Abstract
Purpose
A majority of phakic patients undergoing pars plana vitrectomy for epiretinal membrane or macular hole require subsequent cataract surgery within 1–2 years. Combined phaco-vitrectomy eliminates the need for a second surgery and may enable patients to attain their best vision sooner. This study aims to compare the visual outcomes, complication rates, and costs of combined phaco-vitrectomy versus sequential vitrectomy followed by cataract surgery.
Methods
Records were searched by CPT® codes to identify patients with both cataract and vitrectomy surgery at our institution over a 5-year period (2013–2018). Chart review included medical history, demographics, exam findings, operating room records, visual acuity (VA), and clinical outcomes. Statistical analyses were performed with SPSS v19 (IBM). Area under the curve for visual acuity was calculated as the trapezoidal mean of the change in Early Treatment of Diabetic Retinopathy Study letters.
Results
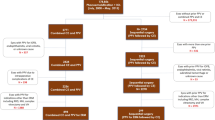
After exclusion, 81 eyes of 78 patients underwent both cataract and vitrectomy surgeries at our institution. Thirty-four eyes underwent separate, sequential vitrectomy then phacoemulsification surgery, and 47 eyes had combined phaco-vitrectomy surgery. Total operating room times (120.81 ± 3.41 vs 161.03 ± 5.45 min; p < 0.0001) and associated costs were significantly lower in the combined surgery compared with those in the sequential surgery group. Baseline and final visual acuity were similar between the two groups. Baseline VA was 35.53 letters (~ 20/200) and 32.81 letters (~ 20/220) and increased to final VA of 63.74 (~ 20/53) and 60.91 letters (~ 20/61), in the sequential and combined groups respectively. Area under the curve for vision was greater in the combined surgery group, with subjects gaining an average of + 9.11 ± 3.32 letters from sequential surgery, and + 19.53 ± 3.53 letters in the combined surgery group (p = 0.04). Additionally, patients in the combined group attained their best visual acuity 449 days (15 months) sooner than those receiving sequential surgery.
Conclusions
Combined phaco-vitrectomy surgery resulted in greater area under the curve visual acuity benefit and attainment of best visual acuity 15 months sooner compared with conventional sequential surgeries. There were no significant differences in complication rates or clinical outcomes between the groups, but operative times and costs were lower for combined surgery, supporting a favorable cost-benefit ratio.

Graphical abstract

Similar content being viewed by others
References
Cheng L, Azen SP, El-Bradey MH et al (2001) Duration of vitrectomy and postoperative cataract in the vitrectomy for macular hole study. Am J Ophthalmol 132:881–887
Jackson TL, Donachie PHJ, Williamson TH et al (2015) The Royal College Of Ophthalmologists’ national ophthalmology database study of vitreoretinal surgery: report 4, epiretinal membrane. Retina Phila Pa 35:1615–1621. https://doi.org/10.1097/IAE.0000000000000523
Jackson TL, Donachie PHJ, Sparrow JM, Johnston RL (2013) United Kingdom National Ophthalmology Database study of vitreoretinal surgery: report 2, macular hole. Ophthalmology 120:629–634. https://doi.org/10.1016/j.ophtha.2012.09.003
Mompremier M, Adyanthaya R Retina today - phacovitrectomy for the retina surgeon. In: Retina Today http://retinatoday.com/2014/10/phacovitrectomy-for-the-retina-surgeon/. Accessed 14 May 2019
Writing Committee for the Diabetic Retinopathy Clinical Research Network, Gross JG, Glassman AR et al (2015) Panretinal photocoagulation vs intravitreous ranibizumab for proliferative diabetic retinopathy: a randomized clinical trial. JAMA 314:2137–2146. https://doi.org/10.1001/jama.2015.15217
Gregori NZ, Feuer W, Rosenfeld PJ (2010) Novel method for analyzing snellen visual acuity measurements. Retina Phila Pa 30:1046–1050. https://doi.org/10.1097/IAE.0b013e3181d87e04
Hamoudi H, Correll Christensen U, La Cour M (2018) Epiretinal membrane surgery: an analysis of 2-step sequential- or combined phacovitrectomy surgery on refraction and macular anatomy in a prospective trial. Acta Ophthalmol 96:243–250. https://doi.org/10.1111/aos.13572
Demetriades A-M, Gottsch JD, Thomsen R et al (2003) Combined phacoemulsification, intraocular lens implantation, and vitrectomy for eyes with coexisting cataract and vitreoretinal pathology. Am J Ophthalmol 135:291–296
Wensheng L, Wu R, Wang X et al (2009) Clinical complications of combined phacoemulsification and vitrectomy for eyes with coexisting cataract and vitreoretinal diseases. Eur J Ophthalmol 19:37–45
Pinarci EY, Bayar SA, Sizmaz S et al (2013) Anterior segment complications after phacovitrectomy in diabetic and nondiabetic patients. Eur J Ophthalmol 23:223–229. https://doi.org/10.5301/ejo.5000203
Höhn F, Kretz F, Pavlidis M (2016) Surgical and functional results of hybrid 25-27-gauge vitrectomy combined with coaxial 2.2 mm small incision cataract surgery. J Ophthalmol 2016:9186351. https://doi.org/10.1155/2016/9186351
Fajgenbaum MAP, Neffendorf JE, Wong RS et al (2018) Intraoperative and postoperative complications in phacovitrectomy for epiretinal membrane and macular hole: a clinical audit of 1,000 consecutive eyes. Retina Phila Pa 38:1865–1872. https://doi.org/10.1097/IAE.0000000000002034
Sizmaz S, Esen E, Isik P et al (2019) Outcome and complications of combined phacoemulsification and 23-gauge pars plana vitrectomy. J Ophthalmol 2019:7918237. https://doi.org/10.1155/2019/7918237
Ercan ZE, Akkoyun İ, Yaman Pınarcı E et al (2017) Refractive outcome comparison between vitreomacular interface disorders after phacovitrectomy. J Cataract Refract Surg 43:1068–1071. https://doi.org/10.1016/j.jcrs.2017.06.034
Erçalık NY, Yenerel NM, Sanisoğlu HA et al (2017) Comparison of intra- and postoperative complications of phaco between sequential and combined procedures of 23-gauge vitrectomy and phaco. Saudi J Ophthalmol Off J Saudi Ophthalmol Soc 31:238–242. https://doi.org/10.1016/j.sjopt.2017.04.005
Lee JY, Kim K-H, Shin KH et al (2012) Comparison of intraoperative complications of phacoemulsification between sequential and combined procedures of pars plana vitrectomy and cataract surgery. Retina Phila Pa 32:2026–2033. https://doi.org/10.1097/IAE.0b013e3182561fab
van der Geest LJ, Siemerink MJ, Mura M et al (2016) Refractive outcomes after phacovitrectomy surgery. J Cataract Refract Surg 42:840–845. https://doi.org/10.1016/j.jcrs.2016.03.034
Shi L, Chang JS, Suh LH, Chang S (2018) Differences in refractive outcomes between phacoemulsification for cataract alone and combined phacoemulsification and vitrectomy for epiretinal membrane. Retina Phila Pa. https://doi.org/10.1097/IAE.0000000000002153
Jee D, Park Y-R, Jung KI et al (2015) Refractive errors in high myopic eyes after phacovitrectomy for macular hole. Int J Ophthalmol 8:369–373. https://doi.org/10.3980/j.issn.2222-3959.2015.02.28
Hamoudi H, La Cour M (2013) Refractive changes after vitrectomy and phacovitrectomy for macular hole and epiretinal membrane. J Cataract Refract Surg 39:942–947. https://doi.org/10.1016/j.jcrs.2013.04.012
Shiraki N, Wakabayashi T, Sakaguchi H, Nishida K (2018) Optical biometry-based intraocular lens calculation and refractive outcomes after phacovitrectomy for rhegmatogenous retinal detachment and epiretinal membrane. Sci Rep 8:11319. https://doi.org/10.1038/s41598-018-29553-w
Seider MI, Michael Lahey J, Fellenbaum PS (2014) Cost of phacovitrectomy versus vitrectomy and sequential phacoemulsification. Retina Phila Pa 34:1112–1115. https://doi.org/10.1097/IAE.0000000000000061
Leiderman YI, Andreoli MT, Sun B, Dawood S (2015) Pars plana vitrectomy combined with cataract extraction: a comparison of surgical outcomes using single-piece and multipiece foldable intraocular lenses. Retina Phila Pa 35:1059–1064. https://doi.org/10.1097/IAE.0000000000000467
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest..
Research involving human participants
This is a retrospective study. This article does not contain any studies with human participants or animals performed by any of the authors.
Ethical approval
Institutional Review Board Approval was obtained prior to initiation of chart review.
Informed consent
This type of study does not require informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Port, A.D., Nolan, J.G., Siegel, N.H. et al. Combined phaco-vitrectomy provides lower costs and greater area under the curve vision gains than sequential vitrectomy and phacoemulsification. Graefes Arch Clin Exp Ophthalmol 259, 45–52 (2021). https://doi.org/10.1007/s00417-020-04877-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-020-04877-4