Abstract
Background
Understanding sex disparities in stroke can identify gaps in clinical care. The objective of this study was to investigate whether sex differences could influence clinical outcomes of patients with acute vertebrobasilar artery occlusion (VBAO) who underwent endovascular therapy (EVT).
Methods
Patients were selected from the ANGEL-ACT Registry. The primary outcome was favorable functional outcome (90-day modified Rankin Scale [mRS] 0–3). Secondary outcomes included 90-day mRS distribution, excellent outcome (mRS 0–1), functional independence (mRS 0–2), early neurological improvement, recanalization, intracranial hemorrhage, and mortality within 90 days. The above outcomes were compared by two adjustment models, including (1) multivariable logistics analysis adjusting for all baseline and procedural variables with a P < 0.05; (2) adjusting for the propensity score.
Results
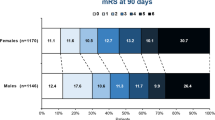
There were 347 acute VBAO patients treated with EVT included, of whom 72 (20.7%) were women and 275 (79.3%) were men. Women were older (72[63–76] vs. 62[53–69], P < 0.001) and had a higher rate of atrial fibrillation (31.9% vs. 8.7%, P < 0.001), lower rates of underlying intracranial atherosclerotic disease (30.6% vs. 51.3%, P = 0.007), and tandem occlusion (8.3% vs. 21.8%, P = 0.009) than men. The rate of favorable outcome (mRS 0–3) was similar between women and men (41.7% vs. 51.3%, adjusted odds ratio 1.56, 95%CI: 0.83–2.95, P = 0.171). There were no sex differences in other clinical outcomes (all P > 0.05).
Conclusions
In the ANGEL-ACT registry, the percentage of men with acute VBAO undergoing EVT was approximately fourfold higher than that of women with acute VBAO undergoing EVT. Sex differences did not modify the outcomes of acute VBAO after EVT.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Zi W, Qiu Z, Wu D, Li F, Liu H, Liu W, Huang W, Shi Z, Bai Y, Liu Z et al (2020) Assessment of endovascular treatment for acute basilar artery occlusion via a nationwide prospective registry. JAMA Neurol 77:561–573. https://doi.org/10.1001/jamaneurol.2020.0156
Haussen DC, Al-Bayati AR, Mohammaden MH, Sheth SA, Salazar-Marioni S, Linfante I, Dabus G, Starosciak AK, Hassan AE, Tekle WG et al (2022) The Society of Vascular and Interventional Neurology (SVIN) Mechanical Thrombectomy Registry: methods and primary results. Stroke Vasc Intervent Neurol. 2:e000234. https://doi.org/10.1161/SVIN.121.000234
Lee SJ, Hong JM, Kim JS, Lee JS (2022) Endovascular treatment for posterior circulation stroke: ways to maximize therapeutic efficacy. J Stroke 24:207–223. https://doi.org/10.5853/jos.2022.00941
Ospel JM, Schaafsma JD, Leslie-Mazwi TM, Amin-Hanjani S, Asdaghi N, Gordon-Perue GL, Couillard P, Hadidi NN, Bushnell C, McCullough LD et al (2022) Toward a better understanding of sex- and gender-related differences in endovascular stroke treatment: a Scientific Statement From the American Heart Association/American Stroke Association. Stroke 53:e396–e406. https://doi.org/10.1161/str.0000000000000411
Rexrode KM, Madsen TE, Yu AYX, Carcel C, Lichtman JH, Miller EC (2022) The impact of sex and gender on stroke. Circ Res 130:512–528. https://doi.org/10.1161/circresaha.121.319915
Jia B, Ren Z, Mokin M, Burgin WS, Bauer CT, Fiehler J, Mo D, Ma N, Gao F, Huo X et al (2021) Current status of endovascular treatment for acute large vessel occlusion in China: a real-world nationwide registry. Stroke 52:1203–1212. https://doi.org/10.1161/strokeaha.120.031869
Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, Marsh EE 3rd (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24:35–41. https://doi.org/10.1161/01.str.24.1.35
Liu X, Dai Q, Ye R, Zi W, Liu Y, Wang H, Zhu W, Ma M, Yin Q, Li M et al (2020) Endovascular treatment versus standard medical treatment for vertebrobasilar artery occlusion (BEST): an open-label, randomised controlled trial. Lancet Neurol 19:115–122. https://doi.org/10.1016/s1474-4422(19)30395-3
Langezaal LCM, van der Hoeven E, Mont’Alverne FJA, de Carvalho JJF, Lima FO, Dippel DWJ, van der Lugt A, Lo RTH, Boiten J, Lycklama À, Nijeholt GJ et al (2021) Endovascular therapy for stroke due to basilar-artery occlusion. N Engl J Med 384:1910–1920. https://doi.org/10.1056/NEJMoa2030297
Jovin TG, Li C, Wu L, Wu C, Chen J, Jiang C, Shi Z, Gao Z, Song C, Chen W et al (2022) Trial of thrombectomy 6 to 24 hours after stroke due to basilar-artery occlusion. N Engl J Med 387:1373–1384. https://doi.org/10.1056/NEJMoa2207576
Tao C, Nogueira RG, Zhu Y, Sun J, Han H, Yuan G, Wen C, Zhou P, Chen W, Zeng G et al (2022) Trial of endovascular treatment of acute basilar-artery occlusion. N Engl J Med 387:1361–1372. https://doi.org/10.1056/NEJMoa2206317
Tao C, Qureshi AI, Yin Y, Li J, Li R, Xu P, Sun J, Liao G, Yue X, Shi H et al (2022) Endovascular treatment versus best medical management in acute basilar artery occlusion strokes: results From the ATTENTION multicenter registry. Circulation 146:6–17. https://doi.org/10.1161/circulationaha.121.058544
Reid JM, Dai D, Gubitz GJ, Kapral MK, Christian C, Phillips SJ (2008) Gender differences in stroke examined in a 10-year cohort of patients admitted to a Canadian teaching hospital. Stroke 39:1090–1095. https://doi.org/10.1161/strokeaha.107.495143
Reeves MJ, Prager M, Fang J, Stamplecoski M, Kapral MK (2014) Impact of living alone on the care and outcomes of patients with acute stroke. Stroke 45:3083–3085. https://doi.org/10.1161/strokeaha.114.006520
Di Carlo A, Lamassa M, Baldereschi M, Pracucci G, Basile AM, Wolfe CD, Giroud M, Rudd A, Ghetti A, Inzitari D (2003) Sex differences in the clinical presentation, resource use, and 3-month outcome of acute stroke in Europe: data from a multicenter multinational hospital-based registry. Stroke 34:1114–1119. https://doi.org/10.1161/01.Str.0000068410.07397.D7
Niewada M, Kobayashi A, Sandercock PA, Kamiński B, Członkowska A (2005) Influence of gender on baseline features and clinical outcomes among 17,370 patients with confirmed ischaemic stroke in the international stroke trial. Neuroepidemiology 24:123–128. https://doi.org/10.1159/000082999
Willers C, Lekander I, Ekstrand E, Lilja M, Pessah-Rasmussen H, Sunnerhagen KS, von Euler M (2018) Sex as predictor for achieved health outcomes and received care in ischemic stroke and intracerebral hemorrhage: a register-based study. Biol Sex Differ 9:11. https://doi.org/10.1186/s13293-018-0170-1
Tan BYQ, Siow I, Lee KS, Chen V, Ong N, Gopinathan A, Yang C, Bhogal P, Lam E, Spooner O et al (2022) Effect of sex on outcomes of mechanical thrombectomy in basilar artery occlusion: a multicentre cohort study. Cerebrovasc Dis 51:639–646. https://doi.org/10.1159/000524048
Ciardi C, Cirio JJ, Scrivano EV, Bleise CD, Lylyk I, Lylyk P (2020) Sex-related differences after endovascular treatment of acute ischemic stroke in the “Real World.” J Stroke Cerebrovasc Dis 29:105240. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.105240
Bala F, Casetta I, Nannoni S, Herlihy D, Goyal M, Fainardi E, Michel P, Thornton J, Power S, Saia V et al (2022) Sex-related differences in outcomes after endovascular treatment of patients with late-window stroke. Stroke 53:311–318. https://doi.org/10.1161/strokeaha.121.037127
Sheth SA, Lee S, Warach SJ, Gralla J, Jahan R, Goyal M, Nogueira RG, Zaidat OO, Pereira VM, Siddiqui A et al (2019) Sex differences in outcome after endovascular stroke therapy for acute ischemic stroke. Stroke 50:2420–2427. https://doi.org/10.1161/strokeaha.118.023867
Deb-Chatterji M, Schlemm E, Flottmann F, Meyer L, Alegiani A, Brekenfeld C, Fiehler J, Gerloff C, Thomalla G (2021) Sex differences in outcome after thrombectomy for acute ischemic stroke are explained by confounding factors. Clin Neuroradiol 31:1101–1109. https://doi.org/10.1007/s00062-020-00983-2
Zerna C, Rogers E, Rabi DM, Demchuk AM, Kamal N, Mann B, Jeerakathil T, Buck B, Shuaib A, Rempel J et al (2021) Sex differences in endovascular treatment for stroke: a population-based analysis. Can J Neurol Sci 48:479–486. https://doi.org/10.1017/cjn.2020.237
Regenhardt RW, Turner AC, Hirsch JA, Young MJ, Alotaibi NM, Stapleton CJ, Patel AB, Leslie-Mazwi TM, Rost NS, Etherton MR (2022) Sex-specific differences in presentations and determinants of outcomes after endovascular thrombectomy for large vessel occlusion stroke. J Neurol 269:307–315. https://doi.org/10.1007/s00415-021-10628-0
Chalos V, de Ridder IR, Lingsma HF, Brown S, van Oostenbrugge RJ, Goyal M, Campbell BCV, Muir KW, Guillemin F, Bracard S et al (2019) Does sex modify the effect of endovascular treatment for ischemic stroke? Stroke 50:2413–2419. https://doi.org/10.1161/strokeaha.118.023743
Carvalho A, Cunha A, Gregório T, Paredes L, Costa H, Veloso M, Castro S, Ribeiro M, Barros PJG (2018) Is the efficacy of endovascular treatment for acute ischemic stroke sex-related. Interv Neurol 7:42–47. https://doi.org/10.1159/000484098
Sun D, Raynald X, Huo X, Jia B, Tong X, Ma G, Wang A, Ma N, Gao F, Mo D et al (2023) Sex-related differences in outcomes of endovascular treatment for anterior circulation large vessel occlusion. Stroke 54:327–336. https://doi.org/10.1161/strokeaha.122.041195
Zhang P, Li H, Wang J, Zhang F, Xiao L, Fang Y, Yan D, Xu G, Liu C, Huang Z et al (2023) Sex differences in outcomes after endovascular treatment of patients with vertebrobasilar artery occlusion. Eur Stroke J 8:566–574. https://doi.org/10.1177/23969873221151142
Phan HT, Blizzard CL, Reeves MJ, Thrift AG, Cadilhac DA, Sturm J, Heeley E, Otahal P, Vemmos K, Anderson C et al (2018) Factors contributing to sex differences in functional outcomes and participation after stroke. Neurology 90:e1945–e1953. https://doi.org/10.1212/wnl.0000000000005602
Klein P, Herning A, Drumm B, Raymond J, Abdalkader M, Siegler JE, Chen Y, Huo X, Schonewille WJ, Liu X, et al. Basilar artery occlusion thrombectomy technique: an international survey of practice patterns. Stroke Vasc Intervent Neurol 1:e000642. https://doi.org/10.1161/SVIN.122.000642
Pérez-Sánchez S, Barragán-Prieto A, Ortega-Quintanilla J, Domínguez-Mayoral A, Gamero-García M, Zapata-Arriaza E, Torres-Chacón R, de Albóniga-Chindurza A, Zapata-Hidalgo M, Moniche F et al (2020) Sex differences by hospital-level in performance and outcomes of endovascular treatment for acute ischemic stroke. J Stroke 22:258–261. https://doi.org/10.5853/jos.2019.03223
Lagebrant C, Ramgren B, Hassani Espili A, Marañon A, Kremer C (2022) Sex differences in collateral circulation and outcome after mechanical thrombectomy in acute ischemic stroke. Front Neurol 13:878759. https://doi.org/10.3389/fneur.2022.878759
Dula AN, Mlynash M, Zuck ND, Albers GW, Warach SJ (2020) Neuroimaging in ischemic stroke is different between men and women in the DEFUSE 3 cohort. Stroke 51:481–488. https://doi.org/10.1161/strokeaha.119.028205
Huo X, Klein P, Raynald X, Drumm B, Chen Y, Qureshi MM, Schonewille WJ, Liu X, Hu W, Ji X et al (2022) Perceptions on basilar artery occlusion management in China versus other countries: analysis of the after the BEST of BASICS (ABBA) survey. J Stroke Cerebrovasc Dis 31:106804. https://doi.org/10.1016/j.jstrokecerebrovasdis.2022.106804
Acknowledgements
The authors thank all clinicians, statisticians, and imaging and laboratory technologists who were involved in the ANGEL-ACT registry.
Funding
The ANGEL-ACT registry was funded by the National Key Research and Development Program of China, Grant number 2016YFC1301500.
Author information
Authors and Affiliations
Consortia
Contributions
ZM, XH, and DS were involved in the study conception. Statistical analysis was done by AW. The article was drafted by DS. All the authors reviewed and approved the final article.
Corresponding authors
Ethics declarations
Conflicts of interest
Dr. Nguyen reports research support from Medtronic and the Society of Vascular and Interventional Neurology (unrelated). Other authors have no conflict of interest.
Ethics approval
The study was approved by the ethics committees of Beijing Tiantan Hospital and all participating centers. The ID of the approval is KY2017-048-01. Subjects or their legally authorized representatives provided written informed consent prior to commencing the study.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Huo, X., Sun, D., Raynald et al. Sex differences in outcomes of endovascular therapy for acute vertebrobasilar occlusion: data from ANGEL-ACT Registry. J Neurol 271, 1376–1384 (2024). https://doi.org/10.1007/s00415-023-12078-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-023-12078-2