Abstract
Purpose
In cases of corneal opacity with vascularization and peripheral thinning, traditional keratoplasty techniques have several risks and drawbacks. We report the results of a two-step surgical strategy consisting in performing a large diameter tectonic lamellar keratoplasty (TLK) to restore appropriate corneal thickness and an avascular recipient bed, followed by central optical PK within the lamellar graft at a later date.
Methods
This single-institution study analyzes the results of 7 eyes of 7 patients who received PK after large diameter TLK. All patients were affected by deep post-infectious corneal opacity with persistent stromal vascularization and peripheral thinning. The main outcomes measured were graft survival, visual acuity, refraction, and endothelial cell density.
Results
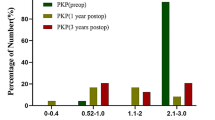
TLK was performed in all cases with 10/10.1-mm diameters. After a mean interval of 14 months, central PK was performed with a median host-graft diameter of 7.75/8.25 mm. Mean follow-up after PK was 52 months. At last follow-up, 6/7 (86%) grafts were clear. Endothelial rejection occurred in 5/7 (71%) eyes, with one patient having multiple episodes and subsequent graft failure. At 2 years, all patients had a visual acuity ≥ 20/40, with an average refractive astigmatism of 3.75 diopters.
Conclusion
Optical PK within a previous TLK is a safe and efficient technique for treating deep corneal opacity associated with extensive vascularization and peripheral thinning. Extended follow-up period is necessary to assess endothelial cell loss and long-term efficacy of the procedure.




Similar content being viewed by others
Data availability
The study and data accumulation were in conformity with all country, federal, and state laws.
Code availability
n/a.
References
Lohchab M, Prakash G, Arora T et al (2019) Surgical management of peripheral corneal thinning disorders. Surv Ophthalmol 64:67–78. https://doi.org/10.1016/j.survophthal.2018.06.002
Cristol SM, Alfonso EC, Guildford JH et al (1996) Results of large penetrating keratoplasty in microbial keratitis. Cornea 15:571–576
Chen WL, Wu CY, Hu FR et al (2004) Therapeutic penetrating keratoplasty for microbial keratitis in Taiwan from 1987 to 2001. Am J Ophthalmol 137:736–743. https://doi.org/10.1016/j.ajo.2003.11.010
Cowden J, Copeland R, Schneider M (1989) Large diameter therapeutic penetrating keratoplasties. J Refract Corneal Surg 5:244–248
Skeens HM, Holland EJ (2010) Large-diameter penetrating keratoplasty: indications and outcomes. Cornea 29:296–301. https://doi.org/10.1097/ICO.0b013e3181b6489e
Speaker MG, Arentsen JJ, Laibson PR (1989) Long-term survival of large diameter penetrating keratoplasties for keratoconus and pellucid marginal degeneration. Acta Ophthalmol Suppl 192:17–19. https://doi.org/10.1111/j.1755-3768.1989.tb07089.x
Wong DW, Chan WK, Tan DT (1997) Harvesting a lamellar graft from a corneoscleral button: a new technique. Am J Ophthalmol 123:688–689. https://doi.org/10.1016/s0002-9394(14)71082-7
Epstein RJ, Seedor JA, Dreizen NG et al (1987) Penetrating keratoplasty for herpes simplex keratitis and keratoconus: allograft rejection and survival. Ophthalmology 94:935–944. https://doi.org/10.1016/s0161-6420(87)33356-1
Ficker LA, Kirkness CM, Rice NSC et al (1988) Long-term prognosis for corneal grafting in herpes simplex keratitis. Eye 2(400–408):10. https://doi.org/10.1038/eye.1988.73
Thompson RW Jr, Price MO, Bowers PJ et al (2003) Long-term graft survival after penetrating keratoplasty. Ophthalmology 110:1396–1402. https://doi.org/10.1016/S0161-6420(03)00463-9
Williams KA, Roder D, Esterman A et al (1992) Factors predictive of corneal graft survival. Report from the Australian corneal graft registry. Ophthalmology 99:403–414. https://doi.org/10.1016/s0161-6420(92)31960-8
Williams KA, Lowe M, Bartlett C et al (2008) Risk factors for human corneal graft failure within the Australian corneal graft registry. Transplantation 86:1720–1724. https://doi.org/10.1097/TP.0b013e3181903b0a
Vail A, Gore SM, Bradley BA et al (1997) Conclusions of the corneal transplant follow up study. Br J Ophthalmol 81:631–636. https://doi.org/10.1136/bjo.81.8.631
Ing JJ, Ing HH, Neson LR et al (1998) Ten-year postoperative results of penetrating keratoplasty. Ophthalmology 105:1855–1865. https://doi.org/10.1016/S0161-6420(98)91030-2
Price FW, Whitson WE, Marks RG (1991) Graft survival in four common groups of patients undergoing penetrating keratoplasty. Ophthalmology 98:322–328. https://doi.org/10.1016/s0161-6420(91)32292-9
Sugita J, Kondo J (1997) Deep lamellar keratoplasty with complete removal of pathologic stroma for vision improvement. Br J Ophthalmol 81:184–188. https://doi.org/10.1136/bjo.81.3.184
Anwar M (2002) Teichmann KD (2002) Deep lamellar keratoplasty: surgical techniques for anterior lamellar keratoplasty with and without baring of Descemet’s membrane. Cornea 21:374–383. https://doi.org/10.1097/00003226-200205000-00009
Tsubota K, Kaido M, Monden Y et al (1998) A new surgical technique for deep lamellar keratoplasty with single running suture adjustment. Am J Ophthalmol 126:1–8. https://doi.org/10.1016/s0002-9394(98)00067-1
Archila EA (1984) Deep lamellar keratoplasty dissection of host tissue with intrastromal air injection. Cornea 3:217–218
Manche EE, Holland GN, Maloney RK (1999) Deep lamellar keratoplasty using viscoelastic dissection. Arch Ophthalmol 117:1561–1565. https://doi.org/10.1001/archopht.117.11.1561
Anshu A, Parthasarathy A, Mehta JS et al (2009) Outcomes of therapeutic deep lamellar keratoplasty and penetrating keratoplasty for advanced infectious keratitis: a comparative study. Ophthalmology 116:615–623. https://doi.org/10.1016/j.ophtha.2008.12.043
Rama P, Knutsson KA, Razzoli G et al (2013) Deep anterior lamellar keratoplasty using an original manual technique. Br J Ophthalmol 97:23–27. https://doi.org/10.1136/bjophthalmol-2011-301168
Ardjomand N, Hau S, McAlister JC et al (2007) Quality of vision and graft thickness in deep anterior lamellar and penetrating corneal allografts. Am J Ophthalmol 143:228–235. https://doi.org/10.1016/j.ajo.2006.10.043
Busin M, Arffa RC (2005) Microkeratome-assisted mushroom keratoplasty with minimal endothelial replacement. Am J Ophthalmol 140:138–140. https://doi.org/10.1016/j.ajo.2004.12.024
Scorcia V, Busin M (2012) Survival of mushroom keratoplasty performed in corneas with postinfectious vascularized scars. Am J Ophthalmol 153:44–50. https://doi.org/10.1016/j.ajo.2011.05.020
Langenbucher A, Seitz B, Nguyen NX et al (2002) Corneal endothelial cell loss after nonmechanical penetrating keratoplasty depends on diagnosis: a regression analysis. Graefes Arch Clin Exp Ophthalmol 240:387–392. https://doi.org/10.1007/s00417-002-0470-2
Lavy I, Verdijk RM, Bruinsma M et al (2017) Sex chromosome analysis of postmortem corneal endothelium after sex-mismatch descemet membrane endothelial keratoplasty. Cornea 36:11–16. https://doi.org/10.1097/ICO.0000000000001019
Regis-Pacheco LF, Binder PS (2014) What happens to the corneal transplant endothelium after penetrating keratoplasty? Cornea 33:587–596. https://doi.org/10.1097/ICO.0000000000000120
Jones DH, Kirkness CM (2001) A new surgical technique for keratoglobus-tectonic lamellar keratoplasty followed by secondary penetrating keratoplasty. Cornea 20:885–887. https://doi.org/10.1097/00003226-200111000-00022
Rasheed K, Rabinowitz YS (2000) Treatment of advanced pellucid marginal degeneration. Ophthalmology 107:1836–1840. https://doi.org/10.1016/S0161-6420(00)00346-8
Anshu A, Price MO, Price FW (2012) Descemet’s stripping endothelial keratoplasty: long-term graft survival and risk factors for failure in eyes with preexisting glaucoma. Ophthalmology 119:1982–1987. https://doi.org/10.1016/j.ophtha.2012.04.031
Kang JJ, Ritterband DC, Lai K et al (2016) Descemet stripping endothelial keratoplasty in eyes with previous glaucoma surgery. Cornea 35:1520–1525. https://doi.org/10.1097/ICO.0000000000001058
Awwad ST, Heilman M, Hogan RN et al (2007) Severe reactive ischemic posterior segment inflammation in acanthamoeba keratitis: a new potentially blinding syndrome. Ophthalmology 114:313–320. https://doi.org/10.1016/j.ophtha.2006.07.038
Shi L, Hager T, Fries FN et al (2019) Reactive uveitis, retinal vasculitis and scleritis as ocular end-stage of Acanthamoeba keratitis: a histological study. Int J Ophthalmol 12:1966–1971. https://doi.org/10.18240/ijo.2019.12.20
Bourne WM, Hodge DO, Nelson LR (1994) Corneal endothelium five years after transplantation. Am J Ophthalmol 118:185–196. https://doi.org/10.1016/S0002-9394(14)72898-3
Bourne WM (2001) Cellular changes in transplanted human corneas. Cornea 20:560–569. https://doi.org/10.1097/00003226-200108000-00002
Patel S, Hodge D, Bourne WM (2004) Corneal endothelium and postoperative outcomes 15 years after penetrating keratoplasty. Trans Am Ophthalmol Soc 102:57–66
Lagali N, Stenevi U, Claesson M et al (2010) Donor and recipient endothelial cell population of the transplanted human cornea: a twodimensional imaging study. Invest Ophthalmol Vis Sci 51:1898–1904. https://doi.org/10.1167/iovs.09-4066
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection and analysis were performed by Karl Anders Knutsson. The first draft of the manuscript was written by Karl Anders Knutsson and all authors contributed to the development of the final version. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical approval was waived by the local Ethics Committee (Ospedale San Raffaele Ethics Committee) in view of the retrospective nature of the study and all the procedures being performed were part of routine care. The study was in adherence to the tenets of the Declaration of Helsinki.
Informed consent was obtained for all patients.
Consent for publication
Not applicable, no identifying information.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Knutsson, K.A., Paganoni, G. & Rama, P. Two-step keratoplasty for deep vascularized corneal opacity with severe peripheral thinning following Acanthamoeba keratitis. Graefes Arch Clin Exp Ophthalmol 259, 2279–2285 (2021). https://doi.org/10.1007/s00417-021-05205-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-021-05205-0