Abstract
Purpose
T helper 17 (Th17) cells are believed to play a critical role in the chronic inflammatory and immune response in streptozotocin (STZ)-induced retinopathy. The purpose of our study was to investigate the effect of the IL-23–Th17–IL-17A pathway via the blood–retinal barrier on STZ-induced diabetic retinopathy in rats.
Methods
The ratio of IL-17A+CD4+ T cells in peripheral blood mononuclear cells of STZ-treated and wild-type rats was determined using flow cytometry. The IL-17A mRNA levels in the retinas were measured using real-time PCR. The protein expression of IL-17A in the peripheral blood and retinas was measured using an ELISA kit. The retinal structure in the wild-type and STZ-treated rats was examined using hematoxylin and eosin (H&E) staining. Additionally, the permeability of the blood–retinal barrier was quantified using the Evans blue technique.
Results
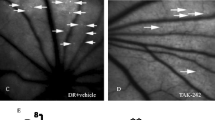
The ratio of IL-17A+CD4+ T cells in peripheral blood mononuclear cells was markedly increased in rats treated with STZ compared to the wild-type group. IL-17A protein levels in the peripheral blood and retinas were also significantly elevated in STZ-treated rats. However, when the anti-IL 23Rp19 antibody was injected into the vitreous cavity in the eyes of STZ-treated rats for a period of one week, retinal pigment epithelium cells became markedly tighter, and micrangium and endothelial cells were significantly reduced. The expression of IL-17A mRNA and protein in the retina also decreased significantly compared with the placebo-treated group.
Conclusions
This study provided further insight into the function of the IL-23–Th17–IL-17A pathway in STZ-induced diabetic retinopathy in rats. Local injection of the anti-IL-23Rp19 antibody may improve the structure of the blood–retinal barrier, thus offering the potential for treatment using intravitreal anti-IL-23Rp19 antibodies.



Similar content being viewed by others
References
Ola MS, Nawaz MI, Siddiquei MM et al (2012) Recent advances in understanding the biochemical and molecular mechanism of diabetic retinopathy. J Diabetes Complicat 26:56–64. doi:10.1016/j.jdiacomp.2011.11.004
Yau JW, Rogers SL, Kawasaki R et al (2012) Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care 35:556–564. doi:10.2337/dc11-1909
Cheung CMG, Vania M, Ang M et al (2012) Comparison of aqueous humor cytokine and chemokine levels in diabetic patients with and without retinopathy. Mol Vis 18:830–837
Giacco F, Brownlee M (2010) Oxidative stress and diabetic complications. Circ Res 107:1058–1070. doi:10.1161/circresaha.110.223545
Milne R, Brownstein S (2013) Advanced glycation end products and diabetic retinopathy. Amino Acids 44:1397–1407. doi:10.1007/s00726-011-1071-3
Tomic M, Ljubic S, Kastelan S (2013) The role of inflammation and endothelial dysfunction in the pathogenesis of diabetic retinopathy. Coll Antropol 37(Suppl 1):51–57
Zipris D (2008) Innate immunity and its role in type 1 diabetes. Curr Opin Endocrinol Diabetes Obes 15:326–331. doi:10.1097/MED.0b013e3283073a46
Shao S, He F, Yang Y et al (2012) Th17 cells in type 1 diabetes. Cell Immunol 280:16–21. doi:10.1016/j.cellimm.2012.11.001
Maddur MS, Miossec P, Kaveri SV et al (2012) Th17 cells: biology, pathogenesis of autoimmune and inflammatory diseases, and therapeutic strategies. Am J Pathol 181:8–18. doi:10.1016/j.ajpath.2012.03.044
Park H, Li Z, Yang XO et al (2005) A distinct lineage of CD4 T cells regulates tissue inflammation by producing interleukin 17. Nat Immunol 6:1133–1141. doi:10.1038/ni1261
Nadeem A, Javaid K, Sami W et al (2013) Inverse relationship of serum IL-17 with type-II diabetes retinopathy. Clin Lab 59:1311–1317
Chen Y, Yang P, Li F et al (2011) The effects of Th17 cytokines on the inflammatory mediator production and barrier function of ARPE-19 cells. PLoS One 6:e18139. doi:10.1371/journal.pone.0018139
Ryba-Stanislawowska M, Skrzypkowska M, Mysliwiec M et al (2013) Loss of the balance between CD4(+)Foxp3(+) regulatory T cells and CD4(+)IL17A(+) Th17 cells in patients with type 1 diabetes. Hum Immunol 74:701–707. doi:10.1016/j.humimm.2013.01.024
Zuniga LA, Jain R, Haines C et al (2013) Th17 cell development: from the cradle to the grave. Immunol Rev 252:78–88. doi:10.1111/imr.12036
Basso AS, Cheroutre H, Mucida D (2009) More stories on Th17 cells. Cell Res 19:399–411. doi:10.1038/cr.2009.26
Bi Y, Yang R (2012) Direct and indirect regulatory mechanisms in TH17 cell differentiation and functions. Scand J Immunol 75:543–552. doi:10.1111/j.1365-3083.2012.02686.x
Yang XO, Pappu BP, Nurieva R et al (2008) T helper 17 lineage differentiation is programmed by orphan nuclear receptors ROR alpha and ROR gamma. Immunity 28:29–39. doi:10.1016/j.immuni.2007.11.016
Lee Y, Awasthi A, Yosef N et al (2012) Induction and molecular signature of pathogenic TH17 cells. Nat Immunol 13:991–999. doi:10.1038/ni.2416
Niimi N, Kohyama K, Matsumoto Y (2013) Therapeutic gene silencing with siRNA for IL-23 but not for IL-17 suppresses the development of experimental autoimmune encephalomyelitis in rats. J Neuroimmunol 254:39–45. doi:10.1016/j.jneuroim.2012.08.015
Toussirot E (2012) The IL23/Th17 pathway as a therapeutic target in chronic inflammatory diseases. Inflamm Allergy Drug Targets 11:159–168
Honkanen J, Nieminen JK, Gao R et al (2010) IL-17 immunity in human type 1 diabetes. J Immunol 185:1959–1967. doi:10.4049/jimmunol.1000788
Iwakura Y, Nakae S, Saijo S et al (2008) The roles of IL-17A in inflammatory immune responses and host defense against pathogens. Immunol Rev 226:57–79. doi:10.1111/j.1600-065X.2008.00699.x
Runkle EA, Antonetti DA (2011) The blood-retinal barrier: structure and functional significance. Methods Mol Biol 686:133–148. doi:10.1007/978-1-60761-938-3_5
Kaya A, Kar T, Aksoy Y et al (2013) Insulin analogues may accelerate progression of diabetic retinopathy after impairment of inner blood-retinal barrier. Med Hypotheses 81:1012–1014. doi:10.1016/j.mehy.2013.09.018
Chen HT, Wang H, Zhao M et al (2012) Regulation of antigen specific Th17 cells differentiation in experimental autoimmune uveitis. Zhonghua Yan Ke Za Zhi 48:234–240
Brandon JA, Jennings CD, Kaplan AM et al (2013) Anti-IL-23p19 therapy inhibits the adoptive transfer of syngeneic graft-versus-host disease. Cytokine 61:732–735. doi:10.1016/j.cyto.2013.01.005
Wu SY, Yu JS, Liu FT et al (2013) Galectin-3 negatively regulates dendritic cell production of IL-23/IL-17-axis cytokines in infection by Histoplasma capsulatum. J Immunol 190:3427–3437. doi:10.4049/jimmunol.1202122
Sato K (2013) The IL-23/IL-17 axis as a therapeutic target. Nihon Rinsho Men’eki Gakkai Kaishi Jpn J Clin Immunol 36:203–208
Kwok SK, Cho ML, Her YM et al (2012) TLR2 ligation induces the production of IL-23/IL-17 via IL-6, STAT3 and NF-kB pathway in patients with primary Sjogren’s syndrome. Arthritis Res Ther 14:R64. doi:10.1186/ar3780
Korn T, Bettelli E, Oukka M et al (2009) IL-17 and Th17 cells. Annu Rev Immunol 27:485–517. doi:10.1146/annurev.immunol.021908.132710
Kim HR, Kim HS, Park MK et al (2007) The clinical role of IL-23p19 in patients with rheumatoid arthritis. Scand J Rheumatol 36:259–264. doi:10.1080/03009740701286813
Ratsimandresy RA, Duvallet E, Assier E et al (2011) Active immunization against IL-23p19 improves experimental arthritis. Vaccine 29:9329–9336. doi:10.1016/j.vaccine.2011.09.134
Acknowledgments
All authors have completed and submitted the ICMJE form for disclosure of potential conflicts of interest, and none were reported. This study was conducted with the approval of the Ethics Committee of Chongqing Medical University. The work was supported by the Health Bureau Foundation of Chongqing Project (2011-1-029) and a National Natural Science Foundation Project Grant (81371843). X.D Zhang and H.Y Xu were involved in the design and conduct of the study; H.Y Xu, M Cai, and C.K Wang were involved in the collection, management, analysis, and interpretation of the data.
Conflict of Interest
None declared.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xu, H., Cai, M. & Zhang, X. Effect of the blockade of the IL-23-Th17-IL-17A pathway on streptozotocin-induced diabetic retinopathy in rats. Graefes Arch Clin Exp Ophthalmol 253, 1485–1492 (2015). https://doi.org/10.1007/s00417-014-2842-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-014-2842-9