABP:
-
Intestinal fatty-acid binding protein
- I-HSP:
-
Intracellular heat shock protein
- ISAK:
-
International Society for the Advancement of Anthropometric Kinanthropometry
- LPS:
-
Lipopolysaccharide
- L/R:
-
Lactulose-to-rhamnose
- MT:
-
Microbial translocation
- qPCR:
-
Quantitative polymerase chain reaction
- RH:
-
Relative humidity
- RPE:
-
Rate of perceived exertion
- SD:
-
Standard deviation
- SEM:
-
Sensor electronics module
- T core :
-
Core body temperature
- T body :
-
Mean body temperature
- T skin :
-
Mean skin temperature
- TS:
-
Thermal sensation
- UT:
-
Untrained
- \(\dot{V}{\text{O}}_{2\max }\) :
-
Maximal oxygen uptake
References
Aguinis H, Gottfredson RK, Joo H (2013) Best-practice recommendations for defining, identifying, and handling outliers. Organ Res Methods 16(2):270–301
Armstrong LE, Lee EC, Armstrong EM (2018) Interactions of gut microbiota, endotoxemia, immune function, and diet in exertional heatstroke. J Sports Med. https://doi.org/10.1155/2018/5724575
Armed Forces Health Surveillance Centre (2020) Update: heat illness, active component, U.S. Armed Forces 2019. Med Surveill Mon Rep 27(4):4–9
Belval LN, Casa DJ, Adams WM, Chiampas GT, Holschen JC, Hosokawa Y, Jardine J, Kane SF, Labotz M, Lemieux RS, McClaine KB (2018) Consensus statement-prehospital care of exertional heat stroke. Prehospital Emerg Care 22(3):392–397
Bischoff SC, Barbara G, Buurman W, Ockhuizen T, Schulzke JD, Serino M, Tilg H, Watson A, Wells JM (2014) Intestinal permeability—a new target for disease prevention and therapy. BMC Gastroenterol 14(1):189
Borg G (1970) Perceived exertion as an indicator of somatic stress. Scand J Rehabil Med 2:92–98
Bosenberg AT, Brock-Utne JG, Gaffin SL, Wells MT, Blake GT (1988) Strenuous exercise causes systemic endotoxemia. J Appl Physiol 65(1):106–108
Bouchama A, Knochel JP (2002) Heat stroke. N Engl J Med 346(25):1978–1988
Camus G, Poortmans J, Nys M, Deby-Dupont G, Duchateau J, Deby C, Lamy M (1997) Mild endotoxaemia and the inflammatory response induced by a marathon race. Clin Sci 92(4):415–422
Cani PD (2018) Human gut microbiome: hopes, threats and promises. Gut 67(9):1716–1725
Casa DJ, Clarkson PM, Roberts WO (2005) American College of Sports Medicine roundtable on hydration and physical activity: consensus statements. Curr Sports Med Rep 4(3):115–127
Cheung SS, McLellan TM (1998) Heat acclimation, aerobic fitness, and hydration effects on tolerance during uncompensable heat stress. J Appl Physiol 84(5):1731–1739
Christensen MJ, Eller E, Kjaer HF, Broesby-Olsen S, Mortz CG, Bindslev-Jensen C (2019) Exercise-induced anaphylaxis: causes, consequences, and management recommendations. Expert Rev Clin Immunol 15(3):265–273
Costa RJS, Snipe RMJ, Kitic CM, Gibson PR (2017) Systematic review: exercise-induced gastrointestinal syndrome—implications for health and intestinal disease. Aliment Pharmacol Ther 46(3):246–265
de Groot DW, Gallimore RP, Thompson SM, Kenefick RW (2013) Extremity cooling for heat stress mitigation in military and occupational settings. J Therm Biol 38(6):305–310
De Jong J, Thompson B, Han A (2019) Methodological recommendations for menstrual cycle research in sports and exercise. Med Sci Sports Exerc 51(12):2610–2617
Deitch EA (2012) Gut-origin sepsis: evolution of a concept. Surgeon 10(6):350–356
Dill DB, Costill DL (1974) Calculation of percentage changes in volumes of blood, plasma, and red cells in dehydration. J Appl Physiol 37(2):247–248
Dokladny K, Zuhl MN, Moseley PL (2016) Intestinal epithelial barrier function and tight junction proteins with heat and exercise. J Appl Physiol 120(6):692–701
Durnin JV, Womersley JV (1974) Body fat assessed from total body density and its estimation from skinfold thickness: measurements on 481 men and women aged from 16 to 72 years. Br J Nutr 32(1):77–97
Edinburgh RM, Hengist A, Smith HA, Travers RL, Koumanov F, Betts JA, Thompson D, Walhin JP, Wallis GA, Hamilton DL, Stevenson EJ (2018) Preexercise breakfast ingestion versus extended overnight fasting increases postprandial glucose flux after exercise in healthy men. Am J Physiol Endocrinol Metab 315(5):1062–1074
Epstein Y, Druyan A, Heled Y (2012) Heat injury prevention—a military perspective. J Strength Cond Res 26:82–86
Epstein Y, Moran DS, Shapiro Y, Sohar E, Shemer J (1999) Exertional heat stroke: a case series. Med Sci Sports Exerc 31(2):224–228
Fallowfield JL, Delves SK, Hill NE, Lanham-New SA, Shaw AM, Brown PE, Bentley C, Wilson DR, Allsopp AJ (2019) Serum 25-hydroxyvitamin D fluctuations in military personnel during 6-month summer operational deployments in Afghanistan. Br J Nutr 121(4):384–392
Fehrenbach E, Niess AM, Veith R, Dickhuth HH, Northoff H (2001) Changes of HSP72-expression in leukocytes are associated with adaptation to exercise under conditions of high environmental temperature. J Leukoc Biol 69(5):747–754
Fleming SC, Duncan A, Russell RI, Laker MF (1996) Measurement of sugar probes in serum: an alternative to urine measurement in intestinal permeability testing. Clin Chem 42(3):445–448
Gaskell SK, Taylor B, Muir J, Costa RJ (2019) Impact of 24-hour high and low fermentable oligo-di-mono-saccharide polyol diets on markers of exercise-induced gastrointestinal syndrome in response to exertional-heat stress. Appl Physiol Nutr Metab. https://doi.org/10.1139/apnm-2019-0187
Gabriel H, Kindermann W (1996) Ultrasound of the abdomen in endurance athletes. Eur J Appl Physiol Occup Physiol 73(1–2):191–193
Havenith G, Luttikholt VG, Vrijkotte TGM (1995) The relative influence of body characteristics on humid heat stress response. Eur J Appl Physiol Occup Physiol 70(3):270–279
Jay O, Kenny GP (2007) The determination of changes in body heat content during exercise using calorimetry and thermometry. J Human Environ Syst 10(1):19–29
Kazman JB, Heled Y, Lisman PJ, Druyan A, Deuster PA, O’Connor FG (2013) Exertional heat illness: the role of heat tolerance testing. Cur Sports Med Rep 12(2):101–105
Komine S, Akiyama K, Warabi E, Oh S, Kuga K, Ishige K, Togashi S, Yanagawa T, Shoda J (2017) Exercise training enhances in vivo clearance of endotoxin and attenuates inflammatory responses by potentiating Kupffer cell phagocytosis. Sci Rep 7(1):1–11
Landers-Ramos RQ, Jenkins NT, Spangenburg EE, Hagberg JM, Prior SJ (2014) Circulating angiogenic and inflammatory cytokine responses to acute aerobic exercise in trained and sedentary young men. Eur J Appl Physiol 114(7):1377–1384
Leon LR, Bouchama A (2011) Heat stroke. Compr Physiol 5(2):611–647
Lim C (2018) Heat sepsis precedes heat toxicity in the pathophysiology of heat stroke—a new paradigm on an ancient disease. Antioxidants 7(11):149
Lippi G, Schena F, Salvagno GL, Montagnana M, Ballestrieri F, Guidi GC (2006) Comparison of the lipid profile and lipoprotein (a) between sedentary and highly trained subjects. Clin Chem Lab Med 44(3):322–326
March DS, Jones AW, Thatcher R, Davison G (2019) The effect of bovine colostrum supplementation on intestinal injury and circulating intestinal bacterial DNA following exercise in the heat. Eur J Nutr 58(4):1441–1451
Marfell-Jones et al (2006) ISAK manual, International standards for anthropometric assessment. In: edited by Marfell-Jones M, Olds T, Stewart A, Lindsay Carter LE. International Society for the Advancement of Kinanthropometry
Met Office (2019) Cambourne. https://www.metoffice.gov.uk/pub/data/weather/uk/climate/stationdata/cambornedata.txt. Accessed 23 Feb 2020
Military Headquarters of the Surgeon General (2019). https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/793094/JSP_539_Part_2_V3.1__Updated_04-19_.pdf. Accessed 24 Mar 2020
Moore AC, Stacey MJ, Bailey KGH, Bunn RJ, Woods DR, Haworth KJ, Brett SJ, Folkes SEF (2016) Risk factors for heat illness among British soldiers in the hot collective training environment. J R Army Med Corps 162(6):434–439
Morrison SA, Cheung SS, Cotter JD (2014) Bovine colostrum, training status, and gastrointestinal permeability during exercise in the heat: a placebo-controlled double-blind study. Appl Physiol Nutr Metab 39(9):1070–1082
Nelson DA, Deuster PA, O'Connor FG, Kurina LM (2018) Timing and predictors of mild and severe heat illness among new military enlistees. Med Sci Sports Exerc 50(8):1603
Ogden HB, Child RB, Fallowfield JL, Delves SK, Westwood CS, Layden JD (2020a) The gastrointestinal exertional heat stroke paradigm: pathophysiology, assessment, severity, aetiology and nutritional countermeasures. Nutrients 12:537
Ogden HB, Fallowfield JL, Child RB, Davison G, Fleming SC, Edinburgh RM, Delves SK, Millyard A, Westwood CS, Layden J (2020b) Reliability of gastrointestinal barrier integrity and microbial translocation biomarkers at rest and following exertional heat stress. Physiol Rep 8:e14374
Païssé S, Valle C, Servant F, Courtney M, Burcelin R, Amar J, Lelouvier B (2016) Comprehensive description of blood microbiome from healthy donors assessed by 16 S targeted metagenomic sequencing. Transfusion 56(5):1138–1147
Pires W, Veneroso CE, Wanner SP, Pacheco DA, Vaz GC, Amorim FT, Tonoli C, Soares DD, Coimbra CC (2017) Association between exercise-induced hyperthermia and intestinal permeability: a systematic review. Sports Med 47(7):1389–1403
Ramanathan NL (1964) A new weighting system for mean surface temperature of the human body. J Appl Physiol 19(3):531–533
Reihmane D, Tretjakovs P, Kaupe J, Sars M, Valante R, Jurka A (2012) Systemic pro-inflammatory molecule response to acute submaximal exercise in moderately and highly trained athletes. Age (years) 26(5):26–32
Sakurada S, Hales JRS (1998) A role for gastrointestinal endotoxins in enhancement of heat tolerance by physical fitness. J Appl Physiol 84(1):207–214
Saltzman JR, Kowdley KV, Perrone G, Russell RM (1995) Changes in small-intestine permeability with aging. J Am Geriatr Soc 43(2):160–164
Saweirs WM, Andrews DJ, Low-Beer TS (1985) The double sugar test of intestinal permeability in the elderly. Age Ageing 14(5):312–315
Sawka MN, Leon LR, Montain SJ, Sonna LA (2011) Integrated physiological mechanisms of exercise performance, adaptation, and maladaptation to heat stress. Compr Physiol 1(4):1883–1928
Selkirk GA, McLellan TM (2001) Influence of aerobic fitness and body fatness on tolerance to uncompensable heat stress. J Appl Physiol 91(5):2055–2063
Selkirk GA, McLellan TM, Wright HE, Rhind SG (2008) Mild endotoxemia, NF-κB translocation, and cytokine increase during exertional heat stress in trained and untrained individuals. Am J Physiol Regul Integr Comp Physiol 295(2):611–623
Selkirk GA, McLellan TM, Wright HE, Rhind SG (2009) Expression of intracellular cytokines, HSP72, and apoptosis in monocyte subsets during exertional heat stress in trained and untrained individuals. Am J Physiol Regul Integr Comp Physiol 296(3):R575–R586
Shirreffs SM, Maughan RJ (1994) The effect of posture change on blood volume, serum potassium and whole body electrical impedance. Eur J Appl Physiol 69(5):461–463
Snipe RM, Khoo A, Kitic CM, Gibson PR, Costa RJ (2018) The impact of exertional-heat stress on gastrointestinal integrity, gastrointestinal symptoms, systemic endotoxin and cytokine profile. Eur J Appl Physiol 118(2):389–400
Spitz MG, Castellani JW, Freund BJ, Sawka MN (2012). https://apps.dtic.mil/dtic/tr/fulltext/u2/a571324.pdf. Accessed 30 Mar 2020
Stacey MJ, Brett S, Woods D, Jackson S, Ross D (2016) Case ascertainment of heat illness in the British Army: evidence of under-reporting from analysis of medical and command notifications, 2009–2013. J R Army Med Corps 162(6):428–433
Stacey MJ, Parsons IT, Woods DR, Taylor PN, Ross D, Brett SJ (2015) Susceptibility to exertional heat illness and hospitalisation risk in UK military personnel. BMJ Open Sport Exerc Med 1(1):e000055
Szymanski MC, Gillum TL, Gould LM, Morin DS, Kuennen MR (2018) Short-term dietary curcumin supplementation reduces gastrointestinal barrier damage and physiological strain responses during exertional heat stress. J Appl Physiol 124(2):330–340
Toner MM, Drolet LL, Pandolf KB (1986) Perceptual and physiological responses during exercise in cool and cold water. Percept Mot Skills 62(1):211–220
van Wijck K, Lenaerts K, Van Bijnen AA, Boonen B, Van Loon LJ, Dejong CH, Buurman WA (2012) Aggravation of exercise-induced intestinal injury by Ibuprofen in athletes. Med Sci Sports Exerc 44(12):2257–2262
van Wijck K, Lenaerts K, Van Loon LJ, Peters WH, Buurman WA, Dejong CH (2011) Exercise-induced splanchnic hypoperfusion results in gut dysfunction in healthy men. PLoS One. https://doi.org/10.1371/journal.pone.0022366
Vargas N, Marino F (2016) Heat stress, gastrointestinal permeability and interleukin-6 signalling—implications for exercise performance and fatigue. Temperature 3(2):240–251
Vincent WJ, Weir JP (1995) Quantifying reliability. In: Statistics in kinesiology, 5th edn. Human Kinetics, Champaign, pp 214–228
Wallace RF, Kriebel D, Punnett L, Wegman DH, Wenger CB, Gardner JW, Kark JA (2006) Risk factors for recruit exertional heat illness by gender and training period. Aviat Space Environ Med 77(4):415–421
Waterhouse J, Drust B, Weinert D, Edwards B, Gregson W, Atkinson G, Kao S, Aizawa S, Reilly T (2005) The circadian rhythm of core temperature: origin and some implications for exercise performance. Chronobiol Int 22(2):207–225
Wells JM, Brummer RJ, Derrien M, MacDonald TT, Troost F, Cani PD, Theodorou V, Dekker J, Méheust A, De Vos WM, Mercenier A (2017) Homeostasis of the gut barrier and potential biomarkers. Am J Physiol Gastrointest Liver Physiol 312(3):171–193
Westwood CS, Fallowfield JL, Delves SK, Nunns M, Ogden HB, Layden JD (2020) Individual risk factors associated with exertional heat illness: a systematic review. Exp Physiol. https://doi.org/10.1113/EP088458
Winter EM, Jones AM, Davison RC, Bromley PD, Mercer TH (2007) The British association of sport and exercise science guidelines, vol 1. Routledge, Oxford
Wright HE, Selkirk GA, McLellan TM (2010) HPA and SAS responses to increasing core temperature during uncompensable exertional heat stress in trained and untrained males. Eur J Appl Physiol 108(5):987–997
Author information
Authors and Affiliations
Contributions
Made substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data; or the creation of new software used in the work: HO, JF, RC, GD, SF, SD, AM, CW, JL. Drafted the work or revised it critically for important intellectual content: HO, JF, RC, GD, SD, JL. Approved the version to be published: HO, JF, RC, GD, SF, SD, AM, CW, JL. Agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved: HO, JF, RC, GD, SF, SD, AM, CW, JL.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Plymouth MARJON University (Approval Code: EP096).
Additional information
Communicated by Narihiko Kondo.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ogden, H.B., Fallowfield, J.L., Child, R.B. et al. Influence of aerobic fitness on gastrointestinal barrier integrity and microbial translocation following a fixed-intensity military exertional heat stress test. Eur J Appl Physiol 120, 2325–2337 (2020). https://doi.org/10.1007/s00421-020-04455-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-020-04455-w