Abstract
Background
To evaluate the perioperative complications and the outcomes of intraocular lens (IOL) exchange in patients with opacified lenses.
Methods
Retrospective multicentrical consecutive series of cases that comprised 22 eyes from 21 patients who had previous phacoemulsification with implantation of an IOL in the capsular bag and developed severe late opacification of the IOL. All patients had loss of vision and reported light disturbances. The IOLs were explanted and replaced with new IOLs. The perioperative complications were evaluated. The best spectacle-corrected visual acuity (BSCVA) before and after the surgery was compared.
Results
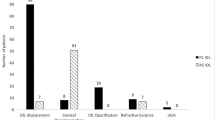
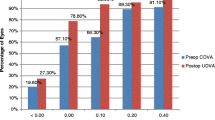
The mean time lapsed between the original cataract surgery and the IOL exchange surgery was 89.1 ± 33.6 [48–216] months. The IOL exchange was uneventful in 14 eyes (63.6 %). Anterior vitrectomy was needed in seven cases (31.8 %). Other complications included zonular dehiscence in one case (4.5 %). In most of the cases, 14 eyes (63.6 %), the IOL was implanted in the sulcus. The most explanted IOL was the Hydroview H60M (Bausch & Lomb). The mean BSCVA (LogMAR) before and after the surgery were 0.57 ± 0.69 (0.10–3) and 0.18 ± 0.22 (0.0–1.10) respectively (t paired test, p < 0.001). After the operation, 20 eyes (90.9 %) achieved a BSCVA ≤ 0.3. No eye lost 1 or more lines of corrected vision after the surgery.
Conclusions
IOL exchange surgery, although associated with a high incidence of complications, restores and significantly improves the visual acuity of patients with opacified IOLs.


Similar content being viewed by others
References
Chang BY, Davey KG, Gupta M, Hutchinson C (1999) Late clouding of an acrylic intraocular lens following routine phacoemulsification. Eye (Lond) 13(Pt 6):807–808
Sharma T, Chawdhary S (2001) The opalescence of hydrogel intraocular lens. Eye (Lond) 15:97–98
Apple DJ, Werner L, Pandey SK (2001) Newly recognized complications of posterior chamber intraocular lenses. Arch Ophthalmol 119:581–582
Werner L, Apple DJ, Kaskaloglu M, Pandey SK (2001) Dense opacification of the optical component of a hydrophilic acrylic intraocular lens: a clinicopathological analysis of 9 explanted lenses. J Cataract Refract Surg 27:1485–1492
Frohn A, Dick HB, Augustin AJ, Grus FH (2001) Late opacification of the foldable hydrophilic acrylic lens SC60B-OUV. Ophthalmology 108:1999–2004
Oner HE, Durak I, Saatci OA (2002) Late postoperative opacification of hydrophilic acrylic intraocular lenses. Ophthalmic Surg Lasers 33:304–308
Pandey SK, Werner L, Apple DJ, Kaskaloglu M (2002) Hydrophilic acrylic intraocular lens optic and haptics opacification in a diabetic patient: bilateral case report and clinicopathologic correlation. Ophthalmology 109:2042–2051
Mamalis N (2002) Complications of foldable intraocular lenses requiring explantation or secondary intervention—2001 survey update. J Cataract Refract Surg 28:2193–2201
Mamalis N, Davis B, Nilson CD, Hickman MS, Leboyer RM (2004) Complications of foldable intraocular lenses requiring explantation or secondary intervention—2003 survey update. J Cataract Refract Surg 30:2209–2218
Fernandez-Buenaga R, Alio JL, Munoz-Negrete FJ, Barraquer-Compte RI, Alio-Del Barrio JL (2012) Causes of IOL explantation in Spain. Eur J Ophthalmol 22:762–768
Werner L (2007) Causes of intraocular lens opacification or discoloration. J Cataract Refract Surg 33:713–726
Werner L, Apple DJ, Escobar-Gomez M, Ohrström A, Crayford BB, Bianchi R, Pandey SK (2000) Postoperative deposition of calcium on the surfaces of a hydrogel intraocular lens. Ophthalmology 107:2179–2185
Pandey SK, Werner L, Apple DJ, Gravel JP (2002) Calcium precipitation on the optical surfaces of a foldable intraocular lens: a clinicopathological correlation. Arch Ophthalmol 120:391–393
Tehrani M, Mamalis N, Wallin T, Dick HB, Stoffelns BM, Olson R, Fry LL, Clifford WS (2004) Late postoperative opacification of MemoryLens hydrophilic acrylic intraocular lenses: case series and review. J Cataract Refract Surg 30:115–122
Neuhann IM, Werner L, Izak AM, Pandey SK, Kleinmann G, Mamalis N, Neuhann TF, Apple DJ (2004) Late postoperative opacification of a hydrophilic acrylic (hydrogel) intraocular lens: a clinicopathological analysis of 106 explants. Ophthalmology 111:2094–2101
Werner L, Hunter B, Stevens S, Chew JJ, Mamalis N (2006) Role of silicon contamination on calcification of hydrophilic acrylic intraocular lenses. Am J Ophthalmol 141:35–43
Izak AM, Werner L, Pandey SK, Apple DJ (2003) Calcification of modern foldable hydrogel intraocular lens designs. Eye (Lond) 17:393–406
Werner L, Michelson J, Ollerton A, Leishman L, Bodnar Z (2012) Anterior segment optical coherence tomography in the assessment of postoperative intraocular lens optic changes. J Cataract Refract Surg 38:1077–1085
Michelson J, Werner L, Ollerton A, Leishman L, Bodnar Z (2012) Light scattering and light transmittance in intraocular lenses explanted because of optic opacification. J Cataract Refract Surg 38:1476–1485
Kodjikian L, Burillon C, Lina G, Roques C, Pellon G, Freney J, Renaud FN (2003) Biofilm formation on intraocular lenses by a clinical strain encoding the ica locus: a scanning electron microscopy study. Invest Ophthalmol Vis Sci 44:4382–4387
Mamalis N, Crandall AS, Pulsipher MW, Follet S, Monson MC (1991) Intraocular lens explantation and exchange. A review of lens styles, clinical indications, clinical results, and visual outcome. J Cataract Refract Surg 17:811–818
Doren GS, Stern GA, Driebe WT (1992) Indications for and results of intraocular lens explantation. J Cataract Refract Surg 18:79–85
Leaming DV (1999) Practice styles and preferences of ASCRS members—1998 survey. J Cataract Refract Surg 25:851–859
Leaming DV (2001) Practice styles and preferences of ASCRS members—2000 survey. American Society of Cataract and Refractive Surgery. J Cataract Refract Surg 27:948–955
Yu AK, Ng AS (2002) Complications and clinical outcomes of intraocular lens exchange in patients with calcified hydrogel lenses. J Cataract Refract Surg 28:1217–1222
Gashau AG, Anand A, Chawdhary S (2006) Hydrophilic acrylic intraocular lens exchange: five-year experience. J Cataract Refract Surg 32:1340–1344
Dagres E, Khan MA, Kyle GM, Clark D (2004) Perioperative complications of intraocular lens exchange in patients with opacified Aqua-Sense lenses. J Cataract Refract Surg 30:2569–2573
Dahlmann AH, Dhingra N, Chawdhary S (2002) Acrylic lens exchange for late opacification of the optic. J Cataract Refract Surg 28:1713–1714
Lee SJ, Choi JH, Sun HJ, Choi KS, Jung GY (2010) Surface calcification of hydrophilic acrylic intraocular lens related to inflammatory membrane formation after combined vitrectomy and cataract surgery. J Cataract Refract Surg 36:676–681
Dhital A, Spalton DJ, Goyal S, Werner L (2012) Calcification in hydrophilic intraocular lenses associated with injection of intraocular gas. Am J Ophthalmol 153:1154–1160
Saeed MU, Singh AJ, Morrell AJ (2006) Sequential Descemet’s membrane detachments and intraocular lens haze secondary to SF6 or C3F8. Eur J Ophthalmol 16:758–760
Acknowledgment
This study has been supported in part by a grant from the Spanish Ministry of Economy and Competitiviness, Instituto Carlos III, Red Temática de Investigación Cooperativa en Salud (RETICS) “Prevención, detección precoz y tratamiento de la patología ocular prevalente, degenerativa y crónica” Subprograma “dioptrio ocular y patologías frecuentes” (RD12/0034/0007).
The authors have no proprietary or commercial interest in the medical devices that are involved in this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
The study was approved by the Institutional Ethics Committee, and adhered to the Tenets of the Declaration of Helsinki (2008).
Rights and permissions
About this article
Cite this article
Fernández-Buenaga, R., Alió, J.L., Pinilla-Cortés, L. et al. Perioperative complications and clinical outcomes of intraocular lens exchange in patients with opacified lenses. Graefes Arch Clin Exp Ophthalmol 251, 2141–2146 (2013). https://doi.org/10.1007/s00417-013-2411-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-013-2411-7