Abstract
Introduction
Strong evidence suggests that olfactory dysfunction (OD) can predict additional neurocognitive decline in neurodegenerative conditions such as Alzheimer’s and Parkinson’s diseases. However, research exploring olfaction and cognition in younger populations is limited. The aim of this review is to evaluate cognitive changes among non-elderly adults with non-COVID-19-related OD.
Methods
We performed a structured comprehensive literature search of PubMed, Ovid Embase, Web of Science, and Cochrane Library in developing this scoping review. The primary outcome of interest was the association between OD and cognitive functioning in adults less than 60 years of age.
Results
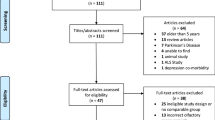
We identified 2878 studies for title and abstract review, with 167 undergoing full text review, and 54 selected for data extraction. Of these, 34 studies reported on populations of individuals restricted to the ages of 18–60, whereas the remaining 20 studies included a more heterogeneous population with the majority of individuals in this target age range in addition to some above the age of 60. The etiologies for smell loss among the included studies were neuropsychiatric disorders (37%), idiopathic cause (25%), type 2 diabetes (7%), trauma (5%), infection (4%), intellectual disability (4%), and other (18%). Some studies reported numerous associations and at times mixed, resulting in a total number of associations greater than the included number of 54 studies. Overall, 21/54 studies demonstrated a positive association between olfaction and cognition, 7/54 demonstrated no association, 25/54 reported mixed results, and only 1/54 demonstrated a negative association.
Conclusion
Most studies demonstrate a positive correlation between OD and cognition, but the data are mixed with associations less robust in this young adult population compared to elderly adults. Despite the heterogeneity in study populations and outcomes, this scoping review serves as a starting point for further investigation on this topic. Notably, as many studies in this review involved disorders that may have confounding effects on both olfaction and cognition, future research should control for these confounders and incorporate non-elderly individuals with non-psychiatric causes of smell loss.


Similar content being viewed by others
Data availability
The data that support the findings of this study are openly available within the references listed, which were accessed through the databases listed in the methods section.
References
Nordin S, Brämerson A (2008) Complaints of olfactory disorders: epidemiology, assessment and clinical implications. Curr Opin Allergy Clin Immunol 8(1):10–15
Desiato VM, Levy DA, Byun YJ et al (2021) The prevalence of olfactory dysfunction in the general population: a systematic review and meta-analysis. Am J Rhinol Allergy 35:195–205. https://doi.org/10.1177/1945892420946254
Yang J, Pinto JM (2016) The epidemiology of olfactory disorders. Curr Otorhinolaryngol Rep 4:130–141
Croy I, Nordin S, Hummel T (2014) Olfactory disorders and quality of life—an updated review. Chem Senses. https://doi.org/10.1093/chemse/bjt072
Rahayel S, Frasnelli J, Joubert S (2012) The effect of Alzheimer’s disease and Parkinson’s disease on olfaction: a meta-analysis. Behav Brain Res 231:60–74. https://doi.org/10.1016/j.bbr.2012.02.047
Sui X, Zhou C, Li J et al (2019) Hyposmia as a predictive marker of Parkinson’s disease: a systematic review and meta-analysis. Biomed Res Int 2019:1
Kotecha AM, Corrêa ADC, Fisher KM, Rushworth JV (2018) Olfactory dysfunction as a global biomarker for sniffing out Alzheimer’s disease: a meta-analysis. Biosensors (Basel). https://doi.org/10.3390/bios8020041
Lafaille-Magnan M-E, Poirier J, Etienne P et al (2017) Odor identification as a biomarker of preclinical AD in older adults at risk From the Centre for Studies on Prevention of AD
Marin C, Vilas D, Langdon C et al (2018) Olfactory dysfunction in neurodegenerative diseases. Curr Allergy Asthma Rep 18:1
Yan Y, Aierken A, Wang C et al (2022) A potential biomarker of preclinical Alzheimer’s disease: the olfactory dysfunction and its pathogenesis-based neural circuitry impairments. Neurosci Biobehav Rev 132:857–869
Wilson RS, Arnold SE, Schneider JA et al (2007) The relationship between cerebral Alzheimer’s disease pathology and odour identification in old age. J Neurol Neurosurg Psychiatry 78:30–35. https://doi.org/10.1136/jnnp.2006.099721
Doty RL (2017) Olfactory dysfunction in neurodegenerative diseases: Is there a common pathological substrate? Lancet Neurol 16(6):478–488
Moberg PJ, Kamath V, Marchetto DM et al (2014) Meta-analysis of olfactory function in schizophrenia, first-degree family members, and youths at-risk for psychosis. Schizophr Bull 40:50–59. https://doi.org/10.1093/schbul/sbt049
Langa KM, Levine DA (2014) The diagnosis and management of mild cognitive impairment: a clinical review. JAMA J Am Med Assoc 312:2551–2561
Oleszkiewicz A, Schriever VA, Croy I et al (2019) Updated Sniffin’ Sticks normative data based on an extended sample of 9139 subjects. Eur Arch Otorhinolaryngol 276:719–728. https://doi.org/10.1007/s00405-018-5248-1
Devanand DP, Tabert MH, Cuasay K et al (2010) Olfactory identification deficits and MCI in a multi-ethnic elderly community sample. Neurobiol Aging 31:1593–1600. https://doi.org/10.1016/j.neurobiolaging.2008.09.008
Roberts RO, Christianson TJH, Kremers WK et al (2016) Association between olfactory dysfunction and amnestic mild cognitive impairment and Alzheimer disease dementia. JAMA Neurol 73:93–101. https://doi.org/10.1001/jamaneurol.2015.2952
Devanand D, Michaels-Marston KS, Xinhua Liu M et al (2000) Olfactory deficits in patients with mild cognitive impairment predict Alzheimer’s disease at follow-up. Am J Psychiatry 157:1399–1405
Tricco AC, Lillie E, Zarin W et al (2018) PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med 169:467–473. https://doi.org/10.7326/M18-0850
Kwak SG, Kim JH (2017) Central limit theorem: the cornerstone of modern statistics. Korean J Anesthesiol 70:144–156. https://doi.org/10.4097/kjae.2017.70.2.144
Park H, Kim H, Kim S, Cha H (2021) The association between olfactory function and cognitive impairment in older persons with cognitive impairments: a cross-sectional study. Healthcare (Switzerland). https://doi.org/10.3390/healthcare9040399
Su B, Bleier B, Wei Y, Wu D (2021) Clinical implications of psychophysical olfactory testing: assessment, diagnosis, and treatment outcome. Front Neurosci. https://doi.org/10.3389/fnins.2021.646956
Sachdev PS, Blacker D, Blazer DG et al (2014) Classifying neurocognitive disorders: the DSM-5 approach. Nat Rev Neurol 10:634–642. https://doi.org/10.1038/nrneurol.2014.181
Brewer WJ, Edwards J, Anderson V et al (1996) Neuropsychological, olfactory, and hygiene deficits in men with negative symptom schizophrenia. Biol Psychiatry 40:1021–1031. https://doi.org/10.1016/0006-3223(95)00594-3
Bersani G, Quartini A, Ratti F et al (2013) Olfactory identification deficits and associated response inhibition in obsessive–compulsive disorder: on the scent of the orbitofronto-striatal model. Psychiatry Res 210:208–214. https://doi.org/10.1016/j.psychres.2013.05.032
Chen B, Klarmann R, Israel M et al (2019) Difference of olfactory deficit in patients with acute episode of schizophrenia and major depressive episode. Schizophr Res 212:99–106. https://doi.org/10.1016/j.schres.2019.08.004
Compton MT, Mack LM, Esterberg ML et al (2006) Associations between olfactory identification and verbal memory in patients with schizophrenia, first-degree relatives, and non-psychiatric controls. Schizophr Res 86:154–166. https://doi.org/10.1016/j.schres.2006.06.007
Goudsmit N, Wolitzky R, Seckinger RA et al (2004) Trail making and olfaction in schizophrenia: implications for processing speed. CNS Spectr 9(344–349):356. https://doi.org/10.1017/s1092852900009329
Karavia A, Kapsali F, Gonidakis F et al (2022) Olfactory capacity in anorexia nervosa: correlations with set-shifting ability. Eat Weight Disord 27:535–542. https://doi.org/10.1007/s40519-021-01188-3
Maurage P, Callot C, Chang B et al (2011) Olfactory impairment is correlated with confabulation in alcoholism: towards a multimodal testing of orbitofrontal cortex. PLoS ONE 6:e23190. https://doi.org/10.1371/journal.pone.0023190
Moberg PJ, Arnold SE, Doty RL et al (2006) Olfactory functioning in schizophrenia: relationship to clinical, neuropsychological, and volumetric MRI measures. J Clin Exp Neuropsychol 28:1444–1461. https://doi.org/10.1080/13803390500434409
Mossaheb N, Kaufmann RM, Schlogelhofer M et al (2018) The impact of sex differences on odor identification and facial affect recognition in patients with schizophrenia spectrum disorders. Front Psychiatry 9:9. https://doi.org/10.3389/fpsyt.2018.00009
Rupp CI, Fleischhacker WW, Drexler A et al (2006) Executive function and memory in relation to olfactory deficits in alcohol-dependent patients. Alcohol Clin Exp Res 30:1355–1362. https://doi.org/10.1111/j.1530-0277.2006.00162.x
Segalàs C, Labad J, Alonso P et al (2011) Olfactory identification and discrimination in obsessive–compulsive disorder. Depress Anxiety 28:932–940. https://doi.org/10.1002/da.20836
Seidman LJ, Goldstein JM, Goodman JM et al (1997) Sex differences in olfactory identification and Wisconsin Card Sorting performance in schizophrenia: relationship to attention and verbal ability. Biol Psychiatry 42:104–115. https://doi.org/10.1016/S0006-3223(96)00300-9
Stedman TJ, Clair AL (1998) Neuropsychological, neurological and symptom correlates of impaired olfactory identification in schizophrenia. Schizophr Res 32:23–30. https://doi.org/10.1016/s0920-9964(98)00021-8
Takahashi T, Nakamura M, Sasabayashi D et al (2018) Olfactory deficits in individuals at risk for psychosis and patients with schizophrenia: relationship with socio-cognitive functions and symptom severity. Eur Arch Psychiatry Clin Neurosci 268:689–698. https://doi.org/10.1007/s00406-017-0845-3
de Nijs J, Meijer JH, de Haan L et al (2018) Associations between olfactory identification and (social) cognitive functioning: a cross-sectional study in schizophrenia patients and healthy controls. Psychiatry Res 266:147–151. https://doi.org/10.1016/j.psychres.2018.05.009
Barnett R, Maruff P, Purcell R et al (1999) Impairment of olfactory identification in obsessive–compulsive disorder. Psychol Med 29:1227–1233. https://doi.org/10.1017/s0033291799008818
Vasterling JJ, Brailey K, Sutker PB (2000) Olfactory identification in combat-related posttraumatic stress disorder. J Trauma Stress 13:241–253. https://doi.org/10.1023/A:1007754611030
Li Z-T, Tan S-Z, Lyu Z-H, Zou L-Q (2022) Olfactory identification impairment in early-and late-onset obsessive–compulsive disorder. Early Interv Psychiatry 16:133–138. https://doi.org/10.1111/eip.13136
Good KP, Martzke JS, Milliken HI et al (2002) Unirhinal olfactory identification deficits in young male patients with schizophrenia and related disorders: association with impaired memory function. Schizophr Res 56:211–223. https://doi.org/10.1016/s0920-9964(01)00227-4
Hernandez AK, Landis B, Altundag A et al (2023) Olfactory nomenclature: an orchestrated effort to clarify terms and definitions of dysosmia, anosmia, hyposmia, normosmia, hyperosmia, olfactory intolerance, parosmia, and phantosmia/olfactory hallucination. ORL J Otorhinolaryngol Relat Spec. https://doi.org/10.1159/000530211
Lahera G, Ruiz-Murugarren S, Fernández-Liria A et al (2016) Relationship between olfactory function and social cognition in euthymic bipolar patients. CNS Spectr 21:53–59. https://doi.org/10.1017/S1092852913000382
Ruff RL, Riechers RG II, Wang XF et al (2012) For veterans with mild traumatic brain injury, improved posttraumatic stress disorder severity and sleep correlated with symptomatic improvement. J Rehabil Res Dev 49:1305–1320. https://doi.org/10.1682/jrrd.2011.12.0251
Dahmani L, Patel RM, Yang Y et al (2018) An intrinsic association between olfactory identification and spatial memory in humans. Nat Commun 9:4162. https://doi.org/10.1038/s41467-018-06569-4
Fagundo AB, Jiménez-Murcia S, Giner-Bartolomé C et al (2015) Modulation of higher-order olfaction components on executive functions in humans. PLoS ONE 10:e0130319. https://doi.org/10.1371/journal.pone.0130319
Herman AM, Critchley H, Duka T (2018) Decreased olfactory discrimination is associated with impulsivity in healthy volunteers. Sci Rep 8:15584. https://doi.org/10.1038/s41598-018-34056-9
Dulay MF, Murphy C (2002) Olfactory acuity and cognitive function converge in older adulthood: support for the common cause hypothesis. Psychol Aging 17:392–404. https://doi.org/10.1037/0882-7974.17.3.392
Cedres N, Aejmelaeus-Lindstrom A, Ekstrom I et al (2022) Subjective impairments in olfaction and cognition predict dissociated behavioural outcomes. J Gerontol B Psychol Sci Soc Sci. https://doi.org/10.1093/geronb/gbac124
Economou A (2003) Olfactory identification in elderly Greek people in relation to memory and attention measures. Arch Gerontol Geriatrics 37:119–130. https://doi.org/10.1016/s0167-4943(03)00025-6
Larsson M, Finkel D, Pedersen NL (2000) Odor identification: Influences of age, gender, cognition, and personality. J Gerontol Ser B Psychol Sci Soc Sci 55:P304–P310. https://doi.org/10.1093/geronb/55.5.P304
Masala C, Cavazzana A, Sanna F et al (2022) Correlation between olfactory function, age, sex, and cognitive reserve index in the Italian population. Eur Arch Otorhinolaryngol 279:4943–4952. https://doi.org/10.1007/s00405-022-07311-z
Schubert CR, Cruickshanks KJ, Fischer ME et al (2017) Sensory impairments and cognitive function in middle-aged adults. J Gerontol Ser A Biol Sci Med Sci 72:1087–1090. https://doi.org/10.1093/gerona/glx067
Schubert CR, Cruickshanks KJ, Fischer ME et al (2013) Odor identification and cognitive function in the Beaver Dam Offspring Study. J Clin Exp Neuropsychol 35:669–676. https://doi.org/10.1080/13803395.2013.809701
Stevens JC, Cruz LA, Marks LE, Lakatos S (1998) A multimodal assessment of sensory thresholds in aging. J Gerontol Ser B Psychol Sci Soc Sci 53:P263–P272. https://doi.org/10.1093/geronb/53B.4.P263
Wehling EI, Nordin S, Espeseth T et al (2010) Familiarity, cued and free odor identification and their association with cognitive functioning in middle aged and older adults. Aging Neuropsychol Cogn 17:205–219. https://doi.org/10.1080/13825580903042684
Yahiaoui-Doktor M, Luck T, Riedel-Heller SG et al (2019) Olfactory function is associated with cognitive performance: results from the population-based LIFE-Adult-Study. Alzheimers Res Ther. https://doi.org/10.1186/s13195-019-0494-z
Tebrugge S, Winkler A, Gerards D et al (2018) Olfactory function is associated with cognitive performance: results of the heinz nixdorf recall study. J Alzheimers Dis 63:319–329. https://doi.org/10.3233/JAD-170863
Lecuyer Giguère F, Frasnelli A, De Guise E, Frasnelli J (2019) Olfactory, cognitive and affective dysfunction assessed 24 hours and one year after a mild Traumatic Brain Injury (mTBI). Brain Inj 33:1184–1193. https://doi.org/10.1080/02699052.2019.1631486
Callahan CD, Hinkebein J (1999) Neuropsychological significance of anosmia following traumatic brain injury. J Head Trauma Rehabil 14:581–587. https://doi.org/10.1097/00001199-199912000-00006
Yulug B, Saatci O, Işıklar A et al (2020) The association between HbA1c levels, olfactory memory and cognition in normal, pre-diabetic and diabetic persons. Endocr Metab Immune Disord Drug Targets 20:198–212. https://doi.org/10.2174/1871530319666190614121738
Zhang Z, Zhang B, Wang X et al (2019) Olfactory dysfunction mediates adiposity in cognitive impairment of type 2 diabetes: insights from clinical and functional neuroimaging studies. Diabetes Care 42:1274–1283. https://doi.org/10.2337/dc18-2584
Zhang Z, Zhang B, Wang X et al (2018) Altered odor-induced brain activity as an early manifestation of cognitive decline in patients with type 2 diabetes. Diabetes 67:994–1006. https://doi.org/10.2337/db17-1274
Midorikawa M, Suzuki H, Suzuki Y et al (2021) Relationships between cognitive function and odor identification, balance capability, and muscle strength in middle-aged persons with and without type 2 diabetes. J Diabetes Res 2021:9961612. https://doi.org/10.1155/2021/9961612
Mueller C, Temmel AF, Quint C et al (2002) Olfactory function in HIV-positive subjects. Acta Otolaryngol 122:67–71. https://doi.org/10.1080/00016480252775760
Razani J, Murphy C, Davidson TM et al (1996) Odor sensitivity is impaired in HIV-positive cognitively impaired patients. Physiol Behav 59:877–881. https://doi.org/10.1016/0031-9384(95)02163-9
Murphy C, Jinich S (1996) Olfactory dysfunction in Down’s syndrome. Neurobiol Aging 17:631–637. https://doi.org/10.1016/0197-4580(96)00008-5
Del Valle RM, Hollander E, McCracken J et al (2016) A multi-center, observational study to explore the relationship between exploratory biomarkers and functional dimensions in adults with autistic spectrum disorders. Eur Neuropsychopharmacol 26:S193
Killgore WD, Killgore DB, Grugle NL, Balkin TJ (2010) Odor identification ability predicts executive function deficits following sleep deprivation. Int J Neurosci 120:328–334. https://doi.org/10.3109/00207450903389396
Schwartz BS, Ford DP, Bolla KI et al (1991) Solvent-associated olfactory dysfunction: not a predictor of deficits in learning and memory. Am J Psychiatry 148:751–756. https://doi.org/10.1176/ajp.148.6.751
Chen L, Wang X, Doty RL et al (2021) Olfactory impairment in Wilson’s disease. Brain Behav 11:e02022. https://doi.org/10.1002/brb3.2022
Hedner M, Nilsson LG, Olofsson JK et al (2010) Age-related olfactory decline is associated with the BDNF val66met polymorphism: evidence from a population-based study. Front Aging Neurosci. https://doi.org/10.3389/fnagi.2010.00024
Dong J, Zhan X, Sun H et al (2022) Olfactory dysfunction is associated with cognitive impairment in patients with obstructive sleep apnea: a cross-sectional study. Eur Arch Otorhinolaryngol 279:1979–1987. https://doi.org/10.1007/s00405-021-07194-6
Antunes MB, Bowler R, Doty RL (2007) San Francisco/Oakland bay bridge welder study: olfactory function. Neurology 69:1278–1284. https://doi.org/10.1212/01.wnl.0000276988.50742.5e
Blanco S, Sanromán L, Pérez-Calvo S et al (2019) Olfactory and cognitive functioning in patients with fibromyalgia. Psychol Health Med 24:530–541. https://doi.org/10.1080/13548506.2018.1549741
Mullin S, Beavan M, Bestwick J et al (2019) Evolution and clustering of prodromal parkinsonian features in GBA1 carriers. Move Disorders 34:1365–1373. https://doi.org/10.1002/mds.27775
Campolo J, Corradi E, Rizzardi A et al (2021) Correlates of olfactory impairment in middle-aged non-diabetic Caucasian subjects with stage I–II obesity. Eur Arch Otorhinolaryngol 278:2047–2054. https://doi.org/10.1007/s00405-020-06442-5
Arnold SE, Hyman BT, Van Hoesen GW et al (1991) Some cytoarchitectural abnormalities of the entorhinal cortex in schizophrenia from the departments of neurology. Arch Gen Psychiatry 48:625–632
Chen Z, Sun J, Yang Y et al (2015) Cortical thinning in type 2 diabetes mellitus and recovering effects of insulin therapy. J Clin Neurosci 22:275–279. https://doi.org/10.1016/j.jocn.2014.07.014
Garcia AD, Buffalo EA (2020) Anatomy and function of the primate entorhinal cortex. Annu Rev Vis Sci 6:411–432. https://doi.org/10.1146/annurev-vision-030320-041115
Maass A, Berron D, Libby LA, Ranganath C (2015) Functional subregions of the human entorhinal cortex. Elife. https://doi.org/10.7554/eLife.06426.001
Mccrimmon RJ, Mccrimmon RJ, Ryan CM, Frier BM (2012) Diabetes 2 diabetes and cognitive dysfunction. Lancet 379:2291–2299. https://doi.org/10.1016/S0140
Damiano RF, Guedes BF, de Rocca CC et al (2022) Cognitive decline following acute viral infections: literature review and projections for post-COVID-19. Eur Arch Psychiatry Clin Neurosci 272:139–154
Walker KR, Tesco G (2013) Molecular mechanisms of cognitive dysfunction following traumatic brain injury. Front Aging Neurosci 5:1
Challakere Ramaswamy VM, Schofield PW (2022) Olfaction and executive cognitive performance: a systematic review. Front Psychol 13:871391. https://doi.org/10.3389/fpsyg.2022.871391
Schäfer L, Schriever VA, Croy I (2021) Human olfactory dysfunction: causes and consequences. Cell Tissue Res. https://doi.org/10.1007/s00441-020-03381-9
Ekström I, Sjölund S, Nordin S et al (2017) Smell loss predicts mortality risk regardless of dementia conversion. J Am Geriatr Soc 65:1238–1243. https://doi.org/10.1111/jgs.14770
Devanand DP, Lee S, Manly J et al (2015) Olfactory identification deficits and increased mortality in the community. Ann Neurol 78:401–411. https://doi.org/10.1002/ana.24447
Lawson RA, Yarnall AJ, Duncan GW et al (2016) Cognitive decline and quality of life in incident Parkinson’s disease: the role of attention. Parkinsonism Relat Disord 27:47–53. https://doi.org/10.1016/j.parkreldis.2016.04.009
Vance DE, Del Bene VA, Kamath V et al (2023) Does olfactory training improve brain function and cognition? A systematic review. Neuropsychol Rev 2023:1
Hedner M, Larsson M, Arnold N et al (2010) Cognitive factors in odor detection, odor discrimination, and odor identification tasks. J Clin Exp Neuropsychol 32:1062–1067. https://doi.org/10.1080/13803391003683070
Acknowledgements
The authors would like to acknowledge Informationist Marian LaForest, MPH at CUIMC Health Sciences Library and Evidence Synthesis Librarian and Information Methodologist Michelle R. Demetres, MLIS at Weill Cornell Medicine for their guidance in the development and revision of the ideal search strategy to comprehensively identify relevant studies.
Funding
This work was supported by Grant K23DC019678 from the National Institute on Deafness and Other Communication Disorders (https://www.nih.gov/about-nih/what-we-do/nih-almanac/national-institute-deafness-other-communication-disorders-nidcd) and the National Institutes of Health. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. The funders did not play any role in study design, data collection/analysis, decision to publish, or manuscript preparation.
Author information
Authors and Affiliations
Contributions
JO, DG, TG, and DPD conceptualized the work. PJ, BV, and JO developed and revised the search terms alongside the librarian team, with subsequent execution of the literature search. PJ, BV, JT, and NW performed article screening and data extraction. PJ and BV drafted the manuscript. All authors critically revised the work.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no relevant financial or non-financial conflict of interests to disclose.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jacobson, P.T., Vilarello, B.J., Tervo, J.P. et al. Associations between olfactory dysfunction and cognition: a scoping review. J Neurol 271, 1170–1203 (2024). https://doi.org/10.1007/s00415-023-12057-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-023-12057-7