Abstract
Introduction
Dance can reduce motor symptoms in persons with Parkinson’s disease (PD). However, the effect on psychosocial wellbeing, including self-esteem and quality of life is less clear.
Methods
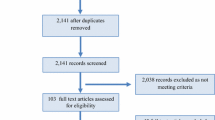
Forty-nine persons with PD (Hoehn and Yahr stage 1–4) participated in weekly dance classes for a consecutive period of 22 weeks, 36 participants completed the classes. Two baseline measurements (T1a and T1b) were performed during a 2-week control period prior to the dance classes. Post-measurements (T2) were performed immediately after 22 weeks of dance classes. Primary outcome was self-esteem as measured with the Rosenberg Self-Esteem Score.
Results
Self-esteem scores were stable across the two baseline measurements and improved significantly after the dance classes (1.5 points improvement between T1b and T2, 95% CI 0.3, 2.7; p = 0.012). Additionally, quality of life as measured with the Parkinson’s Disease Questionnaire 39 improved significantly (3.4 points reduction between T1b and T2, 95%CI − 5.7, − 1.2; p = 0.003) as did motor symptoms as measured with the Movement Disorders Society-Unified Parkinson’s Disease Rating Scale—part III (6.2 points reduction between T1b and T2, 95%CI − 10.1, − 2.4; p = 0.002). Balance confidence as measured with the Activities-Specific Balance Confidence Scale did not change.
Discussion and conclusions
Dance classes seem to improve self-esteem, quality of life and motor symptoms in persons with PD. These effects should be investigated further in a randomized clinical trial.
Clinical message
Dance classes may be a valuable complementary treatment option in people with PD to improve not only motor symptoms, but also self-esteem and quality of life.
Similar content being viewed by others
References
Armstrong MJ, Okun MS (2020) Diagnosis and treatment of Parkinson disease: a review. JAMA - J Am Med Assoc 323:548–560. https://doi.org/10.1001/jama.2019.22360
McNeely ME, Duncan RP, Earhart GM (2015) Impacts of dance on non-motor symptoms, participation, and quality of life in Parkinson disease and healthy older adults. Maturitas 82:336–341. https://doi.org/10.1016/J.MATURITAS.2015.08.002
Perepezko K, Hinkle JT, Shepard MD, Fischer N, Broen MP, Leentjens AF, Gallo JJ, Pontone GM (2019) Social role functioning in Parkinson’s disease: a mixed-methods systematic review. Int J Geriatr Psychiatry 34:1128–1138. https://doi.org/10.1002/GPS.5137
van der Kolk NM, de Vries NM, Kessels RPC, Joosten H, Zwinderman AH, Post B, Bloem BR (2019) Effectiveness of home-based and remotely supervised aerobic exercise in Parkinson’s disease: a double-blind, randomised controlled trial. Lancet Neurol 18:998–1008. https://doi.org/10.1016/S1474-4422(19)30285-6
Schootemeijer S, van der Kolk NM, Ellis T, Mirelman A, Nieuwboer A, Nieuwhof F, Schwarzschild MA, de Vries NM, Bloem BR (2020) Barriers and motivators to engage in exercise for persons with Parkinson’s disease. J Parkinsons Dis 10:1293–1299. https://doi.org/10.3233/JPD-202247
Van Nimwegen M, Speelman AD, Hofman-Van Rossum EJM, Overeem S, Deeg DJH, Borm GF, Van Der Horst MHL, Bloem BR, Munneke M (2011) Physical inactivity in Parkinson’s disease. J Neurol 258:2214–2221. https://doi.org/10.1007/S00415-011-6097-7
Earhart GM (2009) Dance as therapy for individuals with Parkinson disease. Eur J Phys Rehabil Med 45:231–238. https://pubmed.ncbi.nlm.nih.gov/19532110/. Accessed 10 Aug 2020
Keus SHJ, Bloem BR, Hendriks EJM, Bredero-Cohen AB, Munneke M (2007) Evidence-based analysis of physical therapy in Parkinson’s disease with recommendations for practice and research. Mov Disord 22:451–460. https://doi.org/10.1002/mds.21244
Ravenek MJ, Schneider MA (2009) Social support for physical activity and perceptions of control in early Parkinson’s disease. Disabil Rehabil 31:1925–1936. https://doi.org/10.1080/09638280902850261
Shanahan J, Morris ME, Bhriain ON, Saunders J, Clifford AM (2015) Dance for people with Parkinson disease: What is the evidence telling us? Arch Phys Med Rehabil 96:141–153. https://doi.org/10.1016/j.apmr.2014.08.017
Pereira APS, Marinho V, Gupta D, Magalhães F, Ayres C, Teixeira S (2019) Music therapy and dance as gait rehabilitation in patients with Parkinson disease: a review of evidence. J Geriatr Psychiatry Neurol 32:49–56. https://doi.org/10.1177/0891988718819858
Lee HJ, Kim SY, Chae Y, Kim MY, Yin C, Jung WS, Cho KH, Kim MY, Park HJ, Lee H (2018) Turo (Qi Dance) program for Parkinson’s disease patients: randomized, assessor blind, waiting-list control, partial crossover study. Explore (NY) 14:216–223. https://doi.org/10.1016/J.EXPLORE.2017.11.002
Rosenberg M (1989) Society and the adolescent self-image, Revised edn. Wesleyan University Press
Peto V, Jenkinson C, Fitzpatrick R, Greenhall R (1995) The development and validation of a short measure of functioning and well being for individuals with Parkinson’s disease. Qual Life Res 4:241–248. https://doi.org/10.1007/BF02260863
Powell LE, Myers AM (1995) The Activities-specific Balance Confidence (ABC) Scale. J Gerontol A Biol Sci Med Sci 50A:M28–M34. https://doi.org/10.1093/GERONA/50A.1.M28
Goetz CG, Tilley BC, Shaftman SR, Stebbins GT, Fahn S, Martinez-Martin P, Poewe W, Sampaio C, Stern MB, Dodel R, Dubois B, Holloway R, Jankovic J, Kulisevsky J, Lang AE, Lees A, Leurgans S, LeWitt PA, Nyenhuis D, Olanow CW, Rascol O, Schrag A, Jeresi TA, Van Hilten JJ, LaPelle N (2008) Movement Disorder Society-sponsored revision of the Unified Parkinson’s Disease Rating Scale (MDS-UPDRS): scale presentation and clinimetric testing results. Mov Disord 23:2129–2170. https://doi.org/10.1002/MDS.22340
Simpson J, Lekwuwa G, Crawford T (2014) Predictors of quality of life in people with Parkinson’s disease: evidence for both domain specific and general relationships. Disabil Rehabil 36:1964–1970. https://doi.org/10.3109/09638288.2014.883442
Horváth K, Aschermann Z, Kovács M, Makkos A, Harmat M, Janszky J, Komoly S, Karádi K, Kovács N (2017) Changes in quality of life in Parkinson’s disease: how large must they be to be relevant? Neuroepidemiology 48:1–8. https://doi.org/10.1159/000455863
Chen Y, Gao Q, He CQ, Bian R (2020) Effect of virtual reality on balance in individuals with Parkinson disease: a systematic review and meta-analysis of randomized controlled trials. Phys Ther 100:933–945. https://doi.org/10.1093/PTJ/PZAA042
Leavy B, Joseph C, Löfgren N, Johansson H, Hagströmer M, Franzén E (2020) Outcome evaluation of highly challenging balance training for people with Parkinson disease: a multicenter effectiveness-implementation study. J Neurol Phys Ther 44:15–22. https://doi.org/10.1097/NPT.0000000000000298
Shulman LM, Gruber-Baldini AL, Anderson KE, Fishman PS, Reich SG, Weiner WJ (2010) The clinically important difference on the unified Parkinson’s disease rating scale. Arch Neurol 67:64–70. https://doi.org/10.1001/ARCHNEUROL.2009.295
Acknowledgements
We would like to thank ‘Stichting Beatrixoord Noord Nederland’ and ‘Stichting De Friesland’ for their funding of the dance classes and Marrit Klamer and Lisa Rooks for their help with the data collection.
Author information
Authors and Affiliations
Contributions
WF and BB conceived and designed the study. TR, HR and WF collected the data. WF, JN, HR, PD and BB contributed to the interpretation of the data. PD performed the statistical analyses. WF and TR wrote the first draft of the article. All other authors revised the article critically. All authors gave final approval of the version to be submitted.
Corresponding author
Ethics declarations
Conflicts of interest
Wya Feenstra was involved in developing the dance classes, but has no financial interests. The other authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The study was performed in accordance with the guidelines of the 1964 Declaration of Helsinki and was approved by the Medical Ethics Review Board of the University Medical Centre Groningen. All participants signed an informed consent prior to the study.
Rights and permissions
About this article
Cite this article
Feenstra, W., Nonnekes, J., Rahimi, T. et al. Dance classes improve self-esteem and quality of life in persons with Parkinson’s disease. J Neurol 269, 5843–5847 (2022). https://doi.org/10.1007/s00415-022-11206-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-022-11206-8