Abstract
Purpose
The purpose of this study was to evaluate the regression of neovascularization elsewhere (NVE) after panretinal photocoagulation (PRP) based on its location in relation to the internal limiting membrane (ILM).
Methods
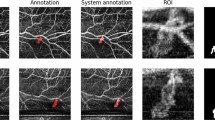
Participants in this retrospective case series were 47 patients with active NVE within the vascular arcade. All patients were treated with PRP and followed up for at least 12 months. The time to regression of NVE based on its location relative to the ILM on spectral domain-optical coherence tomography (SD-OCT) was analyzed.
Results
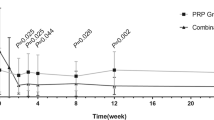
The proportion of eyes, showing regression of NVE at the end of follow-up period was 19/25 (76 %) in the “below ILM” group and 13/22 (59 %) in the “above ILM” group. The “below ILM” group was associated with a twofold enhanced regression of NVE in comparison to the “above ILM” group (HR = 2.13, p = 0.038).
Conclusions
Regression of NVE is determined by its location relative to the ILM. Patients with “below ILM” NVE were found to show a twofold increased regression rate in comparison with the “above ILM” group, while the proportion of eyes showing regression of NVE at the end of the follow-up period was significantly greater in the “below ILM” than the “above ILM” group.




Similar content being viewed by others
References
Wild S, Roglic G, Green A, Sicree R, King H (2004) Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 27:1047–1053
Antonetti DA, Klein R, Gardner TW (2012) Diabetic retinopathy. N Engl J Med 366:1227–1239
Muqit MM, Stanga PE (2014) Fourier-domain optical coherence tomography evaluation of retinal and optic nerve head neovascularisation in proliferative diabetic retinopathy. Br J Ophthalmol 98:65–72
Cho H, Alwassia AA, Regiatieri CV, Zhang JY, Baumal C, Waheed N, Duker JS (2013) Retinal neovascularization secondary to proliferative diabetic retinopathy characterized by spectral domain optical coherence tomography. Retina 33:542–547
Muqit MM, Stanga PE (2014) Swept-source optical coherence tomography imaging of the cortical vitreous and the vitreoretinal interface in proliferative diabetic retinopathy: assessment of vitreoschisis, neovascularisation and the internal limiting membrane. Br J Ophthalmol 98:994–997
Lee CS, Lee AY, Sim DA, Keane PA, Mehta H, Zarranz-Ventura J, Fruttiger M, Egan CA, Tufail A (2015) Reevaluating the definition of intraretinal microvascular abnormalities and neovascularization elsewhere in diabetic retinopathy using optical coherence tomography and fluorescein angiography. Am J Ophthalmol 159:101–110
Miura M, Muramatsu D, Hong YJ, Yasuno Y, Itami A, Iwasaki T, Goto H (2015) Three-dimensional vascular imaging of proliferative diabetic retinopathy by doppler optical coherence tomography. Am J Ophthalmol 159:528–538
The Diabetic Retinopathy Study Research Group (1976) Preliminary report on effects of photocoagulation therapy. Am J Ophthalmol 81:383–396
KARNS number 1 (1993) Randomized comparison of krypton vs argon scatter photocoagulation for diabetic disc neovascularisation. Ophthalmology 100:1655–1664
Nagpal M, Marlecha S, Nagpal K (2010) Comparison of laser photocoagulation for diabetic retinopathy using 532-nm standard laser versus multispot pattern scan laser. Retina 30:452–458
Alasil T, Waheed NK (2014) Pan retinal photocoagulation for proliferative diabetic retinopathy: pattern scan laser versus argon laser. Curr Opin Ophthalmol 25:164–170
Chappelow AV, Tan K, Waheed NK, Kaiser PK (2012) Panretinal photocoagulation for proliferative diabetic retinopathy: pattern scan laser versus argon laser. Am J Ophthalmol 153:137–142
Burton DS, Carrim ZI (2015) Angiographic evidence of peripheral ischemia in diabetic retinopathy and the risk of impending neovascularisation. Can J Diabetes 39:14–15
Zhu Y, Zhang T, Wang KY, Xu GZ (2014) Prognostic value of multifocal electroretinography and optical coherence tomography in eyes undergoing panretinal photocoagulation for diabetic retinopathy. Invest Ophthalmol Vis Sci 55:6358–6364
Yang CS, Hung KC, Huang YM, Hsu WM (2013) Intravitreal bevacizumab (Avastin) and panretinal photocoagulation in the treatment of high-risk proliferative diabetic retinopathy. J Ocul Pharmacol Ther 29:550–555
Muqit MM, Marcellino GR, Henson DB, Young LB, Patton N, Charles SJ, Turner GS, Stanga PE (2013) Optos-guided pattern scan laser (Pascal)-targeted retinal photocoagulation in proliferative diabetic retinopathy. Acta Ophthalmol 91:251–258
Muqit MM, Young LB, McKenzie R, John B, Marcellino GR, Henson DB, Turner GS, Stanga PE (2013) Pilot randomised clinical trial of Pascal TargETEd Retinal versus variable fluence PANretinal 20 ms laser in diabetic retinopathy: PETER PAN study. Br J Ophthalmol 97:220–227
The Early Treatment Diabetic Retinopathy Study Research Group (1987) Techniques for scatter and local photocoagulation treatment of diabetic retinopathy: Early Treatment Diabetic Retinopathy Study Report No 3. Int Ophthalmol Clin 27:254–264
Muqit MM, Marcellino GR, Henson DB, Young LB, Turner GS, Stanga PE (2011) Pascal panretinal laser ablation and regression analysis in proliferative diabetic retinopathy: Manchester Pascal Study Report 4. Eye 25:1447–1456
Flaxel C, Bradle J, Acott T, Samples JR (2007) Retinal pigment epithelium produces matrix metalloproteinases after laser treatment. Retina 27:629–634
Vujosevic S, Bini S, Midena G, Berton M, Pilotto E, Midena E (2013) Hyperreflective intraretinal spots in diabetics without and with nonproliferative diabetic retinopathy: an in vivo study using spectral domain OCT. J Diabetes Res 2013:491835
Zeng HY, Green WR, Tso MO (2008) Microglial activation in human diabetic retinopathy. Arch Ophthalmol 126:227–232
De Benedetto U, Sacconi R, Pierro L, Lattanzio R, Bandello F (2015) Optical coherence tomographic hyperreflective foci in early stages of diabetic retinopathy. Retina 35:449–453
Davis MD (1965) Vitreous contraction in proliferative diabetic retinopathy. Arch Ophthalmol 74:741–751
Ono R, Kakehashi A, Yamagami H, Sugi N, Kinoshita N, Saito T, Tamemoto H, Kuroki M, Lshikawa SE, Kawakami M (2005) Prospective assessment of proliferative diabetic retinopathy with observations of posterior vitreous detachment. Int Ophthalmol 26:15–19
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this research.
Conflict of Interest
Irini Chatziralli and Theodoros Sergentanis certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria, educational grants, or other equity interest), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript. Sobha Sivaprasad has received research grants, attended Advisory Board meetings of Allergan, Bayer and Novartis.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Institutional review board approval is not required in our institute for retrospective studies.
Rights and permissions
About this article
Cite this article
Chatziralli, I.P., Sergentanis, T.N. & Sivaprasad, S. Prediction of regression of retinal neovascularisation after panretinal photocoagulation for proliferative diabetic retinopathy. Graefes Arch Clin Exp Ophthalmol 254, 1715–1721 (2016). https://doi.org/10.1007/s00417-016-3275-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-016-3275-4