Abstract
Background
Muscle weakness is a prominent feature of Parkinson’s disease, but whether the occurrence of this deficit in healthy adults is associated with subsequent PD diagnosis remains unclear.
Objective
This study sought to examine the relationship between muscle strength, represented by grip strength and walking pace, and the risk of incident PD.
Methods
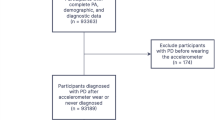
A total of 422,531 participants from the UK biobank were included in this study. Longitudinal associations of grip strength and walking pace with the risk of incident PD were investigated by Cox proportional hazard models adjusting for several well-established risk factors. Subgroup and sensitivity analyses were also conducted for further validation.
Results
After a median follow-up of 9.23 years, 2,118 (0.5%) individuals developed incident PD. For per 5 kg increment of absolute grip strength, there was a significant 10.2% reduction in the risk of incident PD (HR = 0.898, 95% CI [0.872–0.924], P < 0.001). Similarly, per 0.05 kg/kg increment of relative grip strength was related to a 9.2% reduced risk of incident PD (HR = 0.908, 95% CI [0.887–0.929], P < 0.001). Notably, the associations remained consistent when grip strength was calculated as quintiles. Moreover, participants with a slower walking pace demonstrated an elevated risk of incident PD (HR = 1.231, 95%CI [1.075–1.409], P = 0.003). Subgroup and sensitivity analyses further validated the robustness of the observed associations.
Conclusion
Our findings showed a negative association of grip strength and walking pace with the risk of incident PD independent of important confounding factors. These results hold potential implications for the early screening of people at high-risk of PD.




Similar content being viewed by others
Availability of data and materials
The data that support the findings of this study are available from the UK Biobank project site, subject to registration and application process. Further details can be found at https://www.ukbiobank.ac.uk.
References
Bloem BR, Okun MS, Klein C (2021) Parkinson’s disease. Lancet 397:2284–2303
Weber S, Mollenhauer B (2021) Prodromal Parkinson disease - time is brain. Nat Rev Neurol 17:329–330
Berg D, Crotty GF, Keavney JL, Schwarzschild MA, Simuni T, Tanner C (2022) Path to Parkinson disease prevention: conclusion and outlook. Neurology 99:76–83
Soysal P, Hurst C, Demurtas J, Firth J, Howden R, Yang L, Tully MA, Koyanagi A, Ilie PC, López-Sánchez GF, Schwingshackl L, Veronese N, Smith L (2021) Handgrip strength and health outcomes: umbrella review of systematic reviews with meta-analyses of observational studies. J Sport Health Sci 10:290–295
Choi J-Y, Kim K-I, Choi Y, Ahn S-H, Kang E, Oh H-K, Kim D-W, Kim E-K, Yoon Y-S, Kang S-B, Kim H-H, Han H-S, Kim C-H (2020) Comparison of multidimensional frailty score, grip strength, and gait speed in older surgical patients. J Cachexia Sarcopenia Muscle 11:432–440
Yates T, Zaccardi F, Dhalwani NN, Davies MJ, Bakrania K, Celis-Morales CA, Gill JMR, Franks PW, Khunti K (2017) Association of walking pace and handgrip strength with all-cause, cardiovascular, and cancer mortality: a UK Biobank observational study. Eur Heart J 38:3232–3240
Cabanas-Sánchez V, Esteban-Cornejo I, Parra-Soto S, Petermann-Rocha F, Gray SR, Rodríguez-Artalejo F, Ho FK, Pell JP, Martínez-Gómez D, Celis-Morales C (2022) Muscle strength and incidence of depression and anxiety: findings from the UK Biobank prospective cohort study. J Cachexia Sarcopenia Muscle 13:1983–1994
Duchowny KA, Ackley SF, Brenowitz WD, Wang J, Zimmerman SC, Caunca MR, Glymour MM (2022) Associations between handgrip strength and dementia risk, cognition, and neuroimaging outcomes in the UK biobank cohort study. JAMA Netw Open 5:e2218314
Fritz NE, McCarthy CJ, Adamo DE (2017) Handgrip strength as a means of monitoring progression of cognitive decline - a scoping review. Ageing Res Rev 35:112–123
He P, Zhou C, Ye Z, Liu M, Zhang Y, Wu Q, Zhang Y, Yang S, Xiaoqin G, Qin X (2023) Walking pace, handgrip strength, age, APOE genotypes, and new-onset dementia: the UK Biobank prospective cohort study. Alzheimers Res Ther 15:9
Kuo K, Zhang Y-R, Chen S-D, He X-Y, Huang S-Y, Wu B-S, Deng Y-T, Yang L, Ou Y-N, Guo Y, Zhang R-Q, Zhang Y, Tan L, Dong Q, Cheng W, Yu J-T (2022) Associations of grip strength, walking pace, and the risk of incident dementia: a prospective cohort study of 340212 participants. Alzheimers Dement. https://doi.org/10.1002/alz.12793
Abay RJY, Gold LS, Cawthon PM, Andrews JS (2022) Lean mass, grip strength, and hospital-associated disability among older adults in Health ABC. Alzheimers Dement 18:1898–1906
Oveisgharan S, Yu L, Agrawal S, Nag S, Bennett DA, Buchman AS, Schneider JA (2023) Relation of motor impairments to neuropathologic changes of limbic-predominant age-related TDP-43 encephalopathy in older adults. Neurology 101:e1542–e1553
Skillbäck T, Blennow K, Zetterberg H, Skoog J, Rydén L, Wetterberg H, Guo X, Sacuiu S, Mielke MM, Zettergren A, Skoog I, Kern S (2022) Slowing gait speed precedes cognitive decline by several years. Alzheimers Dement 18:1667–1676
Schrag A, Horsfall L, Walters K, Noyce A, Petersen I (2015) Prediagnostic presentations of Parkinson’s disease in primary care: a case-control study. Lancet Neurol 14:57–64
Fereshtehnejad S-M, Yao C, Pelletier A, Montplaisir JY, Gagnon J-F, Postuma RB (2019) Evolution of prodromal Parkinson’s disease and dementia with Lewy bodies: a prospective study. Brain 142:2051–2067
Maraki MI, Stefanis L, Yannakoulia M, Kosmidis MH, Xiromerisiou G, Dardiotis E, Hadjigeorgiou GM, Sakka P, Scarmeas N, Stamelou M (2019) Motor function and the probability of prodromal Parkinson’s disease in older adults. Mov Disord 34:1345–1353
Zheng Z, Lv Y, Rong S, Sun T, Chen L (2023) Physical Frailty, Genetic Predisposition, and Incident Parkinson Disease. JAMA Neurol 80:455–461
Gustafsson H, Aasly J, Stråhle S, Nordström A, Nordström P (2015) Low muscle strength in late adolescence and Parkinson disease later in life. Neurology 84:1862–1869
Ho FKW, Celis-Morales CA, Petermann-Rocha F, Sillars A, Welsh P, Welsh C, Anderson J, Lyall DM, Mackay DF, Sattar N, Gill JMR, Pell JP, Gray SR (2019) The association of grip strength with health outcomes does not differ if grip strength is used in absolute or relative terms: a prospective cohort study. Age Ageing 48:684–691
He P, Ye Z, Liu M, Li H, Zhang Y, Zhou C, Wu Q, Zhang Y, Yang S, Liu C, Qin X (2023) Association of handgrip strength and/or walking pace with incident chronic kidney disease: a UK biobank observational study. J Cachexia Sarcopenia Muscle 14:805–814
Kathryn Bush KR, Tim Wilkinson, Christian Schnier and Cathie Sudlow (March 2018) Definitions of Parkinson’s Disease and the Major Causes of Parkinsonism, UK Biobank Phase 1 Outcomes Adjudication.
Roberts HC, Syddall HE, Butchart JW, Stack EL, Cooper C, Sayer AA (2015) The association of grip strength with severity and duration of Parkinson’s: a cross-sectional study. Neurorehabil Neural Repair 29:889–896
Cruz-Jentoft AJ, Bahat G, Bauer J, Boirie Y, Bruyère O, Cederholm T, Cooper C, Landi F, Rolland Y, Sayer AA, Schneider SM, Sieber CC, Topinkova E, Vandewoude M, Visser M, Zamboni M (2019) Sarcopenia: revised European consensus on definition and diagnosis. Age Ageing 48:16–31
Paz TdSR, de Britto VLS, Yamaguchi B, Israel VL, Swarowsky A, Lourenço Correa C (2021) Hand function as predictor of motor symptom severity in individuals with Parkinson’s disease. Gerontology 67:160–167
Xie H, Ruan G, Deng L, Zhang H, Ge Y, Zhang Q, Lin S, Song M, Zhang X, Liu X, Li X, Zhang K, Yang M, Tang M, Hu W, Weng M, Shi H (2022) Comparison of absolute and relative handgrip strength to predict cancer prognosis: a prospective multicenter cohort study. Clin Nutr 41:1636–1643
Churilla JR, Summerlin M, Richardson MR, Boltz AJ (2020) Mean combined relative grip strength and metabolic syndrome: 2011–2014 national health and nutrition examination survey. J Strength Cond Res 34:995
Shimada H, Doi T, Lee S, Tsutsumimoto K, Bae S, Makino K, Nakakubo S, Arai H (2022) Identification of disability risk in addition to slow walking speed in older adults. Gerontology 68:625–634
Peterson DS, Horak FB (2016) Neural control of walking in people with Parkinsonism. Physiology (Bethesda) 31(2):95–107
Tansey MG, Wallings RL, Houser MC, Herrick MK, Keating CE, Joers V (2022) Inflammation and immune dysfunction in Parkinson disease. Nat Rev Immunol 22:657–673
Jankovic J, Tan EK (2020) Parkinson’s disease: etiopathogenesis and treatment. J Neurol Neurosurg Psychiatry 91:795–808
Müller J, Myers J (2018) Association between physical fitness, cardiovascular risk factors, and Parkinson’s disease. Eur J Prev Cardiol 25:1409–1415
Petzinger GM, Fisher BE, McEwen S, Beeler JA, Walsh JP, Jakowec MW (2013) Exercise-enhanced neuroplasticity targeting motor and cognitive circuitry in Parkinson’s disease. Lancet Neurol 12:716–726
Li G, Huang P, Cui S-S, Tan Y-Y, He Y-C, Shen X, Jiang Q-Y, Huang P, He G-Y, Li B-Y, Li Y-X, Xu J, Wang Z, Chen S-D (2022) Mechanisms of motor symptom improvement by long-term Tai Chi training in Parkinson’s disease patients. Transl Neurodegener 11:6
Rowlands AV, Dempsey PC, Maylor B, Razieh C, Zaccardi F, Davies MJ, Khunti K, Yates T (2023) Self-reported walking pace: A simple screening tool with lowest risk of all-cause mortality in those that “walk the talk.” J Sports Sci 41:333–341
Syddall HE, Westbury LD, Cooper C, Sayer AA (2015) Self-reported walking speed: a useful marker of physical performance among community-dwelling older people? J Am Med Dir Assoc 16:323–328
Keyes KM, Westreich D (2019) UK Biobank, big data, and the consequences of non-representativeness. Lancet 393:1297
Acknowledgements
This study utilized the UK Biobank Resource under application number 19542. We would like to thank all the participants and researchers from the UK Biobank.
Funding
This study was supported by grants from the Science and Technology Innovation 2030 Major Projects (2022ZD0211600), National Natural Science Foundation of China (82071201, 82271471), Shanghai Municipal Science and Technology Major Project (2018SHZDZX01), Research Start-up Fund of Huashan Hospital (2022QD002), Excellence 2025 Talent Cultivation Program at Fudan University (3030277001), Shanghai Talent Development Funding for The Project (2019074), Shanghai Rising-Star Program (21QA1408700), 111 Project (B18015), and ZHANGJIANG LAB, Tianqiao and Chrissy Chen Institute, the State Key Laboratory of Neurobiology and Frontiers Center for Brain Science of Ministry of Education, and Shanghai Center for Brain Science and Brain-Inspired Technology, Fudan University. The funding sources had no role in the design and conduct of the study; collection, analysis and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
JTY, WC and KK were responsible for the conception and design of the study. KMW and KK were responsible for acquisition, analysis of data, drafting of the manuscript and preparing the figures. YTD, LY, YRZ, and SDC were responsible for acquisition and analysis of data. LT, QD and JFF critically revised the manuscript and all authors approved the final version.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval and consent to participate
All participants gave written informed consent at baseline. Ethics approval for the UK biobank study was obtained from the NHS National Research Ethics Service (21/NW/0157).
Consent for publication
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, KM., Kuo, K., Deng, YT. et al. Association of grip strength and walking pace with the risk of incident Parkinson’s disease: a prospective cohort study of 422,531 participants. J Neurol 271, 2529–2538 (2024). https://doi.org/10.1007/s00415-024-12194-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-024-12194-7