Abstract
Aims
To study the safety and effectiveness of a combination of both intravenous injection of lidocaine and intraocular pressure-lowering medications, in the intraocular pressure control and relief of symptoms of refractory acute primary angle-closure glaucoma (PACG).
Methods
Five consecutive patients with their first attack of acute PACG, with intraocular pressure ≥45 mmHg and a failure to release from the attack under antiglaucomatous medications for 4 hours, were recruited into the study. On presentation, each patient received topical pilocarpine and timolol, and systemic acetazolamide and mannitol as primary treatment. Then the patients accepted 2% lidocaine by intravenous injection at dose of 0.8 mg/kg in concert with antiglaucomatous medications. The intraocular pressures after intravenous injection at 30 minutes, and then at 1, 2, 4, 12, and 24 hours, were documented by applanation tonometry. Symptoms, visual acuity, intraocular pressure, corneal edema, angle status on gonioscopy, pupillary size, and reaction were also measured.
Results
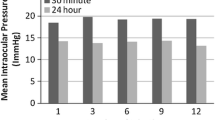
Six eyes of five patients seen with acute PACG were recruited. The mean intraocular pressure was reduced from 50.83 ± 5.34 mmHg to 39.5 ± 3.45 mmHg at 30 minutes after intravenous injection, and then to 33.3 ± 3.56 mmHg at 1 hour, and 24.55 ± 5.09 mmHg at 2 hours after intravenous injection. The mean intraocular pressure was less than 21 mmHg at 4 hours and beyond. There was instant symptomatic relief for all patients. No complications were encountered.
Conclusions
From this preliminary study, intravenous injection of lidocaine seems to be safe and effective in controlling intraocular pressure and eliminating symptoms in acute PACG. But the exact efficacy and safety need further investigation in large case studies.
Similar content being viewed by others
References
Robin AL, Pollack IP (1982) Argon laser peripheral iridotomies in the treatment of primary angle-closure glaucoma: long-term follow-up. Arch Ophthalmol 100:919–923
Airaksinen PJ, Saari KM, Tiainen TJ, Jaanio EAT (1979) Management of acute closed-angle glaucoma with miotics and timolol. Br J Ophthalmol 63:822–825
David R, Tessler Z, Yassur Y (1985) Long-term outcome of primary acute angle-closure glaucoma. Br J Ophthalmol 69:261–262
Markowitz SN, Morin JD (1984) The endothelium in primary angle-closure glaucoma. Am J Ophthalmol 98:103–104
Hart WM Jr, Becker B (1982) The onset and evolution of glaucomatous visual field defects. Ophthalmology 89:268–279
Bigar F, Witmer R (1982) Corneal endothelial changes in primary acute angle-closure glaucoma. Ophthalmology 89:596–599
Lam DSC, Chua JKH, Tham CCY, Lai JSM (2002) Efficacy and safety of immediate anterior chamber paracentesis in the treatment of acute primary angle-closure glaucoma. Ophthalmology 109:64–70
Ritch R (1982) Argon laser treatment for medically unresponsive attacks of angle-closure glaucoma. Am J Ophthalmol 94:197–204
Lev R, Rosen P (1994) Prophylactic lidocaine use preintubation: a review. J Emerg Med 12:499–506
Wang YM, Chung KC, Lu HF, Huang YW, Lin KC, Yang LC, Lin CR (2003) Lidocaine: the optimal timing of intravenous administration in attenuation of increase of intraocular pressure during tracheal intubation. Acta Anaesthesiol Sin 41:71–75
Lam DSC, Lai JSM, Tham CCY (1998) Immediate argon laser peripheral iridoplasty as treatment for acute attack of primary angle-closure glaucoma: a preliminary study. Ophthalmology 105:2231–2236
Lai JSM, Tham CCY, Lam DSC (1999) Limited argon laser peripheral iridoplasty as immediate treatment for an acute attack of primary angle closure glaucoma: a preliminary study. Eye 13:26–30
Tham CCY, Lai JSM, Lam DSC (1999) Immediate argon laser peripheral iridoplasty for acute attack of PACG (addendum of previous report) [letter]. Ophthalmology 106:1042–1043
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jin, X., Xue, A., Zhao, Y. et al. Efficacy and safety of intravenous injection of lidocaine in the treatment of acute primary angle-closure glaucoma: a pilot study. Graefes Arch Clin Exp Ophthalmol 245, 1611–1616 (2007). https://doi.org/10.1007/s00417-007-0572-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-007-0572-y