Abstract
Purpose
Few studies have assessed the time-dependent response of fatigue (i.e., loss of force) during submaximal exercise without the use of maximum contractions. There is unexplored potential in the use of the superimposed muscle twitch (SIT), evoked by transcranial magnetic stimulation (TMS) or motor nerve stimulation (MNS), to assess fatigue during voluntary submaximal contractions. For the human triceps surae muscles, there are also no data on TMS-evoked twitches.
Methods
To optimise the TMS stimulus for assessment of fatigue, we first tested the effects of TMS power (40, 55, 70, 85, 100 % max) on SIT force during contractions (0–100 % MVC in 10 % increments) in six subjects. Then, we compared SIT responses (TMS and MNS) during submaximal contractions and MVCs (all at 60 s intervals) during a continuous protocol of intermittent contractions (30 % MVC) consisting of consecutive 5 min periods of baseline, fatigue (ischaemia) and recovery.
Results
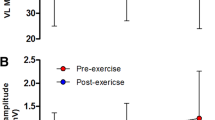
For TMS, SIT force increased as a diminishing function of TMS power (P < 0.05), the relationships between SIT force and the force of voluntary contraction at all TMS powers were parabolic, and SIT force was maximised at ~20–40 % MVC. During intermittent contractions, MVC and SIT forces were stable during baseline, decreased similarly during ischaemia by 40–50 % (P < 0.05), and recovered similarly to baseline values (P > 0.05) before the end of the protocol.
Conclusion
TMS can be used to evoke twitches during submaximal contractions of the human calf muscle and, along with MNS, used to assess fatigue during submaximal exercise.







Similar content being viewed by others
References
Amann M, Blain GM, Proctor LT, Sebranek JJ, Pegelow DF, Dempsey JA (2011) Implications of group III and IV muscle afferents for high-intensity endurance exercise performance in humans. J Physiol 589:5299–5309
Barclay JK (1986) A delivery-independent blood flow effect on skeletal muscle fatigue. J Appl Physiol 61:1084–1090
Belanger AY, McComas AJ (1981) Extent of motor unit activation during effort. J Appl Physiol 51:1131–1135
Bylund-Fellenius AC, Walker PM, Elander A, Holm S, Schersten T (1981) Energy metabolism in relation to oxygen partial pressure in human skeletal muscle during exercise. Biochem J 200:247–255
Donnelly J, Green S (2013) Effect of hypoxia on the dynamic response characteristics of hyperaemia in the contracting human calf muscle. Exp Physiol 98(1):81–93
Egana M, Green S (2005) Effect of body tilt on calf muscle performance and blood flow in humans. J Appl Physiol 98:2249–2258
Egana M, Green S (2007) Intensity-dependent effect of body tilt angle on calf muscle fatigue in humans. Eur J Appl Physiol 99:1–9
Egana M, Ryan K, Warmington S, Green S (2010) Effect of body tilt angle on fatigue and EMG activities in lower limbs during cycling. Eur J Appl Physiol 108:649–656
Enoka RM, Duchateau J (2008) Muscle fatigue: what, why and how it influences muscle function. J Physiol 586:11–23
Fitzpatrick R, Taylor JL, McCloskey DI (1996) Effects of arterial perfusion pressure on force production in working human hand muscles. J Physiol 495(3):885–891
Fulco CS, Lewis SF, Frykman PN, Boushel R, Smith S, Harman EA, Cymerman A, Pandolf KB (1996) Muscle fatigue and exhaustion during dynamic leg exercise in normoxia and hypobaric hypoxia. J Appl Physiol 81:1891–1900
Gandevia SC (2001) Spinal and supraspinal factors in human muscle fatigue. Physiol Rev 81:1725–1789
Green S, Mehlsen J (1999) Peripheral arterial disease. In: Saltin B, Boushel R, Secher N, Mitchell J (eds) Exercise and circulation in health and disease. Human Kinetics, Champaign, pp 283–290
Herbert RD, Gandevia SC (1999) Twitch interpolation in human muscles: mechanisms and implications for measurement of voluntary activation. J Neurophysiol 82:2271–2283
Hogan MC, Richardson RS, Kurdak SS (1994) Initial fall in skeletal muscle force development during ischemia is related to oxygen availability. J Appl Physiol 77:2380–2384
Keller ML, Pruse J, Yoon T, Schlinder-Delap B, Harkins A, Hunter SK (2011) Supraspinal fatigue is similar in men and women for a low-force fatiguing contraction. Med Sci Sports Exerc 43:1873–1883
Knorr S, Ivanova TD, Doherty TJ, Campbell JA, Garland SJ (2011) The origins of neuromuscular fatigue post-stroke. Exp Brain Res 214:303–315
Lamarra N (1990) Variables, constants, and parameters: clarifying the system structure. Med Sci Sports Exerc 22:88–95
Leyk D, Baum K, Wamser P, Wackerhage H, Essfeld D (1999) Cardiac output, leg blood flow and oxygen uptake during foot plantar flexions. Int J Sports Med 20:510–515
McCreary CR, Chilibeck PD, Marsh GD, Paterson DH, Cunningham DA, Thompson RT (1996) Kinetics of pulmonary oxygen uptake and muscle phosphates during moderate-intensity exercise. J Appl Physiol 81:1331–1338
Mileva KN, Sumners DP, Bowtell JL (2012) Decline in voluntary activation contributes to reduced maximal performance of fatigued lower limb muscles. Eur J Appl Physiol 112:3959–3970
Molenaar JP, McNeil CJ, Bredius MS, Gandevia SC (2012) Effects of aging and sex on voluntary activation and peak relaxation rate of human elbow flexors studied with motor cortical stimulation. Age. doi:10.1007/s11357-012-9435-5
Reeder E, Green S (2012) Dynamic response characteristics of muscle hyperaemia: effect of exercise intensity and relation to electromyographic activity. Eur J Appl Physiol 112:3997–4013
Sidhu SK, Bentley DJ, Carroll TJ (2009) Cortical voluntary activation of the human knee extensors can be reliably estimated using transcranial magnetic stimulation. Muscle Nerve 39:186–196
Todd G, Taylor JL, Gandevia SC (2003) Measurement of voluntary activation of fresh and fatigued human muscles using transcranial magnetic stimulation. J Physiol 551:661–671
Tucker KJ, Tuncer M, Turker KS (2005) A review of the H-reflex and M-wave in the human triceps surae. Hum Mov Sci 24:667–688
van Duinen H, Gandevia SC, Taylor JL (2010) Voluntary activation of the different compartments of the flexor digitorum profundus. J Neurophysiol 104:3213–3221
Acknowledgments
The authors thank Professors Simon Gandevia and Janet Taylor from Neuroscience Research Australia for their help and advice in the early phase of this project.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Alain Martin.
Rights and permissions
About this article
Cite this article
Green, S., Robinson, E. & Wallis, E. Assessment of calf muscle fatigue during submaximal exercise using transcranial magnetic stimulation versus transcutaneous motor nerve stimulation. Eur J Appl Physiol 114, 113–121 (2014). https://doi.org/10.1007/s00421-013-2757-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-013-2757-x