Abstract
Objective
To evaluate the functional efficacy of an iridotomy in primary angle closure (PAC) eyes by measuring IOP responses to provocative tests before and after iridotomy.
Design
Prospective cohort study.
Subjects
50 consecutive adult patients, 40–60 years of age, having primary angle closure.
Methods
Clinical examination, perimetry, biometry and ultrasound biomicroscopy of the angle were done. A darkroom prone provocative test (DRPPT), a mydriatic test and a Valsalva maneuver were performed before and after the iridotomy.
Main outcome measures
IOP change in response to the provocative tests before and after iridotomy, and correlation with baseline parameters.
Results
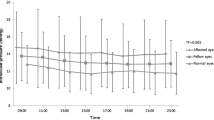
IOP at baseline and after iridotomy was 14.4 ± 2.7 mmHg and 14.3 ± 2.6 mmHg, respectively (p = 0.)83. There was no significant change on diurnal phasing before and after an iridotomy (p = 0.)11. The mean IOP rise was 5.9 ± 3.7 mmHg on the DRPPT, 4.3 ± 3.5 mmHg on the Mydriatic test and 9.1 ± 4.9 mmHg on the Valsalva maneuver, and was reduced significantly to 3.2 ± 2.1 mmHg, 2.3 ± 1.8 and 6.4 ± 3.5, respectively(p < 0.001 for all tests). The decrease in pupillary block component for all 50 eyes was 46.5 % for the mydriatic test, 45.8 % for the DRPPT and 29.7 % for the Valsalva maneuver. PAC eyes positive on the DRPPT and mydriatic test prior to an iridotomy became negative after laser iridotomy in 75.9 and 84.6 % eyes, respectively, but on the Valsalva maneuver, only 23.8 % became negative. After iridotomy, eyes that continued to be positive on the mydriatic test had a significantly thicker lens (p = 0.02), decreased TCPD (p = 0.014) and narrower trabecular–iris angle (p = 0.048). On the DRPPT, they had a thicker lens (p = 0.03), shorter iris thickness (p = 0.025) and TCPD (p = 0.032), and on the Valsalva maneuver, they had a narrower scleral–ciliary process angle (SCPA; p = 0.019) and shorter TCPD (p = 0.015).
Conclusions
This comprehensive functional evaluation of laser iridotomy in early PAC eyes showed a significant reduction in the pupillary block component of IOP response to provocative testing, possibly decreasing IOP fluctuations over time. An iridotomy does not, however, significantly change mean IOP or diurnal phasing of IOP in PAC eyes. Eyes with a very narrow angle or a thick lens may continue to have angle closure due to other pathomechanisms for angle closure.


Similar content being viewed by others
References
Quigley HA, Broman AT (2006) The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol 90:262–267
Foster PJ, Buhrmann R, Quigley HA, Johnson GJ (2002) The definition and classification of glaucoma in prevalence surveys. Br J Ophthalmol 86:238–242
Han S, Sung KR, Lee KS, Hong JW (2014) Outcomes of laser peripheral iridotomy in angle closure subgroups according to anterior segment optical coherence tomography parameters. Invest Ophthalmol Vis Sci 55:6795–6801
Jiang Y, Chang DS, Zhu H, Khawaja AP, Aung T, Huang S, Chen Q, Munoz B, Grossi CM, He M, Friedman DS, Foster PJ (2014) Longitudinal changes of angle configuration in primary angle-closure suspects: the zhongshan angle-closure prevention trial. Ophthalmology 121:1699–1705
He M, Friedman DS, Ge J, Huang W, Jin C, Cai X, Khaw PT, Foster PJ (2007) Laser peripheral iridotomy in eyes with narrow drainage angles: ultrasound biomicroscopy outcomes. The Liwan eye study. Ophthalmology 114:1513–1519
He M, Friedman DS, Ge J, Huang W, Jin C, Lee PS, Khaw PT, Foster PJ (2007) Laser peripheral iridotomy in primary angle-closure suspects: biometric and gonioscopic outcomes: the Liwan eye study. Ophthalmology 114:494–500
See JL, Chew PT, Smith SD, Nolan WP, Chan YH, Huang D, Zheng C, Foster PJ, Aung T, Friedman DS (2007) Changes in anterior segment morphology in response to illumination and after laser iridotomy in Asian eyes: an anterior segment OCT study. Br J Ophthalmol 91:1485–1489
Nolan WP, Foster PJ, Devereux JG, Uranchimeg D, Johnson GJ, Baasanhu J (2000) YAG laser iridotomy treatment for primary angle closure in East Asian eyes. Br J Ophthalmol 84(11):1255–1259
Yip JL, Foster PJ, Uranchimeg D, Javzandulam B, Javzansuren D, Munhzaya T, Lee PS, Baassanhuu J, Gilbert CE, Khaw PT, Johnson GJ, Nolan WP (2010) Randomised controlled trial of screening and prophylactic treatment to prevent primary angle closure glaucoma. Br J Ophthalmol 94(11):1472–1477
Pandav SS, Kaushik S, Jain R, Bansal R, Gupta A (2007) Laser peripheral iridotomy across the spectrum of primary angle closure. Can J Ophthalmol 42:233–237
Yao BQ, Wu LL, Zhang C, Wang X (2009) Ultrasound biomicroscopic features associated with angle closure in fellow eyes of acute primary angle closure after laser iridotomy. Ophthalmology 116:444–448
Choi JS, Kim YY (2005) Progression of peripheral anterior synechiae after laser iridotomy. Am J Ophthalmol 140:1125–1127
Yeung BY, Ng PW (2005) Prevalence and mechanism of appositional angle closure in acute primary angle closure after iridotomy. Clin Exp Ophthalmol 33:478–482
Sihota R, Dada T, Aggarwal A, Srinivasan G, Gupta V, Chabra VK (2008) Does an iridotomy prevent angle closure during Valsalva maneuvre in eyes with primary angle closure? Eye 22:389–393
Garudadri CS, Chelerkar V, Nutheti R (2002) An ultrasound biomicroscopic study of the anterior segment in Indian eyes with primary angle-closure glaucoma. J Glaucoma 11:502–507
Lowe RF (1967) Primary angle-closure glaucoma. A review of provocative tests. Br J Ophthalmol 51(11):727–732
Hong C, Park KH (1996) Evaluation of pupillary block component in angle-closure glaucoma. Jpn J Ophthalmol 40:239–243
Wishart PK (1991) Does the pilocarpine phenylephrine provocative test help in the management of acute and subacute angle closure glaucoma? Br J Ophthalmol 75:284–287
Sihota R, Dada T, Gupta V, Deepak KK, Pandey RM (2006) Narrowing of anterior chamber angle during Valsalva maneuver: a possible mechanism for angle closure. Eur J Ophthalmol 16:81–91
Nonaka A, Kondo T (2006) Angle widening and alteration of ciliary process configuration after cataract surgery for primary angle closure. Ophthalmology 113:437–441
Feibel RM (1981) Edward J Curran and the concept of relative pupillary block. Surv Ophthalmol 25:270–278
Congdon NG, Youlin Q, Quigley H, Hung PT, Wang TH, Ho TC, Tielsch JM (1997) Biometry and primary angle-closure glaucoma among Chinese, white, and black populations. Ophthalmology 104:1489–1495
Marchini G, Pagliarusco A, Toscano A, Tosi R, Brunelli C, Bonomi L (1998) Ultrasound biomicroscopic and conventional ultrasonographic study of ocular dimensions in primary angle-closure glaucoma. Ophthalmology 105:2091–2098
Lei K, Wang N, Wang L, Wang B (2009) Morphological changes of the anterior segment after laser peripheral iridotomy in primary angle closure. Eye (Lond) 23(2):345–350
Ramani KK, Mani B, George RJ, Lingam V (2009) Follow-up of primary angle closure suspects after laser peripheral iridotomy using ultrasound biomicroscopy and a-scan biometry for a period of 2 years. J Glaucoma 18(7):521–527
Talajic JC, Lesk MR, Nantel-Battista M, Harasymowycz PJ (2013) Anterior segment changes after pilocarpine and laser iridotomy for primary angle-closure suspects with scheimpflug photography. J Glaucoma 22(9):776–779
Sawada A, Yamamoto T (2012) Correlation between extent of preexisting organic angle closure and long-term outcome after laser peripheral iridotomy in eyes with primary angle closure. J Glaucoma 21(3):174–179
Baskaran M, Kumar RS, Govindasamy CV, Htoon HM, Wong CY, Perera SA, Wong TT, Aung T (2009) Diurnal intraocular pressure fluctuation and associated risk factors in eyes with angle closure. Ophthalmology 116(12):2300–2304
Chen YY, Sun LP, Thomas R, Liang YB, Fan SJ, Sun X, Li SZ, Zhang SD, Wang NL (2011) Long-term intraocular pressure fluctuation of primary angle closure disease following laser peripheral iridotomy/iridoplasty. Chin Med J (Engl) 124(19):3066–3069
Desgroseilliers A, Harasymowycz PJ, Kamdeu-Fansi A, Tardif D, Lesk MR (2014) Gonioscopic findings associated with a positive dark-room provocative test in narrow angles after laser iridotomy. J Glaucoma 23(6):337–340
Yan Y, Wu L, Wang X, Xiao G (2014) Appositional angle closure in Chinese with primary angle closure and primary angle closure glaucoma after laser peripheral iridotomy. Invest Ophthalmol Vis Sci 55:8506–8512
Caronia RM, Liebmann JM, Stegman Z, Sokol J, Ritch R (1996) Increase in iris-lens contact after laser iridotomy for pupillary block angle closure. Am J Ophthalmol 122:53–57
Lee RY, Kasuga T, Cui QN, Porco TC, Huang G, He M, Lin SC (2014) Association between baseline iris thickness and prophylactic laser peripheral iridotomy outcomes in primary angle-closure suspects. Ophthalmology 121(6):1194–1202
Zheng C, Guzman CP, Cheung CY, He Y, Friedman DS, Ong SH, Narayanaswamy AK, Chew PT, Perera SA, Aung T (2013) Analysis of anterior segment dynamics using anterior segment optical coherence tomography before and after laser peripheral iridotomy. JAMA Ophthalmol 131(1):44–49
Wang BS, Xiao L, Liu J, Dong N, Aung T (2012) Dynamic changes in anterior segment morphology during the Valsalva maneuver assessed with ultrasound biomicroscopy. Invest Ophthalmol Vis Sci 53:7286–7289
Quigley HA (2009) Angle-closure glaucoma-simpler answers to complex mechanisms: LXVI Edward Jackson memorial lecture. Am J Ophthalmol 148(5):657–669
Zhang Z, Wang X, Jonas JB, Wang H, Zhang X, Peng X, Ritch R, Tian G, Yang D, Li L, Li J, Wang N (2014) Valsalva manoeuver, intra-ocular pressure, cerebrospinal fluid pressure, optic disc topography: Beijing intracranial and intra-ocular pressure study. Acta Ophthalmol 92:475–480
Sihota R, Dada T, Gupta R, Lakshminarayan P, Pandey RM (2005) Ultrasound biomicroscopy in the subtypes of primary angle closure glaucoma. J Glaucoma 14:387–391
Mizoguchi T, Ozaki M, Wakiyama H, Ogino N (2014) Peripheral iris thickness and association with iridotrabecular contact after laser peripheral iridotomy in patients with primary angle-closure and primary angle-closure glaucoma. Clin Ophthalmol 8:517–522
Leidl MC, Choi CJ, Syed ZA, Melki SA (2014) Intraocular pressure fluctuation and glaucoma progression: what do we know? Br J Ophthalmol 98(10):1315–1319
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of interest statement
All authors certify that they have NO affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest; and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Sihota, R., Rishi, K., Srinivasan, G. et al. Functional evaluation of an iridotomy in primary angle closure eyes. Graefes Arch Clin Exp Ophthalmol 254, 1141–1149 (2016). https://doi.org/10.1007/s00417-016-3298-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-016-3298-x