Abstract
Purpose
Human daily total water intake (TWI) has a large inter-individual range. Recently, water supplementation has been suggested as a potential preventative and therapeutic modality. Thus, we aimed to measure hydration biomarkers in women with high (HIGH) versus low (LOW) daily TWI to determine baseline differences, and the efficacy of these markers during a systematic alteration in TWI.
Methods
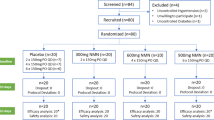
This cohort study identified 14 HIGH [3.34 (0.56) L day−1] and 14 LOW [1.62 (0.48) L day−1] from 120 women. Next, fluid intake was decreased in HIGH [2.00 (0.21) L day−1] while LOW increased [3.50 (0.13) L day−1] across 4 days. Body mass, fluid intake, serum osmolality (S osmo), total plasma protein (TPP), 24 h urine osmolality, and 24 h urine volume, were measured on each day of modified TWI. Estimated plasma volume (E pv) was calculated using measured body mass and hematocrit values.
Results
At baseline, urinary markers and TPP differentiated HIGH from LOW [7.0 (0.3) versus 7.3 (0.3) mg dL−1, respectively]. Upon TWI intervention, (1) body mass decreased in HIGH [−0.7 (1.1) kg, p = 0.010)] but did not increase in LOW [+0.0 (0.6) kg, p = 0.110], (2) E pv decreased 2.1 (2.4) %, p = 0.004, (3) urine osmolality increased in HIGH [397 (144)–605 (230) mOsm kg−1, p < 0.001] and decreased in LOW [726 (248)–265 (97) mOsm kg−1 p < 0.001], and (4) no changes of serum osmolality occurred in either HIGH or LOW (all p > 0.05).
Conclusions
Urinary markers and TPP are sensitive measures to habitual high and low TWI and to changes in TWI. Both groups through urinary and some hematological responses following TWI manipulation achieved regulation of hemoconcentration.


Similar content being viewed by others
Abbreviations
- E pv :
-
Estimated plasma volume
- Hct:
-
Hematocrit (%)
- HIGH:
-
Participant group that habitually consumed 3.34 (0.56) L day−1
- LOW:
-
Participant group that habitually consumed 1.62 (0.48) L day−1
- Serum Cl− :
-
Serum chloride (mmol L−1)
- Serum K+ :
-
Serum potassium (mmol L−1)
- Serum Na+ :
-
Serum sodium (mmol L−1)
- S osmo :
-
Serum osmolality (mOsm kg−1)
- TPP:
-
Total plasma protein (mg dL−1)
- TWI:
-
Total water intake including water from food and beverages
- U col :
-
Urine color
- U osmo :
-
Urine osmolality (mOsm kg-1)
- U sg :
-
Urine specific gravity
- U vol :
-
Volume of urine produced in 24 h urine collection (L)
References
Andersson B (1978) Regulation of water intake. Physiol Rev 58:582
Armstrong LE (2012) Challenges of linking chronic dehydration and fluid consumption to health outcomes. Nutr Rev 70(Suppl 2):S121–S127. doi:10.1111/j.1753-4887.2012.00539.x
Armstrong LE, Maresh CM, Castellani JW et al (1994) Urinary indices of hydration status. Int J Sport Nutr 4:265–279
Armstrong LE, Pumerantz AC, Fiala KA et al (2010) Human hydration indices: acute and longitudinal reference values. Int J Sport Nutr Exerc Metab 20:145–153
Armstrong LE, Johnson EC, Munoz CX et al (2013) Evaluation of Uosm:posm ratio as a hydration biomarker in free-living, healthy young women. Eur J Clin Nutr 67:934–938. doi:10.1038/ejcn.2013.79
Arnaud MJ, Noakes TD (2011) Should humans be encouraged to drink water to excess? Eur J Clin Nutr 65(7):875–876. doi:10.1038/ejcn.2011.40 (author reply 877)
Cairncross S (1997) More water: better health. People Planet 6:10–11
Cheuvront SN, Kenefick RW, Charkoudian N, Sawka MN (2013) Physiologic basis for understanding quantitative dehydration assessment. Am J Clin Nutr 97:455–462. doi:10.3945/ajcn.112.044172
D’Arrigo T (2007) Drink up! The wonder of water. Diabetes Forecast 60:23
Fetissov SO, Thornton SN (2009) Hypovolemia-induced obesity and diabetes. Metab 58:1678. doi:10.1016/j.metabol.2009.06.022 (author reply 1679)
Goodman AB, Blanck HM, Sherry B, Park S, Nebeling L, Yaroch AL (2013) Behaviors and attitudes associated with low drinking water intake among US adults, food attitudes and behaviors survey 2007. Prev Chronic Dis 10:E51. doi:10.5888/pcd10.120248
Greenleaf JE (1992) Problem: thirst, drinking behavior, and involuntary dehydration. Med Sci Sports Exerc 24:645–656
Jequier E, Constant F (2010) Water as an essential nutrient: the physiological basis of hydration. Eur J Clin Nutr 64:115–123. doi:10.1038/ejcn.2009.111
Kant AK, Graubard BI (2010) Contributors of water intake in US children and adolescents: associations with dietary and meal characteristics: National Health and Nutrition Examination Survey 2005–2006. Am J Clin Nutr 92:887–896. doi:10.3945/ajcn.2010.29708
Kaplan AA (1990) A simple and accurate method for prescribing plasma exchange. ASAIO Trans 36:M597–M599
Knepper MA, Star RA (2008) Vasopressin: friend or foe? Nat Med 14:14–16. doi:10.1038/nm0108-14
Lotan Y, Buendia Jimenez I, Lenoir-Wijnkoop I et al (2013) Increased water intake as a prevention strategy for recurrent urolithiasis: major impact of compliance on cost-effectiveness. J Urol 189:935–939. doi:10.1016/j.juro.2012.08.254
Malvin RL, Wilde WS (1959) Washout of renal countercurrent Na gradient by osmotic diuresis. Am J Physiol 197:177–180
Manz F, Wentz A (2003) 24-h Hydration status: parameters, epidemiology and recommendations. Eur J Clin Nutr 57(Suppl 2):S10–S18. doi:10.1038/sj.ejcn.1601896
Manzone TA, Dam HQ, Soltis D, Sagar VV (2007) Blood volume analysis: a new technique and new clinical interest reinvigorate a classic study. J Nucl Med Technol 35(2):55–63. doi:10.2967/jnmt.106.035972 (quiz 77, 79)
McKinley MJ, Cairns MJ, Denton DA et al (2004) Physiological and pathophysiological influences on thirst. Physiol Behav 81:795–803. doi:10.1016/j.physbeh.2004.04.055
Nielsen S, Frokiaer J, Marples D, Kwon TH, Agre P, Knepper MA (2002) Aquaporins in the kidney: from molecules to medicine. Physiol Rev 82:205–244. doi:10.1152/physrev.00024.2001
Nose H, Mack GW, Shi XR, Nadel ER (1988) Role of osmolality and plasma volume during rehydration in humans. J Appl Physiol 65:325–331
Pan A, Malik VS, Hao T, Willett WC, Mozaffarian D, Hu FB (2013) Changes in water and beverage intake and long-term weight changes: results from three prospective cohort studies. Int J Obes (Lond) 37:1378–1385. doi:10.1038/ijo.2012.225
Park S, Blanck HM, Sherry B, Brener N, O’Toole T (2012) Factors associated with low water intake among US high school students—National Youth Physical Activity and Nutrition Study, 2010. J Acad Nutr Diet 112:1421–1427. doi:10.1016/j.jand.2012.04.014
Pedersen RS, Bentzen H, Bech JN, Pedersen EB (2001) Effect of water deprivation and hypertonic saline infusion on urinary AQP2 excretion in healthy humans. Am J Physiol Renal Physiol 280:F860–F867
Perrier E, Demazieres A, Girard N et al (2013a) Circadian variation and responsiveness of hydration biomarkers to changes in daily water intake. Eur J Appl Physiol 113:2143–2151. doi:10.1007/s00421-013-2649-0
Perrier E, Rondeau P, Poupin M et al (2013b) Relation between urinary hydration biomarkers and total fluid intake in healthy adults. Eur J Clin Nutr 67:939–943. doi:10.1038/ejcn.2013.93
Perrier E, Vergne S, Klein A et al (2013c) Hydration biomarkers in free-living adults with different levels of habitual fluid consumption. Br J Nutr 109:1678–1687. doi:10.1017/S0007114512003601
Perrier ET, Armstrong LE, Daudon M et al (2014) From state to process: defining hydration. Obes Facts 7(Suppl 2):6–12. doi:10.1159/000360611
Popkin BM, D’Anci KE, Rosenberg IH (2010) Water, hydration, and health. Nutr Rev 68:439–458. doi:10.1111/j.1753-4887.2010.00304.x
Pross N, Demazieres A, Girard N et al (2014) Effects of changes in water intake on mood of high and low drinkers. PLoS One 9:e94754. doi:10.1371/journal.pone.0094754
Roussel R, Fezeu L, Bouby N et al (2011) Low water intake and risk for new-onset hyperglycemia. Diabetes Care 34:2551–2554. doi:10.2337/dc11-0652
Sawka MN, Coyle EF (1999) Influence of body water and blood volume on thermoregulation and exercise performance in the heat. Exerc Sport Sci Rev 27:167–218
Shafiee MA, Charest AF, Cheema-Dhadli S et al (2005) Defining conditions that lead to the retention of water: the importance of the arterial sodium concentration. Kidney Int 67:613–621. doi:10.1111/j.1523-1755.2005.67117.x
Shoker AS (1994) Application of the clearance concept to hyponatremic and hypernatremic disorders: a phenomenological analysis. Clin Chem 40:1220–1227
Stachenfeld NS, Silva C, Keefe DL, Kokoszka CA, Nadel ER (1999) Effects of oral contraceptives on body fluid regulation. J Appl Physiol 87:1016–1025
Strippoli GF, Craig JC, Rochtchina E, Flood VM, Wang JJ, Mitchell P (2011) Fluid and nutrient intake and risk of chronic kidney disease. Nephrol (Carlton) 16:326–334. doi:10.1111/j.1440-1797.2010.01415.x
Thornton SN, Trabalon M (2012) Dehydration during sleep affects cognitive performance. Sleep Med 13:118. doi:10.1016/j.sleep.2011.06.018 (author reply 118–9)
U.S. Department of Health and Human Services, National Center for Health Statistics (1988–1994.) Third National Health and Nutrition Examination Survey (NHANES III)
Valtin H (2002) “Drink at least eight glasses of water a day.” Really? Is there scientific evidence for “8 × 8”? Am J Physiol Regul Integr Comp Physiol 283:R993–R1004. doi:10.1152/ajpregu.00365.2002
Van Beaumont W, Greenleaf JE, Juhos L (1972) Disproportional changes in hematocrit, plasma volume, and proteins during exercise and bed rest. J Appl Physiol 33:55–61
Acknowledgments
The authors are grateful to Brittany Swokla, Amy McKenzie, Jenna Appicella, Daniel Friedenreich, Holly Emmanuel, Brittanie Volk, Cathy Saenz, Colin Shaughnessy, Theodore Pert III, Ethan Talbot, Corey Dwyer, and Katie Simpson for their technical assistance during data collection and analysis.
Conflict of interest
The current investigation was supported by a grant from DANONE Research. Lawrence Armstrong serves on the Scientific Advisory Board for, and Laurent Le Bellego and Alexis Klien are employees at, DANONE Research.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Massimo Pagani.
Rights and permissions
About this article
Cite this article
Johnson, E.C., Muñoz, C.X., Le Bellego, L. et al. Markers of the hydration process during fluid volume modification in women with habitual high or low daily fluid intakes. Eur J Appl Physiol 115, 1067–1074 (2015). https://doi.org/10.1007/s00421-014-3088-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-014-3088-2