Abstract
Background
To describe the demographics and outcomes of assault-related open-globe injuries (OGI) at University Hospital (UH), Newark, New Jersey over a ten-year period.
Methods
The medical records of all subjects presenting to a single university referral center with an OGI were retrospectively analyzed to identify prognostic factors for enucleation and final visual acuity (VA) of no light perception (NLP).
Results
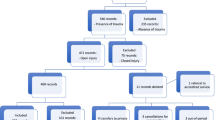
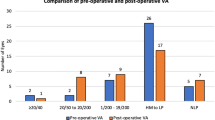
One hundred and forty-eight eyes of 147 patients presented to UH with assault-related OGI. Eighty-two percent of patients were male, and the mean age was 35.9 years. The anatomic site of the wound was zone 3 in the majority (54.1 %) of eyes. Most common type of injury noted was rupture (57.4 %), followed by penetrating injury (35.1 %). Mean initial presenting and final VA in LogMAR were 2.38 ± 0.12 and 2.18 ± 0.16 respectively. Initial Snellen VA was no light perception (NLP) in 57 eyes (38.5 %); four eyes had an initial VA of ≥20/40 (2.7 %). Final VA was NLP in 68 eyes (45.9 %) of which 46 were enucleated (31.1 %); 18 eyes (12.2 %) had a final VA of ≥20/40. Fifty eyes (33.8 %) underwent pars plana vitrectomy (PPV). Significant risk factors of final VA of NLP or enucleation included initial VA of NLP, perforating or rupture type of OGI, and zone 3 injury. Eyes that sustained penetrating injuries were less likely to have final VA of NLP or require enucleation.
Conclusions
Assault-related OGIs carry an extremely poor visual prognosis and a high rate of enucleations. Only eighteen eyes (12.2 %) recovered VA ≥20/40. We found initial VA of NLP and zone 3 injury to be significant predictors of final VA of NLP or undergoing enucleation. Penetrating injuries were less likely to have a final VA of NLP or an enucleation.

Similar content being viewed by others
References
Kuhn F, Morris R, Witherspoon CD, Heimann K, Jeffers JB, Treister G (1996) A standardized classification of ocular trauma. Graefes Arch Clin Exp Ophthalmol 234:399–403
Dannenberg AL, Parver LM, Fowler CJ (1992) Penetrating eye injuries related to assault. The National Eye Trauma System Registry. Arch Ophthalmol 110:849–852
Negrel AD, Thylefors B (1998) The global impact of eye injuries. Ophthalmic Epidemiol 5:143–169
United States Eye Injury Registry. Eye Trauma: Epidemiology and Prevention. Available at http://www.useironline.org/Prevention.htm. Last accessed June 1, 2012
Parver LM (1986) Eye trauma. The neglected disorder. Arch Ophthalmol 104:1452–1453
Esmaeli B, Elner SG, Schork MA, Elner VM (1995) Visual outcome and ocular survival after penetrating trauma. A clinicopathologic study. Ophthalmology 102:393–400
Thach AB, Johnson AJ, Carroll RB, Huchun A, Ainbinder DJ, Stutzman RD, Blaydon SM, Demartelaere SL, Mader TH, Slade CS, George RK, Ritchey JP, Barnes SD, Fannin LA (2008) Severe eye injuries in the war in Iraq, 2003–2005. Ophthalmology 115:377–382
Sobaci G, Mutlu FM, Bayer A, Karagul S, Yildirim E (2000) Deadly weapon-related open-globe injuries: outcome assessment by the ocular trauma classification system. Am J Ophthalmol 129:47–53
Casson RJ, Walker JC, Newland HS (2002) Four-year review of open eye injuries at the Royal Adelaide Hospital. Clin Exp Ophthalmol 30:15–18
Cruvinel Isaac DL, Ghanem VC, Nascimento MA, Torigoe M, Kara-Jose N (2003) Prognostic factors in open globe injuries. Ophthalmologica 217:431–435
May DR, Kuhn FP, Morris RE, Witherspoon CD, Danis RP, Matthews GP, Mann L (2000) The epidemiology of serious eye injuries from the United States Eye Injury Registry. Graefes Arch Clin Exp Ophthalmol 238:153–157
Liggett PE, Pince KJ, Barlow W, Ragen M, Ryan SJ (1990) Ocular trauma in an urban population. Review of 1132 cases. Ophthalmology 97:581–584
Vinger PF (1992) Eye injury resulting from violence. Research and prevention. Arch Ophthalmol 110:765–766
Mader TH, Carroll RD, Slade CS, George RK, Ritchey JP, Neville SP (2006) Ocular war injuries of the Iraqi Insurgency, January–September 2004. Ophthalmology 113:97–104
Weichel ED, Colyer MH (2008) Combat ocular trauma and systemic injury. Curr Opin Ophthalmol 19:519–525
Eagling EM (1976) Perforating injuries of the eye. Br J Ophthalmol 60:732–736
Gordon YJ, Mokete M (1981) Adult ocular injuries in Lesotho. Doc Ophthalmol 51:187–192
Groessl S, Nanda SK, Mieler WF (1993) Assault-related penetrating ocular injury. Am J Ophthalmol 116:26–33
Johnston S (1971) Perforating eye injuries: a five year survey. Trans Ophthalmol Soc U K 91:895–921
Lambah P (1969) Adult eye injuries at Wolverhampton. Trans Ophthalmol Soc U K 88:661–673
Landen D, Baker D, LaPorte R, Thoft RA (1990) Perforating eye injury in Allegheny County, Pennsylvania. Am J Public Health 80:1120–1122
Niiranen M (1981) Perforating eye injuries treated at Helsinki University Eye Hospital 1970 to 1977. Ann Ophthalmol 13:957–961
Punnonen E (1989) Epidemiological and social aspects of perforating eye injuries. Acta Ophthalmol (Copenh) 67(5):492–498
Roper-Hall MJ (1959) The treatment of ocular injuries. Trans Ophthalmol Soc U K 79:57–69
Rufer F, Peters A, Klettner A, Treumer F, Roider J (2010) Influence of alcohol consumption on incidence and severity of open-globe eye injuries in adults. Graefes Arch Clin Exp Ophthalmol 249:1765–1770
Scherf J, Zonis S (1976) Perforating injuries of the eye. Eye Ear Nose Throat Mon 55:32–40
Tielsch JM, Parver L, Shankar B (1989) Time trends in the incidence of hospitalized ocular trauma. Arch Ophthalmol 107:519–523
Kim JH, Yang SJ, Kim DS, Kim JG, Yoon YH (2007) Fourteen-year review of open globe injuries in an urban Korean population. J Trauma 62:746–749
Hyun Lee S, Ahn JK (2010) Emergent risk factors associated with eyeball loss and ambulatory vision loss after globe injuries. J Trauma 69:195–198
Rahman I, Maino A, Devadason D, Leatherbarrow B (2006) Open globe injuries: factors predictive of poor outcome. Eye 20:1336–1341
Colyer MH, Chun DW, Bower KS, Dick JS, Weichel ED (2008) Perforating globe injuries during operation Iraqi Freedom. Ophthalmology 115:2087–2093
Barak A, Elhalel A, Pikkel J, Krauss E, Miller B (2011) Incidence and severity of ocular and adnexal injuries during the Second Lebanon War among Israeli soldiers and civilians. Graefes Arch Clin Exp Ophthalmol 249(12):1771–1774
Rofail M, Lee GA, O’Rourke P (2006) Prognostic indicators for open globe injury. Clin Exp Ophthalmol 34:783–786
Hatton MP, Thakker MM, Ray S (2002) Orbital and adnexal trauma associated with open-globe injuries. Ophthal Plast Reconstr Surg 18:458–461
Babar TF, Khan MT, Marwat MZ, Shah SA, Murad Y, Khan MD (2007) Patterns of ocular trauma. J Coll Phys Surg Pak 17:148–153
Salehi-Had H, Andreoli CM, Andreoli MT, Kloek CE, Mukai S (2009) Visual outcomes of vitreoretinal surgery in eyes with severe open-globe injury presenting with no-light-perception vision. Graefes Arch Clin Exp Ophthalmol 247:477–483
Savar A, Andreoli MT, Kloek CE, Andreoli CM (2009) Enucleation for open globe injury. Am J Ophthalmol 147:595–600
Heidari E, Taheri N (2010) Surgical treatment of severely traumatized eyes with no light perception. Retina 30:294–299
Feng K, Hu YT, Ma Z (2011) Prognostic indicators for no light perception after open-globe injury: Eye Injury Vitrectomy Study. Am J Ophthalmol 152:654–662
Arroyo JG, Postel EA, Stone T, McCuen BW, Egan KM (2003) A matched study of primary scleral buckle placement during repair of posterior segment open globe injuries. Br J Ophthalmol 87:75–78
Kuhn F, Morris R, Witherspoon CD (2002) Birmingham Eye Trauma Terminology (BETT): terminology and classification of mechanical eye injuries. Ophthalmol Clin North Am 15:139–143
Pieramici DJ, Sternberg P Jr, Aaberg TM Sr, Bridges WZ Jr, Capone A Jr, Cardillo JA, De Juan E Jr, Kuhn F, Meredith TA, Mieler WF, Olsen TW, Rubsamen P, Stout T (1997) A system for classifying mechanical injuries of the eye (globe). The Ocular Trauma Classification Group. Am J Ophthalmol 123:820–831
Kuhn F, Maisiak R, Mann L, Mester V, Morris R, Witherspoon CD (2002) The Ocular Trauma Score (OTS). Ophthalmol Clin North Am 15:163–165
Koo L, Kapadia MK, Singh RP, Sheridan R, Hatton MP (2005) Gender differences in etiology and outcome of open globe injuries. J Trauma 59:175–178
Entezari M, Rabei HM, Badalabadi MM, Mohebbi M (2006) Visual outcome and ocular survival in open-globe injuries. Injury 37:633–637
Rao LG, Ninan A, Rao KA (2010) Descriptive study on ocular survival, visual outcome and prognostic factors in open globe injuries. Indian J Ophthalmol 58:321–323
Knyazer B, Levy J, Rosen S, Belfair N, Klemperer I, Lifshitz T (2008) Prognostic factors in posterior open globe injuries (zone-III injuries). Clin Exp Ophthalmol 36:836–841
Schmidt GW, Broman AT, Hindman HB, Grant MP (2008) Vision survival after open globe injury predicted by classification and regression tree analysis. Ophthalmology 115:202–209
Acknowledgments
The research in this project was supported by Research to Prevent Blindness, Inc., The New Jersey Lions Eye Research Foundation, and the Eye Institute of New Jersey.
The authors of this manuscript have no financial relationship with the organization that funded this research.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have full control of all primary data of this research, and agree to allow Graefe’s Clinical and Experimental Ophthalmology to review upon their request.
Rights and permissions
About this article
Cite this article
Bauza, A.M., Emami, P., Soni, N. et al. A 10-year review of assault-related open-globe injuries at an urban hospital. Graefes Arch Clin Exp Ophthalmol 251, 653–659 (2013). https://doi.org/10.1007/s00417-012-2136-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-012-2136-z