Abstract
Background
To assess the effectiveness of OloGen (also named iGen), a porous, bioengineered, biodegradable, collagen-glycoaminoglycan matrix implant, in preventing poor bleb formation and early failure after trabeculectomy in eyes with a surgical wound defect.
Methods
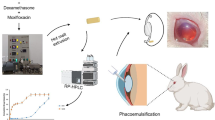
The right eyes of 30 female New Zealand albino rabbits underwent trabeculectomy with OloGen implanted subconjunctivally on top of the scleral flap, while six right eyes received trabeculectomy without the implant to serve as a control group. A 1–2 mm diameter circular conjunctival defect was created in all eyes. Six rabbits in the group receiving the implant were sacrificed on days 3, 5, 7, 21, and 28. Rabbits in the control group were sacrificed on day 28. Perkins applanation tonometry, Seidel test and measurement of both the extent of the conjunctival defect and the anterior chamber depth were performed. Enucleated eyes were fixed in 4% formaldehyde and stained with hematoxylin and eosin (H&E) for general histological observation, and with Sirius and Fast-green stains to assess collagen deposition and cell migration.
Results
Seidel tests were negative for all operated and control eyes. No flat anterior chamber occurred in either group. With the exception of days 5 and 7, post-operative mean IOP difference is significant in both groups, (P > 0.05 for day 5, 7 and P < 0.05 for day 3, 14, 21 and 28). In the implant group, the mean IOP was reduced by between 42% and 35% at days 14, 21, and 28, whereas the mean IOP in the control group was reduced by between only 12% and 2%. In the implant group, histology showed randomized collagen deposition and microcyst formation in the bleb after the matrix had degraded completely at day 28. In the control group, histology showed dense collagen deposition subconjunctivally at day 28.
Conclusions
OloGen successfully serves as a 3-dimensional scaffold for cell migration and proliferation, and can prevent failure by maintaining the size of the bleb in the presence of a large wound defect. It might also be successful at repairing postoperative bleb leaks.








Similar content being viewed by others
References
Young MJ, Borras T, Walter M, Ritch R (2005) Potential applications of tissue engineering to glaucoma. Arch Ophthalmol 123:1725–1731
Azuara-Blanco A, Katz LJ (1998) Dysfunctional filtering blebs. Surv Ophthalmol 43:93–126
Liebmann JM, Ritch R (1988) 5-Fluorouracil in glaucoma filtration surgery. Ophthalmol Clin N Amer 1:125–131
Ball SF (1988) Corticosteroids, including subconjunctival triamcinolone, in glaucoma filtration surgery. Ophthalmol Clin N Amer 1:143–156
Sugar HS (1965) Clinical effect of corticosteroids on conjunctival filtering blebs. Am J Ophthalmol 59:854–860
Cordeiro MF, Gay JA, Khaw PT (1999) Human anti-transforming growth factor antibody: a new glaucoma anti-scarring agent. Invest Ophthalmol Vis Sci 40:2225–2234
Barton K, Budenz DL, Khaw PT, Tseng SCG (2001) Glaucoma filtration surgery using amniotic membrane transplantation. Invest Ophthalmol Vis Sci 42:1762–1768
DeBry PW, Perkins TW, Heatley G, Kaufman P, Brumback LC (2002) Incidence of late-onset bleb-related complications following trabeculectomy with mitomycin. Arch Ophthalmol 120:297–300
Greenfield DS, Liebmann JM, Jee J, Ritch R (1998) Late-onset bleb leaks after glaucoma filtering surgery. Arch Ophthalmol 116:443–447
Soltau JB, Rothman R, Budenz DL, Greenfield DS, Feuer W, Liebmann JM, Ritch R (2000) Risk factors for glaucoma filtering bleb infections. Arch Ophthalmol 118:338–343
Chen HSL, Ritch R, Krupin T, Hsu WC (2006) Control of filtering bleb structure through tissue bioengineering: An animal model. Invest Ophthalmol Vis Sci 47:5310–5314
Broadway DC, Chang LP (2001) Trabeculectomy, risk factors for failure and the preoperative state of the conjunctiva. J Glaucoma 10:237–249
Broadway DC, Grierson I, Sturmer J, Hitchings RA (1996) Reversal of topical antiglaucoma medication effects on the conjunctiva. Arch Ophthalmol 114:262–267
Watson PG, Barnett F (1975) Effectiveness of trabeculectomy in glaucoma. Am J Ophthalmol 79:831–845
Budenz DL, Barton K, Tseng SCG (2000) Amniotic membrane transplantation for repair of leaking glaucoma filtering blebs. Am J Ophthalmol 130:580–588
Buxton JN, Lavery KT, Liebmann JM, Buxton DF, Ritch R (1994) Reconstruction of filtering blebs with free conjunctival autografts. Ophthalmology 101:635–639
Schnyder CC, Shaarawy T, Ravinet E et al (2002) Free conjunctival autologous graft for bleb repair and bleb reduction after trabeculectomy and nonpenetrating filtering surgery. J Glaucoma 11:10–16
Wilson MR, Kotas-Neumann R (1994) Free conjunctival patch for repair of persistent late bleb leak. Am J Ophthalmol 117:569–574
Burnstein AL, WuDunn D, Knotts SL, Catoira Y, Cantor LB (2002) Conjunctival advancement versus nonincisional treatment for late-onset glaucoma filtering bleb leaks. Ophthalmology 109:71–75
Blok MD, Kok JH, van Mil C, Greve EL, Kijlstra A (1990) A use of the megasoft bandage lens for treatment of complications after trabeculectomy. Am J Ophthalmol 110:264–268, Sep
Fourman S, Wiley L (1989) Use of a collagen shield to treat a glaucoma filter bleb leak. Am J Ophthalmol 107:673–674
Hsu WC, Yannas MHS IV, Rubin PA (2000) Inhibition of conjunctival scarring and contraction by a porous collagen-glycosaminoglycan implant. Invest Ophthalmol Vis Sci 41:2404–2411
Chang L, Crowston JG, Cordeiro MF, Akbar AN, Khaw PT (2000) The role of the immune system in conjunctival wound healing after glaucoma surgery. Surv Ophthalmol 45:49–68
Grinnell F (1994) Fibroblasts, myofibroblasts, and wound contraction. J Cell Biol 124:401–403
Kook MS, Lee DA (1995) Improving the success of glaucoma surgery by controlling wound healing. Ophthalmol Clin N Amer 8:393–400
Lieberman M, Ewing R (1990) Drainage implant surgery for refractory glaucoma. Int Ophthalmol Clin 19:802–810
Author information
Authors and Affiliations
Corresponding author
Additional information
Financial interest: Life Spring Biotech Co. Ltd has no financial relationship with any authors.
All authors have full control of all primary data, and agree to allow Graefe’s Archive for Clinical and Experimental Ophthalmology to review their data if requested.
Rights and permissions
About this article
Cite this article
Hsu, WC., Ritch, R., Krupin, T. et al. Tissue bioengineering for surgical bleb defects: an animal study. Graefes Arch Clin Exp Ophthalmol 246, 709–717 (2008). https://doi.org/10.1007/s00417-007-0744-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-007-0744-9