Abstract
Purpose
To investigate the correlation between postoperative corneal astigmatism (PCA) and values of intraoperative keratoscopy analyzed with a newly developed automated technique in patients undergoing big-bubble (BB) deep anterior lamellar keratoplasty (DALK).
Methods
Photographs of keratoscope rings taken at the end of BB-DALK were analyzed using ImageJ for the calculation of “roundness” (R): values = 1 indicate a perfect circle. Pearson’s correlation was used to evaluate the relationship between R and PCA that measured 1 week (V1), 3 months (V2), and 18 months (V3), postoperatively. The area under the curve (AUC) of receiver operating characteristic (ROC) curve was used to evaluate the accuracy of R for identifying patients with PCA < 3 diopters (D). The point on the ROC curve nearest to the coordinate (0,100) was used as a cutoff to determine sensitivity and specificity.
Results
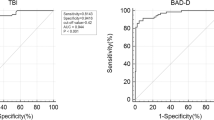
Data from 121 patients were included. The mean value of R*was 0.93 ± 0.04 (range 0.76–0.99). R showed a significant correlation with PA at V3 (R = − 0.42, P < 0.01). The ROC curve had an AUC of 0.69 (95% CI 0.59–0.79). A cutoff value of R = 0.93 had a sensitivity of 70.3% and specificity of 61.0% for identifying patients with PA < 3D at V3.
Conclusions
This new digital analysis of keratoscope rings allows to identify with reasonably good diagnostic accuracy patients with low values of post-DALK astigmatism correctable with spectacles.


Similar content being viewed by others
References
Scorcia V, Giannaccare G, Logozzo L et al (2020) Keratoconus: advances in anterior lamellar keratoplasty techniques. Expert Rev Ophthalmol 1:59–66
Coster DJ, Lowe MT, Keane MC et al (2014) A comparison of lamellar and penetrating keratoplasty outcomes: a registry study. Ophthalmology 121:979–987
Reinhart WJ, Musch DC, Jacobs DS et al (2011) Deep anterior lamellar keratoplasty as an alternative to penetrating keratoplasty a report by the American Academy of Ophthalmology. Ophthalmology 118:209–218
Giannacccare G, Weiss JS, Sapigni L et al (2018) Immunologic stromal rejection after deep anterior lamellar keratoplasty with grafts of a larger size (9 mm) for various stromal diseases. Cornea 37:967–972
Anwar M, Teichmann KD (2002) Big bubble technique to bare Descemet's membrane in anterior lamellar keratoplasty. J Cataract Refract Surg 28:398–403
Fontana L, Parente G, Tassinari G (2007) Clinical outcomes after deep anterior lamellar keratoplasty using the big-bubble technique in patients with keratoconus. Am J Ophthalmol 143:117–124
Romano V, Iovieno A, Parente G et al (2015) Long-term clinical outcomes of deep anterior lamellar keratoplasty in patients with keratoconus. Am J Ophthalmol 159:505–511
Brahma A, Ridgway A, Tullo A et al (2000) Centration of donor trephination in human corneal transplantation. Cornea 19:325–328
Huang T, Hu Y, Gui M et al (2015) Large-diameter deep anterior lamellar keratoplasty for keratoconus: visual and refractive outcomes. Br J Ophthalmol 99:1196–1200
Feizi S, Javadi MA, Behnaz N et al (2018) Effect of suture removal on refraction and graft curvature after deep anterior lamellar keratoplasty in patients with keratoconus. Cornea 37:39–44
Busin M, Leon P, Nahum Y et al (2017) Large (9 mm) deep anterior lamellar keratoplasty with clearance of a 6-mm optical zone optimizes outcomes of keratoconus surgery. Ophthalmology 124:1072–1080
Salouti R, Zamani M, Ghoreyshi M et al (2019) Comparison between manual trephination versus femtosecond laser-assisted deep anterior lamellar keratoplasty for keratoconus. Br J Ophthalmol 103:1716–1723
Chamberlain WD (2020) Femtosecond laser-assisted deep anterior lamellar keratoplasty. Curr Opin Ophthalmol 30:256–263
Masket S (1988) Correlation between intraoperative and early postoperative keratometry. J Cataract Refract Surg 14:277–280
Morlet N (1994) Clinical utility of the astigmatic dial Barrett keratoscope with astigmatic dial. Ophthalmic Surg 25:150–153
Serdarevic ON, Renard GJ, Pouliquen Y (1995) Randomized clinical trial of penetrating keratoplasty. Before and after suture removal comparison of intraoperative and postoperative suture adjustment. Ophthalmology 102:1497–1503
Shimazaki J, Shimmura S, Tsubota K (1998) Intraoperative versus postoperative suture adjustment after penetrating keratoplasty. Cornea 17:590–594
Scorcia V, Giannaccare G, Lucisano A et al (2020) Predictors of bubble formation and type obtained with pneumatic dissection during deep anterior lamellar keratoplasty in keratoconus. Am J Ophthalmol 212:127–133
Scorcia V, De Luca V, Lucisano A et al (2020) Comparison of corneal densitometry between big-bubble and visco-disco-bubble deep anterior lamellar keratoplasty. Br J Ophthalmol 104:336–340
Troutman RC, Kelly S, Kaye D et al (1977) The use and preliminary results of the Troutman surgical keratometer in cataract and corneal surgery. Trans Am Acad Ophthalmol Otolaryngol 83:232–238
Pellegrini M, Bernabei F, Moscardelli F et al (2019) Assessment of corneal fluorescein staining in different dry eye subtypes using digital image analysis. Transl Vis Sci Technol 8:34
Fares U, Sarhan AR, Dua HS (2012) Management of post-keratoplasty astigmatism. J Cataract Refract Surg 38:2029–2039
Kaufman HE (1982) Astigmatism after keratoplasty - possible cause and method of prevention. Am J Ophthalmol 94:556–557
Elkadim M, Myerscough J, Bovone C et al (2020) Astigmatism orientation after deep anterior lamellar keratoplasty for keratoconus and its correlation with preoperative peripheral corneal astigmatism. Cornea 39:192–195
Schnitzler AC, Salla S, Hamsley N et al (2016) Role of the endothelial layer in the deswelling process of organ-cultured human corneas before transplantation. Cornea 35:1216–1221
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (Comitato Etico Regione Calabria Sezione Area Centro – 280-2019) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Graefe’s Archive for Clinical and Experimental Ophthalmology – Cornea
Rights and permissions
About this article
Cite this article
Giannaccare, G., Lucisano, A., Pellegrini, M. et al. Automated digital analysis of intraoperative keratoscopy and its correlation with postoperative astigmatism after big-bubble deep anterior lamellar keratoplasty. Graefes Arch Clin Exp Ophthalmol 259, 469–474 (2021). https://doi.org/10.1007/s00417-020-04912-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-020-04912-4