Abstract
Background
Keratoplasty may induce major spherical refractive error related to abnormal corneal radius of curvature (CRC).
Methods
Two hundred and thirty-eight consecutive eyes of 238 patients with clear graft and at least one postoperative Orbscan examination performed after suture removal (average follow-up time, 86 months) were retrospectively analyzed. Anterior lamellar keratoplasties (ALK group, n = 119) and penetrating keratoplasties (PK group, n = 119) were matched for preoperative diagnosis and lens status.
Results
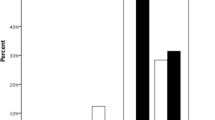
The average postoperative, suture-out, Orbscan 3-mm CRC was 7.17 mm with a wide 95 % confidence interval [6.26 mm; 8.37 mm]. It was 7.05 mm in the ALK group and 7.31 mm in the PK group (p < 0.01). In the ALK group, this figure was 7.00 mm for oversized grafts and 7.67 mm for non-oversized grafts (p < 0.001). CRC values were significantly lower for eyes with keratoconus (7.00 mm) or stromal scar after infectious keratitis (7.06 mm) compared with stromal scar after trauma (7.74 mm) or stromal dystrophies (8.17 mm). Values were significantly lower for big-bubble ALKs (6.92 mm) and manual dissection-ALKs (7.14 mm) compared with PKs (7.31 mm) and microkeratome-assisted ALKs (7.45 mm). The average Orbscan 3-mm SimK cylinder, irregularity, and refractive power symmetry index were, respectively, 4.7 D/4.8 D/1.9 D for ALKs and 5.2 D/4.8 D/1.8 D for PKs (p = 0.99).
Conclusions
The CRC is lower after ALK compared with PK, and features important variability. In eyes with ALK, non-oversized grafts result in postoperative CRC close to normal values and corneal diseases associated with stromal thinning and DALK result in lower postoperative CRC.




Similar content being viewed by others
References
Koo TS, Finkelstein E, Tan D, Mehta JS (2011) Incremental cost-utility analysis of deep anterior lamellar keratoplasty compared with penetrating keratoplasty for the treatment of keratoconus. Am J Ophthalmol 152:40–47
van den Biggelaar FJ, Cheng YY, Nuijts RM, Schouten JS, Wijdh RJ, Pels E, van Cleynenbreugel H, Eggink CA, Zaal MJ, Rijneveld WJ, Dirksen CD (2011) Economic evaluation of deep anterior lamellar keratoplasty versus penetrating keratoplasty in The Netherlands. Am J Ophthalmol 151:449–459
Reinhart WJ, Musch DC, Jacobs DS, Lee WB, Kaufman SC, Shtein RM (2011) Deep anterior lamellar keratoplasty as an alternative to penetrating keratoplasty a report by the American academy of ophthalmology. Ophthalmology 118:209–218
Shimazaki J, Shimmura S, Ishioka M, Tsubota K (2002) Randomized clinical trial of deep lamellar keratoplasty vs. penetrating keratoplasty. Am J Ophthalmol 134:159–165
Han DC, Mehta JS, Por YM, Htoon HM, Tan DT (2009) Comparison of outcomes of lamellar keratoplasty and penetrating keratoplasty in keratoconus. Am J Ophthalmol 148:744–751
Cheng YY, Visser N, Schouten JS, Wijdh RJ, Pels E, van Cleynenbreugel H, Eggink CA, Zaal MJ, Rijneveld WJ, Nuijts RM (2011) Endothelial cell loss and visual outcome of deep anterior lamellar keratoplasty versus penetrating keratoplasty: a randomized multicenter clinical trial. Ophthalmology 118:302–309
Borderie VM, Sandali O, Bullet J, Gaujoux T, Touzeau O, Laroche L (2012) Long-term results of deep anterior lamellar versus penetrating keratoplasty. Ophthalmology 119:249–255
Borderie VM, Guilbert E, Touzeau O, Laroche L (2011) Graft rejection and graft failure after anterior lamellar versus penetrating keratoplasty. Am J Ophthalmol 151:1024–1029
Borderie VM, Scheer S, Touzeau O, Vedie F, Carvajal-Gonzalez S, Laroche L (1998) Donor corneal tissue selection before penetrating keratoplasty. Br J Ophthalmol 82:382–388
Borderie VM, Touzeau O, Allouch C, Scheer S, Carvajal-Gonzalez S, Laroche L (1999) The results of successful penetrating keratoplasty using donor organ-cultured corneal tissue. Transplantation 67:1433–1438
Borderie VM, Werthel AL, Touzeau O, Allouch C, Boutboul S, Laroche L (2008) Comparison of techniques used for removing the recipient stroma in anterior lamellar keratoplasty. Arch Ophthalmol 126:31–37
Borderie VM, Laroche L (1996) Measurement of irregular astigmatism using semimeridian data from videokeratographs. J Refract Surg 12:595–600
Bland JM, Altman DG (1995) Multiple significance tests: the Bonferroni method. London. BMJ 310:170–170
Wiffen SJ, Maguire LJ, Bourne WM (1997) Keratometric results of penetrating keratoplasty with the Hessburg-Barron and Hanna trephine systems using a standard double-running suture technique. Cornea 16:306–313
Liu Z, Huang AJ, Pflugfelder SC (1999) Evaluation of corneal thickness and topography in normal eyes using the Orbscan corneal topography system. Br J Ophthalmol 83:774–778
Kim KH, Choi SH, Ahn K, Chung ES, Chung TY (2011) Comparison of refractive changes after deep anterior lamellar keratoplasty and penetrating keratoplasty for keratoconus. Jpn J Ophthalmol 55:93–97
Fontana L, Parente G, Tassinari G (2007) Clinical outcomes after deep anterior lamellar keratoplasty using the big-bubble technique in patients with keratoconus. Am J Ophthalmol 143:117–124
Javadi MA, Feizi S, Rastegarpour A (2011) Effect of vitreous length and trephine size disparity on post-DALK refractive status. Cornea 30:419–423
Sogutlu Sari E, Kubaloglu A, Unal M, Pinero Llorens D, Koytak A, Ofluoglu AN, Ozerturk Y (2012) Penetrating keratoplasty versus deep anterior lamellar keratoplasty: comparison of optical and visual quality outcomes. Br J Ophthalmol 96:1063–1067
Acar BT, Utine CA, Acar S, Ciftci F (2012) Laser in situ keratomileusis to manage refractive errors after deep anterior lamellar keratoplasty. J Cataract Refract Surg 38:1020–1027
Frost NA, Wu J, Lai TF, Coster DJ (2006) A review of randomized controlled trials of penetrating keratoplasty techniques. Ophthalmology 113:942–949
Touzeau O, Borderie VM, Allouch C, Scheer S, Laroche L (1999) Effects of penetrating keratoplasty suture removal on corneal topography and refraction. Cornea 18:638–644
Busin M, Zambianchi L, Arffa RC (2005) Microkeratome-assisted lamellar keratoplasty for the surgical treatment of keratoconus. Ophthalmology 112:987–997
Tuft SJ, Fitzke FW, Buckley RJ (1992) Myopia following penetrating keratoplasty for keratoconus. Br J Ophthalmol 1992:642–645
Randleman JB, Woodward M, Lynn MJ, Stulting RD (2008) Risk assessment for ectasia after corneal refractive surgery. Ophthalmology 115:37–50
Kaiserman I, Bahar I, Rootman DS (2008) Corneal wound malapposition after penetrating keratoplasty: an optical coherence tomography study. Br J Ophthalmol 92:1103–1107
Seitz B, Langenbucher A, Kuchle M, Naumann GO (2003) Impact of graft diameter on corneal power and the regularity of postkeratoplasty astigmatism before and after suture removal. Ophthalmology 110:2162–2167
Jaycock PD, Jones MN, Males J, Armitage WJ, Cook SD, Tole DM, Kaye SB (2008) Outcomes of same-sizing versus oversizing donor trephines in keratoconic patients undergoing first penetrating keratoplasty. Ophthalmology 115:268–275
Vajpayee RB, Dada T, Ray M, Tandon R, Sethi A, Turaka K (2001) Oversized corneal grafts for corneal opacities with iridocorneal adhesions. Ophthalmology 108:2026–2028
Völker-Dieben HJ, Kok-van Alphen CC, D'Amaro J, de Lange P (1982) Different influences on corneal graft survival in 539 transplants. Acta Ophthalmol (Copenh) 60:190–202
Touzeau O, Allouch C, Borderie V, Ameline B, Chastang P, Bouzegaou F, Laroche L (2001) Precision and reliability of Orbscan and ultrasonic pachymetry. J Fr Ophtalmol 24:912–921
Acknowledgments
Supported by Université Pierre et Marie Curie-Paris 6, Paris, France. The sponsor or funding organization had no role in the design or conduct of this research.
Conflict of interest
No conflicting relationship exists for any author.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Borderie, V.M., Georgeon, C., Borderie, M. et al. Corneal radius of curvature after anterior lamellar versus penetrating keratoplasty. Graefes Arch Clin Exp Ophthalmol 252, 449–456 (2014). https://doi.org/10.1007/s00417-013-2545-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-013-2545-7