Abstract
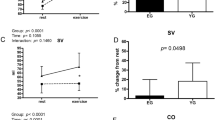
Overweight and obesity are associated with hemodynamic changes at rest. Whether these changes are mirrored during exercise is uncertain. We compared cardiac output (Q) and stroke volume (SV) in 12 overweight (OW) and 12 normal weight (NW) adults at rest and during exercise. Participants were assessed for body composition, peak oxygen consumption, and Q and SV at rest and during cycling exercise at 50, 75 and 100 W. Cardiac output was significantly higher at rest and during exercise in OW than NW when fat mass and ethnicity were used as covariates. When fat free mass was added as a covariate, Q was no longer different between groups. Stroke volume tended to be higher in OW than NW when fat mass and ethnicity were used as covariates (P = 0.055) with no differences in heart rate observed. Although the total change in Q and SV was similar between groups with each exercise intensity, overall Q was higher in the OW than NW participants. The higher Q is likely explained by a higher SV, secondary to a greater blood volume in the OW. The elevated hemodynamic response in OW may reflect the early cardiac adaptations of excess body mass.


Similar content being viewed by others
References
Alaud-din A, Meterissian S, Lisbona R, MacLean LD, Forse RA (1990) Assessment of cardiac function in patients who were morbidly obese. Surgery 108:809–818 (discussion 818–820)
Barbier J, Ville N, Kervio G, Walther G, Carre F (2006) Sports-specific features of athlete’s heart and their relation to echocardiographic parameters. Herz 31:531–543. doi:10.1007/s00059-006-2862-2
Bella JN, Devereux RB, Roman MJ, O’Grady MJ, Welty TK, Lee ET, Fabsitz RR, Howard BV (1998) Relations of left ventricular mass to fat-free and adipose body mass: the strong heart study. The strong heart study investigators. Circulation 98:2538–2544
Collier CR (1956) Determination of mixed venous CO2 tensions by rebreathing. J Appl Physiol 9:25–29
Collis T, Devereux RB, Roman MJ, de Simone G, Yeh J, Howard BV, Fabsitz RR, Welty TK (2001) Relations of stroke volume and cardiac output to body composition: the strong heart study. Circulation 103:820–825
Defares JG (1958) Determination of PVCO2 from the exponential CO2 rise during rebreathing. J Appl Physiol 13:159–164
de Simone G, Devereux RB, Kizer JR, Chinali M, Bella JN, Oberman A, Kitzman DW, Hopkins PN, Rao DC, Arnett DK (2005) Body composition and fat distribution influence systemic hemodynamics in the absence of obesity: the HyperGEN Study. Am J Clin Nutr 81:757–761
Du Bois D, Du Bois EF (1989) A formula to estimate the approximate surface area if height and weight be known. 1916. Nutrition 5:303–311 (discussion 312–303)
Espersen K, Jensen EW, Rosenborg D, Thomsen JK, Eliasen K, Olsen NV, Kanstrup IL (1995) Comparison of cardiac output measurement techniques: thermodilution, Doppler, CO2 rebreathing and the direct Fick method. Acta Anaesthesiol Scand 39:245–251
Ferraro S, Perrone-Filardi P, Desiderio A, Betocchi S, D’Alto M, Liguori L, Trimigliozzi P, Turco S, Chiariello M (1996) Left ventricular systolic and diastolic function in severe obesity: a radionuclide study. Cardiology 87:347–353
Forbes GB, Welle SL (1983) Lean body mass in obesity. Int J Obes 7:99–107
Giordano U, Ciampalini P, Turchetta A, Santilli A, Calzolari F, Crino A, Pompei E, Alpert BS, Calzolari A (2003) Cardiovascular hemodynamics: relationships with insulin resistance in obese children. Pediatr Cardiol 24:548–552. doi:10.1007/s00246-003-0368-8
Gledhill N, Cox D, Jamnik R (1994) Endurance athletes’ stroke volume does not plateau: major advantage is diastolic function. Med Sci Sports Exerc 26:1116–1121. doi:10.1249/00005768-199409000-00008
Granath A, Strandell T (1964) Relationships between cardiac output, stroke volume and intracardiac pressures at rest and during exercise in supine position and some anthropometric data in healthy old men. Acta Med Scand 176:447–466
Grundy SM, Cleeman JI, Daniels SR, Donato KA, Eckel RH, Franklin BA, Gordon DJ, Krauss RM, Savage PJ, Smith SC Jr, Spertus JA, Costa F (2005) Diagnosis and management of the metabolic syndrome. An American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Executive summary. Cardiol Rev 13:322–327
Haskall WL, Lee IM, Pate RR, Powell KE, Blair SN, Franklin BA, Macera CA, Heath GW, Thompson PD, Bauman A (2007) Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Med Sci Sports Exerc 39(8):1423–1434. doi:10.1249/mss.0b013e3180616b27
Hunt BE, Davy KP, Jones PP, DeSouza CA, Van Pelt RE, Tanaka H, Seals DR (1998) Role of central circulatory factors in the fat-free mass-maximal aerobic capacity relation across age. Am J Physiol 275:H1178–H1182
Jones NL (1997) Clinical exercise testing. Saunders, Philadelphia
Licata G, Scaglione R, Paterna S, Parrinello G, Indovina A, Dichiara MA, Alaimo G, Merlino G (1992) Left ventricular function response to exercise in normotensive obese subjects: influence of degree and duration of obesity. Int J Cardiol 37:223–230. doi:10.1016/0167-5273(92)90212-L
Lopaschuk GD, Folmes CDL, Stanley WC (2007) Cardiac energy metabolism in obesity. Circ Res 110:335–347. doi:10.1161/CIRCRESAHA.107.150417
Melanson KJ, McInnis KJ, Rippe JM, Blackburn G, Wilson PF (2001) Obesity and cardiovascular disease risk: research update. Cardiol Rev 9:202–207. doi:10.1097/00045415-200107000-00005
Messerli FH, Ventura HO, Reisin E, Dreslinski GR, Dunn FG, MacPhee AA, Frohlich ED (1982) Borderline hypertension and obesity: two prehypertensive states with elevated cardiac output. Circulation 66:55–60
Morricone L, Malavazos AE, Coman C, Donati C, Hassan T, Caviezel F (2002) Echocardiographic abnormalities in normotensive obese patients: relationship with visceral fat. Obes Res 10:489–498. doi:10.1038/oby.2002.67
Muscelli E, Camastra S, Catalano C, Galvan AQ, Ciociaro D, Baldi S, Ferrannini E (1997) Metabolic and cardiovascular assessment in moderate obesity: effect of weight loss. J Clin Endocrinol Metab 82:2937–2943. doi:10.1210/jc.82.9.2937
National Heart Lung Blood Institute (1997) The sixth report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure. Report number 98-4080, National Institutes of Health
O’Connor F, Fleg JL, Gerstenblith G, Becker LC, Goldberg AP, Hagberg JM, Lakatta L, Lakatta EG, Schulman SP (1994) Effect of body fat on exercise hemodynamics in sedentary older men. Aging (Milano) 6:257–265
Pascual M, Pascual DA, Soria F, Vicente T, Hernandez AM, Tebar FJ, Valdes M (2003) Effects of isolated obesity on systolic and diastolic left ventricular function. Heart 89:1152–1156. doi:10.1136/heart.89.10.1152
Peterson LR, Waggoner AD, Schechtman KB, Meyer T, Gropler RJ, Barzilai B, Davila-Roman VG (2004) Alterations in left ventricular structure and function in young healthy obese women: assessment by echocardiography and tissue Doppler imaging. J Am Coll Cardiol 43:1399–1404. doi:10.1016/j.jacc.2003.10.062
Poirier P, Giles TD, Bray GA, Hong Y, Stern JS, Pi-Sunyer FX, Eckel RH (2006) Obesity and cardiovascular disease: pathophysiology, evaluation, and effect of weight loss. Arterioscler Thromb Vasc Biol 26:968–976. doi:10.1161/01.ATV.0000216787.85457.f3
Powell BD, Redfield MM, Bybee KA, Freeman WK, Rihal CS (2006) Association of obesity with left ventricular remodeling and diastolic dysfunction in patients without coronary artery disease. Am J Cardiol 98:116–120. doi:10.1016/j.amjcard.2006.01.063
Rowland TW (2007) Effect of obesity on cardiac function in children and adolescents: a review. J Sports Sci Med 6:319–326
Rowland T, Bhargava R, Parslow D, Heptulla RA (2003) Cardiac response to progressive cycle exercise in moderately obese adolescent females. J Adolesc Health 32:422–427. doi:10.1016/S1054-139X(03)00051-X
Salvadori A, Fanari P, Fontana M, Buontempi L, Saezza A, Baudo S, Miserocchi G, Longhini E (1999) Oxygen uptake and cardiac performance in obese and normal subjects during exercise. Respiration 66:25–33. doi:10.1159/000029333
Sasso FC, Carbonara O, Nasti R, Marfella R, Esposito K, Rambaldi P, Mansi L, Salvatore T, Torella R, Cozzolino D (2005) Effects of insulin on left ventricular function during dynamic exercise in overweight and obese subjects. Eur Heart J 26:1205–1212. doi:10.1093/eurheartj/ehi271
Savage DD, Levy D, Dannenberg AL, Garrison RJ, Castelli WP (1990) Association of echocardiographic left ventricular mass with body size, blood pressure and physical activity (the Framingham Study). Am J Cardiol 65:371–376. doi:10.1016/0002-9149(90)90304-J
Stickland MK, Welsh RC, Petersen SR, Tyberg JV, Anderson WD, Jones RL, Taylor DA, Bouffard M, Haykowsky MJ (2006) Does fitness level modulate the cardiovascular hemodynamic response to exercise? J Appl Physiol 100:1895–1901. doi:10.1152/japplphysiol.01485.2005
Strandell T (1964) Circulatory studies on healthy old men with special reference to the limitation of the maximal physical working capacity. Acta Med Scand 414(suppl 414):411–444
Unnithan VB, Baynard T, Potter CR, Barker P, Heffernan KS, Kelly E, Yates G, Fernhall B (2007) An exploratory study of cardiac function and oxygen uptake during cycle ergometry in overweight children. Obesity (Silver Spring) 15:2673–2682. doi:10.1038/oby.2007.319
Acknowledgments
The authors would like to thank all the participants who took part in this study, Julia Bader, Ph.D. for her statistical assistance, Veni Kong, Ph.D. for external review of the paper, and the University of Texas Research Institute for funding a part of the study. The address of the following author differs from that in the affiliation line: Stephen Burns, Ph.D., Division of Weight Management and Wellness, Children’s Hospital Pittsburgh, Pittsburgh, PA15213, USA.
Author information
Authors and Affiliations
Corresponding author
Additional information
University of Texas Research Institute funded part of this study.
Rights and permissions
About this article
Cite this article
Vella, C.A., Zubia, R.Y., Burns, S.F. et al. Cardiac response to exercise in young, normal weight and overweight men and women. Eur J Appl Physiol 105, 411–419 (2009). https://doi.org/10.1007/s00421-008-0918-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-008-0918-0