Abstract
Background
The non-contact specular microscope has become the method of choice for a quick, accurate and non-invasive assessment of central corneal thickness (CCT), which is an important variable to monitor before and after refractive surgery. The consistency of the results produced by such widely used methods/equipment must be assessed to determine their reliability. The purpose of this study was to assess within- and between-observer repeatability of, and to determine if a systematic bias exists in the measurements made by, the Topcon SP2000P specular microscope.
Methods
The CCT of the right eyes of 70 adult subjects, divided equally between men and women, was assessed on two separate occasions (4–7 days apart) by each of two examiners using the low-intensity auto mode of the SP2000P specular microscope.
Results
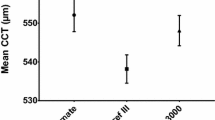
The average CCT values for men and women, measured by one observer, were 0.52±0.03 mm (mean ± SD) and 0.52±0.04 mm, respectively. The average for the entire sample was 0.52±0.04 mm. Within- and between-observer repeatability were assessed by plotting the mean difference (for each subject) between two readings made by the same observer or one each by both observers against the combined average CCT reading of both sessions; the mean difference between two sets of observations was not significantly different from zero (P<0.05). For the first observer, the 95% limits of repeatability were between −0.015 and 0.017 mm. For the second observer, the 95% limits of repeatability were between −0.018 and 0.018 mm. For the between-observer repeatability, the 95% limits of agreement were between −0.016 and 0.016 mm. For both within- and between-observer repeatability, we found no systematic bias of the mean difference with the average CCT reading.
Conclusion
The within- and between-observer limits of agreement we found were similar to those previously reported for the Topcon SP2000P specular microscope; the range of the 95% limits of repeatability were within ±1 SD of the average CCT reading for both sessions. We suggest that a technique be considered reliable if: (1) the mean difference between two measurements does not vary significantly from zero, (2) there is no systematic bias of the mean difference with the magnitude of the measured quantity and (3) the error inherent in a measurement technique is within ±1 SD of the average measurement of the two sessions.



Similar content being viewed by others
References
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Bovelle R, Kaufmann SC, Thompson HW, Hamano H (1999) Corneal thickness measurements with the Topcon SP-2000P specular microscope and an ultrasound pachymeter. Arch Ophthalmol 117:868–870
Cho P, Cheung SW (2000) Central and peripheral corneal thickness measured with the Topcon specular microscope SP-2000P. Curr Eye Res 21(4):799–807
Copt RP, Thomas R, Mermoud A (1999) Corneal thickness in ocular hypertension, primary open-angle glaucoma, and normal tension glaucoma. Arch Ophthalmol 106:2154–2160
De Paiva CS, Harris LD, Pflugfelder SC (2003) Keratoconus-like topographic changes in keratoconjunctivitis sicca. Cornea 22:22–24
Ehlers N, Bramsen T, Sperling S (1975) Applanation tonometry and central corneal thickness. Acta Ophthalmol (Copenh) 53:34–43
Guzey M, Satici A, Karadede S (2002) Corneal thickness in trachomatous dry eye. Eur J Ophthalmol 12:18–23
Insler MS, Baumann JD (1986) Corneal thinning syndromes. Ann Ophthalmol 18:74–75
Kawana K, Tokunaga T, Miyata K, Okamoto F, Kiuchi T, Oshika T (2004) Comparison of corneal thickness measurements using Orbscan II, non-contact specular microscopy, and ultrasonic pachymetry in eyes after laser in situ keratomileusis. Br J Ophthalmol 88:466–468
Lattimore MR Jr, Kaupp S, Schallhorn S, Lewis R IV (1999) Orbscan pachymetry: implications of a repeated measures and diurnal variation analysis. Ophthalmology 106:977–981
Liu Z, Pflugfelder SC (1999) Corneal thickness is reduced in dry eye. Cornea 18:403–407
Miglior S, Albe E, Guareschi M, Mandelli G, Gomarasca S, Orzalesi N (2004) Intraobserver and interobserver reproducibility in the evaluation of ultrasonic pachymetry measurements of central corneal thickness. Br J Ophthalmol 88:174–177
Modis L Jr, Langenbucher A, Seitz B (2001) Scanning-slit and specular microscopic pachymetry in comparison with ultrasonic determination of corneal thickness. Cornea 20:711–714
Portney LG, Watkins MP (2000) Statistical measures of reliability. Foundations of clinical research: applications to practice, 2nd edn. Appleton and Lange: New Jersey
Suzuki S, Oshika T, Oki K, Sakabe I, Iwase A, Amano S, Araie M (2004) Corneal thickness measurements: scanning-slit corneal topography and non-contact specular microscopy versus ultrasonic pachymetry. J Cataract Refract Surg 29:1313–1318
Tam ES, Rootman DS (2003) Comparison of central corneal thickness measurements by specular microscopy, ultrasound pachymetry, and ultrasound biomicroscopy. J Cataract Refract Surg 29:1179–1184
Vogt A (1920) Die Sichtbarkeit des lebenden Hornhautendothels; Ein Beitrag zur Methodik der Spaltleampenmikroskopie. Graefes Arch Clin Exp Ophthalmol 101:123–144
Waring GO III, Bourne WM, Edelhauser HF, Kenyon KR (1982) The corneal endothelium: normal and pathologic structure and function. Ophthalmology 89:531–590
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ogbuehi, K.C., Almubrad, T.M. Repeatability of central corneal thickness measurements measured with the Topcon SP2000P specular microscope. Graefe's Arch Clin Exp Ophthalmol 243, 798–802 (2005). https://doi.org/10.1007/s00417-005-1149-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-005-1149-2