Abstract
Background
To evaluate femtosecond laser interaction with the applanation lens during pre-programmed penetrating keratoplasty corneal cuts.
Methods
Three different-shaped penetrating keratoplasty dissections were performed on edematous corneas from bank eyes using a clinical femtosecond laser system (Intralase FS60) with energies higher than 2 μJ, and the “depth into glass” parameter at 50 μm, which is defined as the length over which the laser interacts with the glass of the applanation cone in contact with the cornea. Additional full-thickness corneal incisions were obtained with an experimental laser source with technical characteristics similar to the clinical laser. Following cutting, tissue sections were examined by optical microscopy (OM), transmission electron microscopy (TEM), and electron energy loss spectroscopy (EELS). After the procedure, the cones were examined by optical and scanning electron microscopy (SEM). A control was obtained by repeating the procedures and stopping the laser at the cornea–lens interface.
Results
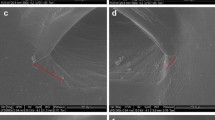
OM and TEM analysis of the tissue showed the presence of solid particles of a maximum dimension of 1.5 μm on the epithelium and the anterior stroma, regardless of the laser system used to cut. The EELS technique revealed their composition as silicon dioxide. We believe that the fragments originate from the applanation cone, which is machined by the laser interacting with the glass in contact with cornea. This is consistent with the structures observed on the lens by OM and SEM. Radial and circumferential tracks on the surface of the lens are visible, corresponding to the laser path in penetrating keratoplasty protocols. No particles were found in the control samples.
Conclusions
When performing penetrating keratoplasty corneal cuts by infra-red femtosecond laser, the applanation lens in contact with the cornea is machined by the laser depending on the system parameters. As a consequence, microscopic glass fragments are created, which may remain in the tissue. This unwanted effect can be avoided by stopping the procedure at the lens-cornea interface.





Similar content being viewed by others
References
Nordan LT, Slade SG, Baker RN, Suarez C, Juhasz T, Kurtz R (2003) Femtosecond laser flap creation for laser in situ keratomileusis: six-month follow-up of initial U.S. clinical series. J Refract Surg 19:8–14
Stonecipher K, Ignacio TS, Stonecipher M (2006) Advances in refractive surgery: microkeratome and femtosecond laser flap creation in relation to safety, efficacy, predictability, and biomechanical stability. Curr Opin Ophthalmol 17:368–372, doi:10.1097/01.icu.0000233957.88509.2d
Slade SG (2007) Applications for the femtosecond laser in corneal surgery. Curr Opin Ophthalmol 18:338–341, doi:10.1097/ICU.0b013e3281bd88b2
Durrie DS, Kezirian GM (2005) Femtosecond laser versus mechanical keratome flaps in wavefront-guided laser in situ keratomileusis: prospective contralateral eye study. J Cataract Refract Surg 31:120–126, doi:10.1016/j.jcrs.2004.09.046
Tran DB, Sarayba MA, Bor Z, Garufis C, Duh YJ, Soltes CR et al (2005) Randomized prospective clinical study comparing induced aberrations with IntraLase and Hansatome flap creation in fellow eyes: potential impact on wavefront-guided laser in situ keratomileusis. J Cataract Refract Surg 31:97–105, doi:10.1016/j.jcrs.2004.10.037
Steinert RF, Ignacio TS, Sarayba MA (2007) Top hat-shaped penetrating keratoplasty using the femtosecond laser. Am J Ophthalmol 143:689–691, doi:10.1016/j.ajo.2006.11.043
Seitz B, Brünner H, Viestenz A, Hofmann-Rummelt C, Schlötzer-Schrehardt U, Naumann GO et al (2005) Inverse mushroom-shaped nonmechanical penetrating keratoplasty using a femtosecond laser. Am J Ophthalmol 139:941–944, doi:10.1016/j.ajo.2004.11.028
Holzer MP, Rabsilber TM, Auffarth GU (2007) Penetrating keratoplasty using femtosecond laser. Am J Ophthalmol 143:524–526, doi:10.1016/j.ajo.2006.08.029
Buratto L, Bohm E (2007) The use of the femtosecond laser in penetrating keratoplasty. Am J Ophthalmol 143:737–742, doi:10.1016/j.ajo.2007.01.056
Seitz B, Langenbucher A, Hofmann-Rummelt C, Schlötzer-Schrehardt U, Naumann GO (2003) Nonmechanical posterior lamellar keratoplasty using the femtosecond laser (femto-plak) for corneal endothelial decompensation. Am J Ophthalmol 136:769–772, doi:10.1016/S0002–9394(03)00449–5
Sarayba MA, Juhasz T, Chuck RS, Ignacio TS, Nguyen TB, Sweet P et al (2005) Femtosecond laser posterior lamellar keratoplasty: a laboratory model. Cornea 24:328–333, doi:10.1097/01.ico.0000138830.50112.f4
Soong HK, Mian S, Abbasi O, Juhasz T (2005) Femtosecond laser-assisted posterior lamellar keratoplasty: initial studies of surgical technique in eye bank eyes. Ophthalmology 112:44–49, doi:10.1016/j.ophtha.2004.06.037
Mian SI, Soong HK, Patel SV, Ignacio T, Juhasz T (2006) In vivo femtosecond laser-assisted posterior lamellar keratoplasty in rabbits. Cornea 25:1205–1209, doi:10.1097/01.ico.0000231491.95377.0b
Vogel A, Noack J, Hüttman G, Paltauf G (2005) Mechanisms of femtosecond laser nanosurgery of cells and tissues. Appl Phys B 81:1015–1047, doi:10.1007/s00340–005–2036–6
Niemz MH, Hoppeler T, Juhasz T, Bille JF (1993) Threshold fluence measurements for plasma-mediated ablation in corneal tissue. Laser pulse duration was between 120 fs and 100 ps. Laser and light in ophthalmology 5:149–155
Stuart BC, Feit MD, Herman S, Rubenchik AM, Shore BW, Perry MD (1996) Nanosecond-to-femtosecond laser-induced breakdown in dielectrics. Phys Rev B 53:1749–1761, doi:10.1103/PhysRevB.53.1749
Giguère D, Olivié G, Vidal F, Toetsch S, Girard G, Ozaki T et al (2007) Laser ablation threshold dependence on pulse duration for fused silica and corneal tissue: experiments and modeling. J Opt Soc Am A Opt Image Sci Vis 24:1562–1568, doi:10.1364/JOSAA.24.001562
Vogel A, Venugopalan V (2003) Mechanisms of pulsed laser ablation of biological tissues. Chem Rev 103:577–644, doi:10.1021/cr010379n
Nuzzo V, Plamann K, Savoldelli M, Merano M, Donate D, Albert O et al (2007) In situ monitoring of second harmonic generation in human corneas to compensate for femtosecond laser pulse attenuation in keratoplasty. J Biomed Opt 12:064032. doi:10.1117/1.2811951
Arnold CL, Heisterkamp A, Ertmer W, Lubatschowski H (2005) Streak formation as side effect of optical breakdown during processing the bulk of transparent Kerr media with ultra-short laser pulses. Appl Phys B 80:247–253, doi:10.1007/s00340–004–1701–5
Tommila M, Jokinen J, Wilson T, Forsback AP, Saukko P, Penttinen R et al (2008) Bioactive glass-derived hydroxyapatite-coating promotes granulation tissue growth in subcutaneous cellulose implants in rats. Acta Biomater 4:354–361, doi:10.1016/j.actbio.2007.07.005
Belda JI, Artola A, Alió J (2003) Diffuse lamellar keratitis 6 months after uneventful laser in situ keratomileusis. J Refract Surg 19:70–71
Kymionis GD, Diakonis VF, Bouzoukis DI, Lampropoulou I, Pallikaris AI (2007) Idiopathic recurrence of diffuse lamellar keratitis after LASIK. J Refract Surg 23:720–721
Chung MS, Pepose JS, El-Agha MS, Cavanagh HD (2002) Confocal microscopic findings in a case of delayed-onset bilateral diffuse lamellar keratitis after laser in situ keratomileusis. J Cataract Refract Surg 28:1467–1470, doi:10.1016/S0886–3350(01)01353–0
Price FW Jr, Price MO (2008) Femtosecond laser shaped penetrating keratoplasty: one-year results utilizing a top-hat configuration. Am J Ophthalmol 145:210–214, doi:10.1016/j.ajo.2007.09.026
Gillette RL, Swaim SF, Sartin EA, Bradley DM, Coolman SL (2001) Effects of a bioactive glass on healing of closed skin wounds in dogs. Am J Vet Res 62:1149–1153, doi:10.2460/ajvr.2001.62.1149
Acknowledgements
We gratefully acknowledge Dr. Patrick Sabatier of the Banque Française des Yeux (French Eye Bank) for the supply of the human corneas.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have no financial interest in the article’s subject matter, materials or treatments mentioned. There is no outside source of financial support. Also, the authors have full control of all primary data and they agree to allow Graefe’s Archive for Clinical and Experimental Ophthalmology to review their data upon request.
Rights and permissions
About this article
Cite this article
Nuzzo, V., Plamann, K., Savoldelli, M. et al. Deposit of glass fragments during femtosecond laser penetrating keratoplasty. Graefes Arch Clin Exp Ophthalmol 247, 107–113 (2009). https://doi.org/10.1007/s00417-008-0948-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-008-0948-7