Abstract
Background
Volatile organic compounds (VOCs) are a broad class of chemicals, and previous studies showed that VOCs could increase the risk of central nervous system disorders. However, few studies have comprehensively explored their association with depression among general adults.
Objective
We aimed to explore the association between blood VOCs and depression risk based on a large cross-sectional study of the National Health and Nutrition Examination Survey (NHANES).
Methods
We analyzed data from 3449 American adults in the NHANES 2013–2016. Survey-weighted logistic regression model was used to explore the association of ten blood VOCs with depression. Subsequently, the relative importance of the selected VOCs was determined using the XGBoost model. The weighted quantile sum (WQS) regression model was used to explore the overall association of 10 blood VOCs with depression. Subgroup analyses were performed to identify high-risk populations. Finally, restricted cubic spline (RCS) analysis was utilized to explore the dose–response relationship between blood VOCs and the risk of depression.
Results
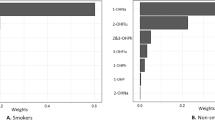
XGBoost Algorithm model identified blood 2,5-dimethylfuran was the most critical variable in depression. The logistic regression model showed that blood benzene, blood 2,5-dimethylfuran, and blood furan showed a positive correlation with depression. In subgroup analysis, we found that the effects of the above VOCs on depression existed among the female, young middle-aged, and overweight-obese population. Mixture VOCs exposure was positively associated with depression risk (OR = 2.089, 95% CI: 1.299–3.361), and 2,5-dimethylfuran had the largest weights in WQS regression. RCS displayed that blood benzene, blood 2,5-dimethylfuran, and blood furan were positively associated with depression.
Conclusion
The results of this study indicated that VOCs exposure was associated with an increased prevalence of depression in U.S. adults. Women, young and middle-aged, and overweight-obese populations are more vulnerable to VOCs.





Similar content being viewed by others
Data availability
Data will be made available on request.
References
Amiry GY, Haidary M, Azhdari-Zarmehri H, Beheshti F, Ahmadi-Soleimani SM (2023) Omega-3 fatty acids prevent nicotine withdrawal-induced exacerbation of anxiety and depression by affecting oxidative stress balance, inflammatory response, BDNF and serotonin metabolism in rats. Eur J Pharmacol 947:175634. https://doi.org/10.1016/j.ejphar.2023.175634
Association AP (2013) Diagnostic and statistical manual of mental disorders: DSM-5™, 5th edn. American Psychiatric Publishing Inc, Arlington, VA, USA
Beckley JT, Randall PK, Smith RJ, Hughes BA, Kalivas PW, Woodward JJ (2016) Phenotype-dependent inhibition of glutamatergic transmission on nucleus accumbens medium spiny neurons by the abused inhalant toluene. Addict Biol 21:530–546. https://doi.org/10.1111/adb.12235
Black CN, Bot M, Scheffer PG, Cuijpers P, Penninx BW (2015) Is depression associated with increased oxidative stress? A systematic review and meta-analysis. Psychoneuroendocrinology 51:164–175. https://doi.org/10.1016/j.psyneuen.2014.09.025
Castellanos M, Suñer R, Fernández-Real JM, Sanchez JM (2019) 2,5-Dimethylfuran as a validated biomarker of smoking status. Nicotine Tob Res 21:828–834. https://doi.org/10.1093/ntr/nty078
Chambers DM, Ocariz JM, McGuirk MF, Blount BC (2011) Impact of cigarette smoking on volatile organic compound (VOC) blood levels in the U.S. population: NHANES 2003–2004. Environ Int 37:1321–1328. https://doi.org/10.1016/j.envint.2011.05.016
Chen F, Zhou L, Bai Y, Zhou R, Chen L (2015) Hypothalamic-pituitary-adrenal axis hyperactivity accounts for anxiety- and depression-like behaviors in rats perinatally exposed to bisphenol A. J Biomed Res 29:250–258. https://doi.org/10.7555/jbr.29.20140058
Churchill JE, Ashley DL, Kaye WE (2001) Recent chemical exposures and blood volatile organic compound levels in a large population-based sample. Arch Environ Health 56:157–166. https://doi.org/10.1080/00039890109604068
Collaborators GDaI (2020) Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 396:1204–1222. https://doi.org/10.1016/s0140-6736(20)30925-9
Cruz SL, Balster RL, Woodward JJ (2000) Effects of volatile solvents on recombinant N-methyl-D-aspartate receptors expressed in Xenopus oocytes. Br J Pharmacol 131:1303–1308. https://doi.org/10.1038/sj.bjp.0703666
Farrow A, Taylor H, Northstone K, Golding J (2003) Symptoms of mothers and infants related to total volatile organic compounds in household products. Arch Environ Health 58:633–641. https://doi.org/10.3200/aeoh.58.10.633-641
Gotohda T, Tokunaga I, Kubo S (2005) Toluene inhalation-induced adrenocortical hypertrophy and endocrinological changes in rat. Life Sci 76:1929–1937. https://doi.org/10.1016/j.lfs.2004.08.035
Hanna GB, Boshier PR, Markar SR, Romano A (2019) Accuracy and methodologic challenges of volatile organic compound-based exhaled breath tests for cancer diagnosis: a systematic review and meta-analysis. JAMA Oncol 5:e182815. https://doi.org/10.1001/jamaoncol.2018.2815
Hester SD, Johnstone AF, Boyes WK, Bushnell PJ, Shafer TJ (2011) Acute toluene exposure alters expression of genes in the central nervous system associated with synaptic structure and function. Neurotoxicol Teratol 33:521–529. https://doi.org/10.1016/j.ntt.2011.07.008
Hong JY, Yu SY, Kim GW, Ahn JJ, Kim Y, Lim S, Son SW, Hwang SY (2016) Identification of time-dependent biomarkers and effects of exposure to volatile organic compounds using high-throughput analysis. Environ Toxicol 31:1563–1570. https://doi.org/10.1002/tox.22160
Inamdar AA, Masurekar P, Bennett JW (2010) Neurotoxicity of fungal volatile organic compounds in Drosophila melanogaster. Toxicol Sci 117:418–426. https://doi.org/10.1093/toxsci/kfq222
Jacobson MH, Ghassabian A, Gore AC, Trasande L (2022) Exposure to environmental chemicals and perinatal psychopathology. Biochem Pharmacol 195:114835. https://doi.org/10.1016/j.bcp.2021.114835
Jayaraj RL, Rodriguez EA, Wang Y, Block ML (2017) Outdoor ambient air pollution and neurodegenerative diseases: the neuroinflammation hypothesis. Curr Environ Health Rep 4:166–179. https://doi.org/10.1007/s40572-017-0142-3
Kanada M, Miyagawa M, Sato M, Hasegawa H, Honma T (1994) Neurochemical profile of effects of 28 neurotoxic chemicals on the central nervous system in rats (1). Effects of oral administration on brain contents of biogenic amines and metabolites. Ind Health 32:145–164. https://doi.org/10.2486/indhealth.32.145
Kilburn KH, Warshaw RH (1993) Neurobehavioral testing of subjects exposed residentially to groundwater contaminated from an aluminum die-casting plant and local referents. J Toxicol Environ Health 39:483–496. https://doi.org/10.1080/15287399309531766
Kim JK, Jung KH, Noh JH, Eun JW, Bae HJ, Xie HJ, Jang JJ, Ryu JC, Park WS, Lee JY, Nam SW (2011) Identification of characteristic molecular signature for volatile organic compounds in peripheral blood of rat. Toxicol Appl Pharmacol 250:162–169. https://doi.org/10.1016/j.taap.2010.10.009
Kim J, Lim J, Moon SH, Liu KH, Choi HJ (2020) Toluene inhalation causes early anxiety and delayed depression with regulation of dopamine turnover, 5-HT(1A) receptor, and adult neurogenesis in mice. Biomol Ther (seoul) 28:282–291. https://doi.org/10.4062/biomolther.2020.055
Kodavanti PR, Royland JE, Richards JE, Besas J, Macphail RC (2011) Toluene effects on oxidative stress in brain regions of young-adult, middle-age, and senescent Brown Norway rats. Toxicol Appl Pharmacol 256:386–398. https://doi.org/10.1016/j.taap.2011.04.012
Kodavanti PR, Royland JE, Moore-Smith DA, Besas J, Richards JE, Beasley TE, Evansky P, Bushnell PJ (2015) Acute and subchronic toxicity of inhaled toluene in male long-Evans rats: oxidative stress markers in brain. Neurotoxicology 51:10–19. https://doi.org/10.1016/j.neuro.2015.09.001
Kroenke K, Spitzer RL, Williams JB (2001) The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 16:606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Lei T, Qian H, Yang J, Hu Y (2023) The association analysis between exposure to volatile organic chemicals and obesity in the general USA population: a cross-sectional study from NHANES program. Chemosphere 315:137738. https://doi.org/10.1016/j.chemosphere.2023.137738
Malhi GS, Mann JJ (2018) Depression. Lancet 392:2299–2312. https://doi.org/10.1016/s0140-6736(18)31948-2
Manea L, Gilbody S, McMillan D (2015) A diagnostic meta-analysis of the patient health questionnaire-9 (PHQ-9) algorithm scoring method as a screen for depression. Gen Hosp Psychiatry 37:67–75. https://doi.org/10.1016/j.genhosppsych.2014.09.009
Miller AH, Raison CL (2016) The role of inflammation in depression: from evolutionary imperative to modern treatment target. Nat Rev Immunol 16:22–34. https://doi.org/10.1038/nri.2015.5
Myhre O, Sterri SH, Bogen IL, Fonnum F (2004) Erk1/2 phosphorylation and reactive oxygen species formation via nitric oxide and Akt-1/Raf-1 crosstalk in cultured rat cerebellar granule cells exposed to the organic solvent 1,2,4-trimethylcyclohexane. Toxicol Sci 80:296–303. https://doi.org/10.1093/toxsci/kfh166
Owumi SE, Adedara IA, Otunla MT, Owoeye O (2023) Influence of furan and lead co-exposure at environmentally relevant concentrations on neurobehavioral performance, redox-regulatory system and apoptotic responses in rats. Environ Toxicol Pharmacol 97:104011. https://doi.org/10.1016/j.etap.2022.104011
Pandit GG, Srivastava PK, Rao AM (2001) Monitoring of indoor volatile organic compounds and polycyclic aromatic hydrocarbons arising from kerosene cooking fuel. Sci Total Environ 279:159–165. https://doi.org/10.1016/s0048-9697(01)00763-x
Park D, Hwang C (2015) Toluene-induced encephalopathy: a case report. Brain Neurorehabil 8:109. https://doi.org/10.12786/bn.2015.8.2.109
Tan J, Chen N, Bai J, Yan P, Ma X, Ren M, Maitland E, Nicholas S, Cheng W, Leng X, Chen C, Wang J (2023) Ambient air pollution and the health-related quality of life of older adults: evidence from Shandong China. J Environ Manage 336:117619. https://doi.org/10.1016/j.jenvman.2023.117619
Touloumis C (2021) The burden and the challenge of treatment-resistant depression. Psychiatriki 32:11–14. https://doi.org/10.22365/jpsych.2021.046
Trombley J (2023) Fine particulate matter exposure and pediatric mental health outcomes: an integrative review. J Nurs Scholarsh. https://doi.org/10.1111/jnu.12888
Vona R, Gambardella L, Cittadini C, Straface E, Pietraforte D (2019) Biomarkers of oxidative stress in metabolic syndrome and associated diseases. Oxid Med Cell Longev 2019:8267234. https://doi.org/10.1155/2019/8267234
Wang R, Ye C, Huang X, Halimulati M, Sun M, Ma Y, Fan R, Zhang Z (2023a) cMIND diet, indoor air pollution, and depression: a cohort study based on the CLHLS from 2011 to 2018. Nutrients 15:1203. https://doi.org/10.3390/nu15051203
Wang Y, Han X, Li J, Zhang L, Liu Y, Jin R, Chen L, Chu X (2023b) Associations between the compositional patterns of blood volatile organic compounds and chronic respiratory diseases and ages at onset in NHANES 2003–2012. Chemosphere 327:138425. https://doi.org/10.1016/j.chemosphere.2023.138425
Win-Shwe TT, Fujimaki H (2010) Neurotoxicity of toluene. Toxicol Lett 198:93–99. https://doi.org/10.1016/j.toxlet.2010.06.022
Wootton RE, Richmond RC, Stuijfzand BG, Lawn RB, Sallis HM, Taylor GMJ, Hemani G, Jones HJ, Zammit S, Davey Smith G, Munafò MR (2020) Evidence for causal effects of lifetime smoking on risk for depression and schizophrenia: a Mendelian randomisation study. Psychol Med 50:2435–2443. https://doi.org/10.1017/s0033291719002678
World Health Organization (2023) Depression. Health topics-depression. https://www.who.int/health-topics/depression#tab=tab_1. Accessed 10 Apr 2023
Wu Z, Yue Q, Zhao Z, Wen J, Tang L, Zhong Z, Yang J, Yuan Y, Zhang X (2023) A cross-sectional study of smoking and depression among US adults: NHANES (2005–2018). Front Public Health 11:1081706. https://doi.org/10.3389/fpubh.2023.1081706
Xiong X, Chen B, Wang Z, Ma L, Li S, Gao Y (2022) Association between perfluoroalkyl substances concentration and bone mineral density in the US adolescents aged 12–19 years in NHANES 2005–2010. Front Endocrinol (lausanne) 13:980608. https://doi.org/10.3389/fendo.2022.980608
Yu SY, Koh EJ, Kim SH, Lee SY, Lee JS, Son SW, Hwang SY (2021) Integrated analysis of multi-omics data on epigenetic changes caused by combined exposure to environmental hazards. Environ Toxicol 36:1001–1010. https://doi.org/10.1002/tox.23099
Acknowledgements
Not applicable.
Funding
This research received no external funding.
Author information
Authors and Affiliations
Contributions
YZ and RW conceived the idea. YZ wrote the manuscript. RW and YZ collected, read the literature, and revised the article. YHJ collated the data needed for this article. YYY and MLW read through and corrected the manuscript. All authors approved the final version of the manuscript, and read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethics approval
The studies involving human participants were reviewed and approved by The National Center for Health Statistics (NCHS) Research Ethics Review Board.
Consent to participate
The patients/participants provided their written informed consent to participate in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, Y., Ju, Y., Wang, M. et al. Association of volatile organic compounds exposure with the risk of depression in U.S. adults: a cross‑sectional study from NHANES 2013–2016. Int Arch Occup Environ Health 96, 1101–1111 (2023). https://doi.org/10.1007/s00420-023-01993-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00420-023-01993-6