Abstract
Background and objective
Brain arteriovenous malformations (bAVMs) carry a risk of hemorrhage. We aim to identify factors associated with subsequent hemorrhages.
Methods
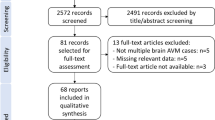
Systematic searches were conducted across the ScienceDirect, Medline, and Cochrane databases. Assessed risk factors included bAVM size, bAVM volume, hemorrhage and seizure presentations, presence of deep venous drainage, deep-seated bAVMs, associated aneurysms, and Spetzler–Martin grade. Subgroup analyses were conducted on prior treatments, hemorrhage presentation, AVM size, and type of management.
Results
The meta-analysis included 8 cohort studies and 2 trials, with 4,240 participants. Initial hemorrhage presentation (HR 2.41; 95% CI 1.94–2.98; p < 0.001), any deep venous drainage (HR 1.52; 95% CI 1.09–2.13; p = 0.01), and associated aneurysms (HR 1.78; 95% CI 1.41–2.23; p < 0.001) increased secondary hemorrhage risk. Conversely, higher Spetzler–Martin grades (HR 0.77; 95% CI 0.68–0.87; p < 0.001) and larger malformation volumes (HR 0.87; 95% CI 0.76–0.99; p = 0.04) reduced risk. Subgroups showed any deep venous drainage in patients without prior treatment (HR 1.64; 95% CI 1.25–2.15; p < 0.001), bAVM > 3 cm (HR 1.79; 95% CI 1.15–2.78; p = 0.01), and multimodal interventions (HR 1.69; 95% CI 1.12–2.53; p = 0.01) increased risk. The reverse effect was found for patients initially presented without hemorrhage (HR 0.79; 95% CI 0.67–0.93; p = 0.01). Deep bAVM was a risk factor in > 3 cm cases (HR 2.72; 95% CI 1.61–4.59; p < 0.001) and multimodal management (HR 2.77; 95% CI 1.66–4.56; p < 0.001). Kaplan–Meier analysis revealed increased hemorrhage risk for initial hemorrhage presentation, while cumulative survival was higher in intervened patients over 72 months.
Conclusion
Significant risk factors for bAVMs hemorrhage include initial hemorrhage, any deep venous drainage, and associated aneurysms. Deep venous drainage involvement is a risk factor in cases without prior treatment, those with bAVM > 3 cm, and cases managed with multimodal interventions. Deep bAVM involvement also emerges as a risk factor in cases > 3 cm and those managed with multimodal approaches.



Similar content being viewed by others
Data availability
All data relevant to the study are included in the article or uploaded as supplementary information.
Abbreviations
- ARUBA:
-
A Randomized Trial of Unruptured Brain Arteriovenous Malformations
- bAVM:
-
Brain arteriovenous malformation
- CI:
-
Confidence interval
- CT:
-
Computed tomography
- HRs:
-
Hazard ratios
- MRI:
-
Magnetic resonance imaging
- NOS:
-
Newcastle–Ottawa scale
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- PROSPERO:
-
International Prospective Register of Systematic Reviews
- REML:
-
Restricted maximum likelihood
- RCT:
-
Randomized controlled trial
- SIVMS:
-
Steering Committee and the Oxford Vascular Study
References
Ozpinar A, Mendez G, Abla AA (2017) Epidemiology, genetics, pathophysiology, and prognostic classifications of cerebral arteriovenous malformations. Handb Clin Neurol 143:5–13
Lawton MT, Rutledge WC, Kim H, Stapf C, Whitehead KJ, Li DY et al (2015) Brain arteriovenous malformations. Nat Rev Dis Primers 1:15008
Shaligram SS, Winkler E, Cooke D, Su H (2019) Risk factors for hemorrhage of brain arteriovenous malformation. CNS Neurosci Ther 25(10):1085–1095
Da Costa L, Wallace MC, Ter Brugge KG, O’Kelly C, Willinsky RA, Tymianski M (2009) The natural history and predictive features of hemorrhage from brain arteriovenous malformations. Stroke 40(1):100–105
Zuurbier SM, Al-Shahi SR (2019) Interventions for treating brain arteriovenous malformations in adults. Cochrane Database Syst Rev 9(9):CD003436
Pollock BE, Link MJ, Brown RD (2013) The risk of stroke or clinical impairment after stereotactic radiosurgery for ARUBA-eligible patients. Stroke 44(2):437–441
Mohr JP, Parides MK, Stapf C, Moquete E, Moy CS, Overbey JR et al (2014) Medical management with or without interventional therapy for unruptured brain arteriovenous malformations (ARUBA): A multicentre, non-blinded, randomised trial. The Lancet 383(9917):614–621
Ding D, Yen CP, Xu Z, Starke RM, Sheehan JP (2013) Radiosurgery for patients with unruptured intracranial arteriovenous malformations: Clinical article. J Neurosurg 118(5):958–966
Halim AX, Johnston SC, Singh V, McCulloch CE, Bennett JP, Achrol AS et al (2004) Longitudinal risk of intracranial hemorrhage in patients with arteriovenous malformation of the brain within a defined population. Stroke 35(7):1697–1702
Kim H, Sidney S, McCulloch CE, Poon KYT, Singh V, Johnston SC et al (2007) Racial/ethnic differences in longitudinal risk of intracranial hemorrhage in brain arteriovenous malformation patients. Stroke 38(9):2430–2437
Nerva JD, Barber J, Levitt MR, Rockhill JK, Hallam DK, Ghodke BV et al (2018) Onyx embolization prior to stereotactic radiosurgery for brain arteriovenous malformations: a single-center treatment algorithm. J Neurointerv Surg 10(3):258–267
Al-Shahi Salman R, White PM, Counsell CE, Du PJ, Van Beijnum J, Josephson CB et al (2014) Outcome after conservative management or intervention for unruptured brain arteriovenous malformations. JAMA 311(16):1661–1669
Al-Shahi R, Bhattacharya JJ, Currie DG, Papanastassiou V, Ritchie V, Roberts RC et al (2003) Scottish Intracranial Vascular Malformation Study (SIVMS): evaluation of methods, ICD-10 coding, and potential sources of bias in a prospective, population-based cohort. Stroke 34(5):1156–1162
Stapf C, Mast H, Sciacca RR, Choi JH, Khaw AV, Connolly ES, et al (2006) Predictors of hemorrhage in patients with untreated brain arteriovenous malformation [Internet]. Vol. 66, Neurology. www.neurology.org
Thenier-Villa JL, Galárraga-Campoverde RA, Martínez Rolán RM, De La Lama Zaragoza AR, Martínez Cueto P, Muñoz Garzón V et al (2017) Linear accelerator stereotactic radiosurgery of central nervous system arteriovenous malformations: a 15-year analysis of outcome-related factors in a single tertiary center. World Neurosurg 1(103):291–302
Yamada S, Takagi Y, Nozaki K, Kikuta KI, Hashimoto N (2007) Risk factors for subsequent hemorrhage in patients with cerebral arteriovenous malformations. J Neurosurg 107(5):965–972
Sterne J, Harbord R (2004) Funnel plots in meta-analysis. Stata J 1(4):127–141
Lv X, Hu X, Liu J, He H, Li Y (2016) The influence of age and the initial clinical presentations of patients with an arteriovenous malformation on the risk of hemorrhage. Neurol India 64(Suppl):S87-94
Ogilvy CS, Stieg PE, Awad I, Brown J, Kondziolka D, Rosenwasser R et al (2001) Recommendations for the management of intracranial arteriovenous malformations: A statement for healthcare professionals from a special writing group of the Stroke Council. American Stroke Association Circulation 103(21):2644–2657
Kim H, Al-Shahi Salman R, McCulloch CE, Stapf C, Young WL (2014) Untreated brain arteriovenous malformation: patient-level meta-analysis of hemorrhage predictors. Neurology 83(7):590–597
Tong X, Wu J, Lin F, Cao Y, Zhao Y, Wang S et al (2016) Risk factors for subsequent hemorrhage in patients with cerebellar arteriovenous malformations. World Neurosurg [Internet] 92:47–57. https://doi.org/10.1016/j.wneu.2016.04.082
Lin TM, Yang HC, Lee CC, Wu HM, Hu YS, Luo CB et al (2019) Stasis index from hemodynamic analysis using quantitative DSA correlates with hemorrhage of supratentorial arteriovenous malformation: a cross-sectional study. J Neurosurg 132(5):1574–1582
Chen Y, Chen P, Li R, Han H, Li Z, Ma L et al (2023) Rupture-related quantitative hemodynamics of the supratentorial arteriovenous malformation nidus. J Neurosurg 138(3):740–749
Zhu H, Liu L, Chang Y, Song Y, Liang S, Ma C et al (2023) Quantitative evaluation of the subsequent hemorrhage with arteriography-derived hemodynamic features in patients with untreated cerebral arteriovenous malformation. Front Neurol 14:1174245
Gross BA, Du R (2013) Natural history of cerebral arteriovenous malformations: a meta-analysis. J Neurosurg 118(2):437–443
Platz J, Berkefeld J, Singer OC, Wolff R, Seifert V, Konczalla J et al (2014) Frequency, risk of hemorrhage and treatment considerations for cerebral arteriovenous malformations with associated aneurysms. Acta Neurochir (Wien) 156(11):2025–2034
D’Aliberti G, Talamonti G, Cenzato M, La Camera A, Debernardi A, Valvassori L et al (2015) Arterial and venous aneurysms associated with arteriovenous malformations. World Neurosurg 83(2):188–196
Ryu B, Ishikawa T, Kawamata T (2017) Multimodal Treatment Strategy for Spetzler-Martin Grade III Arteriovenous Malformations of the Brain. Neurol Med Chir (Tokyo) 57(2):73–81
Padilla-Vazquez F, Zenteno MA, Balderrama J, Escobar-de la Garma VH, Juan DS, Trenado C (2017) A proposed classification for assessing rupture risk in patients with intracranial arteriovenous malformations. Surg Neurol Int 8:303
Tasic G, Jovanovic V, Djurovic B, Nikolic I, Janicijevic M, Samardzic M et al (2011) Natural course of the arteriovenous malformations of the brain initially presented by hemorrhage: analysis of a clinical series of 39 patients. Turk Neurosurg 21(3):280–289
Subat YW, Dasenbrock HH, Gross BA, Patel NJ, Frerichs KU, Du R, et al (2020) Periprocedural intracranial hemorrhage after embolization of cerebral arteriovenous malformations: a meta-analysis. J Neurosurg JNS [Internet] 133(5):1417–27. https://thejns.org/view/journals/j-neurosurg/133/5/article-p1417.xml
Feghali J, Huang J (2019) Updates in arteriovenous malformation management: the post-Aruba Era. Stroke Vasc Neurol. 5:34–39
Acknowledgements
The authors also acknowledge the contribution of the Department of Neurology, Universitas Udayana for the supports given.
Funding
The authors did not receive any grant or funding for this research from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
BGdL: acquisition of data, analysis and interpretation of data, wrote the first draft, study supervision. AAIKA: analysis and interpretation of data, wrote the first draft. CPK: wrote the first draft. NAKP: critical revision of manuscript for intellectual content. KT: critical revision of manuscript for intellectual content. IPEW: study concept and design, critical revision of manuscript for intellectual content. ISP: critical revision of manuscript for intellectual content. BGdL is the guarantor.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethics approval
Not applicable.
Consent for publication
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
de Liyis, B.G., Arini, A.A.I.K., Karuniamaya, C.P. et al. Risk of intracranial hemorrhage in brain arteriovenous malformations: a systematic review and meta-analysis. J Neurol 271, 2274–2284 (2024). https://doi.org/10.1007/s00415-024-12235-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-024-12235-1