Abstract
Background
To present a method for performing photodynamic therapy (PDT) with a constant predictable light fluence based on actual laser spot magnification.
Methods
A calibrated Gullstrand-type model eye with a scale of half circles in the centre of the artificial fundus was used for this study. The axial length of the model eye was set to different values ranging from 20 to 31 mm, and the actual laser spot magnification of four indirect condensing laser lenses were determined using a PDT laser unit.
Results
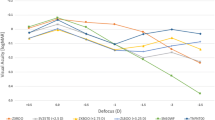
Equations for determining the actual laser spot magnification were calculated for each laser lens. The total change in laser spot magnification from hyperopia (axial length 20 mm) to myopia (axial length 31 mm) was −20% to +24.8% for Mainster Standard lens (Ocular Instruments Inc, Bellevue, Washington, USA), −15.7% to +27.7% for Mainster Wide Field lens (Ocular Instruments Inc), −16.3% to +33.1% for Volk Transequator lens (Volk Optical Inc, Mentor, Ohio, USA), and −19.2% to +24.4% for Volk PDT Laser lens (Volk Optical Inc).
Conclusions
Axial length of the eye has a considerable effect on PDT laser spot magnification when an indirect laser lens is used. By calculating the actual laser spot magnification in conjunction with knowledge of the true greatest linear dimension of the neovascular lesion, the clinician may be able to deliver a constant predictable amount of light fluence to the fundus independent of the axial length of the PDT treating eye.

Similar content being viewed by others
References
Age-Related Eye Disease Study Research Group (2000) Risk factors associated with age-related macular degeneration. A case-control study in the age-related eye disease study: Age-Related Eye Disease Study Report Number 3. Ophthalmology 107:2224–2232
Altman DG, Bland JM (1983) Measurement in medicine: the analysis of method comparison studies. Statistician 32:307–317
Ansari-Shahrezaei S, Stur M (2005) Magnification-corrected indirect biomicroscopy of the optic nerve head. Graefes Arch Clin Exp Ophthalmol 243:257–262
Ansari-Shahrezaei S, Ergun E, Stur M (2006) The effect of digital measurement software on photodynamic therapy. Graefes Arch Clin Exp Ophthalmol 244:137–142
Ansari-Shahrezaei S, Ergun E, Stur M (2006) The effect of axial length on photodynamic therapy. Am J Ophthalmol 141:699–702
Ansari-Shahrezaei S, Ergun E, Stur M (2006) Digital area measurement of fundus landmarks. Graefes Arch Clin Exp Ophthalmol 244:649–653
Bennett AG, Rudnicka AR, Edgar DF (1994) Improvements on Littmann’s method of determining the size of retinal features by fundus photography. Graefes Arch Clin Exp Ophthalmol 232:361–367
Fankhauser F, Durr U, Giger H, Rol P, Kwasniewska S (1996) Lasers, optical systems and safety in ophthalmology: a review. Graefes Arch Clin Exp Ophthalmol 234:473–487
Husain D, Gragoudas ES, Miller JW (1998) Photodynamic therapy. In: Berger JW, Fine SL, Maguire MG (eds) Age-Related Macular Degeneration. Mosby, St. Louis, pp 297–307
Husain D, Kramer M, Kenny AG, Michaud N, Flotte TJ, Gragoudas ES, Miller JW (1999) Effects of photodynamic therapy using verteporfin on experimental choroidal neovascularization and normal retina and choroid up to 7 weeks after treatment. Invest Ophthalmol Vis Sci 40:2322–2331
Kondo M, Ito Y, Miyata K, Kondo N, Ishikawa K, Terasaki H (2006) Effect of axial length on laser spot size during photodynamic therapy: an experimental study in monkeys. Am J Ophthalmol 141:214–215
Kramer M, Miller JW, Michaud N, Moulton RS, Hasan T, Flotte TJ, Gragoudas ES (1996) Liposomal benzoporphyrin derivative verteporfin photodynamic therapy: selective treatment of choroidal neovascularization in monkeys. Ophthalmology 103:427–438
Littmann H (1982) Determination of the real size of an object on the fundus of the living eye [in German]. Klin Mbl Augenheilk 180:286–289
Littmann H (1988) Determining the true size of an object on the fundus of the living eye [in German]. Klin Mbl Augenheilk 192:66–67
Michels S, Hansmann F, Geitzenauer W, Schmidt-Erfurth U (2006) Influence of treatment parameters on selectivity of verteporfin therapy. Invest Ophthalmol Vis Sci 47:371–376
Miller JW, Schmidt-Erfurth U, Sickenberg M, Pournaras CJ, Laqua H, Barbazetto I, Zografos L, Piguet B, Donati G, Lane AM, Birngruber R, van den Berg H, Strong A, Manjuris U, Gray T, Fsadni M, Bressler NM, Gragoudas ES (1999) Photodynamic therapy with verteporfin for choroidal neovascularization caused by age-related macular degeneration: results of a single treatment in a phase 1 and 2 study. Arch Ophthalmol 117:1161–1173
Rassow B (1972) A model of Gullstrand’s normal eye [in German]. Ophthalmologica 164:143–148
Reinke MH, Canakis C, Husain D, Michaud N, Flotte TJ, Gragoudas ES, Miller JW (1999) Verteporfin photodynamic therapy retreatment of normal retina and choroid in the cynomolgus monkey. Ophthalmology 106:1915–1923
Rudnicka AR, Burk RO, Edgar DF, Fitzke FW (1998) Magnification characteristics of fundus imaging systems. Ophthalmology 105:2186–2192
Sandberg MA, Tolentino MJ, Miller S, Berson EL, Gaudio AR (1993) Hyperopia and neovascularization in age-related macular degeneration. Ophthalmology 100:1009–1013
Schmidt-Erfurth U, Miller JW, Sickenberg M, Laqua H, Barbazetto I, Gragoudas ES, Zografos L, Piguet B, Pournaras CJ, Donati G, Lane AM, Birngruber R, van den Berg H, Strong HA, Manjuris U, Gray T, Fsadni M, Bressler NM (1999) Photodynamic therapy with verteporfin for choroidal neovascularization caused by age-related macular degeneration: results of retreatments in a phase 1 and 2 study. Arch Ophthalmol 117:1177–1187
Stur M, Ansari-Shahrezaei S (2001) The effect of axial length on laser spot size and laser irradiance. Arch Ophthalmol 119:1323–1328
Treatment of Age-Related Macular Degeneration with Photodynamic Therapy (TAP) Study Group (1999) Photodynamic therapy of subfoveal choroidal neovascularization in age-related macular degeneration with verteporfin: One-year results of 2 randomized clinical trials—TAP Report 1. Arch Ophthalmol 117:1329–1345
Treatment of Age-Related Macular Degeneration with Photodynamic Therapy (TAP) Study Group (2001) Photodynamic therapy of subfoveal choroidal neovascularization in age-related macular degeneration with verteporfin: Two-year results of 2 randomized clinical trials—TAP Report 2. Arch Ophthalmol 119:198–207
Visudyne in Minimally Classic Choroidal Neovascularization (VIM) Study Group (2005) Verteporfin therapy of subfoveal minimally classic choroidal neovascularization in age-related macular degeneration: 2-year results of a randomized clinical trial. Arch Ophthalmol 123:448–457
Acknowledgement
The authors thank Bernhard Rassow for providing the model eye.
Author information
Authors and Affiliations
Corresponding author
Additional information
No Grant/Financial Support.
The authors have no financial interest in any of the products discussed in this article.
Rights and permissions
About this article
Cite this article
Ansari-Shahrezaei, S., Ergun, E., Chong, R. et al. Magnification-corrected photodynamic therapy. Graefe's Arch Clin Exp Ophthalmol 245, 333–337 (2007). https://doi.org/10.1007/s00417-006-0419-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-006-0419-y