Abstract
Purpose
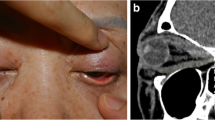
To examine Bell’s phenomenon in patients with unilateral thyroid-associated inferior rectus myopathy and changes in this phenomenon after inferior rectus muscle recession.
Methods
This prospective interventional study included 12 patients who underwent inferior rectus muscle recession with or without nasal transposition. Bell’s phenomenon was examined before and 3 months after surgery. The upper eyelid was held open by a finger to prevent complete eyelid closure. Then, the distance of upward excursion of the inferior corneal limbus or the corneal light reflex was measured during voluntary maximum forced eyelid closure. The pre- and postoperative distances of upward excursion on the affected side were statistically compared with the preoperative distance on the unaffected side using the Mann-Whitney U test, and the pre- and postoperative distances on the affected side were statistically compared using paired t-test. The relationships among postoperative changes of Bell’s phenomenon, patient age, the amount of recession and nasal transposition of the inferior rectus muscle, postoperative angle of ocular deviation, and reduction in the angle after surgery were analyzed using stepwise multiple regression analyses.
Results
The preoperative measurement of Bell’s phenomenon was significantly shorter on the affected side (1.6 ± 1.6 mm) than the unaffected side (4.3 ± 1.6 mm; P = 0.001). However, the distance on the affected side significantly increased after surgery (4.1 ± 1.9 mm; P < 0.001), compared to the preoperative distance on the unaffected side (P = 0.843). Using a stepwise method, all variables were deleted from the regression equation.
Conclusions
Bell’s phenomenon decreased on the affected side, which improved after inferior rectus muscle recession.

Similar content being viewed by others
References
Jones DH (2001) Bell's phenomenon should not be regarded as a pathognomonic sign. BMJ 323:935
Yoon JS, Lew H, Lee SY (2008) Bell’s phenomenon protects the tear film and ocular surface after frontalis suspension surgery for congenital ptosis. J Pediatr Ophthalmol Strabismus 45:350–355
Takahashi Y, Kakizaki H (2015) Predictors of the dose-effect relationship regarding unilateral inferior rectus muscle recession in patients with thyroid eye disease. Int J Endocrinol 2015:703671
Eckstein AK, Finkenrath A, Heiligenhaus A, Renzing-Köhler K, Esser J, Krüger C, Quadbeck B, Steuhl KP, Gieseler RK (2004) Dry eye syndrome in thyroid-associated ophthalmopathy: lacrimal expression of TSH receptor suggests involvement of TSHR-specific autoantibodies. Acta Ophthalmol Scand 82:291–297
Wiersinga WM, Kahaly GJ (2007) Graves’ Orbitopathy: A Multidisciplinary Approach. Karger, Basel, pp 176–200
Shen S, Fong KS, Wong HB, Looi A, Chan LL, Rootman J, Seah LL (2010) Normative measurements of the Chinese extraocular musculature by high-field magnetic resonance imaging. Invest Ophthalmol Vis Sci 51:631–636
Alvarez G (1980) Bell’s phenomenon in normal adults and in Parkinson’s disease. Acta Neurol Scand 62:127–131
Takahashi Y, Kitaguchi Y, Nakakura S, Mito H, Kimura A, Kakizaki H (2016) Correction of excyclotropia by surgery on the inferior rectus muscle in patients with thyroid eye disease: a retrospective, observational study. PLoS One 11:e0159562
Kakizaki H, Zako M, Iwaki M (2007) Lower eyelid lengthening surgery targeting the posterior layer of the lower eyelid retractors via a transcutaneous approach. Clin Ophthalmol 1:141–147
Miyata K, Amano S, Sawa M, Nishida T (2003) A novel grading method for superficial punctate keratopathy magnitude and its correlation with corneal epithelial permeability. Arch Ophthalmol 121:1537–1539
Dutton JJ (2011) Extraocular muscles. In: Dutton JJ (ed) Atlas of Clinical and Surgical Orbital Anatomy, 2nd edn. Elsevier Saunders, Philadelphia, pp 29–49
Akbari MR, Raygan F, Ameri A, Jafari A, Eshraghi B, Fard MA (2013) Lower eyelid retractor lysis versus Lockwood advancement to minimize lower eyelid retraction resulting from inferior rectus muscle recession. J AAPOS 17:445–447
Wright KW, Strube YNJ (2015) Thyroid strabismus. In: Wright KW, Strube YNJ (eds) Color Atlas of Strabismus Surgery: Strategies and Techniques, 4th edn. Springer, New York, p 45
Dutton J (2002) Surgical management of eyelid retraction in thyroid eye disease. In: Dutton J, Haik BG (eds) Thyroid Eye Disease: Diagnosis and Treatment. Marcel Dekker Inc., New York, pp 413–422
Gilbert J, Dailey RA, Christensen LE (2005) Characteristics and outcomes of strabismus surgery after orbital decompression surgery. J AAPOS 9:26–30
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
All authors have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers' bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Other Contributors
None.
Rights and permissions
About this article
Cite this article
Takahashi, Y., Sabundayo, M.S., Mito, H. et al. Bell’s phenomenon in thyroid-associated inferior rectus myopathy. Graefes Arch Clin Exp Ophthalmol 255, 2467–2471 (2017). https://doi.org/10.1007/s00417-017-3792-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-017-3792-9