Abstract
Purpose
To compare visual outcomes, incidence of cystoid macular edema (CME), and rate of repeat epiretinal membrane (ERM) surgery following phacovitrectomy for primary and secondary ERM.
Methods
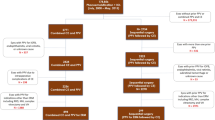
Retrospective review of 178,856 cataract surgeries from 2003 to 2015. Eyes that underwent cataract surgery combined with ERM peel were included (n = 708). Eyes were divided into primary (n = 538) and secondary (n = 170) ERM groups. Patient demographics, visual acuity (VA), and postoperative CME were recorded.
Results
Patients with secondary ERM had worse preoperative VA, 0.9 ± 0.6 logMAR (20/160 Snellen equivalent) as compared to patients with primary ERM, 0.6 ± 0.3 (20/80), respectively (p < 0.0001). There was no difference between the secondary and primary ERM groups in postoperative vision (0.5 ± 0.4 logMAR vs. 0.5 ± 0.3; p = 0.9962) or proportion with VA ≥ 20/40 (46.4% vs. 43.1%; p = 0.6744) at 12–24 weeks. Postoperative CME was twice as likely in the secondary ERM group (16.5%) compared to the primary ERM group (7.8%) (p = 0.0018). There was no difference in the rate of repeat ERM surgery between the secondary ERM group (1.8%) and the primary ERM group (1.5%) (p = 0.7308).
Conclusion
Eyes with secondary ERM had significant postoperative improvement in VA. They had worse preoperative VA and had a twofold increase in postoperative CME than primary ERM.


Similar content being viewed by others
References
Stevenson W, Prospero Ponce CM, Agarwal DR et al (2016) Epiretinal membrane: optical coherence tomography-based diagnosis and classification. Clin Ophthalmol 10:527–534. https://doi.org/10.2147/OPTH.S97722
Xiao W, Chen X, Yan W et al (2017) Prevalence and risk factors of epiretinal membranes: a systematic review and meta-analysis of population-based studies. BMJ Open 7:e014644. https://doi.org/10.1136/bmjopen-2016-014644
Ng CH, Cheung N, Wang JJ et al (2011) Prevalence and risk factors for epiretinal membranes in a multi-ethnic United States population. Ophthalmology 118:694–699. https://doi.org/10.1016/j.ophtha.2010.08.009
Miyazaki M, Nakamura H, Kubo M et al (2003) Prevalence and risk factors for epiretinal membranes in a Japanese population: the Hisayama study. Graefes Arch Clin Exp Ophthalmol 241:642–646. https://doi.org/10.1007/s00417-003-0723-8
Aung KZ, Makeyeva G, Adams MK et al (2013) The prevalence and risk factors of epiretinal membranes: the Melbourne Collaborative Cohort Study. Retina 33:1026–1034. https://doi.org/10.1097/IAE.0b013e3182733f25
Ueki M, Morishita S, Kohmoto R et al (2016) Comparison of histopathological findings between idiopathic and secondary epiretinal membranes. Int Ophthalmol 36:713–718. https://doi.org/10.1007/s10792-016-0194-7
Yazici A, Alagöz N, Celik H et al (2011) Idiopathic and secondary epiretinal membranes: do they differ in terms of morphology? An optical coherence tomography-based study. Retina 31:779–784. https://doi.org/10.1097/IAE.0b013e3181ef8786
Kang KT, Kim KS, Kim YC (2014) Surgical results of idiopathic and secondary epiretinal membrane. Int Ophthalmol 34:1227–1232. https://doi.org/10.1007/s10792-014-0010-1
Dugas B, Ouled-Moussa R, Lafontaine PO et al (2010) Idiopathic epiretinal macular membrane and cataract extraction: combined versus consecutive surgery. Am J Ophthalmol 149:302–306. https://doi.org/10.1016/j.ajo.2009.09.011
Yiu G, Marra KV, Wagley S et al (2013) Surgical outcomes after epiretinal membrane peeling combined with cataract surgery. Br J Ophthalmol 97:1197–1201. https://doi.org/10.1136/bjophthalmol-2013-303189
Lee PY, Cheng KC, Wu WC (2011) Anatomic and functional outcome after surgical removal of idiopathic macular epiretinal membrane. Kaohsiung J Med Sci 27:268–275. https://doi.org/10.1016/j.kjms.2011.02.001
Oshima Y, Ohju M, Tano Y (2006) Surgical outcomes of 25-gauge transconjunctival vitrectomy combined with cataract surgery for vitreoretinal diseases. Annals Academy of Medicine Singapore 35:175–180
Okamoto F, Okamoto Y, Hiraoka T et al (2009) Effect of vitrectomy for epiretinal membrane on visual function and vision-related quality of life. Am J Ophthalmol 147:869-874-874 e861. https://doi.org/10.1016/j.ajo.2008.11.018
Song S, Kuriyan A, Smiddy W (2015) Results and prognostic factors for visual improvement after pars plana vitrectomy for idiopathic epiretinal membrane. Retina 35:866–872
Jackson TLDP, Williamson TH, Sparrow JM et al (2015) The Royal College of Ophthalmologist’s National Ophthalmology Database Study of Vitreoretinal Surgery: Report 4, Epiretinal Membrane. Retina 35:1615–1621. https://doi.org/10.1097/IAE.0000000000000523
Council MD, Shah GK, Lee HC et al (2005) Visual outcomes and complications of epiretinal membrane removal secondary to rhegmatogenous retinal detachment. Ophthalmology 112:1218–1221. https://doi.org/10.1016/j.ophtha.2005.01.051
Dev S, Mieler WF, Pulido JS et al (1999) Visual outcomes after pars plana vitrectomy for epiretinal membranes associated with pars planitis. Ophthalmology 106:1086–1090. https://doi.org/10.1016/s0161-6420(99)90247-6
Kang HM, Koh HJ, Lee SC (2015) Visual outcome and prognostic factors after surgery for a secondary epiretinal membrane associated with branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol 253:543–550. https://doi.org/10.1007/s00417-014-2731-2
Sakimoto S, Saito Y, Nakata K et al (2008) Surgical outcomes of epiretinal membrane removal after successful pars plana vitrectomy for retinal diseases. Jpn J Ophthalmol 52:227–230. https://doi.org/10.1007/s10384-008-0539-5
Tanawade R, Tsierkezou L, Bindra M et al (2015) Visual outcomes of pars plana vitrectomy with epiretinal membrane peel in patients with uveitis. Retina 35:736–741
Rice TA, De Bustros S, Michels RG et al (1986) Prognostic factors in vitrectomy for epiretinal membranes of the macula. Ophthalmology 93:602–610. https://doi.org/10.1016/s0161-6420(86)33689-3
Branson SV, McClafferty BR, Kurup SK (2017) Vitrectomy for epiretinal membranes and macular holes in uveitis patients. J Ocul Pharmacol Ther 33:298–303. https://doi.org/10.1089/jop.2016.0142
Chu CJ, Johnston RL, Buscombe C et al (2016) Risk factors and incidence of macular edema after cataract surgery: a database study of 81984 eyes. Ophthalmology 123:316–323. https://doi.org/10.1016/j.ophtha.2015.10.001
Hardin JS, Gauldin DW, Soliman MK et al (2018) Cataract surgery outcomes in eyes with primary epiretinal membrane. JAMA Ophthalmol 136:148–154. https://doi.org/10.1001/jamaophthalmol.2017.5849
Henderson BA, Kim JY, Ament CS et al (2007) Clinical pseudophakic cystoid macular edema. Risk factors for development and duration after treatment. J Cataract Refract Surg 33:1550–1558. https://doi.org/10.1016/j.jcrs.2007.05.013
Schaub F, Adler W, Enders P et al (2018) Preexisting epiretinal membrane is associated with pseudophakic cystoid macular edema. Graefes Arch Clin Exp Ophthalmol 256:909–917. https://doi.org/10.1007/s00417-018-3954-4
Soliman MK, Hardin JS, Jawed F et al (2018) A database study of visual outcomes and intraoperative complications of postvitrectomy cataract surgery. Ophthalmology 125:1683–1691. https://doi.org/10.1016/j.ophtha.2018.05.027
Demetriades A-M, Gottsch JD, Thomsen R et al (2003) Combined phacoemulsification, intraocular lens implantation, and vitrectomy for eyes with coexisting cataract and vitreoretinal pathology. Am J Ophthalmol 135:291–296. https://doi.org/10.1016/s0002-9394(02)01972-4
Wensheng L, Wu R, Wang X et al (2009) Clinical complications of combined phacoemulsification and vitrectomy for eyes with coexisting cataract and vitreoretinal diseases. Eur J Ophthalmol 19:37–45. https://doi.org/10.1177/112067210901900106
Grewing R, Mester U (1996) Results of surgery for epiretinal membranes and their recurrences. Br J Ophthalmol 80:323–326. https://doi.org/10.1136/bjo.80.4.323
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent
For this type of study, formal consent is not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Norton, J.C., Soliman, M.K., Yang, Y.C. et al. Visual outcomes of primary versus secondary epiretinal membrane following vitrectomy and cataract surgery. Graefes Arch Clin Exp Ophthalmol 260, 817–825 (2022). https://doi.org/10.1007/s00417-021-05425-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-021-05425-4