Abstract
Introduction
While autonomic failure is a well-known prognostic factor for more aggressive disease progression in Parkinson’s disease (PD), with a three- to sevenfold higher risk of dementia and death within 10 years after the diagnosis, the individual impact of cardiovascular, gastrointestinal, urogenital, thermoregulatory, and pupillomotor autonomic domains on PD clinical outcomes remains unclear.
Objectives
We sought to determine the 5-year risk of developing dementia, falls, postural instability, dysarthria, and dysphagia in PD patients with and without autonomic impairment at baseline and to assess the joint and individual association of each autonomic domain on these key functional outcomes. In addition, we aimed to determine the impact of each autonomic domain on activities of daily living (ADLs) and health-related quality of life (HRQoL).
Methods
We enrolled 65 consecutive PD patients in a 5-year cohort study involving standardized evaluations of autonomic symptoms, orthostatic hypotension, and motor and non-motor features, including cognitive function. Associations were estimated as odds ratio and adjusted for PD duration, age, and baseline motor impairment.
Results
Cardiovascular dysautonomia was associated with a sevenfold higher risk of developing dementia (95%CI: 1.154–50.436; p = 0.035) and a fivefold higher risk of falls (95%CI: 1.099–18.949; p = 0.039), as well as significantly higher impairment in ADLs (p = 0.042) and HRQoL (p = 0.031). No relevant associations were found between the other autonomic domains and these outcomes.
Conclusions
Cardiovascular dysautonomia, but not other domains, showed an association with worse 5-year clinical outcomes in PD. Our data suggest a specific role for cardiovascular autonomic dysregulation in the pathogenic mechanisms of PD progression.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It has been estimated that 50–70% of individuals with Parkinson’s disease (PD) experience disturbances from autonomic nervous system failure, including cardiovascular, urogenital, gastrointestinal, thermoregulatory, and pupillomotor dysfunction [1,2,3]. Previous studies showed that general dysautonomia, and neurogenic orthostatic hypotension (OH) in particular, are associated with negative health outcomes in PD, including faster motor and cognitive decline, more frequent falls and hospitalizations, and a higher risk of developing dementia, disability, and death [4,5,6,7]. Still, the individual impact of each autonomic domain on disease progression and whether autonomic disturbances contribute directly to worse outcomes (e.g., extreme hemodynamic fluctuations potentially causing repeated cerebral hypoperfusion) or are merely associated with them (i.e., a marker of a more aggressive disease phenotype) remains unclear [8, 9].
In this 5-year prospective observational study, our primary aim was to determine the individual and joint association of each autonomic domain on developing critical PD disability milestones, including dementia, falls, postural instability, dysarthria, and dysphagia. Our secondary aim was to determine the impact of autonomic domains on progression of activities of daily living (ADLs) and health-related quality of life (HRQoL) impairment. Furthermore, we investigated the association between clinically defined OH and these outcomes.
Methods
Study design
This single-center, prospective, observational cohort study aimed to evaluate the impact of autonomic symptoms on disability milestones and functional outcomes in PD. Consecutive participants were enrolled from the Movement Disorders Center of the University of Torino between April 2015 and March 2016. The local institutional review board approved the study, and all participants gave written informed consent.
Eligibility criteria
Inclusion criteria were as follows: PD diagnosed according to the United Kingdom Brain Bank Criteria [10]; disease duration at least two years at baseline; age between 18 and 80 years; and stable dose of dopaminergic therapy and/or antihypotensive or antihypertensive medications for at least 4 weeks. Exclusion criteria were neurological signs suggestive of a diagnosis other than idiopathic PD; diabetes mellitus or other condition associated with autonomic neuropathy [11]; cardiac arrhythmia or coronary artery disease, cardiac valve disease or clinically relevant cardiac structural abnormalities; severe chronic renal insufficiency (glomerular filtration rate < 30 ml/min); undergoing chemotherapy; monoclonal gammopathy of uncertain significance (MGUS); major psychiatric disorder in accordance with Diagnostic and Statistical Manual of Mental Disorders (DSM) 5th ed. Criteria (American Psychiatric Association, 2013); or treatment with alpha-adrenergic antagonists for prostatic disorders.
Baseline assessments
Clinical and demographic data at baseline included age, medical history, and duration of PD from symptom onset. All medications were recorded and the levodopa equivalent daily dose (LEDD) calculated according to the conversion table proposed by Tomlisonet al. [12].
Clinical rating scales included motor assessment using the Movement Disorder Society-Unified Parkinson's Disease Rating Scale (MDS-UPDRS) Part III (motor examination) [12] during the best “on” state, defined as the period of perceived maximal efficacy from dopaminergic medications. Non-motor symptoms were assessed using the Non-Motor Symptoms Scale (NMSS) [13].
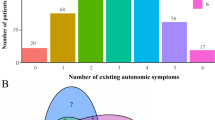
Autonomic and blood pressure (BP) assessments included the validated 25-item Scale for Outcomes in Parkinson’s Disease-Autonomic (SCOPA-AUT), a one-dimensional linear scale with high internal construct validity [14]. The following SCOPA-AUT subscales were independently rated: gastrointestinal (items 1–7); urogenital (8–13, for men 22–23 and for women 24–25); cardiovascular (14–16); thermoregulatory (17–18, 20–21); and pupillomotor (19). The impairment of an autonomic domain was defined when according to symptoms experienced in the past month at least one of the related items was rated ≥ 2; wherein 0, never; 1, sometimes; 2, regularly; and 3, often [15].
Patients underwent BP measurements using an automated sphygmomanometer (HEM-7200—Omron Healthcare Co. Kyoto, Japan) placed at heart level on the left arm, in the following conditions: (a) while sitting in a chair after at least 10 min of rest; (b) after a minimum of 10 min of supine rest; and (c) after one and three minutes of active standing. To minimize BP variability due to antiparkinsonian medications, patients were evaluated in standardized conditions. BP assessments were performed in the morning in the best “on” state, and at least 3 h after a meal. OH was defined as a BP drop ≥ 20 mmHg systolic or 10 mmHg diastolic within 3 min of standing from a supine position [16]. Patients with a rise in heart rate (HR)/fall in systolic BP ratio > 0.5 beats per minute (bpm)/mmHg [17] were considered as having non-neurogenic OH (i.e., due to iatrogenic cause, dehydration, venous pooling in the lower limbs, cardiac failure, etc.) and were excluded from the OH analyses. Hemodynamically relevant OH was defined as orthostatic mean arterial pressure (MAP) ≤ 75 mmHg [18]. Supine hypertension (SH) was defined as supine systolic BP ≥ 140 mmHg or diastolic BP ≥ 90 mmHg in patients affected by neurogenic OH (nOH) [19].
Functional and cognitive assessments included the MDS-UPDRS Parts I (non-motor experience of daily living), II (motor experience of daily living), and IV (motor complications) [13]; Montreal Cognitive Assessment (MoCA; range 0–30, lower is worse) [20]; and the 8-item PD Quality of Life Questionnaire (PDQ-8 single index; range 0–100, higher is worse) [21].
Follow-up assessments
After 5 years, the patients underwent the following assessments to evaluate functional outcomes, independence in ADLs, and HRQoL: MDS-UPDRS Parts I and II, MoCA, and PDQ-8; the number of falls in the previous 4 weeks.
Five specific disability milestones were chosen to define disease progression, including the following: (1) dementia, defined as MoCA score < 21/30 [22]; (2) falls in the 4 weeks prior to the evaluation; (3) postural instability, defined as a score ≥ 3 of item 3.12 of the MDS-UPDRS; (4) dysphagia, defined as a score ≥ 3 of item 2.3 of the MDS-UPDRS; and (5) dysarthria, defined as a score ≥ 3 of item 2.1 of the MDS-UPDRS.
Outcome measures and statistical analyses
Our primary aim was to evaluate the 5-year risk of developing the five key disability milestones listed above in patients with and without PD-associated autonomic symptoms and with and without nOH at baseline, evaluating the individual and joint impact of each autonomic domain. Our secondary aim was to determine the role of autonomic dysfunction and nOH in progression of ADL and HRQoL impairment.
Primary endpoints were dementia, falls, postural instability, dysphagia, and dysarthria. A binary logistic regression was used to estimate the odds ratio (OR) of global autonomic impairment at baseline, as measured by the total SCOPA-AUT score, and of each individual autonomic domain impairment (independent variables) on the occurrence of disability milestones along the 5-year follow-up (dependent variables), adjusting for age, disease duration, and motor symptom severity (MDS-UPDRS Part III) at baseline. The logistic regression was run twice as follows: (a) considering SCOPA-AUT and each autonomic domain separately (univariate); and (b) considering all the autonomic domains together (multivariate). Only for dementia, the analyses were run including the entire sample and, then again, excluding the individuals who had dementia at baseline. The same analyses were used to evaluate the association between nOH at baseline and disability milestones, and between hemodynamically relevant nOH and disability milestones. A sub-analysis on the impact of SH associated with nOH was also included. The Hosmer and Lemeshow’s goodness-of-fit test was applied.
Secondary endpoints included impairment of ADLs, as measured by the MDS-UPDRS Parts I and II, and HRQoL, as measured by the PDQ-8. A repeated-measures ANOVA was used to evaluate progression independent variables (MDS-UPDRS Part I, Part II, Parts I + II combined, and PDQ-8), adjusting for age, disease duration, and motor symptom severity at baseline (covariates), between patients with and without the following conditions: (a) impairment in each autonomic domain; (b) nOH; and (c) hemodynamically relevant nOH.
Clinical and demographic characteristics were summarized as mean ± standard deviation and range or absolute number and percentages, as appropriate. The differences between SCOPA-AUT, MDS-UPDRS Parts I and II, MoCA, and PDQ-8 scores at baseline and at 5-year follow-up were evaluated by means of the Wilcoxon non-parametric test. All the analyses were performed with Statistical Package for the Social Sciences (SPSS 27.0 for Macintosh, Chicago, IL), using two-tailed p-values with a level of significance of 0.05.
Data availability
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
Results
Out of the 65 PD patients enrolled in the study, nine (15.3%) died during the observational study period (mean time from baseline: 29.7 ± 7.7 months), and six (9.2%) were lost to follow-up (Supplementary Table 1). Thus, 5-year follow-up data were available for 50 patients (Tables 1 and 2), and showed a 66.9% overall progression in global ADL impairment (MDS-UPDRS Parts I + II: from 23.1 ± 10.3 to 38.6 ± 17.8; p < 0.001) and a significant 81.4% worsening in HRQoL (PDQ-8: from 22.6 ± 19.0 to 41.0 ± 29.4; p < 0.001). MoCA score significantly declined by 12.3% (from 26.1 ± 3.5 to 22.9 ± 5.4; p < 0.001), with the prevalence of demented patients rising from 8.0% (4/50) to 30% (15/50); the 5-year incidence of dementia was 23.9% (11/46).
The vast majority of patients (86.0%) reported a significant progression in their baseline autonomic symptoms over follow-up, with the SCOPA-AUT total score increasing from 13.1 ± 8.7 at baseline to 21.3 ± 10.4 points at year 5 (62.6% worsening) (p < 0.001). The gastrointestinal domain worsened by 70.3% (from 3.7 ± 2.9 to 6.3 ± 3.8; p < 0.001), the urogenital by 55.4% (from 5.6 ± 5.2 to 8.7 ± 5.2; p < 0.001), the cardiovascular by 66.7% (from 1.2 ± 1.9 to 2.0 ± 2.3; p < 0.001); the thermoregulatory by 54.5% (from 2.2 ± 2.5 to 3.4 ± 3.1; p = 0.008), and the pupillomotor by 125% (from 0.4 ± 0.7 to 0.9 ± 1.0; p = 0.002).
Dysautonomia and disability milestones
The total SCOPA-AUT score was not associated with any of the disability milestones evaluated: dementia (p = 0.478), falls (p = 0.790), postural instability (p = 0.326), or dysphagia (p = 0.253), with a trend towards statistical significance only for dysarthria (p = 0.061) (Table 3). However, the cardiovascular score was independently associated with a higher risk of developing dementia, both in the univariate and in the multivariate analysis (OR: 9.058; 95% CI: 1.548–53.000; p = 0.014; and OR: 7.630; 95% CI: 1.154–50.436; p = 0.035, respectively) (Table 3) and with falls in the univariate analysis (OR: 5.701; 95% CI: 1.099–18.949; p = 0.039) (Table 3). None of the autonomic domains were associated with postural instability, dysphagia, or dysarthria (Table 3).
Neurogenic OH and disability milestones
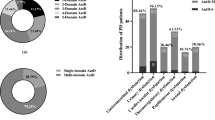
At baseline, 13/50 patients (28.8%) had clinically defined nOH (Table 1), with 10 of those patients (76.9%) meeting the criteria for hemodynamically relevant OH. Four patients (30.8%) with nOH did not report significant OH-related symptoms on the SCOPA-AUT evaluation; despite that, two of them (50%; one demented and one non-demented) had hemodynamically relevant nOH. Only one patient reported cardiovascular dysautonomia symptoms without having OH. Six out of 13 patients with nOH (46.2%) met the criteria for SH (Table 1). Finally, two patients had non-neurogenic OH. The presence of nOH at baseline, after correcting for age, disease duration, and motor impairment, was associated with dementia at the 5-year follow-up (OR: 5.213; 95% CI: 1.194–24.391; p = 0.036), even after removing patients already affected by dementia at baseline (OR: 5.153; 95% CI: 1.289–26.943; p = 0.029). This association was even stronger when considering patients with concomitant SH (OR: 8.265; 95% CI: 2.026–32.103; p = 0.012). nOH was also associated with falls (OR: 7.129; 95% CI: 1.212–41.921; p = 0.030), but concomitant SH did not have an influence on falls (OR: 5.732; 95% CI: 0.492–49.271; p = 0.492). No association was found with postural instability (p = 0.655), dysphagia (p = 0.086), or dysarthria (p = 0.641). Similar results were found when analyzing patients with hemodynamically relevant nOH, confirming a significant, and even stronger, association with the development of dementia at the 5-year follow-up both before (OR: 7.713; 95% CI: 1.305–45.599; p = 0.024) and after (OR: 8.750; 95% CI: 1.502–50.987; p = 0.016) removing patients with dementia at baseline, and with falls (OR: 12.391; 95% CI: 1.215–58.367; p = 0.034). Again, no association was found with postural instability (p = 0.714), dysphagia (p = 0.129), or dysarthria (p = 0.155).
Dysautonomia, ADL impairment, and quality of life
Among the different autonomic domains, only the cardiovascular domain was associated with a worse progression of functional disability. Patients with cardiovascular autonomic symptoms showed a greater worsening of the motor experience of daily living (MDS-UPDRS Part II, F: 4.187; p = 0.039) (Fig. 1A), the global experience of daily living (MDS-UPDRS Parts I + II, F: 3.786; p = 0.042) (Fig. 1B), and HRQoL (PDQ-8, F: 4.927; p = 0.031) (Fig. 1C).
Five-year progression of activities of daily living and health-related quality of life impairment in patients with and without cardiovascular dysautonomia symptoms and patients with and without neurogenic orthostatic hypotension. Patients with cardiovascular dysautonomia symptoms showed greater worsening of motor experience of daily living (A), global experience of daily living (B), and health-related quality of life (C). Patients with orthostatic hypotension showed greater worsening of motor experience of daily living (D) and health-related quality of life (E). Patients with hemodynamically relevant orthostatic hypotension showed greater worsening of motor experience of daily living (F), global experience of daily living (G), and health-related quality of life (H). Covariates considered for ANCOVA analysis: age, disease duration, and MDS-UPDRS Part III at baseline. MDS-UPDRS, Movement Disorders Society Unified Parkinson’s Disease Rating Scale; PDQ-8, Parkinson’s Disease Questionaire-8
Neurogenic OH, ADL impairment, and quality of life
Patients with nOH showed worse function in the motor experience of daily living (F: 3.174; p = 0.048) (Fig. 1D) and HRQoL (F: 3.316; p = 0.045) (Fig. 1E).
When considering only hemodynamically relevant nOH, there remained a significant association with a worse progression of the motor experience of daily living (MDS-UPDRS Part II, F: 3.534; p = 0.043) (Fig. 1F), the global experience of daily living (MDS-UPDRS Parts I + II, F: 3.267; p = 0.046) (Fig. 1G), and HRQoL (F: 3.700; p = 0.042) (Fig. 1H).
Discussion
In this 5-year prospective follow-up study comparing an outpatient cohort of 65 PD patients with and without autonomic impairment at baseline, we analyzed the contribution of general dysautonomia and individual autonomic domain dysfunction on disability milestones and progression of ADL impairment and HRQoL. Cardiovascular dysautonomia was associated with worse clinical outcomes at five years, including 7-times higher odds of dementia and 5-times higher odds of falls, and worse deterioration in functional impairment and HRQoL. These negative associations were confirmed when comparing patients with and without clinically defined nOH and further reinforced when considering the subset of patients with hemodynamically relevant nOH. No associations were found between global dysautonomia or any other autonomic domain and these outcomes.
Other studies have demonstrated a strong relationship between cardiovascular dysautonomia and disability in PD, including cognitive impairment, falls, postural instability, and functional decline [6, 9, 23]. A retrospective review of clinical data from 100 autopsy-confirmed PD patients revealed that earlier autonomic dysfunction, defined by more than one autonomic symptom documented for at least 6 months, was associated with 14% higher risk per year of developing any disability milestone, including falls, wheelchair dependence, cognitive impairment, dysphagia, dysarthria, and placement in a residential facility [7]. Moreover, a prospective study of 336 PD patients followed over 2 years found that baseline general dysautonomia (SCOPA-AUT total score) was associated with worse deterioration in HRQoL, assessed with the EuroQol Visual Analogue Scale [24]. However, neither of these studies investigated the association of individual autonomic domains.
In our study, we found that nOH was the major driver of disability progression and functional impairment in PD. Several theories exist to explain the pathophysiological mechanisms of this association. The “causative hypothesis” [25] posits that repeated episodes of cerebral hypoperfusion, often associated with increased BP variability and/or hypertensive events, damage the brain cumulatively, which causes cortical damage [26]. The causative hypothesis is supported by animal models of neurodegenerative dementia, where it has been suggested that hypoperfusion could impair regional brain microcirculation, reducing the delivery of energy substrates needed for proper neuronal function. This “critically attained threshold of cerebral hypoperfusion” could favor oxidative stress and mitochondrial abnormalities [27], and finally lead to the progression of metabolic and tissue pathology [28]. However, human studies on this topic are limited. In this context, we observed a higher incidence of dementia in patients with nOH and concomitant SH, suggesting a possible role of SH in promoting additional brain injury. However, this association should be interpreted with caution given our small sample size and contrasting results in the existing literature [26, 29]. Furthermore, managing individuals that have nOH and concomitant SH often presents a clinical dilemma given the narrow therapeutic window for blood pressure targets – since treating nOH can worsen SH and vice versa [30]. As confirmed in our study, the MAP seems to represent a key factor in predicting falls and OH complications: therefore, some extent of SH may be advisable when the MAP is excessively low (e.g., below 75 mmHg) [18].
An alternative theory, the “associative hypothesis”, suggests that dysautonomia, including cardiovascular dysfunction, is associated with a malignant phenotype of PD that progresses faster and manifests with rapid eye movement (REM) sleep behavior disorder and earlier development of cognitive impairment [31]. It is hypothesized that in this PD subtype, dysautonomia may occur due to diffuse alpha-synuclein pathology involving the central autonomic network, i.e., the insular cortex and brainstem as well as peripheral noradrenergic denervation [32]. However, these theories are not mutually exclusive. Extreme fluctuations in cerebral perfusion and neurodegeneration may have a synergistic effect on brain injury, leading to worse outcomes [33]. In a rat model of dementia, chronic hypoxic injury seems to accelerate the deposition of amyloid β in the frontal cortex and hippocampus and of hyperphosphorylated tau in the temporal cortex [34]. Furthermore, in PD patients with cardiovascular autonomic failure, arterial walls may become stiffer to enhance vasoconstriction in compensation for reduced noradrenaline release—increased arterial wall stiffness may contribute to cerebrovascular changes that associate with cognitive impairment and white matter lesions on magnetic resonance imaging [35].
Despite needing further validation, our findings seem to be more supportive of the “causative hypothesis”, since neither general autonomic impairment nor other individual autonomic domains were associated with worse outcomes in our cohort, as would be expected if dysautonomia was associated with the so-called “diffuse malignant” PD phenotype [31]. Furthermore, although we found an association between cardiovascular dysautonomia and falls, we did not find any association with postural instability. This discrepancy seems to suggest that cardiovascular dysautonomia is an independent risk factor for falls, even in the absence of a significant association with postural instability, which is another well-known risk factor for falls [36]. Whether this observation is due to the relatively small sample size or, on the contrary, suggests the predominant role of cardiovascular dysautonomia in the development of worse clinical outcomes, independently from the “associative hypothesis” of a widespread neurodegeneration, still needs further confirmation.
Although we did not find that any autonomic domains besides cardiovascular were associated with PD disability milestones, other longitudinal observational studies have shown that severity of general dysautonomia is associated with postural instability-gait disturbances motor phenotype in PD [37] and that gastrointestinal dysfunction is associated with worse cognition in early PD [38, 39]. However, these studies analyzed newly diagnosed PD patients, with a mean age at the disease onset greater than 60 years; therefore, their results are not fully comparable to ours and could reflect a phenotypic, rather than a causal, association.
Strengths of our study include the long-term prospective and longitudinal design, with detailed characterization of autonomic symptoms, and high retention rate. Limitations include the relatively small sample size and the monocentric design. Moreover, while the SCOPA-AUT is a robust and MDS-recommended rating scale for autonomic symptoms in PD, we acknowledge that its subjective nature has intrinsic limitations, which include the following: (a) difficulty for most patients in differentiating the "sometimes" and "regularly" responses [14], (b) the potential clinimetric weaknesses of dividing the scale into different autonomic domains [14, 40, 41]; (c) the limited capability in capturing pupillomotor and thermoregulatory dysfunction [42, 43]; and (d) the potential weak correlation between subjectively reported and objectively measured cardiovascular dysfunction [44,45,46]. Additionally, the use of the ΔHR/ΔBP ratio for the definition of nOH [17] may have excluded some patients with nOH. Finally, due to the COVID-19 pandemic, we were not able to repeat a complete motor examination and nOH assessment at the 5-year follow-up.
In summary, our results showed that among autonomic domains, cardiovascular dysautonomia was associated with a higher risk of developing disability milestones and worse progression of functional impairment and HRQoL over the course of 5 years. Whether cardiovascular dysautonomia directly causes worse outcomes in PD or is only one of the features of a multifaceted malignant phenotype remains a major knowledge gap. To clarify these hypotheses, and to determine the potential role of delaying, or even preventing, the development of dementia and other disability milestones by treating cardiovascular dysautonomia, additional prospective research in larger multicentric cohorts is needed.
Data availability statement
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
References
Simuni T, Caspell-Garcia C, Coffey CS, Weintraub D, Mollenhauer B, Lasch S, Tanner CM, Jennings D, Kieburtz K, Chahine LM, Marek K (2018) Baseline prevalence and longitudinal evolution of non-motor symptoms in early Parkinson’s disease: the PPMI cohort. J Neurol Neurosurg Psychiatry 89:78–88. https://doi.org/10.1136/jnnp-2017-316213
Merola A, Romagnolo A, Comi C, Rosso M, Artusi CA, Zibetti M, Lanotte M, Duker AP, Maule S, Lopiano L, Espay AJ (2017) Prevalence and burden of dysautonomia in advanced Parkinson’s disease. Mov Disord 32:796–797. https://doi.org/10.1002/mds.26970
Martinez-Martin P, Chaudhuri KR, Rojo-Abuin JM, Rodriguez-Blazquez C, Alvarez-Sanchez M, Arakaki T, Bergareche-Yarza A, Chade A, Garretto N, Gershanik O, Kurtis MM, Martinez-Castrillo JC, Mendoza-Rodriguez A, Moore HP, Rodriguez-Violante M, Singer C, Tilley BC, Huang J, Stebbins GT, Goetz CG (2015) Assessing the non-motor symptoms of Parkinson’s disease: MDS-UPDRS and NMS Scale. Eur J Neurol 22:37–43. https://doi.org/10.1111/ene.12165
Goldstein DS, Holmes C, Sharabi Y, Wu T (2015) Survival in synucleinopathies: a prospective cohort study. Neurology 85:1554–1561. https://doi.org/10.1212/WNL.0000000000002086
Maule S, Milazzo V, Maule MM, Di Stefano C, Milan A, Veglio F (2012) Mortality and prognosis in patients with neurogenic orthostatic hypotension. Funct Neurol 27:101–106
Pilotto A, Romagnolo A, Tuazon JA, Vizcarra JA, Marsili L, Zibetti M, Rosso M, Rodriguez-Porcel F, Borroni B, Rizzetti MC, Rossi C, Vizcarra-Escobar D, Molano JR, Lopiano L, Ceravolo R, Masellis M, Espay AJ, Padovani A, Merola A (2019) Orthostatic hypotension and REM sleep behaviour disorder: impact on clinical outcomes in alpha-synucleinopathies. J Neurol Neurosurg Psychiatry 90:1257–1263. https://doi.org/10.1136/jnnp-2019-320846
De Pablo-Fernandez E, Tur C, Revesz T, Lees AJ, Holton JL, Warner TT (2017) Association of autonomic dysfunction with disease progression and survival in Parkinson disease. JAMA Neurol 74:970–976. https://doi.org/10.1001/jamaneurol.2017.1125
Stankovic I, Petrovic I, Pekmezovic T, Markovic V, Stojkovic T, Dragasevic-Miskovic N, Svetel M, Kostic V (2019) Longitudinal assessment of autonomic dysfunction in early Parkinson’s disease. Parkinsonism Relat Disord 66:74–79. https://doi.org/10.1016/j.parkreldis.2019.07.008
Sklerov M, Shih CH, Browner N, Palma JA, Styner M, Dayan E (2020) Longitudinal change in autonomic symptoms predicts activities of daily living and depression in Parkinson’s disease. Clin Auton Res. https://doi.org/10.1007/s10286-020-00672-7
Gibb WR, Lees AJ (1988) The relevance of the Lewy body to the pathogenesis of idiopathic Parkinson’s disease. J Neurol Neurosurg Psychiatry 51:745–752. https://doi.org/10.1136/jnnp.51.6.745
Freeman R (2005) Autonomic peripheral neuropathy. Lancet 365:1259–1270. https://doi.org/10.1016/S0140-6736(05)74815-7
Goetz CG, Tilley BC, Shaftman SR, Stebbins GT, Fahn S, Martinez-Martin P, Poewe W, Sampaio C, Stern MB, Dodel R, Dubois B, Holloway R, Jankovic J, Kulisevsky J, Lang AE, Lees A, Leurgans S, LeWitt PA, Nyenhuis D, Olanow CW, Rascol O, Schrag A, Teresi JA, van Hilten JJ, LaPelle N, Movement Disorder Society URTF (2008) Movement Disorder Society-sponsored revision of the Unified Parkinson's Disease Rating Scale (MDS-UPDRS): scale presentation and clinimetric testing results. Mov Disord 23:2129-2170. https://doi.org/10.1002/mds.22340
Chaudhuri KR, Martinez-Martin P, Brown RG, Sethi K, Stocchi F, Odin P, Ondo W, Abe K, Macphee G, Macmahon D, Barone P, Rabey M, Forbes A, Breen K, Tluk S, Naidu Y, Olanow W, Williams AJ, Thomas S, Rye D, Tsuboi Y, Hand A, Schapira AH (2007) The metric properties of a novel non-motor symptoms scale for Parkinson’s disease: Results from an international pilot study. Mov Disord 22:1901–1911. https://doi.org/10.1002/mds.21596
Forjaz MJ, Ayala A, Rodriguez-Blazquez C, Frades-Payo B, Martinez-Martin P, Longitudinal Parkinson's Disease Patient Study EldpcedP-EG (2010) Assessing autonomic symptoms of Parkinson's disease with the SCOPA-AUT: a new perspective from Rasch analysis. Eur J Neurol 17:273-279. https://doi.org/10.1111/j.1468-1331.2009.02835.x
Merola A, Romagnolo A, Rosso M, Suri R, Berndt Z, Maule S, Lopiano L, Espay AJ (2018) Autonomic dysfunction in Parkinson's disease: a prospective cohort study. Mov Disord 33:391–397. https://doi.org/10.1002/mds.27268
Gibbons CH, Schmidt P, Biaggioni I, Frazier-Mills C, Freeman R, Isaacson S, Karabin B, Kuritzky L, Lew M, Low P, Mehdirad A, Raj SR, Vernino S, Kaufmann H (2017) The recommendations of a consensus panel for the screening, diagnosis, and treatment of neurogenic orthostatic hypotension and associated supine hypertension. J Neurol 264:1567–1582. https://doi.org/10.1007/s00415-016-8375-x
Norcliffe-Kaufmann L, Kaufmann H, Palma JA, Shibao CA, Biaggioni I, Peltier AC, Singer W, Low PA, Goldstein DS, Gibbons CH, Freeman R, Robertson D, Autonomic Disorders C (2018) Orthostatic heart rate changes in patients with autonomic failure caused by neurodegenerative synucleinopathies. Ann Neurol 83:522–531. https://doi.org/10.1002/ana.25170
Palma JA, Gomez-Esteban JC, Norcliffe-Kaufmann L, Martinez J, Tijero B, Berganzo K, Kaufmann H (2015) Orthostatic hypotension in Parkinson disease: how much you fall or how low you go? Mov Disord 30:639–645. https://doi.org/10.1002/mds.26079
Fanciulli A, Jordan J, Biaggioni I, Calandra-Buonaura G, Cheshire WP, Cortelli P, Eschlboeck S, Grassi G, Hilz MJ, Kaufmann H, Lahrmann H, Mancia G, Mayer G, Norcliffe-Kaufmann L, Pavy-Le Traon A, Raj SR, Robertson D, Rocha I, Struhal W, Thijs R, Tsioufis KP, van Dijk JG, Wenning GK (2018) Consensus statement on the definition of neurogenic supine hypertension in cardiovascular autonomic failure by the American Autonomic Society (AAS) and the European Federation of Autonomic Societies (EFAS): Endorsed by the European Academy of Neurology. Clin Auton Res 28:355–362. https://doi.org/10.1007/s10286-018-0529-8
Nasreddine ZS, Phillips NA, Bedirian V, Charbonneau S, Whitehead V, Collin I, Cummings JL, Chertkow H (2005) The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc 53:695–699. https://doi.org/10.1111/j.1532-5415.2005.53221.x
Jenkinson C, Fitzpatrick R, Peto V, Greenhall R, Hyman N (1997) The PDQ-8: development and validation of a short-form Parkinson’s disease questionnaire. Psychol Health 12:805–814
Dalrymple-Alford JC, MacAskill MR, Nakas CT, Livingston L, Graham C, Crucian GP, Melzer TR, Kirwan J, Keenan R, Wells S, Porter RJ, Watts R, Anderson TJ (2010) The MoCA: well-suited screen for cognitive impairment in Parkinson disease. Neurology 75:1717–1725. https://doi.org/10.1212/WNL.0b013e3181fc29c9
Merola A, Romagnolo A, Rosso M, Lopez-Castellanos JR, Wissel BD, Larkin S, Bernardini A, Zibetti M, Maule S, Lopiano L, Espay AJ (2016) Orthostatic hypotension in Parkinson’s disease: Does it matter if asymptomatic? Parkinsonism Relat Disord 33:65–71. https://doi.org/10.1016/j.parkreldis.2016.09.013
Visser M, Verbaan D, van Rooden S, Marinus J, van Hilten J, Stiggelbout A (2009) A longitudinal evaluation of health-related quality of life of patients with Parkinson’s disease. Value Health 12:392–396. https://doi.org/10.1111/j.1524-4733.2008.00430.x
McDonald C, Newton JL, Burn DJ (2016) Orthostatic hypotension and cognitive impairment in Parkinson’s disease: causation or association? Mov Disord 31:937–946. https://doi.org/10.1002/mds.26632
Pilotto A, Romagnolo A, Scalvini A, Masellis M, Shimo Y, Bonanni L, Camicioli R, Wang LL, Dwivedi AK, Longardner K, Rodriguez-Porcel F, DiFrancesco M, Vizcarra JA, Montanaro E, Maule S, Lupini A, Ojeda-Lopez C, Black SE, Delli Pizzi S, Gee M, Tanaka R, Yamashiro K, Hatano T, Borroni B, Gasparotti R, Rizzetti MC, Hattori N, Lopiano L, Litvan I, Espay AJ, Padovani A, Merola A (2021) Association of orthostatic hypotension with cerebral atrophy in patients with Lewy body disorders. Neurology 97:e814–e824. https://doi.org/10.1212/WNL.0000000000012342
Aliev G, Smith MA, Obrenovich ME, de la Torre JC, Perry G (2003) Role of vascular hypoperfusion-induced oxidative stress and mitochondria failure in the pathogenesis of Azheimer disease. Neurotox Res 5:491–504. https://doi.org/10.1007/BF03033159
de la Torre JC (2000) Critically attained threshold of cerebral hypoperfusion: the CATCH hypothesis of Alzheimer’s pathogenesis. Neurobiol Aging 21:331–342. https://doi.org/10.1016/s0197-4580(00)00111-1
Palma JA, Redel-Traub G, Porciuncula A, Samaniego-Toro D, Millar Vernetti P, Lui YW, Norcliffe-Kaufmann L, Kaufmann H (2020) The impact of supine hypertension on target organ damage and survival in patients with synucleinopathies and neurogenic orthostatic hypotension. Parkinson Relat Disord 75:97–104. https://doi.org/10.1016/j.parkreldis.2020.04.011
Espay AJ, LeWitt PA, Hauser RA, Merola A, Masellis M, Lang AE (2016) Neurogenic orthostatic hypotension and supine hypertension in Parkinson’s disease and related synucleinopathies: prioritisation of treatment targets. Lancet Neurol 15:954–966. https://doi.org/10.1016/S1474-4422(16)30079-5
Fereshtehnejad SM, Romenets SR, Anang JB, Latreille V, Gagnon JF, Postuma RB (2015) New clinical subtypes of Parkinson disease and their longitudinal progression: a prospective cohort comparison with other phenotypes. JAMA Neurol 72:863–873. https://doi.org/10.1001/jamaneurol.2015.0703
Coon EA, Cutsforth-Gregory JK, Benarroch EE (2018) Neuropathology of autonomic dysfunction in synucleinopathies. Mov Disord 33:349–358. https://doi.org/10.1002/mds.27186
Udow SJ, Robertson AD, MacIntosh BJ, Espay AJ, Rowe JB, Lang AE, Masellis M (2016) “Under pressure”: is there a link between orthostatic hypotension and cognitive impairment in alpha-synucleinopathies? J Neurol Neurosurg Psychiatry 87:1311–1321. https://doi.org/10.1136/jnnp-2016-314123
Park JH, Hong JH, Lee SW, Ji HD, Jung JA, Yoon KW, Lee JI, Won KS, Song BI, Kim HW (2019) The effect of chronic cerebral hypoperfusion on the pathology of Alzheimer’s disease: a positron emission tomography study in rats. Sci Rep 9:14102. https://doi.org/10.1038/s41598-019-50681-4
Kim JS, Oh YS, Lee KS, Kim YI, Yang DW, Goldstein DS (2012) Association of cognitive dysfunction with neurocirculatory abnormalities in early Parkinson disease. Neurology 79:1323–1331. https://doi.org/10.1212/WNL.0b013e31826c1acd
Fasano A, Canning CG, Hausdorff JM, Lord S, Rochester L (2017) Falls in Parkinson’s disease: a complex and evolving picture. Mov Disord 32:1524–1536. https://doi.org/10.1002/mds.27195
Malek N, Lawton MA, Grosset KA, Bajaj N, Barker RA, Burn DJ, Foltynie T, Hardy J, Morris HR, Williams NM, Ben-Shlomo Y, Wood NW, Grosset DG, Consortium PRC (2017) Autonomic dysfunction in early Parkinson's disease: results from the united kingdom tracking Parkinson's study. Movement disorders clinical practice 4:509-516. https://doi.org/10.1002/mdc3.12454
Leta V, Urso D, Batzu L, Weintraub D, Titova N, Aarsland D, Martinez-Martin P, Borghammer P, van Wamelen DJ, Yousaf T, Rizos A, Rodriguez-Blazquez C, Chung-Faye G, Chaudhuri KR (2021) Constipation is associated with development of cognitive impairment in de novo Parkinson’s disease: a longitudinal analysis of two international cohorts. J Parkinsons Dis 11:1209–1219. https://doi.org/10.3233/JPD-212570
Jones JD, Rahmani E, Garcia E, Jacobs JP (2020) Gastrointestinal symptoms are predictive of trajectories of cognitive functioning in de novo Parkinson’s disease. Parkinson Relat Disord 72:7–12. https://doi.org/10.1016/j.parkreldis.2020.01.009
Rodriguez-Blazquez C, Forjaz MJ, Frades-Payo B, de Pedro-Cuesta J, Martinez Martin P, Longitudinal Parkinson's Disease Patient Study ELdPcEdPG (2010) Independent validation of the scales for outcomes in Parkinson's disease-autonomic (SCOPA-AUT). Eur J Neurol 17:194–201. https://doi.org/10.1111/j.1468-1331.2009.02788.x
Carod-Artal FJ, Ribeiro Lda S, Kummer W, Martinez-Martin P (2010) Psychometric properties of the SCOPA-AUT Brazilian Portuguese version. Mov Disord 25:205–212. https://doi.org/10.1002/mds.22882
Leclair-Visonneau L, Magy L, Volteau C, Clairembault T, Le Dily S, Preterre C, Peyre A, Damier P, Neunlist M, Pereon Y, Derkinderen P (2018) Heterogeneous pattern of autonomic dysfunction in Parkinson’s disease. J Neurol 265:933–941. https://doi.org/10.1007/s00415-018-8789-8
Rocchi C, Cerroni R, Conti M, Lauretti B, Mercuri NB, Stefani A, Pierantozzi M (2021) Sudomotor and cardiovascular autonomic function in de novo Parkinson’s disease assessed by sudoscan and cardiovascular reflexes. J Neurol Sci 427:117502. https://doi.org/10.1016/j.jns.2021.117502
Berganzo K, Tijero B, Somme JH, Llorens V, Sanchez-Manso JC, Low D, Iodice V, Vichayanrat E, Mathias CJ, Lezcano E, Zarranz JJ, Gomez-Esteban JC (2012) SCOPA-AUT scale in different parkinsonisms and its correlation with (123) I-MIBG cardiac scintigraphy. Parkinson Relat Disord 18:45–48. https://doi.org/10.1016/j.parkreldis.2011.08.018
Papapetropoulos S, Argyriou AA, Chroni E (2006) No correlation between the clinical severity of autonomic symptoms (SCOPA-AUT) and electrophysiological test abnormalities in advanced Parkinson’s disease. Mov Disord 21:430–431. https://doi.org/10.1002/mds.20782
Garg D, Srivastava AK, Jaryal AK, Rajan R, Singh A, Pandit AK, Vibha D, Shukla G, Garg A, Pandey RM, Prasad K (2020) Is there a difference in autonomic dysfunction between multiple system atrophy subtypes? Mov Disord Clin Pract 7:405–412. https://doi.org/10.1002/mdc3.12936
Funding
Open access funding provided by Università degli Studi di Torino within the CRUI-CARE Agreement. This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
KL: study conception and design; interpretation of data; drafting the manuscript. AM: study conception and design; interpretation of data; revising the manuscript for intellectual content. IL: interpretation of data; revising the manuscript for intellectual content. AMS: acquisition of data; revising the manuscript for intellectual content. SM: interpretation of data; revising the manuscript for intellectual content. FV: interpretation of data; revising the manuscript for intellectual content. LL: interpretation of data; revising the manuscript for intellectual content. AR: study conception and design; acquisition, analysis and interpretation of data; drafting and revising the manuscript for intellectual content. All the co-authors listed above gave their final approval of this manuscript version.
Corresponding author
Ethics declarations
Conflicts of interest
Dr. Longardner: received advisory board compensation from Lundbeck and Acadia Pharmaceuticals. Her research is supported in part by the NIH National Institute of Neurological Disorders and Stroke (Grant Number R21 NS114764-01A1). Dr. Merola: received speaker honoraria from Abbott and Boston Scientific, advisory board compensation from Abbott, Abbvie, Boston Scientific, and Lundbeck, and compensation as Chief Editor from Frontiers in Neurology Experimental Therapeutics. Dr. Litvan: Research is supported by the National Institutes of Health grants: 2R01AG038791-06A, U01NS100610, U01NS80818, R25NS098999; U19 AG063911-1 and 1R21NS114764-01A1; the Michael J Fox Foundation, Parkinson Foundation, Lewy Body Association, CurePSP, Roche, Abbvie, Biogen, Centogene. EIP-Pharma, Biohaven Pharmaceuticals, Novartis, Brain Neurotherapy Bio and United Biopharma SRL—UCB. She was a member of the Scientific Advisory Board of Lundbeck and is a Scientific advisor for Amydis and Rossy Center for Progressive Supranuclear Palsy University of Toronto. She receives her salary from the University of California San Diego and as Chief Editor of Frontiers in Neurology. Dr. Maria De Stefano: None. Dr. Maule: None. Dr. Vallelonga: None. Dr. Lopiano: received honoraria for lecturing and travel grants from Medtronic, UCB Pharma, and AbbVie. Dr. Romagnolo: received grant support and speaker honoraria from AbbVie, speaker honoraria from Bial and Chiesi Farmaceutici and travel grants from Lusofarmaco, Chiesi Farmaceutici, Medtronic, and UCB Pharma.
Data access and responsibility statement
A. Romagnolo has full access to all the data in the study and takes responsibility for the integrity of the data, the accuracy of the data analysis, and the conduct of the research.
Ethical standard
The authors declare that they acted in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki. The local institutional review board approved the study and all participants provided written informed consent.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Longardner, K., Merola, A., Litvan, I. et al. Differential impact of individual autonomic domains on clinical outcomes in Parkinson’s disease. J Neurol 269, 5510–5520 (2022). https://doi.org/10.1007/s00415-022-11221-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-022-11221-9