Abstract
Background
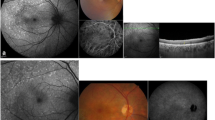
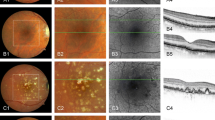
As members of the Fundus Autofluorescence in Age-related Macular Degeneration Study Group (FAM Study Group), we report changes of fundus autofluorescence (AF) in patients with multiple soft drusen in correlation to visual function.
Methods
Inclusion criteria were age >50 years, the presence of soft drusen, visual acuity of 20/100 or better, and no previous laser treatment in the study eye. All patients underwent a detailed ophthalmological examination including ETDRS visual acuity, binocular funduscopy, and color fundus photography. AF imaging was performed with a confocal scanning laser ophthalmoscope following a standard protocol. We used the classification of the International Fundus Autofluorescence Classification Group (IFAG) for the description of the AF patterns.
Results
One hundred and twenty-five patients (81 women, 44 men) aged from 55 to 86 years (mean 70±7 years) were included in this prospective study. During follow-up (mean 18±6 months), 6 of 35 eyes with patchy AF pattern developed exudative changes, as well as 2 eyes with focal–plaque-like AF pattern and 1 eye with reticular pattern at baseline. Geographic atrophy was seen in two eyes with focal AF pattern and one eye with focal–plaque-like pattern at baseline. A total of 11 eyes presented with severe visual loss (≧6 ETDRS lines). Ten (91%) of these had patchy AF pattern.
Conclusion
Imaging of fundus AF in patients with age-related maculopathy allows identification of different patterns of fundus AF. Our preliminary data suggest that a patchy pattern of AF indicates a relatively high risk of progression to age-related macular degeneration with visual loss.






Similar content being viewed by others
References
Bindewald A, Bird A, Dandekar S, Dolar-Szczasny J, Fitzke F, Einbock W, Holz F, Jorzik J, Keilhauer C, Mlynsk J, Staurenghi G, Wolf S (2004) Classification of fundus autofluorescence patterns early age-related macular degeneration (in press)
Bird AC (1991) Pathogenesis of retinal pigment epithelial detachment in the elderly; the relevance of Bruch’s membrane change. Eye 5:1–12
Bressler SB, Maguire MG, Bressler NM, Fine SL (1990) Relationship of drusen and abnormalities of the retinal pigment epithelium to the prognosis of neovascular macular degeneration. The Macular Photocoagulation Study Group. Arch Ophthalmol 108:1442–1447
Chen JC, Fitzke FW, Pauleikhoff D, Bird AC (1992) Functional loss in age-related Bruch’s membrane change with choroidal perfusion defect. Invest Ophthalmol Vis Sci 33:334–340
Delori FC (1994) Spectrophotometer for noninvasive measurement of intrinsic fluorescence and reflectance of the ocular fundus. Appl Opt 33:7439–7452
Delori FC, Dorey CK, Staurenghi G, Arend O, Gorger DG, Weiter JJ (1995a) In vivo fluorescence of the ocular fundus exhibits retinal pigment epithelium lipofuscin characteristics. Invest Ophthalmol Vis Sci 36:718–729
Delori FC, Staurenghi G, Arend O (1995b) In vivo measurement of lipofuscin in Stargardt’s disease. Invest Ophthalmol 36:2327–2331
Delori FC, Fleckner MR, Goger DG, Weiter JJ, Dorey CK (2000) Autofluorescence distribution associated with drusen in age-related macular degeneration. Invest Ophthalmol Vis Sci 41:496–504
Dorey CK, Staurenghi G, Delori FC (1993) Lipofuscin in aged and AMD eyes. Plenum, New York
Green WR, Enger C (1993) Age-related macular degeneration histopathologic studies. Ophthalmology 100:1519–1535
Holz FG, Wolfensberger TJ, Piquet B, Gross-Jendroska M, Wells JA, Minassian DC, Chisholm IH, Bird AC (1994) Bilateral macular drusen in age-related macular degeneration. Ophthalmology 101:1522–1528
Lois N, Halfyard AS, Bunce C, Bird AC, Fitzke FW (1999) Reproducibility of fundus autofluorescence measurements obtained using a confocal scanning laser ophthalmoscope. Br J Ophthalmol 83:276–279
Marmorstein AD, Marmorstein LY, Sakaguchi H, Hollyfield JG (2002) Spectral profiling of autofluorescence associated with lipofuscin, Bruch’s membrane, and sub-RPE deposits in normal and AMD eyes. Invest Ophthalmol Vis Sci 43:2435–2441
Okubo A, Rosa RH Jr, Bunce CV, Alexander RA, Fan JT, Bird AC, Luthert PJ (1999) The relationships of age changes in retinal pigment epithelium and Bruch’s membrane. Invest Ophthalmol Vis Sci 40:443–449
Pauleikhoff D, Barondes MJ, Minassian D, Chisholm IH, Bird AC (1990a) Drusen as risk factors in age related macular disease. Am J Ophthalmol 109:38–43
Pauleikhoff D, Chen JC, Chisholm IH, Bird AC (1990b) Choroidal perfusion abnormality with age-related Bruch’s membrane change. Am J Ophthalmol 109:211–217
Pauleikhoff D, Harper A, Marshall J, Bird AC (1990c) Aging changes in Bruch’s membrane. A histochemical and morphologic study. Ophthalmology 97:171–178
von Rückmann A, Fitzke FW, Bird AC (1995) Distribution of fundus autofluorescence with a scanning laser ophthalmoscope. Br J Ophthalmol 79:407–412
von Rückmann A, Fitzke FW, Bird A (1997a) Fundus autofluorescence in age-related macular disease imaged with a scanning laser ophthalmoscope. Invest Ophthalmol Vis Sci 38:478–486
von Rückmann A, Fitzke FW, Bird AC (1997b) In vivo fundus autofluorescence in macular dystrophies. Arch Ophthalmol 115:609–615
Sarks JP, Sarks SH, Killingsworth MC (1994) Evolution of soft drusen in age-related macular degeneration. Eye 8:269–283
Acknowledgement
Supported by DFG AZ Wo478/10-1.
Author information
Authors and Affiliations
Consortia
Corresponding author
Appendix
Appendix
Members of the Fundus Autofluorescence in Age-related Maculopathy Study Group (FAM Study Group) are:
-
University Eye Hospital Aachen (PI: A.Weinberger)
-
University Eye Hospital Bonn (PI: F. Holz)
-
University Eye Hospital Heidelberg: (PI: J. Jorzik)
-
University Eye Hospital Leipzig (PI: S. Wolf)
-
Eye department St. Franziskus Hospital Münster (PI: G. Spital)
-
University Eye Hospital Würzburg (PI: C. Keilhauer)
Rights and permissions
About this article
Cite this article
Einbock, W., Moessner, A., Schnurrbusch, U.E.K. et al. Changes in fundus autofluorescence in patients with age-related maculopathy. Correlation to visual function: a prospective study. Graefe's Arch Clin Exp Ophthalmol 243, 300–305 (2005). https://doi.org/10.1007/s00417-004-1027-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-004-1027-3